Buscar
-
Del paciente al PAR: Camino de Jodee hacia Renown
When faced with chronic pain, that agonizing feeling of dread can be overwhelming to anyone, let alone a cancer survivor. Take Renown Patient Access Representative (PAR) Jodee Elder, for example. As she was receiving radiation treatments while Fighting the Good Fight against cancer, she started to experience pain at the base of her spine that ended up progressing to lower spine arthritis. On top of trying to beat cancer, the last thing she needed to deal with was the intense pain that was affecting her everyday life – and she deserved a solution that was going to provide her with the relief she needed for the long term. That’s where the Special Procedures – Pain Management department at Renown Rehabilitation Hospital – a part of Renown Spine, Sports & Pain Management – stepped in. But the team of doctors, nurses and imaging technologists Special Procedures had more on their minds for Jodee beyond pain relief. As a Renown employee, they knew what a best-in-class PAR Jodee was in her unit at the time, and they wanted that level of passion as the face of their department. Little did they know that Jodee shared the exact same sentiments. From Patient... As a skilled Patient Access team member since 2018, Jodee knows first-hand how important it is to set patients up for success before, during and after an intimidating procedure. She began her Renown career as a Pre-Registration PAR, eventually taking her expertise to Surgical Preadmission. During her years on those two teams, she honed her craft as a personable, patient-facing guide, continually going above and beyond for every patient and employee. But there was one problem: the chronic pain in her lower back that happened as a result of her radiation treatments. This pain ended up being diagnosed as lumbar spondylosis, a degenerative spinal condition that causes arthritis in the back. And when you work a desk job, back pain can be especially excruciating. When 2023 rolled in, Jodee knew she needed to try something new for her pain, something that would give her relief once and for all. After some research and advice from her doctor, she learned about Special Procedures, a team at Renown Rehabilitation Hospital offering pain management options that she wasn’t previously familiar with. Eventually, her care teams discovered that a bilateral radiofrequency nerve ablation may give her the relief she needed. Throughout the entire process, Jodee recalls feeling supported every step of the way with an experience personalized just for her. Despite being nervous at first, she was quickly put at ease by the caring nature of her pain management team. “From scheduling and the pre-operative process to the procedure and recovery experience, I often think about the amazing care I received from the entire team,” said Jodee. “Dr. Casey Keating and the nurses were with me at every point of my procedure. This was such a personal experience. I was treated like I was their only patient for the day, and everyone tried hard to alleviate any anxiety, stress or worries I had by comforting me with things like music, rubbing my leg and one-on-one conversations throughout the process.” Since her procedure, Jodee has been virtually pain-free, happily noting that she hasn’t taken any pain relievers from that day on. She gained a lot of coping skills from her care team that, as fate would have it, would inspire her to help other patients who are preparing for their own procedures. ...To Pain Management Patient Access... Before her first procedure even began, Dr. Keating was already told all about Jodee by a former coworker, who applauded her organizational skills. He very quickly was impressed by her work ethic and experience as a PAR. While she was undergoing her procedure, Jodee couldn’t help but notice how the nurses went above-and-beyond for her and treated her like she was a part of the team – even before they knew her. She immediately felt at home in Special Procedures, not only because of the level of care the team provided but also because of how much her life changed after receiving the much-needed relief for her back pain. “When I came for my first injection, Dr. Keating introduced me to the nurses as ‘the PAR we want over here,’” said Jodee. “I was on the fence regarding leaving my current PAR role, but after my experience with Special Procedures, the team really sold me on the opportunity. I immediately thought, ‘I want to be a part of this.' They were so appreciative of me from the start." And the rest is history. On Nov. 17, 2023, Jodee began her journey as the PAR dedicated solely to Special Procedures. On a typical day, you can find Jodee interacting with patients ahead of time to make checking in more enjoyable, helping patients through the pre-registration process, scheduling our Renown-employed and community providers for each procedure, checking up on authorizations, and of course, leaving a positive impact on everyone she connects with. In addition, she is known as the Special Procedures “chart master” as the main employee organizing each patient’s chart. But her duties as a PAR go beyond the desk. As a former patient herself, she has the unique ability to relate to Special Procedures patients who are worried and anxious about the road ahead. “When nervous patients come in, I can connect with them on a personal level and support them with suggestions that helped me out when I was going through my procedure,” said Jodee. “I love being patient-facing. You wouldn’t believe how many patients we’ve helped enter their procedures calmer than they were before and get the relief they need. I enjoy taking care of these patients – that's why I got into healthcare. I wanted to make a difference.” ...And Beyond Today, Jodee has been a proud PAR in Special Procedures for almost a year. She has thoroughly enjoyed her time with her fellow team members, who have been nothing short of a family to her in more ways than one. “This team is incredibly supportive of me both at work and in my personal life,” said Jodee. “When my mother passed away, they sent me a beautiful flower arrangement and a card that they all signed. The day I came back to work, they all hugged me and said they were always there for me if I wanted to talk. It’s like a big family here.” In her experience as a patient and a PAR, Jodee lives by one main motto: start a chain reaction. As she emphasizes, it only takes one of us to start a chain reaction to affect patients and the community. In Special Procedures, it starts with Jodee. And in life, she tells her kids to be that chain reaction starter. Outside of work, Jodee enjoys spending time with her kids and is happily anticipating the arrival of her grandson, who was conceived very close to the day that her mother passed away. She always makes time to create new memories with her family, including “tattoo roulettes,” where they each put a few tattoo ideas in a hat and pick one at random; they then go out and each get matching tattoos as a testament to their love for one another. “When one life ends, another life blooms,” said Jodee. If you are interested in receiving care with Renown Spine, Sports & Pain Management, speak with your provider about a referral to our specialized team. In the meantime, we encourage you to learn more about navigating your pain management care with Renown Health.
-
Un viaje de apoyo: Cómo las subvenciones de la Sociedad Americana contra el Cáncer afectan a los pacientes en Renown
For many cancer patients, a significant hurdle is simply getting to treatment. Patients from Nevada and California often face considerable financial and logistical challenges when traveling for care. Limited resources for transportation and lodging can result in missed appointments, treatment interruptions and delays in follow-up care. To address this crucial need, Renown Health Foundation partners with the American Cancer Society (ACS) to ensure our patients can access the care they need by reducing financial barriers many patients face ACS awarded $70,000 to Renown Health Foundation last year. These funds, distributed as gas cards and lodging support to qualifying patients, have proven to be a lifeline in assisting those in need. Fueling Hope with Gas Cards Through our partnership with ACS, Renown supported 128 cancer patients over the past year. This assistance provided 2,260 round trips, ensuring that patients from Nevada and California could attend their critical treatments at the William N. Pennington Cancer Institute at Renown. These patients, aged 15 to 94, traveled up to 320 miles, sometimes from remote areas such as Tonopah, Elko and Susanville, for their cancer care “We're deeply committed to supporting our patients through every step of their journey, and our partnership with the American Cancer Society is instrumental in making that happen,” said Jocelyn Mata, Oncology Social Worker at the Pennington Cancer Institute. “Without them, we wouldn't be able to provide the crucial financial assistance that many of our patients need.” Jocelyn works with qualifying patients to provide gas cards and accommodations at The Inn at Renown, a hotel at Renown Regional Medical Center. She ensures they can focus on their treatment without worrying about the financial burden. Lodging Support for Peace of Mind Along with transportation aid, we can provide safe and comfortable lodging for qualifying patients. "We encourage patients to rest and, if they have a long journey home, to stay overnight," said Dr. Max Coppes, Director of the William N. Pennington Cancer Institute. "Providing lodging support ensures they have a safe and comfortable place to recover before making the trip back." This assistance is crucial for those who travel far from home, allowing them to focus on healing without the added stress of finding and affording accommodation.
-
Cómo manejar el dolor con Renown Spine, Sports & Pain Management
Chances are you or someone you know will deal with chronic pain at some point in life. In fact, in the U.S. alone, one in five adults have experienced chronic pain in recent years, according to the Centers for Disease Control and Prevention (CDC). The road to relief is a frequently traveled one that can be filled with twists and turns, so it’s important for patients to have a trusted provider by their side navigating that journey. We interviewed Dr. Sharlene Su, a pain management physician with Renown Medical Group, who told us what patients can expect when seeking care with Renown Spine, Sports & Pain Management (RSSPM) and all about the variety of pain relief options available to patients. What pain management treatment options are available outside of painkillers? This depends on someone’s root cause of pain. For example, for pain from arthritis of the spine or major joints, radiofrequency ablation can relieve most of the pain for six months to two years, which can be life changing. If someone is suffering from a pinched nerve in the neck or back, an epidural can be useful. Nerve stimulators can also be a great option to relieve pain for years. One of the advantages of the procedures we perform at RSSPM is that they reduce the need for painkillers, which are notorious for having side effects of their own. Physical therapy can also be a very helpful tool to treat pain. It is an exciting time in the field of pain medicine right now because new advances are -constantly being made. At Renown, we pride ourselves on staying current with the most cutting-edge treatments to ensure our patients always have the best available to them. What are some at-home tips and tricks that patients experiencing pain can do on their own for some relief? If pain is related to posture or physical activity, consider doing stretching and strengthening exercises. YouTube can be a great (and free) resource for this. In terms of medications, over the counter topical pain creams can be great. Tylenol is one of the safest pain medications for those without preexisting liver conditions. On a short-term basis, anti-inflammatory medications can often be used safely depending on one’s overall health. Ice and heat can both be useful for treating muscle pain. Can you tell us more about the services Renown Spine, Sports & Pain Management offers? Our team specializes in identifying the root cause of each patient’s pain and partnering with them to develop a custom plan tailored to their individual needs, which can involve injections, physical therapy and medications. We treat patients ranging from top-level athletes, to weekend warriors, to grandparents who’d like to be able to keep up with their grandkids. Once we relieve a patient’s pain, our role then transforms into a coach, educating and guiding our patients on how to prevent their pain from coming back. At RSSPM, you’ll see the same doctor every time, which means that your provider will get to know you very well, and you’ll receive the same high-quality consistent care whenever you come for a visit. Renown has a unique pain management team called “Special Procedures” that not many people may realize is a great option for care. How does this team treat pain? Our Special Procedures team is crucial to the high-quality pain management care that we provide. We have an amazing staff that assists with X-ray guided procedures including epidurals, radiofrequency ablations, joint injections and nerve stimulators. Dr. Casey Keating, our division chief, and I work with this team to ensure that every procedure is done with the same precision, attention to detail and quality. The Special Procedures team regularly receives feedback from patients on how well taken care of they felt during their procedure. If someone is experiencing pain from an injury or even an unknown reason, what should they do to get care for their concerns? Contact your primary care provider for a referral to have an evaluation with us! RSSPM accepts most insurance plans and are proud that our wait times are averaging less than one week to be seen as a new patient. Two more doctors will be joining us in the next few months, which should reduce our wait times even more. There are so many targeted and effective ways to treat pain nowadays, and it is worth addressing to live the life you want to live.
Read More About Navigating Pain with Renown Spine, Sports & Pain Management
-
Las piezas del rompecabezas: Thonet LaBadie’s Breast Cancer Journey
“A breast cancer diagnosis begins much like a jigsaw puzzle to be worked through. It’s an overwhelming mess of scattered pieces that make no clear sense, poured out of the box into a crumbling pile of confusion. But slowly with persistence, focus, determination, a positive attitude and working through the challenges day by day and piece by piece, they in time both become whole and beautiful again.” – Thonet LaBadie On Feb. 13, 2015, Thonet’s life as she knew it took a drastic turn. In just one moment, everything shifted. The happy and healthy wife, mother of 17-year-old twins, former teacher and immunization specialist was about to face the fight for her life. That fateful day nearly a decade ago was when she received the unsettling news: she had breast cancer, and it had metastasized to her lymph nodes. Though she was faced with a daunting diagnosis, Thonet’s positive spirit and zest for life never wavered. Never did she think, “why me?” Nor did she think, “I’m not strong enough.” Her thought process was quite the opposite – “I am going to ride this rollercoaster until it stops, and I walk away cancer free.” With her loving family and friends rallying behind her, as well as her expert Cancer Care teams at Renown Health and Cancer Care Specialists (formerly known as Reno Oncology Consultants), Thonet knew that her journey would not be traveled alone, and she was determined to defeat cancer once and for all. She promised her daughter Jourdyn she would stay strong and not give up the fight. The Unexpected Discovery Thonet did everything she believed was right in her preventative healthcare journey. She lived an active lifestyle, she filled her life with love and happiness, she did not have any genetic markers for breast cancer and never missed a preventive check-up. Someone like her shouldn’t develop such a debilitating disease, right? As it turns out, she was told by professionals that with this disease, it’s become more often not about who develops breast cancer – but when. Breast cancer makes up for about 30% of cancer diagnoses in women across the U.S. So, when Thonet felt a lump in her breast in Nov. 2014, she knew she had better play it safe than sorry. She took her concerns to her doctors, who ran all the necessary tests. The unfortunate result: invasive ductal carcinoma (stage 2B), the most common form of breast cancer. Though Thonet was terrified, she was also tenacious. She was ready to Fight the Good Fight right then and there. Thonet chose to undergo a bilateral mastectomy. So that’s precisely what she did in April 2015 at Renown Regional Medical Center. Thonet was ready to put breast cancer behind her, but unfortunately, the trek was just beginning. During her mastectomy, her care team tested her lymph nodes. Four were removed. What came next was her most valiant fight of all: chemotherapy coupled with radiation, as well as more reconstructive breast surgeries along the way. Courageous Connections With 36 radiation treatments, 8 rounds of chemotherapy, 6 surgeries and 1 brave spirit, Thonet's healthcare journey has been nothing short of vigorous. Fortunately, she had an expert oncology team on her side every step of the way. And it goes even further – Thonet’s college acquaintance Dr. Jennifer Sutton, an oncology physician at the William N. Pennington Cancer Institute (formerly the Renown Institute for Cancer), was her radiation oncologist. She felt comfort knowing that a significant aspect of her care was in the hands of a trusted physician and a team of loving nurses, cancer care navigators and radiation therapists, whom she calls the “Renown Radiation Rockstars.” Thonet felt an immense connection not only to her warm and welcoming care team but also the other oncology patients she met along the journey. Patients facing cancer often receive radiation treatments several times a week, so Thonet had a chance to make close relationships with the other patients who were on a similar path as she was. Throughout her treatment process, Thonet participated in cancer support groups, which she believes are vital for anyone diagnosed with the disease. “Had it not been for my diagnosis, I would have never met all the amazing people I did at Renown and beyond,” she recalls. “At the end of my treatments, I knew I was going to miss them.” The love and support of Thonet’s care team, fellow patients, family, friends and community helped her remain positive throughout the entire process, always focusing on the positive – even during the most physically and emotionally tolling parts of treatment. Crossing the Finish Line Every day brought a new obstacle to overcome, whether it was a treatment, a side effect or an emotional response to the intense journey. Thonet’s motto throughout it all was “day by day, one foot in front of the other, from start to finish.” In Dec. 2016, Thonet finally made it to that finish line. With the completion of chemotherapy and radiation behind her, she walked out the front doors of the Pennington Cancer Institute, threw her fist in the air in excitement and finally got to revel in the fact that she had her health back. She had survived. Inspired by her journey and her breast cancer “sisters” she met while in treatment, Thonet wanted to give the same level of care and attention she received back to her fellow community members battling cancer. She proudly serves as a breast cancer “angel,” offering comfort and support to those who need it most. Thonet is also looking forward to the completion of the Pennington Cancer Institute’s Conrad Breast Center, currently under construction at Renown South Meadows Medical Center, noting how important it is for breast cancer patients to have expanded access to crucial cancer care in south Reno. Today, at nine years cancer-free, Thonet is thoroughly enjoying her life. She loves traveling, spending time with family and seeing her now-adult son and daughter thrive in their own lives. She also recently underwent hip replacement surgery and is proud to be back on her tandem bike with her loving husband of 33 years, Mike, who she credits for his never-ending support in sickness and in health. “No looking back – only forward to healthy living. Onward!” Thonet exclaims. And for anyone out there going through cancer treatments, Thonet has some words of wisdom to take to heart: “Cancer chose the wrong person when it tried to tackle us. Stay strong and fight on, day by day. On even the most difficult, darkest day, remember that you are stronger than you know.”
Read More About The Pieces of the Puzzle: Thonet LaBadie’s Breast Cancer Journey
-
Conozca a Haley Longfield: Un terapeuta de radiación y corredor de barril reconocido
Many Renown Health employees have deep roots in the northern Nevada community and Haley Longfield is one of them. She’s a fifth-generation northern Nevadan currently living in Fernley and commuting to Reno three days a week for her job as a Radiation Therapist for the William N. Pennington Cancer Institute at Renown Health. She’s also a wife, mother of a 1-year-old, and an avid horseback rider who enjoys the western way of life. This year, Haley is excited to compete in the Reno Rodeo for a second time. A Life-Long Passion Haley started riding horses in the fourth grade and quickly fell in love with it. A few years later, she started barrel racing and developed a profound love for the adrenaline-filled sport. “When I turned 18, my dad gave me all of the responsibility of owning a horse,” said Haley. “Ever since then, I’ve been paying for and taking care of my own horses.” As many who know and love horses would likely agree, Haley says they are therapeutic for the mind, body and soul. “Riding horses is a great way for me to use my brain and focus, or think about nothing at all,” said Haley. Recently, Haley qualified to compete in this year’s Reno Rodeo in barrel racing with her 7-year-old mare named Hershey. “The first time I competed in the Reno Rodeo was quite a few years ago with my high school rodeo horse, and Hershey is the granddaughter of that horse,” said Haley. “The thing that I’m most excited about in competing at this year’s Reno Rodeo is getting to ride a homegrown horse in my hometown rodeo – she’s gorgeous, easy-going and gives it her all.” Above: Haley Longfield on her horse Hershey at a barrel race Circle of Support Haley feels grateful to have the support of her family, friends and team at Renown. “In addition to my family and friends, I have an incredible team at Renown that cheers me on both in my professional and personal endeavors,” said Haley. “I couldn’t do it all without them.” Alongside qualifying for the Reno Rodeo, Haley also recently received her bachelor's degree in applied science with an emphasis in radiation therapy. Her career development goals consist of moving into leadership within her department. “My leader and team have been nothing but supportive of my goals. Our leader is invested in everyone’s personal development and aspirations, as well as our professional and career development,” said Haley. “I’m excited to one day follow in my leader’s footsteps and help employees in our department reach their own goals. I aspire to become a great leader like she’s been to us.”
Read More About Meet Haley Longfield: A Renown Radiation Therapist & Barrel Racer
-
Departamento destacado: Programación de cirugías y procedimientos
When it comes to intimidating procedures such as surgery, cardiac catheterization (Cath) or interventional radiology (IR), there can be a lot of unknowns. What can I expect on the big day? What will happen after I’m all done? Will I have to worry about my orders not being in the system? Who can I call if I have any last-minute questions? It’s easy for your thoughts to race as you approach your procedure date, but luckily, there is a team who puts your mind at ease. With Renown Health’s Surgery & Procedure Scheduling department, patients can breathe a sigh of relief knowing that all the nitty-gritty is taken care of before they step foot in the procedure room. This team operates in the mindset of a complex Tetris board – fitting in all the pieces to make sure every patient is set on the path for surgery success. Consistent Contact Our Surgery & Procedure Scheduling team has a unique history. Initially operating as two separate teams, over the last year, our leaders skillfully combined the two teams together under one umbrella. That allows the now singular team to have line of sight across every surgery and Cath or IR procedure plan and be better stewards of the resources they have at their fingertips to provide streamlined, more-connected care for patients. As one might imagine, with the merger of the two teams, the day-in-the-life of each team member is full of a variety of crucial checklist items to cross off – all supporting constant communication from patients to providers. On the surgery scheduling front, these team members are resource rockstars. From working with referring providers to get patients scheduled appropriately to ensuring rooms and equipment are available for every patient, this team makes sure everything and everyone is in place when the time comes to help create a successful procedure and the best possible patient experience. “In surgery scheduling, we handle inbound calls for the outside offices to get time scheduled for each patient in the operating room (OR),” said Lydia Sharkey, Senior Scheduler. “We make sure there are plenty of anesthesia resources and equipment for every surgery, including any important information that we need to schedule patients appropriately and adding all documents to the OR board. If we need to swap rooms or move patients around, we handle that process too.” Over on the IR/Cath scheduling side of things, this team is on the frontlines of patient communication. They are experts in helping patients navigate their procedure from start (seeing their provider and obtaining the proper referrals) to finish (the day of the procedure and post-procedure process). “My day is a little different than the hospital schedulers; our part of the team handles the outpatient aspect,” said Adrienne White, Senior Scheduler. “We are in constant contact with patients and the IR and Cath departments. We help them navigate their procedure, including what to expect during and after the procedure. We get them through the process as easily as possible and ease their minds, so they know what is going to happen every step of the way. It’s all about communication, communication, communication!” This department has a significant overarching role: make sure all documents and ancillary information is set up for all our clinical teams that help with surgeries and procedures. This critical work means that every process is followed, and no important details are left out. “No one wakes up and says, ‘I want to have surgery;” our team goes above and beyond to make sure every single detail is taken care of so that when patients arrive, everything is in place,” said Trisha White. “Our team works hard to ensure everything runs as efficiently as possible because we want to use our resources in the best way possible to serve our patients without delays. We make sure we receive all the orders, codes and insurance and that the teams that follow after us – including our pre-admit team and nurses – have all the information they need to do their job seamlessly." With all the work they accomplish daily – not to mention how they wholeheartedly support each other through it all – it’s no question that the entire team has a lot to be proud of. Besides helping make patient care possible, the team puts their departmental merger and the move to fully remote work at the top of the list. “We’re most proud of merging the surgery scheduling and procedure scheduling teams together and therefore more cohesive,” said Mary Gray, Senior Scheduler. “The merger has made our team blossom and be able to connect with and rely on one another even more. We aren’t afraid to speak up and say something. At the end of the day, we’re here to take care of the patient, but we also help each other out. Our morale has gone up, and everybody is happier. Even though we all work remotely, we are more connected and have a great work-life balance.” “Along with transitioning the two teams into one big team, the move to being fully remote was huge," added Patricia Cruz-Hernandez, Surgical RN Scheduling Coordinator. “We worked through all the glitches, and it was a seamless transition to move into a remote setting. What’s great is that it did not affect patients at all; everything still gets done exactly as it should.” No matter how busy the days may get, Renown’s surgery and procedure schedulers always remember one thing: they are incredibly grateful for their fellow team members. “We have a very efficient and hard-working team of women,” said Pam Chapa Valencia, Senior Scheduler. “I could not have handpicked better people for our team,” added Trisha White. “I feel so lucky to have the team that we have.” A Renown “Why” Our Surgery and Procedure Scheduling team members all have diverse stories to tell about their road to Renown and why they’ve stayed in the department for as long as they have. Whether they’ve been with us for two years or two decades, they all share the same strong calling to care for their community. “I always wanted to help people, and my grandma was a nurse,” said Pam Chapa Valencia, Senior Scheduler. “I loved hearing her stories, and it made me want to be involved in patient care.” “I have a caring nature, and a hospital nature seemed like the right fit – I've been here for 25 years,” added Mary Gray. Several of our schedulers recognized the influence Renown has within our community and the ability to grow professionally and personally, both of which were a driving factor in their decision to make our health system their long-term career. “I’m originally from southern California, and I moved here about eight years ago; my husband always talked so positively about Renown, especially with how big it is and how it has the only level II trauma center in northern Nevada, so my goal was always to get a job here,” said Lydia Sharkey. “It’s been a great environment to be a part of.” “I’ve been with Renown for 17 years, and I chose to come here because of the reputation of the services Renown provided and care they gave,” added Trisha White. “I also knew what opportunities there were for me professionally, and in doing so, we are taking care of our community. I’ve had the chance to grow within my own professional skills and leadership skillset.” A profound feeling of ‘home’ is a common theme among this department. These team members appreciate the sense of community Renown has, the strides we’ve made in expanding our reach and how our health system gives healthcare professionals who are new to the field a chance to succeed. “At the time, Renown was the only hospital that would train nurses, and as a brand-new nurse, I had no experience – Renown took a chance on me,” said Patricia Cruz-Hernandez. “I feel like this is home. Our health system is so community-based and people-first minded, keeping ‘mission over margin.’ We’re growing, we’re expanding, we’re everywhere!” “I was a part of a transition as the cardiology private practice I worked with became a Renown practice, and it was great,” added Adrienne White. “This transition enabled us to provide more services and better care to patients. I stay here because I see the leaps and bounds we’ve been able to make in terms of procedures, accessibility and patient experience.” As true advocates for both patients and each other, the team is proud to have found their niche – and the ultimate beneficiaries? Everyone undergoing a surgery or procedure at Renown. A Culture of Kindness and Gratitude When you meet the Surgery & Procedure Scheduling team, you are greeted with warm smiles and an enthusiastic “Nice to meet you!” You can’t help but smile back and feel the infectious kindness they exude. Renown operates with a People-First mindset, a vision that this department especially takes to heart. They emulate the exact definition of our “Collaboration” cultural commitment. “We’ve built very good relationships and rapport with the OR managers and board runners,” said Lydia Sharkey. “The communication that we have at all three locations is very solid.” “The OR leadership is always so willing to help out whenever they can, and the resources they’ve provided have been huge for us,” added Adrienne White. “All the teams that see the patients after us – especially the surgical pre-admit team and the case managers, are fantastic about collaborating with us and reaching out to solve any issues they may have,” added Trisha White. “We all work so well together, especially since we all impact patient care.” In any organization, strong and compassionate leadership is key to a thriving team. Luckily for our surgery and procedure schedulers, they have Trisha White on their side. They attribute a lot of their success to having a supportive leader who “gets it.” “Trisha has been a scheduler like us, so she completely understands when we’re having an issue, because she’s struggled with the same thing and knows where we are coming from,” said Mary Gray. “It makes us feel like we are not alone – I can always reach out to her, or any of my other coworkers, to ask questions and figure out a solution together.” Despite being a remote-only team that meets in-person only one or two times a month, this group never misses an opportunity to reconnect both online and offline. They frequently shout out their Culture Ambassadors, schedulers Pam Chapa Valencia and Roxanne Abundis, for their team’s high morale. “Even though we all primarily work remotely, our in-person days are some of my favorite days of the month,” said Trisha White. “We feel so uplifted, we laugh and we have fun. We love being with each other. Pam and Roxanne are our Culture Ambassadors, and they both have been amazing at planning fun things for our teams. They go above and beyond to make our team feel cohesive and included.” “Pam and Roxanne have been leaders in creating a fun environment and supportive culture for us,” added Lydia Sharkey. “Whether it’s creating care packages or making sure we all have a good time when we see each other in person, they deserve a lot of credit.” As this team excels in their roles and foster a culture rooted in kindness and gratitude, we can trust that Renown’s surgeries and procedures will continue to thrive, and patients will continue to benefit from their diligent efforts and commitment to efficiency. “We make the magic happen!” closes Mary Gray.
Read More About Department Spotlight: Surgery & Procedure Scheduling
-
Por qué son tan importantes las inmunizaciones infantiles
Immunizations save thousands of lives each year by preventing serious illnesses, hospitalizations, and deaths. They also protect those who can't be vaccinated, like young children and the elderly, through herd immunity. Renown Pediatrician Dr. Kristin Wilson highlights the crucial role of vaccines. Immunizations Your Child Needs (and when) Birth to 6 Months Hepatitis B: Shortly after birth, first vaccine dose Diphtheria, Tetanus, and Pertussis (DTaP), Polio, Haemophilus Influenza (HiB), Pneumonia, Hepatitis B and Rotavirus: Ages 2, 4 and 6 months, boosters and vaccines One Year to 18 Months MMR and Varicella (chickenpox) vaccine: Age 1, first vaccine dose Hepatitis A, HiB and Pneumonia: Age 1, booster DTaP: 15 months, fourth vaccine dose Hepatitis, second dose: 18 months Flu Vaccine: 6 months and older, annually* *In the year after receiving their first dose, an infant will need a booster one month later. Four Years Old MMRV, DTaP and Polio, final dose: Four years of age Pre-Teen and Beyond Tdap and Meningitis: Before starting middle school, children receive these vaccines. They are also old enough to start the HPV vaccine, an essential vaccine for all young adults to protect against cancer, genital warts and cervical dysplasia.
Read More About Why Childhood Immunizations Are So Important
-
Lo que necesita saber sobre el ahogamiento por agua fría
Northern Nevada's stunning lakes, including Lake Tahoe, with its average summer water temperature of 50 degrees, present a potential risk of hypothermia. Unlike mild 50-degree air, water at the same temperature poses severe, life-threatening risks, including rapid-onset hypothermia and drowning. Awareness of the symptoms and taking proper precautions are crucial to prevent cold-water drowning. The 4 Phases of Cold-Water Drowning 1. Cold Shock Response: This response affects breathing and happens within the first minute. An automatic gasp reflex occurs in response to rapid skin cooling. If the head goes below water, water may be breathed into the lungs, resulting in drowning. A life jacket will help keep your head above water during this critical phase. Additionally, hyperventilation, like the gasp reflex, is a response to the cold and will subside. Panic will make this worse, so the key is to control breathing. 2. Cold Incapacitation: This response occurs within the first five to 15 minutes in cold water. In order to preserve core heat, vasoconstriction takes place decreasing blood flow to the extremities to protect the vital organs. The result is a loss of movement to hands, feet, arms and legs. Unless a life jacket is being worn, the ability to stay afloat is next to impossible. 3. Hypothermia: Important to note, it can take 30 minutes or more for most adults to become hypothermic. So there’s time to take action and survive. Keeping panic at bay is critical, as you have more survival time than you think. Symptoms include: Shivering Slow and shallow breathing Confusion Drowsiness or exhaustion Slurred speech Loss of coordination Weak pulse 4. Circum-rescue Collapse: This experience can happen just before rescue and is not well understood. Symptoms range anywhere from fainting to death. Some experts believe an abrupt drop in blood pressure may cause this final stage of cold water drowning, post-rescue. Additional Safety Tips and Helpful Resources Always wear a personal flotation device as well as a wetsuit or drysuit. Your personal flotation device is the most important piece of water safety gear. Try not to panic as the first phases will subside. Controlled breathing is to staying calm. Research suggests the body can withstand the cold longer than we think. The Heat Escape Lessening Posture (HELP) is a position which helps conserve energy if you’re wearing a personal flotation device. By hugging your knees to your chest, this posture helps maintain body heat for some time.
Read More About What You Need To Know About Cold Water Drowning
-
Departamento destacado: Procedimientos especiales
Chronic pain can be one of the most distressing feelings someone may encounter – and more likely than not, you know someone who is managing their pain as a part of their healthcare journey. In fact, according to the Centers for Disease Control and Prevention, about 1 in 5 U.S. adults have experienced chronic pain in recent years. One of the most common methods of treating pain is through prescription pain medications; however, with the rise of the opioid epidemic across the country, leveraging other interventions to help patients manage their chronic pain has become increasingly more important. What if there was a way to treat pain directly without the automatic need for pain medication? Luckily for patients in northern Nevada, our Special Procedures department at Renown Rehabilitation Hospital specializes in exactly that: interventional pain mitigation sans painkillers. With nearly 95% of their patients who come in with pain-related mobility issues being able to physically walk out of the hospital after their treatment, much-needed relief is clearly in store. Tight-knit and forever-caring, the Special Procedures team knows how to transform the purpose of pain management. A Penchant for Pain Alleviation Renown's Special Procedures team offers a wide variety of pain management solutions that are uniquely tailored to each individual patient’s needs. With the help of a team of 14 attentive nurses, interventional radiology technologists and a surgical technician – plus a dedicated patient access representative ensuring everything goes smoothly behind-the-scenes – these lifechanging interventions include: Epidurals (including steroid epidurals) Nerve blocks Ablations Tenotomies Spinal cord stimulator trials Peripheral nerve stimulator trials The nurses on this specialized team guide patients before, during and after their procedures, making sure they are at ease throughout the entire process. Each nurse emulates both expertise and empathy to help light the path towards healing. “Before each procedure, we get the patient’s vitals, health history and work with the doctor to answer any questions they may have about what is going to happen in the procedure room,” said Michon Edgington, RN. “After they’re all done, they come back to me, and I make sure they are ready to go home by educating them on their discharge. Our goal is to get them back to their families very quickly.” “In the actual procedure room, we perform safety checks, do charting, prepare the sterile tray for the doctor and give medication for conscious sedations, all while consistently monitoring the patient and helping the doctor out along the way to help the procedure go well,” added Shannon Boelow, RN. This team’s dedicated imaging professionals harness expertise that goes beyond capturing images. Their skillful utilization of X-ray technology serves as a guide for doctors administering treatments for pain – and according to our own physicians, our imaging technologists are some of the best in the business. “Our X-ray skills here are specialized,” said Julie Smith, Imaging Lead. “Visually, the doctor needs to see what’s going on inside the body so they can accurately place needles and steroids. We all work together collectively and work with each doctor to accommodate their preferences, helping the treatments go much faster and minimizing the patient’s exposure to radiation.” Serving as the ideal representation of both precision and support, the surgical technician on this team is an important collaborator in the procedure room, helping to ensure the success of every interventional procedure with a meticulous eye for detail. “As the Special Procedures surgical technician, I get the room ready with all the necessary instruments, including making sure everything is sterile,” said Carrie Crow, Surgical Technician. “I enjoy keeping the team organized.” Overseeing it all are the physicians, who are eternally grateful for the team for the life-changing interventions they offer every day. “Our physicians are so phenomenal,” said Brittney Summerfield, Manager of Nursing. “They are very supportive and collaborative, and they always do the right thing. They have total confidence in us.” Seeing patients walk out of the hospital happy and healthy is a driving motivator for this team. Whether they had significant experience in pain management or were ready for a completely new challenge, each team member comes to work every day inspired to move mountains. “I had worked in pain management in other facilities, and I was extremely excited to come here and solely focus on pain,” said Jodi Eldridge, Supervisor of Special Procedures. “I enjoy seeing the patients so happy when they leave no longer in pain. I feel immediate gratification, because you truly feel like you’re doing something big for the patient. It’s very rewarding.” “I decided to come work here because I worked in the inpatient setting for a long time, and I was ready to see a different side of healthcare and provide a different type of care to our community; plus, my coworkers are the best,” added Lisa Dunnivant, RN. There’s no question that the realm of pain management is a delicate one – and there is no team better suited to take on that challenge than Special Procedures, working harmoniously to bring relief and a renewed sense of livelihood for every patient they serve. “Some people believe pain management is just all about pills, and that is simply not true,” said Carrie Crow. “Our procedures are yet another way to help them manage their pain and find relief.”
-
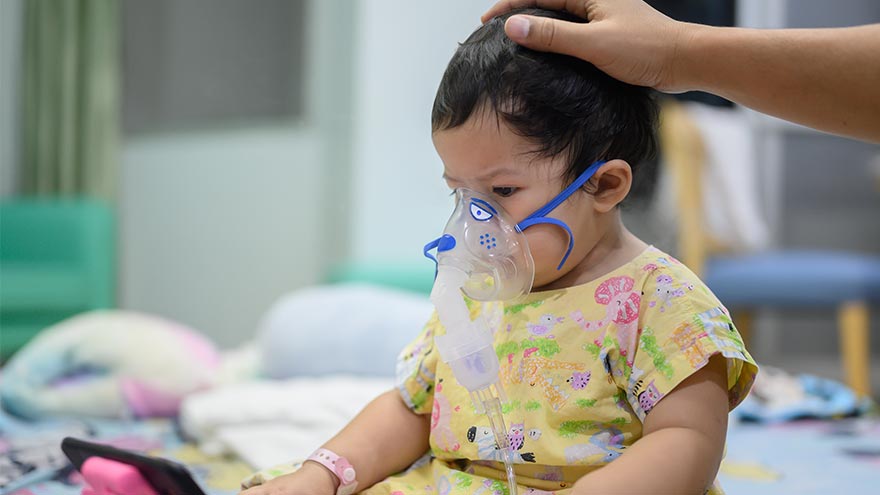
Lo que necesita saber sobre el VRS
Respiratory syncytial virus, also known as RSV, is a common respiratory virus that impacts the lungs and breathing pathways. The virus can be dangerous for infants and young children and is also concerning for older adults. While most older kids and adults only experience cold-like systems and recover in a week or two, an estimated 58,000-80,000 children younger than 5 years old are hospitalized due to RSV each year, and in 2022 healthcare organizations across the country are experiencing higher infection rates than in years past. "We are experiencing a strong RSV season and do not expect it to go away anytime soon," said Dr. Kris Wilson, Division Chief of Renown Children's Primary Care. "Infants who are infected with RSV almost always show symptoms of runny noses and cough. Call your healthcare provider immediately if your child is having difficulty breathing, is not drinking enough fluids, or is experiencing any worsening of these symptoms.” Symptoms of RSV: Runny nose Decrease in appetite/inability to drink Dry diapers, an indication of dehydration Cough, which may progress to wheezing or difficulty breathing Irritability (most common in very young infants) Decreased activity (most common in very young infants) Decreased appetite (most common in very young infants) Apnea, pauses in breathing for more than 10 seconds (most common in very young infants) What to do if you think your child has RSV: Call your pediatrician! If you suspect your child might have RSV, consulting their healthcare provider is the best first line of defense. From here they will help you build an appropriate treatment plan for child. Keep in mind that many pediatrician offices offer 24/7 call lines. If your child is experiencing retracted breathing (when the area between the ribs and in the neck sinks in when a person attempts to inhale), dehydration (not drinking and decrease in wet diapers) or apnea (pauses in breathing for more than 10 seconds) please call 911 or go to the closest emergency room.
-
Estrategias para una pérdida de peso duradera
Managing weight is a complicated and often difficult journey for many individuals, and obesity stands as a common and serious chronic health condition. In fact, the Center for Disease Control and Prevention reports that the prevalence of obesity in the US is greater than 40% in adults and 20% in children, and those numbers are continuing to climb. In Nevada, according to the 2020 Behavioral Risk Factor Surveillance System, 28.7% of adults reported being obese. By 2030, almost 80% of American adults may be overweight and half of them will be obese. But obesity isn't just about the numbers on the scale; it's a multifaceted, lifelong, neurobehavioral disease triggered by a combination of factors. These include abnormal eating patterns, reduced physical activity levels, environmental stressors, genetics and various other contributors. Obesity extends far beyond appearance, often leading to the development of numerous medical conditions such as diabetes, heart disease, elevated blood pressure, stroke, sleep apnea, liver disease, various cancers and infertility. Join us as we delve into the complexities of obesity and explore strategies for effective weight management available right here in northern Nevada. Why Can Losing Weight be so Difficult? The challenge behind weight loss finds its roots in the Set-Point Theory of Obesity, a concept that says our bodies have a predetermined weight, or fat mass, within a defined set-point range. In other words, when an individual's weight deviates from this set point, the body initiates mechanisms to bring it back to the established range. So, if someone loses weight below their set point, the body may respond by increasing hunger and reducing metabolism, making it challenging to sustain weight loss. There Isn’t One Right Answer, But Renown is Here to Help Various weight management strategies can be utilized by patients struggling with obesity, which may lead to substantial weight loss, resolution of associated medical conditions and improved psychosocial health. In fact, the most successful strategy involves a multidisciplinary approach under the guidance of trained specialists that includes a combination of tactics, including: Behavioral adaptations Dietary modifications Physical exercise Anti-obesity medications Weight loss surgery
-
6 Elementos de acción de atención médica para la comunidad LGBTQIA+
Every patient, regardless of how they may identify, greatly benefits from preventive healthcare and early detection. Members of the LGBTQIA+ community face unique considerations when it comes to their health, and a proactive approach to preventive screenings and vaccines is important in order to address their individual health needs. Dr. Karen Thiele, Family Medicine Physician with University Health and Assistant Professor of Family and Community Medicine at the University of Nevada, Reno School of Medicine, breaks down key steps that LGBTQIA+ patients should take to safeguard their health. PrEP and PEP Pre-exposure prophylaxis (PrEP) is a strategy to prevent human immunodeficiency virus (HIV) infection. It is an important measure for those who are HIV-negative but may be at risk of contracting it. The highest risk sexual practice is receptive anal intercourse, due to the relative fragility of rectal tissue. This medication can stop HIV from spreading in the body and help patients maintain their HIV-negative status. PrEP is available in both pill form, which is taken every day, and injection form, of which the first two injections are initiated one month after another while all other injections are initiated every two months. Post-exposure prophylaxis (PEP) is an antiretroviral drug regimen taken after potential HIV exposure to prevent an HIV-negative individual from converting to HIV-positive status. PEP is only for emergency situations and must be started within 72 hours of exposure – sooner is always better than later – and must be taken for 28 days. PrEP and PEP are available in many ways, including visiting your primary care provider (PCP) or an urgent care location. HPV Immunization All genders and identities can protect themselves against human papillomavirus (HPV), a sexually transmitted infection (STI) that can lead to the risk of cervical, mouth, head, neck, throat, anal, vaginal, penile and vulvar cancers. HPV is so common that nearly all sexually active people, regardless of sexual orientation and practices, will be exposed at some point in their lifetime. The HPV vaccine (common brands include Gardasil and Cervarix) is a safe and effective method to prevent HPV, according to the Centers for Disease Control and Prevention (CDC). This vaccine protects against infections that can lead to HPV-related cancers and precancers, as well as genital warts. While patients should start receiving the vaccine at 9 years old years old, unvaccinated adults up to the age of 45 can also receive the vaccine through their PCP – better late than never!
Read More About 6 Healthcare Action Items for the LGBTQIA+ Community