Buscar
-
Motivar a los niños a comer alimentos saludables
Do you have a picky eater in your household? Or maybe you've got a snack monster who’s all about chips and candy? We're here to share a few fun strategies to motivate your little superheroes to snack on healthy foods instead! Rainbow Power-Up Eating a rainbow isn't just for unicorns! Different colors mean different powers: Red foods like strawberries and tomatoes help your heart. Orange foods like carrots and sweet potatoes help your eyes spot things like an eagle! Green foods like spinach and broccoli help you grow super strong bones. So, create a plate with as many colors as possible. The more colors, the more powers! Super Smoothies Blend your favorite fruits, such as bananas, berries and mangoes. Add some milk or yogurt and a handful of spinach. Your kids won't taste the spinach, and they'll drink a supercharged smoothie that gives them the energy to tackle any challenge. Create a Parfait Packed with Delicious Layers! Veggie Villans Who said veggies can't be fun? Turn them into heroes by giving them cool names and fun shapes. Make carrot sticks "Captain Crunch" or broccoli florets "Broc the Rock." Dip them in hummus or peanut butter for an extra flavor kick. Snack Attack Plates Create snack plates that are as fun as they are nutritious. Combine: Cheese cubes Grapes or apple slices Nuts or seeds Whole-grain crackers Mix and match these for your perfect plate! Make Your Own Trail Mix Fuel-Up Challenges Challenge your kids to eat three different healthy foods each day. Turn it into a family game to see who can eat the most colors or try the most fruits and veggies. You can even draw up a "super snacks" chart to keep track of your progress. Final Super Tip! Even superheroes have cheat days. Don't worry if your family doesn't eat healthy every meal. Just aim to eat more of the good stuff than the not-so-great stuff. Your kid's bodies will reward them with tremendous energy, focus and strength.
-
Make Your Own Trail Mix: 4 Quick and Easy Recipes
Craving a snack with crunch, sweet flavor and a powerful nutritious punch? These healthy, homemade variants of this make-it-and-take-it super snack are sure to satisfy your sweet tooth and your healthy lifestyle. Who says healthy snacks and bland taste go together? We say you can have it all — nutritious and delicious snack foods that taste great and satisfy — and trail mix fits the bill. Your homemade batch can be as healthy as you like. The nuts provide fiber, protein and a whole lot of crunchy goodness; dried fruit and touches of chocolate infuse the mix with just the right amount of sweetness. We’ve compiled some simple-to-make and hard-to-resist recipes so you can easily pick up a few items from the grocery store’s bulk bins, or your kitchen cupboard, and put together a snack for your kiddos lunches or the office. Better yet, grab your mix and head out for a stroll or hike, or take along on your next road trip or adventure in Nevada’s rugged, desert locales.
Read More About Make Your Own Trail Mix: 4 Quick and Easy Recipes
-
Nourishing Your Loved One Through Cancer Treatment
Eating healthy is a daily challenge for many, but for those with cancer, it is an even harder struggle. A cancer diagnosis affects not only those diagnosed but family members and friends, too. One key area of concern is making sure your loved one stays well by eating healthy food every day. Here are some vital cancer nutrition tips from Jessica Blauenstein, a Board Certified Specialist in Oncology Nutrition and Registered Dietitian at Renown Health. Help to Prepare Meals and Snacks for Daily Cancer Nutrition Make it grab and go. Easy-to-make meals help reduce the burden of having to cook and prepare food. Having easy to grab snacks on the counter or in the fridge can help ensure your loved one has access to those nutrients when needed. Sit outside of the kitchen. This allows your loved one to avoid cooking smells which can make them feel sick as a side effect of cancer treatments. Also try serving them cold foods such as sandwiches, cheese and crackers, or shakes which have a mild scent. Try drinkable meals. Some people with cancer find it easier to sip their calories over the course of 30 minutes to an hour. Consider smoothies or supplemental shakes such as Ensure Complete, Fairlife shakes, Orgain shakes, or Boost Plus to name a few. A great foundation for a smoothie is a protein source (Greek yogurt, protein powder, nut butters or milk) with a carbohydrate (fruits, juice or berries). Add other ingredients as desired, such as spinach, kale, and ground flaxseed or chia seeds to give it more vitamins, minerals, and fiber. Snack Ideas for Those Undergoing Cancer Treatment The following ideas are both quick and easy to make for your loved one. Chicken or tuna salad with whole grain crackers or as a sandwich on whole grain bread Greek yogurt mixed with cereal, fruit and/or nuts Cottage cheese with banana, cinnamon and/or peanut butter Favorite fruit with 100% natural peanut or almond butter spread - Try peanut butter with bananas, apples, or even celery Their favorite veggies dipped in a salad dressing of your choice - For example, carrots with hummus, tahini, or ranch dressing Cheese and whole grain crackers - Add tomato slices with a small amount of avocado, and a dash of oregano on top for more flavor Eggs scrambled with cheese, vegetables and/or salsa Peanut butter and jelly sandwich on whole grain bread A baked sweet potato with some favorite toppings Hard boiled eggs and/or egg salad with whole grain crackers, or as a sandwich on whole grain bread Oatmeal or cream of wheat prepared with milk, fruit and/or nuts Sometimes your loved one may not feel like eating or refuse to eat. If treatment side effects are impacting your loved one’s ability to eat, please visit the websites below containing recipes tailored to treat side effects. Cook for Your Life ELLICSR Of course, you may also consult a registered dietitian and/or the patients care team, if you have more cancer nutrition concerns.
Read More About Nourishing Your Loved One Through Cancer Treatment
-
Departamento destacado: Special Procedures
Chronic pain can be one of the most distressing feelings someone may encounter – and more likely than not, you know someone who is managing their pain as a part of their healthcare journey. In fact, according to the Centers for Disease Control and Prevention, about 1 in 5 U.S. adults have experienced chronic pain in recent years. One of the most common methods of treating pain is through prescription pain medications; however, with the rise of the opioid epidemic across the country, leveraging other interventions to help patients manage their chronic pain has become increasingly more important. What if there was a way to treat pain directly without the automatic need for pain medication? Luckily for patients in northern Nevada, our Special Procedures department at Renown Rehabilitation Hospital specializes in exactly that: interventional pain mitigation sans painkillers. With nearly 95% of their patients who come in with pain-related mobility issues being able to physically walk out of the hospital after their treatment, much-needed relief is clearly in store. Tight-knit and forever-caring, the Special Procedures team knows how to transform the purpose of pain management. A Penchant for Pain Alleviation Renown's Special Procedures team offers a wide variety of pain management solutions that are uniquely tailored to each individual patient’s needs. With the help of a team of 14 attentive nurses, interventional radiology technologists and a surgical technician – plus a dedicated patient access representative ensuring everything goes smoothly behind-the-scenes – these lifechanging interventions include: Epidurals (including steroid epidurals) Nerve blocks Ablations Tenotomies Spinal cord stimulator trials Peripheral nerve stimulator trials The nurses on this specialized team guide patients before, during and after their procedures, making sure they are at ease throughout the entire process. Each nurse emulates both expertise and empathy to help light the path towards healing. “Before each procedure, we get the patient’s vitals, health history and work with the doctor to answer any questions they may have about what is going to happen in the procedure room,” said Michon Edgington, RN. “After they’re all done, they come back to me, and I make sure they are ready to go home by educating them on their discharge. Our goal is to get them back to their families very quickly.” “In the actual procedure room, we perform safety checks, do charting, prepare the sterile tray for the doctor and give medication for conscious sedations, all while consistently monitoring the patient and helping the doctor out along the way to help the procedure go well,” added Shannon Boelow, RN. This team’s dedicated imaging professionals harness expertise that goes beyond capturing images. Their skillful utilization of X-ray technology serves as a guide for doctors administering treatments for pain – and according to our own physicians, our imaging technologists are some of the best in the business. “Our X-ray skills here are specialized,” said Julie Smith, Imaging Lead. “Visually, the doctor needs to see what’s going on inside the body so they can accurately place needles and steroids. We all work together collectively and work with each doctor to accommodate their preferences, helping the treatments go much faster and minimizing the patient’s exposure to radiation.” Serving as the ideal representation of both precision and support, the surgical technician on this team is an important collaborator in the procedure room, helping to ensure the success of every interventional procedure with a meticulous eye for detail. “As the Special Procedures surgical technician, I get the room ready with all the necessary instruments, including making sure everything is sterile,” said Carrie Crow, Surgical Technician. “I enjoy keeping the team organized.” Overseeing it all are the physicians, who are eternally grateful for the team for the life-changing interventions they offer every day. “Our physicians are so phenomenal,” said Brittney Summerfield, Manager of Nursing. “They are very supportive and collaborative, and they always do the right thing. They have total confidence in us.” Seeing patients walk out of the hospital happy and healthy is a driving motivator for this team. Whether they had significant experience in pain management or were ready for a completely new challenge, each team member comes to work every day inspired to move mountains. “I had worked in pain management in other facilities, and I was extremely excited to come here and solely focus on pain,” said Jodi Eldridge, Supervisor of Special Procedures. “I enjoy seeing the patients so happy when they leave no longer in pain. I feel immediate gratification, because you truly feel like you’re doing something big for the patient. It’s very rewarding.” “I decided to come work here because I worked in the inpatient setting for a long time, and I was ready to see a different side of healthcare and provide a different type of care to our community; plus, my coworkers are the best,” added Lisa Dunnivant, RN. There’s no question that the realm of pain management is a delicate one – and there is no team better suited to take on that challenge than Special Procedures, working harmoniously to bring relief and a renewed sense of livelihood for every patient they serve. “Some people believe pain management is just all about pills, and that is simply not true,” said Carrie Crow. “Our procedures are yet another way to help them manage their pain and find relief.”
-
Celebrating Blood Sugar Balance This Holiday Season
As the holiday season draws near, we find more reasons to celebrate with loved ones. At Renown Health, we are kicking off the celebrations early this November with American Diabetes Month. Approximately 37 million Americans, including 270,000 Nevadans, have been diagnosed with diabetes with as many as 95% of those diagnosed living with type 2 diabetes mellitus (T2DM). What is Type 2 Diabetes? Type 2 diabetes is a chronic health condition that occurs because your body is not using insulin (a hormone made by the pancreas to help cells use the food we eat for energy) as well as it should, resulting in high blood sugar levels. It is important to obtain a diagnosis for T2DM and ensure it is well-controlled to prevent serious health complications. Those with diabetes are at higher risk for blindness, kidney failure, heart disease, stroke and amputation. Tips for Supporting Your Health with Type 2 Diabetes Know Your Blood Sugar Levels: Work with your healthcare provider to establish target blood sugar levels, and make sure to monitor your levels regularly as advised by your healthcare provider to prevent or delay health complications associated with T2DM. Focus on Your Plate: Eating foods such as fruits and vegetables, lean meats or plant-based proteins, healthy fats and whole grains supports diabetes management. If choosing healthy foods is difficult due to your busy schedule, cost or simply because you aren’t sure where to start, talk with your healthcare provider who may refer you to a registered dietitian. Registered dietitian nutritionists are certified nutrition specialists who can provide education and practical tips for eating to support your T2DM diagnosis with visits covered by many insurance plans. Prioritize Staying Active: Engaging in regular exercise is good for everyone, especially those living with T2DM. Exercise helps your cells become more sensitive to insulin and therefore supports healthy blood sugar levels. Always check with your healthcare provider prior to beginning a new exercise plan. Support Stress Reduction: Stress is unavoidable but can be managed through regular exercise, getting enough quality sleep (7-8 uninterrupted hours per night) and practicing meditation and other mindfulness techniques. Plan Ahead for Holiday Gatherings: There’s still room for celebration while focusing on blood sugar management. Consider bringing a healthy dish to your gathering, focus on filling your plate with vegetable sides and eating those first and incorporate a family walk after dinner. If traveling, pack nutritious snacks that support your health and keep you full. Lastly, enjoy the special dishes and desserts this season has to offer in single-serving portions.
Read More About Celebrating Blood Sugar Balance This Holiday Season
-
Living with COPD? How to Maximize Your Summer Experience
June offers an official welcome to summer and the height of outdoor activities in northern Nevada such as hiking, camping, days spent at the lake and embracing long days and warm evenings with friends and family. Enjoying all that the summer season has to offer may not be as easy for those living with chronic obstructive pulmonary disease, or COPD, which effects more than 15 million Americans. What is COPD? COPD is a group of lung diseases including emphysema and chronic bronchitis that result in airflow blockages from the lungs. People may experience frequent coughing and shortness of breath among other symptoms. COPD typically impacts adults ages 65 and older and is becoming increasingly more common among women. Although smoking plays a key role in the development of COPD, air pollution and indoor air quality, and respiratory infection also contribute to disease development. While there is no cure for COPD, limiting progression of disease and managing symptoms can be achieved through lifestyle changes, therapy, and medications. Tips for Living with COPD This Summer, and Always Stay Hydrated: Staying hydrated is extremely important for people with COPD, especially during the summer. Not drinking enough water can make breathing more difficult because it increases respiratory symptoms. Make sure to always keep a water bottle with you and aim to drink 8-10 glasses of water daily. Be Mindful of Temperature: COPD symptoms can be exacerbated by hot weather. It is best to participate in outdoor activities during the cooler times of day, like the morning or evening. Check Air Quality Before You Go: Before engaging in outdoor activities, be sure to check the air quality index and plan your activities accordingly. Pace Yourself: Exercising can be difficult for people who have COPD. To make the most of your summer, try not to push yourself too hard and take breaks when you need them. If you start to feel out of breath or tired, take a break in a cool, shaded area until you feel better. Take Matters Into Your Own Hands To address the needs of community members living with COPD, the Renown Health Research Office has teamed up with Pulmonary Medicine to provide patients who are former or current smokers and have a history of frequent exacerbations with an option to participate in the ARNASA study. "COPD exacerbations have a huge negative impact on patient’s lung function” states Dr. Farah Madhani-Lovely, Chief of Pulmonary Medicine at Renown Health and Assistant Dean of Clinical Research at the University of Nevada, Reno School of Medicine. “We have had inhalers and prednisone for decades but patients are still having exacerbations. Now we have a new pathway we think will prevent exacerbations which is what this clinical trial is designed to prove.” This study will evaluate the efficacy and safety of astegolimab compared with placebo in participants 40-80 years of age with COPD. “This study in particular is so exciting because of the enthusiasm from the sponsor’s end” says Katie Buckley, Lead Clinical Research Coordinator working on pulmonology studies at Renown’s Clinical Research Office. “Often times sites aren’t assigned particularly passionate or engaged personnel who aid in carrying out these studies, but you can tell Roche Genentech’s team truly cares about the success of the study, the safety of their participants, and proving the efficacy of the investigational agent. Working on a study like this takes a village, and when the individuals on all ends share similar mindsets and work towards success as a collective unit instead of as individual moving parts, it’s amazing to see everything we’re able to accomplish.” Renown’s team of expert pulmonologists and researchers are available to join patients with COPD in support of their healthcare journey. If you are interested in learning more about this clinical trial option at Renown Health, talk to your pulmonologist at your next appointment or contact us at 775-982-3646. At Renown Health, our goal is to make it easy for patients to access clinical research as a care opportunity where patients can access a variety of standard care treatment options for their health condition or choose to participate in a clinical trial. For more information about clinical trial opportunities available to you or to ask any questions, contact the Renown Research Office at Renown-CRD@renown.org or 775-982-3646.
Read More About Living with COPD? How to Maximize Your Summer Experience
-
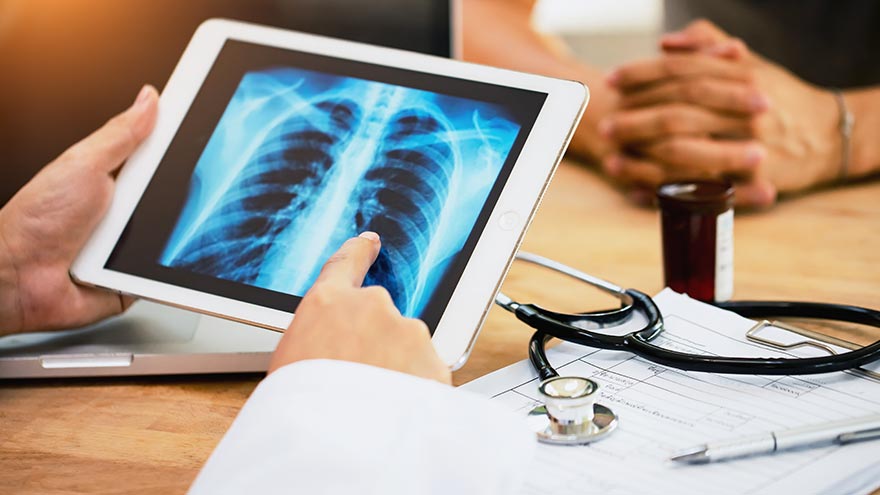
Lung Cancer Screening and Early Detection
Lung cancer is the leading cause of cancer deaths in both men and women in the U.S. The good news is the five-year survival rate increases dramatically if lung cancer is treated before spreading to other parts of the body. Julie Locken, MD, of Renown Health Imaging, explains more. What are the signs and symptoms of lung cancer? As you might expect, most lung cancer symptoms appear in the chest and can affect your breathing. Watch for signs such as: Persistent cough Constant chest pain Shortness of breath Wheezing Bloody or rust-colored phlegm Hoarseness Swelling of the neck Pain or weakness in the shoulder, arm or hand Recurring pneumonia, bronchitis or other lung infections Loss of appetite and loss of weight can also be signs of lung cancer That said, there are usually no symptoms in the early stages of lung cancer, which means getting screened can truly be a lifesaver. If you have a history of smoking, you should get screened as a precaution. What are the risk factors of lung cancer? Around 80% of lung cancer cases stem from a history of smoking tobacco. But there are other known causes, such as secondhand smoke, radon, asbestos and diesel exhaust. It’s important to do what you can to eliminate exposure to all of these to reduce your lung cancer risk. People with an immediate relative – a parent, sibling or child – diagnosed with lung cancer and people between 50 and 80 years old are also at higher risk and may need to consider screening. People who are at the highest risk are those with a history of smoking tobacco, particularly smokers who averaged one pack of cigarettes per day for 20 years or more, as well as former heavy smokers who quit in the last 15 years.
-
Alzheimer's Safety Tips for Caregivers to Know
November is National Alzheimer’s Disease Awareness Month. At Renown Health, we know that Alzheimer's safety for your loved one is a priority, as the symptoms can sometimes lead to unsafe situations. We asked Dr. Jonathan Artz – a neurology physician with Renown Health and an assistant professor of clinical neurology at the University of Nevada, Reno School of Medicine – for tips on keeping loved ones safe and secure. According to the Alzheimer’s Association, Alzheimer’s disease affects safety in various ways, specifically due to body and brain adjustments. These changes can include: Judgment, including forgetfulness Sense of place – getting lost on the way home Behavior – being suspicious or fearful Body difficulty – losing balance Sensing ability – noticeable sensitivity in hearing, seeing or temperature Dr. Artz gives us four major tips to ensure your loved one’s safety as you both navigate this disease together. Watch for Wandering Those experiencing Alzheimer’s disease tend to wander and get lost. Try the following tips to reduce the risk of wandering: Get your loved one an ID bracelet and have them wear it at all times. You can also enroll your loved one in “Wandering Support.” Install door chimes so you know when exterior doors are open. Ask neighbors to call you if they see your loved one out alone. Go with your loved one when they insist on leaving the house. Don’t argue or yell. Instead, use distraction or gentle hints to get them to return home. Discourage Driving Driving can be unsafe for someone with this disease. With this in mind, ask a doctor whether it’s safe for your loved one to drive. For example, on a case-by-case basis, there are certain situations where doctors are required to report individuals with particular cognitive impairments, wherein a form of a driving assessment will be recommended. Limit access to the car. Keep the keys with you or lock them away. Ask an authority figure, such as an insurance agent or a doctor, to tell them not to drive. Adult-Proof Your Abode A simple living space is a safe living space. This means reducing clutter and removing any issues that may pose a safety concern. You may also want to get advice from an occupational therapist (home safety expert). Keep in mind that some changes may not be needed right away. Focus on major safety concerns first. Try the following tips: Add lighting (or glow-in-the-dark tape) to brighten dark areas, including stairways and halls. Use color contrast or texture indicators for dials, knobs and appliance controls. Remind your loved one not to carry items while walking to avoid a fall. Remove sharp objects from drawers and countertops. Avoid using small throw rugs or doormats, as they are easy to trip on. Move frequently used items so that they are easy to reach. Lock away alcohol and tobacco products, as they are not recommended for dementia patients. Install handrails in the shower, tub and near the toilet. Bathroom falls are especially common. Adjust the setting on your hot water heater so water does not scald. Those with Alzheimer’s can lose their sensitivity to temperature. Move and lock up hazardous chemicals and cleaning supplies, such as bleach and insecticides. Disable and remove guns or any weapons. Supervise any medication taken by your loved one. Promote a Positive & Healthy Lifestyle Continually emphasize the strengths of your loved one by promoting participation in meaningful activities, wellness visits and healthy habits to help them improve their well-being. Here are some ways to keep them physically and mentally active: Maintain regular vision and hearing screenings and make necessary adaptations. Establish a routine for daily activities. Encourage participation in self-care and leisure activities. Work with your loved one’s doctor to establish a healthy diet. Ensure proper hydration. It may help to set reminders for your loved one to drink fluids. Encourage regular exercise. Exercise delivers oxygen to the brain, improving brain health. Promote good sleep habits. Good quality sleep can increase overall brain health and has been associated with improving memory, attention and concentration. Resources and support are available with the Renown Memory Disorders Program. Providers within this program are specifically dedicated to treating several different memory-related disorders. Memory Disorders Resources & Support.
Read More About Alzheimer's Safety Tips for Caregivers to Know
-
Departamento destacado: Food & Nutrition Services
Nutrition is a vital aspect of patient care. At Renown Health, the Food & Nutrition Services (FNS) teams take their mission of delivering patients high-quality, cost-effective, nutritious and attractive foods to the next level. From a thrice-daily trayline service with a wide variety of delicious food to the personalized dietitian services that ensure every patient gets the nutrients they need for optimal healing and recovery, Renown’s FNS teams at Regional, South Meadows and Rehab are unmatched. Food for the Good Fight The hustle and bustle of early morning food preparations gears the FNS team up to, as Renown Regional Food Service Worker Molly Kalsman puts it, “provide patients with adequate nutrition to heal.” From morning until nighttime, the team prepares three meals a day along with late trays and snacks. This isn’t your run-of-the-mill hospital food, either. Think anywhere from cheeseburgers and salads to pork roasts and baked potatoes. As you can imagine, food of this caliber requires all hands on deck in the kitchen, especially during trayline times, to ensure all patients receive quality meals that meet their individual nutrition needs. “We make an impact with good service and great food,” said Mario Nunez, a Food Service Worker at Renown South Meadows. As the food service workers are hard at work cooking and assembling, the nutrition representatives visit each patient to learn their individual dietary restrictions, allergies and food preferences. For Julie Macaluso, Nutrition Representative at Renown South Meadows, “letting the patients choose their meals” is one of the highlights of her job. “We go over meal choices for their stay, so the patient can pick out something they would like to eat and find enjoyable,” added Tara Sprehe, Nutrition Representative at Renown Regional. The immense care and attention our nutrition representatives give to every patient paves the way for our clinical dietitians to build a nutrient-dense diet plan based on the individual patient’s preferences. Dietitians are the only licensed providers that can leverage nutrition to treat, manage and prevent illness and disease to improve patient outcomes. Every day, our experienced dietitians “make recommendations in the adjustment of macro and micronutrients in order to best manage a person’s health status in the setting of trauma, diabetes, heart disease and other morbidities,” said Jessica Blauenstein, a Registered Dietitian and Board-Certified Specialist in Oncology Nutrition at the William N. Pennington Cancer Institute. Overall, for this department, the phrase “that’s not my job” will never be heard, according to Lupe Ayala, a Cook at the Renown Rehabilitation Hospital. Day-in and day-out, it’s a massive group effort – and that’s the way they like it. Setting the Service Bar High Hitting milestones and accomplishments comes naturally to this crew. The FNS team sets the bar incredibly high for food and service standards across the Renown Regional, South Meadows and Rehabilitation hospitals. The key ingredient? Synchronized teams that operate like a well-oiled machine. The meticulous trayline schedules and assembly lines, the cooks that put their heart into patient meals, the nutrition representatives and dietitians who ensure patient food wants and dietary needs are being met... the list goes on. And to top it all off, these teams certainly know the meaning of “service with a smile.” Their efforts do not go unnoticed. “I am very proud of the team I have,” said Monica Lara-Yanez, Supervisor of Food and Nutrition Services at Renown South Meadows. “They have improved their knowledge and participated in cross-training, and they are very efficient doing their jobs and helping each other. Moreover, they care about the service we provide.” One major accomplishment the FNS department achieved in recent years was implementing Room Service Connect, which aids in direct communication with patients, letting them know what foods are available to them during their stay at Renown based on their dietary needs. Locating trays of food has also never been easier. According to Tara Sprehe, “This system is also beneficial for letting food service workers know when a diet has been upgraded, discontinued, changed to NPO status or downgraded. This reduces the risk of giving the patient a diet that is not appropriate for them,” which saves both time and money for the department. At the end of the day, the FNS department has one mission, and it’s the same mission we all employ as Renown team members: do it for the patient. “It’s all about patient care,” said Jesse Holman, Cook Lead at Renown Regional. “That is the best accomplishment!” A Dedication to Renown The patients, the providers, and the passion: these are the most common themes that keep the FNS department passionate about Renown and their team. Whether they are just starting out in a career in food service or have established themselves in the clinical field, the FNS department proudly upholds the greatest standards of nutritional care that enhance Renown’s status as a top healthcare leader in northern Nevada. “I choose Renown because it is a very distinguished institution with an amazing reputation, offering a lot of benefits and growth opportunities to employees,” said Monica Lara. “It makes me feel proud to say, ‘I work at Renown.’” Renown Rehab Food Service Worker Margretta Corbet echoes this sentiment, adding, “There are good people here with happy dispositions.” Many FNS team members are especially enthusiastic about Renown’s robust benefits and career growth opportunities. For Molly Kalsman, working at Renown gives her the experience necessary to enter a career in dietetics. “Food service and hospital experience is encouraged to be accepted into a dietetics internship program, and Renown was the perfect opportunity for me to gain that experience,” said Molly. Carleigh Bates, Nutrition Representative at Renown South Meadows, is on a similar path: “Renown is a vehicle for so many things I am aspiring towards, such as getting my foot in the door for working in healthcare, improving the experiences of patients and gaining experience that will aid in my future goals.” Carleigh emphasizes that the team’s commitment to Renown’s mission is at the core of what they do every day. “We impact patient care by providing nutrition to fuel their wellness and improve their stay.” Lupe Ayala wraps up this strong conviction from the team very well: “I didn’t choose Renown; Renown chose me.” Fight the Good Fight With Us This future-minded, patient-centric department is growing! The Food & Nutrition Services teams at Regional, South Meadows and Rehab are actively hiring eager, collaborative new team members. Natasha Frisbie, FNS Lead at Renown Regional, reports that the team has “successfully hired and trained 24 new employees in the past three months” and is still expanding. “Teamwork, communication, and enthusiasm are very valuable skills to have in this department,” said Molly Kalsman. If you or anyone you know is looking for their next growing career opportunity, apply today!
Read More About Department Spotlight: Food & Nutrition Services
-
Grilled Lemon Salmon Kebabs
Salmon is a highly nutritious fish loaded with heart-healthy fats. A 3-ounce portion of salmon contains between 700–1,800 milligrams of omega-3 fatty acid. Research indicates that diets rich in omega-3 fatty acids can reduce inflammation and heart disease risk. Because salmon can be a strong flavor, lemon helps balance and bring a light citrus taste. In contrast, dill adds a slightly green, fresh note to this entrée. So, if you’re looking for a quick and wholesome meal, try this grilled lemon salmon kebabs recipe—ready in just 20 minutes!
-
Tazón saludable de verano
Say Hello to Summer in a Bowl If you've wanted to add a healthy new dish to your recipe repertoire, now's the time. This tasty vegan bowl loaded with turmeric chickpeas, marinated tofu, and quinoa is the perfect summer addition.
-
Los seis alimentos con más sal: ¿El alto contenido de sodio aumenta el riesgo de sufrir un derrame cerebral?
Excess amounts of sodium doesn’t just increase your risk of a heart attack, it can also increase your risk of a stroke. Unfortunately, avoiding that saltshaker may not be enough. Did you know that the average American consumes 3,400 milligrams of sodium each day? That’s a dangerous number considering that the American Heart Association recommends limiting daily sodium intake to 1,500 milligrams (about half the weight of a penny) to reduce the risk of heart disease and stroke. The problem is not necessarily that you’re putting too much salt on your food, it’s that salt is already in the foods you’re regularly eating. To help keep your sodium intake at a healthy level, make sure you’re aware of “The Salty Six,” six sneaky foods that are surprisingly high in sodium. Breads, Rolls and Tortillas: Although breads and tortillas may not initially appear to be high in sodium, we often consume several servings. Make sure to keep track of your total servings to see how they add up. Deli Meat, Cured Meats and Poultry: It may surprise you that six thin slices of deli meat can add up to more than half of your daily limit, so be mindful when building those sandwiches. Also, do your best to avoid cured meats, which often means the meat has been salted. Substitute uncured, skinless meats instead. Cheese: Salt is an important addition in the cheese-making process, as it prevents bacterial growth. Unfortunately, that added salt can increase your health risks. Limit the amount of cheese you add to meals to keep your sodium content down. Pizza: Take a quick look at the first three items above and it should be no surprise as to why pizza made the list. One slice and you’ve met at least half of your daily limit. Go easy on the cheese and try adding more veggies instead of meat. Canned Soup: One cup of canned soup can be as high as nearly 1,000 milligrams of sodium. When shopping for canned soup it’s important to check the label – not just on sodium content but serving size as well. Always select low-sodium options when possible or cook your own soup at home. Sandwiches and Burgers: A sandwich or burger from your favorite restaurant can contain more than 100 percent of your daily sodium limit. When dining out, it is best to select low-sodium options or eat a half portion to limit the amount of salt. If some of your favorite foods are on this Salty Six list, don’t panic. Although these foods can be high in sodium, it isn’t necessary to cut these foods out of your diet completely. It’s just important to eat them in moderation and be mindful of your daily sodium intake. Look for low-sodium options, use herbs and spices instead of table salt and do your best to stay under the recommended daily limit of 1,500 milligrams.”
Read More About The Salty Six: Are High-Sodium Foods Increasing Your Stroke Risk?