Buscar
-
What You Need to Know About RSV
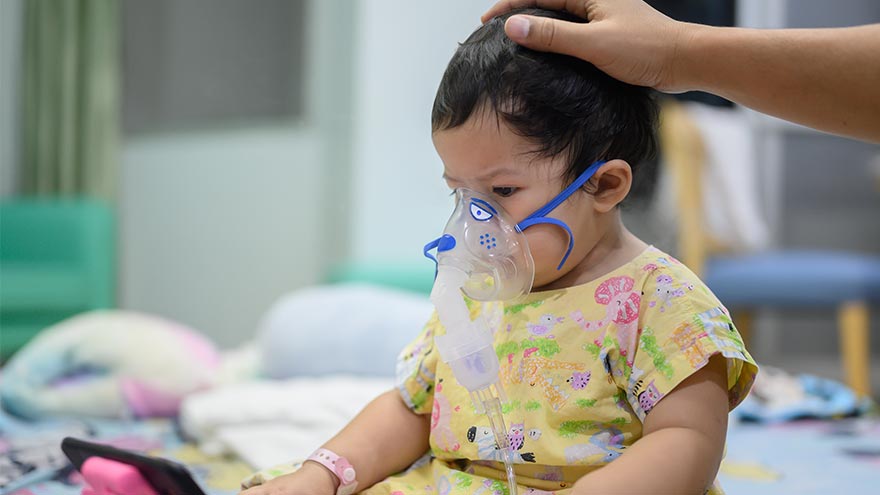
Respiratory syncytial virus, also known as RSV, is a common respiratory virus that impacts the lungs and breathing pathways. The virus can be dangerous for infants and young children and is also concerning for older adults. While most older kids and adults only experience cold-like systems and recover in a week or two, an estimated 58,000-80,000 children younger than 5 years old are hospitalized due to RSV each year, and in 2022 healthcare organizations across the country are experiencing higher infection rates than in years past. "We are experiencing a strong RSV season and do not expect it to go away anytime soon," said Dr. Kris Wilson, Division Chief of Renown Children's Primary Care. "Infants who are infected with RSV almost always show symptoms of runny noses and cough. Call your healthcare provider immediately if your child is having difficulty breathing, is not drinking enough fluids, or is experiencing any worsening of these symptoms.” Symptoms of RSV: Runny nose Decrease in appetite/inability to drink Dry diapers, an indication of dehydration Cough, which may progress to wheezing or difficulty breathing Irritability (most common in very young infants) Decreased activity (most common in very young infants) Decreased appetite (most common in very young infants) Apnea, pauses in breathing for more than 10 seconds (most common in very young infants) What to do if you think your child has RSV: Call your pediatrician! If you suspect your child might have RSV, consulting their healthcare provider is the best first line of defense. From here they will help you build an appropriate treatment plan for child. Keep in mind that many pediatrician offices offer 24/7 call lines. If your child is experiencing retracted breathing (when the area between the ribs and in the neck sinks in when a person attempts to inhale), dehydration (not drinking and decrease in wet diapers) or apnea (pauses in breathing for more than 10 seconds) please call 911 or go to the closest emergency room.
-
Young and Resilient Fighters: Advanced Childhood Cancer Treatment Close to Home
Austin was five years old when he was diagnosed with leukemia. A fever and pale looking skin prompted his mom, Brenda, to bring him into his primary care physician in Carson City. After doing some blood work, the fight to beat Austin's cancer began. The initial shock of learning your child has cancer is traumatic and can feel like a whirlwind. Then the questions begin – will my child survive, what happens next, how will we tell his siblings, will we have to travel out of state for quality care? The list of questions feel endless. While grappling with the news, Brenda brought Austin to Renown Children’s Hospital for an additional check-up. This weeklong hospitalization started with a series of tests to confirm Austin’s diagnosis and ultimately it led to treatment for the leukemia. Dr. Jacob Zucker, a pediatric oncologist at Renown Children's Hospital, was with Austin every step of the way, even meeting him in the parking garage on his first day of treatment. Brenda is eternally grateful that Dr. Zucker was on staff at Renown Children's Hospital, which allowed them to keep Austin's care in Reno. The alternative was to travel out of state for care. "Dr. Zucker was the best thing to ever happen to our family. I consider him a part of our family now," said Brenda. "His kindness and knowledge gave us faith in him." Treatment for Childhood Leukemia Austin’s treatment was broken into a number of stages with the first eight months of therapy being the hardest. He would receive almost weekly therapy at Renown Children’s Infusion Center as well as frequent spinal taps with chemotherapy. After eight months, and for the next three years, Austin would receive a maintenance phase therapy. This meant oral chemotherapy every day, IV chemotherapy once a month, spinal chemotherapy every three months and steroids for the first five days of every month. After more than four years of fighting cancer, Austin, now 10, is free of any disease. Currently, he has blood work every two months to ensure he is on the right track. Seeking Advice from Children’s Oncology Groups Throughout Austin's treatment, Brenda regularly sought advice from Children's Oncology Group (COG) members. COG is the world’s largest organization devoted exclusively to childhood cancer. Renown Children's was not a member of COG at the time of Austin's treatment -- with the closest facilities located in the Bay Area and Salt Lake City – but it is /now. “When faced with pediatric cancer, the last thing parents should worry about is traveling great lengths to receive the best in cancer care," said Larry Duncan, Vice President of Pediatrics and Surgery and Administrator at Renown Children's Hospital. "We are proud to now offer the most advanced childhood cancer treatment options here at Renown, close to home and convenient for area patients and their families.” This membership allows Renown to enroll our youngest patients – just like Austin – in the latest clinical trials, including groundbreaking treatments, studies to understand these diseases better and in addition, this program will focus on supportive care and survivorship. "The COG allows Renown providers to access treatment plans that were not available to non-COG hospitals when Austin was receiving treatment," said Brenda. "It comforts me to know that not only can children receive cancer treatment right at home, but their parents can now elect for them to participate in trials and plans that are at the forefront of cancer treatment today." How You Can Help Make a Difference Renown Health is focused on being the destination for all your family’s health and healthcare needs. As a not-for-profit health system, Renown relies heavily on community funding. If you are interested in supporting Renown Health, and kids like Austin, please consider giving to Renown Health Foundation. Donations are accepted through the following ways: Make a gift at www.renown.org/give Call Renown Health Foundation at 775-982-5545 Mail a check to Renown Health Foundation, 1155 Mill St., 02, Reno, NV 89502
Read More About Young and Resilient Fighters: Advanced Childhood Cancer Treatment Close to Home
-
Experto en escoliosis pediátrica de Reno da nuevas esperanzas a una niña
For Michael J. Elliott, MD, a pediatric orthopedic surgeon specializing in scoliosis, it’s just another day helping patients. But to local five-year-old Makenna Christensen, her substantial spine correction is life-changing. Though her journey to body confidence was months in the making, her smiles are a reminder that a thorough, thoughtful treatment plan can yield amazing results. A Surprising Start Words don’t adequately describe the feelings you have when you unexpectedly learn your child has a birth defect. For Nicole and Nick Christensen it was a shocking surprise. During Nicole’s sonogram appointment something unusual was seen. After an amniocentesis, their baby girl was diagnosed with Noonan syndrome, which can affect a child’s height and bones. To prepare, the couple read all they could on the subject. Fortunately their daughter Makenna, was born full term and healthy. Shortly after birth, Makenna had some feeding issues and returned to the hospital. Although they resolved and she had no major complications, both parents felt unsure about their newborn’s future. With the help of Nevada Early Intervention Services , Makenna’s development was monitored until she was three years old. “Her posture has been an issue her whole life,” says Nicole. Nick also noticed when Makenna started walking her range of motion was poor. It was especially noticeable when she got dressed and raised her arms to put on clothing. Nicole observed Makenna was falling a lot in preschool. She asked Makenna’s pediatrician about physical therapy to support her coordination and muscle tone. Although physical therapy was helping Makenna, her therapist suggested Nicole seek the opinion of Dr. Michael Elliott, a pediatric specialist in orthopedics at Renown Children’s Hospital. Scoliosis Casting - A Successful Treatment Approach Dr. Elliott diagnosed Makenna with scoliosis, an abnormal curvature of the spine. While this condition is most common during a teenage growth spurt, it can also happen in early childhood. Affecting about four million people in the United States, it is estimated 20 percent of all spinal deformities in the U.S. are people living with scoliosis. Makenna’s spinal curve was significant – over 30 degrees. Through years of experience Dr. Elliott opted to put Makenna in a spinal cast, instead of multiple surgeries. “My approach is to postpone surgery as long as possible - it is tough for the patient and families,” he says. “Often excellent results can be achieved through non-invasive treatments such as, casting and bracing.” Nicole appreciated Dr. Elliott’s reassurance through the treatment plan. “It was obvious through the X-rays that there was a significant issue,” she shares. “He guided us through the timing and process and how correcting it sooner would help keep her future growth on track.” For seven months Makenna wore a cast that looked like a tank top, bracing her spine while allowing movement. Now she wears a hard plastic brace, specially fitted to her body. “Kids tolerate casting well,” explains Dr. Elliott. “It is a 45-minute procedure. The patient sleeps while their spine is put into traction as the cast dries.” She will continue to wear larger braces as she grows, eventually only wearing them at night. A Straight Path into the Future Dr. Elliott admits, “Not every cast is a cure. Two thirds of a child’s spinal growth happens by the age of five. Getting past the five-year mark means fewer surgeries. It’s wonderful to see Makenna’s body image improved.” Nicole agrees, “The way Makenna holds herself is completely different. She’s more confident on her feet and more balanced.” She can now play with her sister Aria, 4, and brother Lexi, 8 months, without the fear of falling. Nick is in awe of the improvements she has made, “Seeing her thrive more has been wonderful.” The Christensen’s are hopeful about the future. “Makenna is doing really good. She’s wearing her hard brace full time and her growth is consistent,” expresses Nicole. “She’s even starting swim lessons this week.” With mask wearing at every doctor visit during the COVID-19 pandemic, Makenna and Dr. Elliott look forward to seeing each other’s smiles in the future. Makenna’s story highlights the over 18 different specialty options for children locally at Renown Children’s Hospital.
Read More About Reno Pediatric Scoliosis Expert Gives New Hope to Young Girl
-
Bone Fractures in Children Honest Expert Advice
Michael Elliott, MD, head of the Department of Pediatric Orthopedics and Scoliosis, answers some common questions about bone fractures. Is there a difference between broken bones and fractures? No, these are two different names for the same injury. Of course the common term is a broken bone. Using either name will describe your concerns. Medical personnel typically describe a broken bone as a fracture to a specific bone. For example, a broken wrist is also a fractured distal radius. To clarify, this describes the injured bone and the precise location. How do I know if my child has broken their bone? Many times children will fall and complain of their arm or leg hurting. In most cases the pain goes away and the child will return to their activities. When there is a deformity to the limb (curve in arm) and the child is complaining of pain, it is probably a fracture. If the arm or leg looks straight, look to see if there is any swelling or bruising. Both are signs of a possible fracture. Finally, if the limb looks normal but the child continues to complain, gently push on the bone. Likewise if it causes the same pain, then they likely have a fracture and should have an x-ray. My child fractured their growth plate, what does this mean? Growth comes from this area of the bone. In detail, these are located all over the body but typically at the end of the bones. With this in mind, fractures to these areas can result in the bone growing abnormally. Because of potential shortening of the arm or leg, or bones growing crooked, it is important to follow fractures closely (up to 1-2 years or longer). It is better to identify a problem early. Small problems can be treated with small surgeries. What if the bones of the x-ray do not line up? Because children are growing, unlike adults, their bones will remodel and straighten with growth. The amount of remodeling occurring depends on a child’s age, the bone fractured and the location. In many cases an angled bone will grow straight over the course of a year. For this reason, someone with experience in caring for children needs to follow bone growth. How long does it take fractures to heal? Factors deciding when a cast can come off include: Child’s age. Bone fractured. Fracture location. Young children heal faster than teens, teens heal faster than young adults, who heal faster than older adults. In young children most fractures heal in 4-6 weeks. However, teens generally take 6 weeks to heal, and adults can take much longer. Although your child is out of their cast, it may not be healed completely to return to all activities. Placing a splint is during this time is common. This typically gives them added protection for several weeks after their cast is removed - in case they forget their limitations. What if my child is still limping? Whether a child is in a walking or non-weight bearing cast, removing it often leaves them stiff and sore. Therefore many children will walk as though they still have a cast in place. In most cases this resolves in about three weeks. Regardless, if your child is still limping or walking abnormally after three weeks, contact the treating doctor. They may benefit from physical therapy or a repeat evaluation. (This article was original published in the July 2019 issue of South Reno Kids & Sports.)
Read More About Bone Fractures in Children Honest Expert Advice
-
Clubfoot An Unexpected Story of Expert Baby Care
A clubfoot is where the foot is turned in on itself and points toward the ground. A clubfoot diagnosis during pregnancy is surprising and challenging during any circumstance. And in the case of parents anticipating surgery during a pandemic, options can be scarce. These parents took a deep breath, and with the help of Michael J. Elliott, MD, pediatric surgeon with Renown Children’s Hospital, their baby is on the road to recovery.
Read More About Clubfoot An Unexpected Story of Expert Baby Care