Buscar
-
El viaje de resiliencia de Tariq en Renown Rehab
Pictured above are members of the interdisciplinary team at Renown Rehabilitation Hospital, representing the diverse array of caregivers who supported Tariq's recovery journey. For Tariq Kuraishy and his wife Melissa, the focus is on his journey and getting back to life as he knew it rather than the stroke he experienced in June 2024, which led him to Renown Regional Medical Center and later to Renown Rehabilitation Hospital (otherwise known as “Renown Rehab”). From the swift assessment by first responders to the immediate treatment at Renown Emergency Room and the critical care received in Renown's Intensive Care Unit (ICU), Tariq’s journey has been marked by resilience and exceptional support beyond the couple’s expectations. Navigating the First Moments After Stroke Melissa shared how Tariq’s care team’s calm demeanor and expertise eased the initial shock of his diagnosis, treatment and plan of care. For Melissa, staying informed during crucial care discussions was vital. She noted that the team's professionalism and reassurance gave her the confidence to let go of some of the mental and emotional burden she felt during the immediate period after the stroke, allowing her to focus on both her and Tariq's physiological and emotional needs. “I felt very safe being at Renown, knowing that we were being cared for to the greatest extent,” said Melissa. Rising to His Personalized Rehabilitation Plan Tariq began the Renown Rehab program on June 19 with one goal in mind: to regain 70% of his brain function within 30 days. To achieve this, he spends four to five hours per day participating in physical, occupational, speech and recreational therapies as part of a comprehensive rehabilitation program tailored to his specific needs. If that sounds like a rigorous schedule, it's because it is, but Tariq prefers it that way because it means he’s actively working towards regaining his sense of normalcy with his care team alongside him every step of the way. “Unlike other places that might take a more lenient approach, the responsibility for progress not only lies with the Renown Rehab team but also the patient. If you are prepared to do the work, Renown Rehab is prepared to get you there,” Tariq said. Melissa emphasizes that Renown Rehab provides comprehensive, whole-person care with a variety of innovative, individualized therapies. These therapies keep patients engaged and busy throughout the day, addressing not just the affected areas but also the entire body and mind, ensuring holistic recovery and facilitating progress in unique ways. Activities like catching a ball or putting a ball in a hole help restore function, much like restoring power to a building that has lost electricity. It’s All About the Support and the Team’s Know-How From the moment he arrived, the Renown Rehab team has been continuously assessing Tariq’s abilities and tailoring his rehabilitation plan to propel him to the next level. Melissa, who spends up to 12 hours a day at the facility supporting her husband, highlighted the daily therapeutic sessions as an impressive way the care team evaluates Tariq’s readiness for more challenging tasks. Communication between the couple and Tariq’s team of doctors, nurses, therapists, techs and certified nursing assistants is constant as they actively involve them in decisions. As Tariq put it, they don’t cater to his comfort zone but instead push for progress, understanding it may not always be linear. It’s a true collaboration. “It doesn’t feel like it's being done to us but being done with us,” Melissa said. Looking Ahead Tariq and Melissa feel immensely fortunate to be at Renown Rehabilitation Hospital, which offers an exceptional blend of equipment, technology and expert care teams. “The Rehab facility is a treasure,” Tariq said. “Every member of the care team has displayed the utmost level of professionalism and expertise, and there hasn't been a single person who hasn't shown compassion and competence,” Melissa added. “I feel I will get the most out of being at Renown Rehab. I plan to take full advantage of the services and use every bit of the team’s talent, training and expertise. I will not leave anything on the table,” Tariq said. As Tariq continues to progress, he and Melissa are optimistic about the future. Tariq continues to receive physical, occupational and speech therapy at Renown Rehab. Their journey, marked by determination and strong support from Renown, offers hope to others facing similar challenges.
Read More About Tariqs Journey of Resilience at Renown Rehab
-
Cómo la dieta puede afectar el riesgo y la recuperación del cáncer
Cancer affects millions of lives worldwide. Though medical advancement has done a great deal to increase the human lifespan, proper nutrition has also been proven to help in the prevention of cancer. As researchers continue their hunt for a cure, there is a lot of information out there to support the argument that nutrition is an essential component in disease prevention and management. Nutrition Services: To learn more, call us at 775-982-4000 Linking Diet and Cancer Risk Evidence shows that our diets impact our vulnerability to cancer – and our ability to fight it. The American Cancer Society states that at least 18% of all cancers in the United States are related to excess body weight, physical inactivity, alcohol consumption, and/or poor nutrition. (American Cancer Society Guideline for Diet and Physical Activity | American Cancer Society). Sure, genetics can contribute, but research continues to support the belief that following a healthy diet can reduce the likelihood of developing cancer in the first place. Renown Health’s Jessica Blauenstein, MS, RDN, LDN, CSO, Registered Dietitian and Board-Certified Specialist in Oncology Nutrition confirms the importance of a nutritious diet consisting of: Fruits and Vegetables: Eating a variety of fruits and vegetables provides large amounts of vitamins, minerals and antioxidants. Nutrient-rich, they help in fighting off oxidative stress and inflammation, both of which are factors for developing cancer. Whole Grains: A diet rich in grains such as brown rice, quinoa and oats, contains substantial amounts of fiber that helps in digestion. A few studies have shown that whole grains might offer some protection against colorectal cancer. Lean Proteins: Reducing the amount of red and processed meats in the diet by substituting lean proteins, such as poultry, fish, beans and lentils may lower the risk of developing cancer. Red and processed meats have been associated with colorectal and other cancers when consumed in large amounts. Healthy Fats: Begin focusing on healthy fats from foods like avocados, nuts, seeds and olive oil. These fats are anti-inflammatory, which may play a beneficial role in disease prevention. Avoidance of Sugar and Processed Foods: Sugar and foods high in processed ingredients have been linked to an increased risk of obesity, type 2 diabetes and some cancers. It's important to limit the intake of sugary drinks, candy and snacks in the battle against cancer. A Role of Nutrition in Cancer Recovery Nutrition becomes even more critical for individuals who receive treatment and are in recovery. Treatments such as chemotherapy, radiation therapy and surgery can take a lot out of a body, affecting appetite, digestion and nutrient absorption. Proper nutrition during and after treatment can help: Support Immune Function: A good, balanced diet will provide the essential nutrients that support a resilient immune system, which is important in fighting off infections and supporting overall health during cancer treatment. Maintain Strength and Energy Levels: Proper caloric intake, protein and micronutrients prevent muscle wasting and fatigue, allowing patients to sustain their strength and energy. Address Side Effects: Certain foods and diets can help reduce or alleviate some common side effects associated with cancer treatment, including nausea, vomiting and mucositis. Eating small, frequent meals, maintaining good hydration, and avoiding spicy or acidic foods can all ease treatment-related discomfort associated with the GI tract. Facilitate Healing and Recovery: Nutrient-rich foods promote healing and the repair of tissues that may be damaged after surgery or other medical interventions. Foods high in proteins, vitamins and minerals play a significant role in repairing and replacing damaged tissues and cells. Correct Nutritional Deficiencies: Cancer and its treatment cause vitamin D, vitamin B12 and iron deficiencies in the diet. Nutrition therapy through a registered dietitian or nutritionist can identify those deficiencies and help manage them through dietary changes or supplementary means. Related information: Nourishing Your Loved One Through Cancer Treatment
Read More About How Diet Can Affect Cancer Risk and Recovery
-
Tazón saludable de verano
Say Hello to Summer in a Bowl If you've wanted to add a heart-healthy dish to your recipe repertoire, now's the time. This tasty vegan bowl loaded with turmeric chickpeas, marinated tofu and quinoa offers essential nutrients and beneficial fats to help maintain healthy cholesterol levels and reduce the risk of heart disease.
-
Por qué son tan importantes las inmunizaciones infantiles
Immunizations save thousands of lives each year by preventing serious illnesses, hospitalizations, and deaths. They also protect those who can't be vaccinated, like young children and the elderly, through herd immunity. Renown Pediatrician Dr. Kristin Wilson highlights the crucial role of vaccines. Immunizations Your Child Needs (and when) Birth to 6 Months Hepatitis B: Shortly after birth, first vaccine dose Diphtheria, Tetanus, and Pertussis (DTaP), Polio, Haemophilus Influenza (HiB), Pneumonia, Hepatitis B and Rotavirus: Ages 2, 4 and 6 months, boosters and vaccines One Year to 18 Months MMR and Varicella (chickenpox) vaccine: Age 1, first vaccine dose Hepatitis A, HiB and Pneumonia: Age 1, booster DTaP: 15 months, fourth vaccine dose Hepatitis, second dose: 18 months Flu Vaccine: 6 months and older, annually* *In the year after receiving their first dose, an infant will need a booster one month later. Four Years Old MMRV, DTaP and Polio, final dose: Four years of age Pre-Teen and Beyond Tdap and Meningitis: Before starting middle school, children receive these vaccines. They are also old enough to start the HPV vaccine, an essential vaccine for all young adults to protect against cancer, genital warts and cervical dysplasia.
Read More About Why Childhood Immunizations Are So Important
-
Motivar a los niños a comer alimentos saludables
Do you have a picky eater in your household? Or maybe you've got a snack monster who’s all about chips and candy? We're here to share a few fun strategies to motivate your little superheroes to snack on healthy foods instead! Rainbow Power-Up Eating a rainbow isn't just for unicorns! Different colors mean different powers: Red foods like strawberries and tomatoes help your heart. Orange foods like carrots and sweet potatoes help your eyes spot things like an eagle! Green foods like spinach and broccoli help you grow super strong bones. So, create a plate with as many colors as possible. The more colors, the more powers! Super Smoothies Blend your favorite fruits, such as bananas, berries and mangoes. Add some milk or yogurt and a handful of spinach. Your kids won't taste the spinach, and they'll drink a supercharged smoothie that gives them the energy to tackle any challenge. Create a Parfait Packed with Delicious Layers! Veggie Villans Who said veggies can't be fun? Turn them into heroes by giving them cool names and fun shapes. Make carrot sticks "Captain Crunch" or broccoli florets "Broc the Rock." Dip them in hummus or peanut butter for an extra flavor kick. Snack Attack Plates Create snack plates that are as fun as they are nutritious. Combine: Cheese cubes Grapes or apple slices Nuts or seeds Whole-grain crackers Mix and match these for your perfect plate! Make Your Own Trail Mix Fuel-Up Challenges Challenge your kids to eat three different healthy foods each day. Turn it into a family game to see who can eat the most colors or try the most fruits and veggies. You can even draw up a "super snacks" chart to keep track of your progress. Final Super Tip! Even superheroes have cheat days. Don't worry if your family doesn't eat healthy every meal. Just aim to eat more of the good stuff than the not-so-great stuff. Your kid's bodies will reward them with tremendous energy, focus and strength.
-
Prepare su propia mezcla de senderos: 4 Recetas rápidas y fáciles
Craving a crunchy, sweet, and nutritious snack? Try making your own trail mix! Perfect blends of nuts, dried fruits, and a touch of chocolate can be whipped up using bulk bin ingredients or pantry staples. Enjoy this delicious, healthy snack on a hike, at the office, or on your next road trip through Nevada's scenic deserts.
Read More About Make Your Own Trail Mix: 4 Quick and Easy Recipes
-
Nutrir a su ser querido a través del tratamiento contra el cáncer
Eating healthy is a daily challenge for many, but for those with cancer, it is an even harder struggle. A cancer diagnosis affects not only those diagnosed but family members and friends, too. One key area of concern is making sure your loved one stays well by eating healthy food every day. Here are some vital cancer nutrition tips from Jessica Blauenstein, a Board Certified Specialist in Oncology Nutrition and Registered Dietitian at Renown Health. Help to Prepare Meals and Snacks for Daily Cancer Nutrition Make it grab and go. Easy-to-make meals help reduce the burden of having to cook and prepare food. Having easy to grab snacks on the counter or in the fridge can help ensure your loved one has access to those nutrients when needed. Sit outside of the kitchen. This allows your loved one to avoid cooking smells which can make them feel sick as a side effect of cancer treatments. Also try serving them cold foods such as sandwiches, cheese and crackers, or shakes which have a mild scent. Try drinkable meals. Some people with cancer find it easier to sip their calories over the course of 30 minutes to an hour. Consider smoothies or supplemental shakes such as Ensure Complete, Fairlife shakes, Orgain shakes, or Boost Plus to name a few. A great foundation for a smoothie is a protein source (Greek yogurt, protein powder, nut butters or milk) with a carbohydrate (fruits, juice or berries). Add other ingredients as desired, such as spinach, kale, and ground flaxseed or chia seeds to give it more vitamins, minerals, and fiber. Snack Ideas for Those Undergoing Cancer Treatment The following ideas are both quick and easy to make for your loved one. Chicken or tuna salad with whole grain crackers or as a sandwich on whole grain bread Greek yogurt mixed with cereal, fruit and/or nuts Cottage cheese with banana, cinnamon and/or peanut butter Favorite fruit with 100% natural peanut or almond butter spread - Try peanut butter with bananas, apples, or even celery Their favorite veggies dipped in a salad dressing of your choice - For example, carrots with hummus, tahini, or ranch dressing Cheese and whole grain crackers - Add tomato slices with a small amount of avocado, and a dash of oregano on top for more flavor Eggs scrambled with cheese, vegetables and/or salsa Peanut butter and jelly sandwich on whole grain bread A baked sweet potato with some favorite toppings Hard boiled eggs and/or egg salad with whole grain crackers, or as a sandwich on whole grain bread Oatmeal or cream of wheat prepared with milk, fruit and/or nuts Sometimes your loved one may not feel like eating or refuse to eat. If treatment side effects are impacting your loved one’s ability to eat, please visit the websites below containing recipes tailored to treat side effects. Cook for Your Life ELLICSR Of course, you may also consult a registered dietitian and/or the patients care team, if you have more cancer nutrition concerns.
Read More About Nourishing Your Loved One Through Cancer Treatment
-
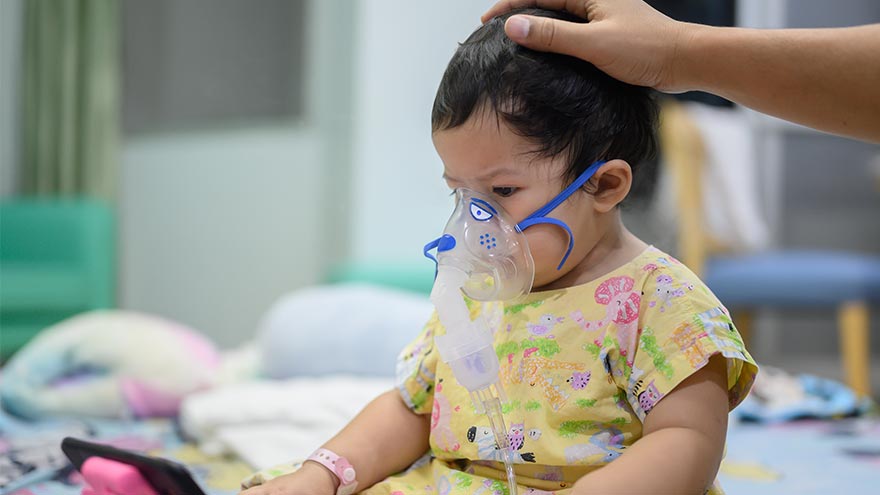
Lo que necesita saber sobre el VRS
Respiratory syncytial virus, also known as RSV, is a common respiratory virus that impacts the lungs and breathing pathways. The virus can be dangerous for infants and young children and is also concerning for older adults. While most older kids and adults only experience cold-like systems and recover in a week or two, an estimated 58,000-80,000 children younger than 5 years old are hospitalized due to RSV each year, and in 2022 healthcare organizations across the country are experiencing higher infection rates than in years past. "We are experiencing a strong RSV season and do not expect it to go away anytime soon," said Dr. Kris Wilson, Division Chief of Renown Children's Primary Care. "Infants who are infected with RSV almost always show symptoms of runny noses and cough. Call your healthcare provider immediately if your child is having difficulty breathing, is not drinking enough fluids, or is experiencing any worsening of these symptoms.” Symptoms of RSV: Runny nose Decrease in appetite/inability to drink Dry diapers, an indication of dehydration Cough, which may progress to wheezing or difficulty breathing Irritability (most common in very young infants) Decreased activity (most common in very young infants) Decreased appetite (most common in very young infants) Apnea, pauses in breathing for more than 10 seconds (most common in very young infants) What to do if you think your child has RSV: Call your pediatrician! If you suspect your child might have RSV, consulting their healthcare provider is the best first line of defense. From here they will help you build an appropriate treatment plan for child. Keep in mind that many pediatrician offices offer 24/7 call lines. If your child is experiencing retracted breathing (when the area between the ribs and in the neck sinks in when a person attempts to inhale), dehydration (not drinking and decrease in wet diapers) or apnea (pauses in breathing for more than 10 seconds) please call 911 or go to the closest emergency room.
-
Celebramos el equilibrio del azúcar en sangre esta temporada de fiestas
As the holiday season draws near, we find more reasons to celebrate with loved ones. At Renown Health, we are kicking off the celebrations early this November with American Diabetes Month. Approximately 37 million Americans, including 270,000 Nevadans, have been diagnosed with diabetes with as many as 95% of those diagnosed living with type 2 diabetes mellitus (T2DM). What is Type 2 Diabetes? Type 2 diabetes is a chronic health condition that occurs because your body is not using insulin (a hormone made by the pancreas to help cells use the food we eat for energy) as well as it should, resulting in high blood sugar levels. It is important to obtain a diagnosis for T2DM and ensure it is well-controlled to prevent serious health complications. Those with diabetes are at higher risk for blindness, kidney failure, heart disease, stroke and amputation. Tips for Supporting Your Health with Type 2 Diabetes Know Your Blood Sugar Levels: Work with your healthcare provider to establish target blood sugar levels, and make sure to monitor your levels regularly as advised by your healthcare provider to prevent or delay health complications associated with T2DM. Focus on Your Plate: Eating foods such as fruits and vegetables, lean meats or plant-based proteins, healthy fats and whole grains supports diabetes management. If choosing healthy foods is difficult due to your busy schedule, cost or simply because you aren’t sure where to start, talk with your healthcare provider who may refer you to a registered dietitian. Registered dietitian nutritionists are certified nutrition specialists who can provide education and practical tips for eating to support your T2DM diagnosis with visits covered by many insurance plans. Prioritize Staying Active: Engaging in regular exercise is good for everyone, especially those living with T2DM. Exercise helps your cells become more sensitive to insulin and therefore supports healthy blood sugar levels. Always check with your healthcare provider prior to beginning a new exercise plan. Support Stress Reduction: Stress is unavoidable but can be managed through regular exercise, getting enough quality sleep (7-8 uninterrupted hours per night) and practicing meditation and other mindfulness techniques. Plan Ahead for Holiday Gatherings: There’s still room for celebration while focusing on blood sugar management. Consider bringing a healthy dish to your gathering, focus on filling your plate with vegetable sides and eating those first and incorporate a family walk after dinner. If traveling, pack nutritious snacks that support your health and keep you full. Lastly, enjoy the special dishes and desserts this season has to offer in single-serving portions.
Read More About Celebrating Blood Sugar Balance This Holiday Season
-
6 Elementos de acción de atención médica para la comunidad LGBTQIA+
Every patient, regardless of how they may identify, greatly benefits from preventive healthcare and early detection. Members of the LGBTQIA+ community face unique considerations when it comes to their health, and a proactive approach to preventive screenings and vaccines is important in order to address their individual health needs. Dr. Karen Thiele, Family Medicine Physician with University Health and Assistant Professor of Family and Community Medicine at the University of Nevada, Reno School of Medicine, breaks down key steps that LGBTQIA+ patients should take to safeguard their health. PrEP and PEP Pre-exposure prophylaxis (PrEP) is a strategy to prevent human immunodeficiency virus (HIV) infection. It is an important measure for those who are HIV-negative but may be at risk of contracting it. The highest risk sexual practice is receptive anal intercourse, due to the relative fragility of rectal tissue. This medication can stop HIV from spreading in the body and help patients maintain their HIV-negative status. PrEP is available in both pill form, which is taken every day, and injection form, of which the first two injections are initiated one month after another while all other injections are initiated every two months. Post-exposure prophylaxis (PEP) is an antiretroviral drug regimen taken after potential HIV exposure to prevent an HIV-negative individual from converting to HIV-positive status. PEP is only for emergency situations and must be started within 72 hours of exposure – sooner is always better than later – and must be taken for 28 days. PrEP and PEP are available in many ways, including visiting your primary care provider (PCP) or an urgent care location. HPV Immunization All genders and identities can protect themselves against human papillomavirus (HPV), a sexually transmitted infection (STI) that can lead to the risk of cervical, mouth, head, neck, throat, anal, vaginal, penile and vulvar cancers. HPV is so common that nearly all sexually active people, regardless of sexual orientation and practices, will be exposed at some point in their lifetime. The HPV vaccine (common brands include Gardasil and Cervarix) is a safe and effective method to prevent HPV, according to the Centers for Disease Control and Prevention (CDC). This vaccine protects against infections that can lead to HPV-related cancers and precancers, as well as genital warts. While patients should start receiving the vaccine at 9 years old years old, unvaccinated adults up to the age of 45 can also receive the vaccine through their PCP – better late than never!
Read More About 6 Healthcare Action Items for the LGBTQIA+ Community
-
Enfermedad de Lyme: 3 Cosas que debe saber
Approximately 476,000 Americans are diagnosed and treated for Lyme disease every year. Lyme disease is an infection that is transmitted to humans through the bite of infected black-legged or “deer” tick. It’s the most common and fastest-growing vector-borne disease in the United States. This bacterial infection, if left untreated, can cause serious pain, fatigue and other crippling symptoms. Keeping an eye out for early signs of Lyme disease, implementing prevention techniques and understanding testing and treatment options can go a long way in maintaining your health. We consulted with Peter O’Reilly, PA-C at Renown Medical Group – South Carson to learn more. 1. Recognizing the Signs of Lyme Disease Lyme disease is extremely easy to misdiagnose, given that most of its early signs and symptoms mimic those of other conditions, such as COVID-19. Common Lyme Disease symptoms include: Fever Chills Joint or muscle pain Swollen glands Extreme fatigue Headache The primary initial symptom that occurs in about 80 percent of Lyme disease cases is a “bulls-eye” rash that spreads around the site of the tick bite – called “erythema migrans.” Tick bites can be hard to find and not everyone gets the classic bullseye rash, making Lyme disease difficult to self-diagnose. O’Reilly suggests talking to either your primary care doctor or infection doctor as soon as possible if you’re concerned about Lyme disease.
-
La prevención contra las ITS importa
According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new sexually transmitted infection (STI) cases in the United States each year, with rates continuing to increase. What you may not know is most STIs are preventable. We talked with Renown Adolescent Medicine Specialist, Caroline Barangan, MD to learn more about STIs. How Can You Get an STI? The CDC (Center for Disease Control) says that STIs are acquired through sexual contact. There are bacteria, viruses or parasites that can cause an STI which may pass from person to person in blood, semen, vaginal and other bodily fluids. How Do You Know if You Have an STI? STIs can have a range of signs and symptoms such as: Warts, bumps or sores on or near the penis, vagina, mouth or anus Swelling, redness or severe itching near the penis or vagina Discharge from the penis Vaginal bleeding that’s not your period Painful or uncomfortable sex Vaginal discharge that has an unpleasant odor, causes irritation or is a different color or amount than usual Weight loss, diarrhea or night sweats Aches, pains, fever and chills Jaundice (yellowing of the skin and whites of the eyes) Painful or frequent urination Sore throat if you engage in oral sex It’s important to know that the majority of people who have an STI commonly have no symptoms at all, which is why it’s important to get regularly tested once you have had any sexual activity. Young people less than 25 years of age should be screened on a yearly basis at minimum.