Buscar
-
How Regular Cervical Cancer Screenings Can Save Lives
According to the American Cancer Society, approximately 13,820 new cases of invasive cervical cancer will be diagnosed, and 4,360 women will die from cervical cancer. However, cervical cancer is preventable with regular screening tests and the HPV vaccine. It’s important to note that medical advances have allowed progress in diagnosing and treating cervical cancer. While it used to be one of the most common causes of cancer death for American women, the incidence of death has significantly declined. What to Know About the HPV Vaccine HPV vaccination is the best way to prevent cervical cancer and is recommended for all youth starting as early as age 9, or for teens and adults up to age 45 who didn’t start or finish the series. In Nevada, only 50.1% of teens ages 13-17 have been vaccinated for HPV. There are 13 types of HPV, and the vaccine Gardasil 9 protects against 9 of those HPV strains, greatly reducing the incidence of cervical cancer among vaccinated individuals. What to Know About Cervical Cancer Screenings The CDC says the most important thing you can do to help prevent cervical cancer is to have regular screening tests starting at age 21. And there are two common tests that can detect early stages of cervical cancer (or precancer) and improve health outcomes. The pap test (or pap smear). This screening looks for precancers. Women should begin getting pap smears when they’re 21. The human papillomavirus (HPV) test looks for the virus that can cause these cell changes. Cervical Cancer Screening Schedule The American Cancer Society offers the following guidelines for screenings: All women should begin cervical cancer screening at 21. Women between 21 and 29 should have a pap test every three years. Beginning at 30, the preferred way to screen is with a pap test combined with an HPV test every five years. This is called co-testing and should continue until age 65. A pap test (or pap smear) is performed during a regular screening appointment to look for precancers, cell changes on the cervix that might become cervical cancer if they are not evaluated or appropriately treated. Typically outpatient procedures can reduce the risk of long-term health impacts that prevent pre-cancerous cells from becoming cancer cells. Women over 65 who have had regular screenings in the previous ten years should stop cervical cancer screening as long as they haven’t had any severe precancers found in the last 20 years. How to Get Screened Request an appointment with your primary care physician or OBGYN to schedule a screening.
Read More About How Regular Cervical Cancer Screenings Can Save Lives
-
Departamento destacado: Oncología médica
The month of September recognizes several cancer-related health observances. Join us in celebrating our Medical Oncology team at Renown! No person ever wants to hear the words, “You have cancer.” Those three short yet impactful words immediately change the course of someone’s life. As these patients Fight the Good Fight against cancer, there are a lot of intimidating unknowns that can take over their minds. What happens next? What will my treatment be like? What is my prognosis? How will I be able to handle this physically and emotionally? What will it take for me to beat this? Who is better to be by their side than the devoted team members at the William N. Pennington Cancer Institute at Renown Health? From helping patients manage the process of complex paperwork and referrals to delivering personalized oncology and hematology treatment options tailored to each individual diagnosis, those fighting virtually any type of cancer are never alone, thanks to this team. The William N. Pennington Cancer Institute always lives up to that promise, guiding patients through the daunting journey of cancer treatment ahead, one step at a time. Courageous Against Cancer Our exceptional Medical Oncology department inherently understands that each moment in life is precious, especially for patients battling cancer. This team is dedicated to orchestrating the most comprehensive plan for each patient, seamlessly weaving together diagnoses and treatments, oral chemotherapy, medication management, clinical trials, radiation oncology and more. With the many patients they impact, there’s no question that there is never a dull moment in the day of the life of a healing hero like those in this department. “No day is the same in Medical Oncology,” said Hollyann Dehm, Registered Nurse. “As a nurse, we wear many hats in the clinic. Our role is to educate patients on their treatment plans and specific drugs they are receiving, triage symptom calls from patients, refill medications and implement our oral chemotherapy program. We help provide direct patient care by accessing ports, drawing labs and giving IV hydration when needed. We also help fill out family and medical leave (FMLA)/disability paperwork, help with physician orders, help obtain prior authorizations for prescribed medications and treatments.” “We do our best to let our patients know that they will not be going through this alone,” added Danielle Say, Physician Scheduling Coordinator. "We will be here for them every step of the way, guiding them and making sure their treatment is as smooth as possible and making ourselves available to them as much as we can. We end up getting to know many of our patients on a very close, personal level, and this helps to build that trust.” “Our day-to-day activities include seeing patients and helping to manage their therapies as well as their toxicities,” added Dr. Harry Menon, DO, Oncology Physician. “We work closely with our infusion room staff and have a robust team to help us deal with these complex patients. We also work very closely with our surgical and radiation oncology colleagues in a multidisciplinary fashion to provide comprehensive care for our patients.” The Medical Oncology team excels not only in providing cutting-edge cancer care but also in their compassionate approach to helping patients reduce the anxieties they understandably feel. Recognizing that a cancer diagnosis can be an emotionally overwhelming experience, this dedicated team combines medical expertise with unwavering support to create a healing environment. “When patients are referred to our department, a lot of them have many fears and questions,” said Heather Cortez, Medical Assistant. “A majority of what our team does is focused on the mental support that our patients require to help them have the most successful outcomes. One thing I have learned about cancer care is that positivity in the face of adversity is everything. Just being there to listen to our patient’s concerns can make all the difference. Helping them to navigate their many appointments and taking the time to explain things in a patient and compassionate way, is part of how our team serves this vulnerable population.” “The uncertainty is one of my patients' biggest fears: How far has my cancer progressed? How long will I have left? Is treatment even an option?” added Mary Wilson, Senior Medical Assistant. “The best advice that I can give my patients is that they are not alone. While this battle is going to be one of the hardest parts of their lives, they are surrounded by constant support to try and help with any burdens they may be facing. I also tell my patients that we have to take the little wins no matter how small they may be, because while cancer treatment is a physical battle, it is also a large mental battle." “While we don’t have answers to all the questions patients and their family members may have, we do our best to listen to their questions and concerns regarding their cancer diagnosis and treatment and guide them through their cancer journey," added Hollyann Dehm. “We provide emotional support and education on their type of cancer, managing their pain and side effects of their treatment. We also connect them to nurse navigators and our social worker who also help identify barriers to care and provide the patient with resources.” Whether it's explaining treatment options in understandable terms or offering emotional support through difficult moments, this department is committed to empowering patients on their journey toward healing. Their holistic approach not only treats the disease but also nurtures the spirit, all while being a strong advocate on each patient’s behalf. “Getting a cancer diagnosis can be the worst news that a person can hear; what we try to do is focus on improving quality life and focus on goals that help to promote quality of life,” said Dr. Harry Menon. “If the option for a cure is on the table, we try and focus on that goal in concert with promoting quality life. I try and have our patients focus on what they can control, with the understanding that even if some things are out of our control, the way we approach and manage those things, including our mindset, is still within our control.” “In our clinic, we truly value our patients and how they are cared for,” added Mary Wilson. “The amount of compassion our team shows is incredible. Patients constantly commend our team on how much they feel like the provider's care. Our providers and staff are not afraid to advocate for patients and that truly is an accomplishment in and of itself.” “We know patients are only hearing a small amount of the immense volume of information we provide them, so we encourage them to ask questions until it makes sense because the timeframe is different for every patient,” said Lillian Morton, APRN of Medical Oncology. “Cancer is an anxiety inducing lack of control whirlwind – if we can help by being responsive to patient calls and messages, we do so.” With their harmonious and integrated approach, each patient’s treatment journey progresses uninterrupted, bringing them closer to a brighter and healthier future.
-
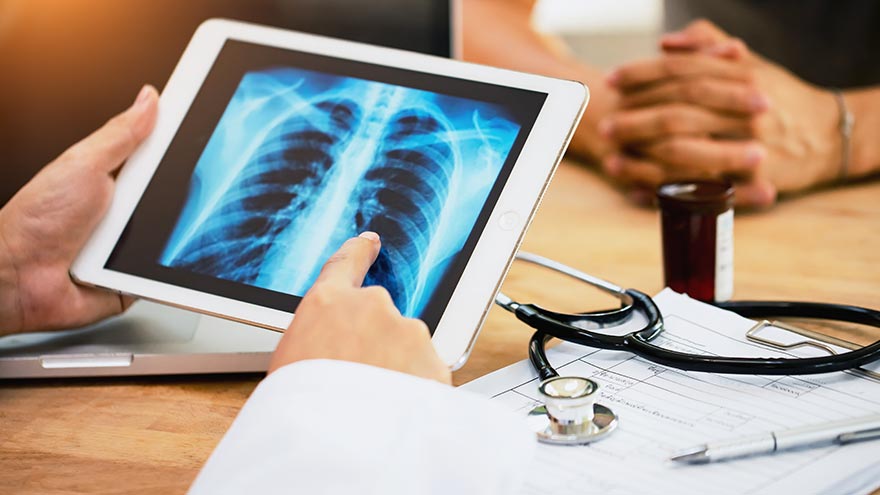
Lung Cancer Screening and Early Detection
Lung cancer is the leading cause of cancer deaths in both men and women in the U.S. The good news is the five-year survival rate increases dramatically if lung cancer is treated before spreading to other parts of the body. Julie Locken, MD, of Renown Health Imaging, explains more. What are the signs and symptoms of lung cancer? As you might expect, most lung cancer symptoms appear in the chest and can affect your breathing. Watch for signs such as: Persistent cough Constant chest pain Shortness of breath Wheezing Bloody or rust-colored phlegm Hoarseness Swelling of the neck Pain or weakness in the shoulder, arm or hand Recurring pneumonia, bronchitis or other lung infections Loss of appetite and loss of weight can also be signs of lung cancer That said, there are usually no symptoms in the early stages of lung cancer, which means getting screened can truly be a lifesaver. If you have a history of smoking, you should get screened as a precaution. What are the risk factors of lung cancer? Around 80% of lung cancer cases stem from a history of smoking tobacco. But there are other known causes, such as secondhand smoke, radon, asbestos and diesel exhaust. It’s important to do what you can to eliminate exposure to all of these to reduce your lung cancer risk. People with an immediate relative – a parent, sibling or child – diagnosed with lung cancer and people between 50 and 80 years old are also at higher risk and may need to consider screening. People who are at the highest risk are those with a history of smoking tobacco, particularly smokers who averaged one pack of cigarettes per day for 20 years or more, as well as former heavy smokers who quit in the last 15 years.
-
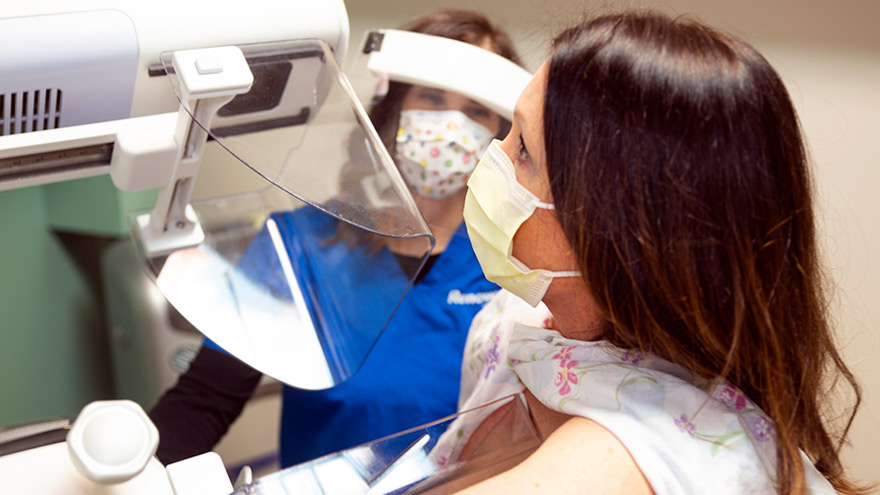
Ladies! Get Screened for Breast Cancer
Early detection is a significant piece of the breast cancer puzzle. Susan Cox, Renown Health Director of Cancer Operations, discusses what you need to watch for and how the latest technology can help detect potential cancer sooner. When should women start getting breast exams? It depends on risk factors: Average-risk women: Most medical organizations recommend the first mammogram between 40 and 44. Higher-risk women: Dependent on their high risk, which will dictate when they start screening, but generally around the age of 30 and not before 25 years old.
-
8 pruebas de evaluación de la salud importantes para hombres
Unfortunately, men are less likely to visit their doctor for exams, screenings, and consults than women. So with the help of Bonnie Ferrara, MD of Renown Health, we've put together a list of eight screenings to help men stay on top of their health game. 1. Blood Pressure Tests Ages 20+ Blood Pressure tests measure the pressure in your arteries as your heart pumps. Biennial (every two years) checks are recommended if you have normal blood pressure or more frequently if you have high blood pressure (hypertension) or low blood pressure (hypotension). The United States Preventative Services Taskforce cites normal blood pressure below 120 systolic (top number) and 80 diastolic (bottom number). 2. Cholesterol Screening Ages 20+ High levels of cholesterol increase your risk of stroke and heart disease. A simple blood test will help your healthcare provider determine your numbers and if you're at risk. If you have a family history of diabetes or heart disease, you may need yearly screenings. But, again, your doctor can provide the best course of action.
-
3D vs Whole Breast Ultrasound Which is Right for You
Breast cancer is the leading cause of cancer deaths in women in the U.S. That’s why early detection is so important. Dr. George Krakora, a radiologist with Renown Institute for Cancer, explains what to watch for and how new technology can lead to early detection. Most women know the importance of breast health and staying current with annual breast exams, but may not know that both screening guidelines and technology is evolving. So we asked George Krakora, MD, a radiologist for the Renown Institute for Cancer, what every woman should know about breast cancer detection and which screening method is right for them. First off, when should women start getting breast exams? Generally, women should start getting breast exams using mammography or ultrasound after they turn 40 years old. But we also want women ages 18 to 39 to talk to their primary care provider and ask for what’s called a formal risk assessment to see if screening is needed sooner. And you want to make sure your care provider is giving you a breast exam starting at age 25. It’s also a good idea to be familiar with how your breasts look and feel so you can report any changes to your care provider. What are the risk factors for breast cancer? Are there any preventive steps women can take? There a few risk factors you can’t control, like your age, family history of breast or other cancers, and if you have dense breast tissue. Your risk for breast cancer increases as you get older, and most breast cancers are diagnosed after age 50. Knowing your family history is important because a history of cancer and shared lifestyle can raise your risk. Your breast density can also increase your risk: Women with high breast density are four-to-five times more likely to get breast cancer than women with low breast density. But the good news is there are quite a few things you can do to prevent breast cancer, like not smoking, watching your alcohol intake, and maintaining a healthy weight with good diet and exercise. There are a lot of newer screenings out today. What is the difference between 2-D and 3-D mammography? In a 2-D mammogram, the tech takes X-rays of the breast. These pictures can show the radiologist if there are any lumps or tumors you might not be able to feel. In 3-D mammography, the process is largely the same but more X-rays are taken and it takes a few seconds longer for each image. This kind of exam detects 41 percent more cancers and reduces the number of false-positive results given to patients. This improvement in technology is great for both patients and their care providers. 3-D mammography provides better images of the breast, which allow doctors to more clearly diagnose and avoid false positives, especially in women with dense breast tissue. And what about a whole breast ultrasound. What is that? A whole breast ultrasound uses sound waves to detect cancerous tumors in the breast without using any radiation — it’s an ultrasound just like pregnant women get to check up on their baby. And the exam only takes about 20 minutes. We recommend these exams for patients whose mammograms have shown that they have dense breast tissue. Dense breast tissue can make it harder for doctors to see any abnormalities, lumps or tumors in a mammogram, so this technology ensures better early detection.
Read More About 3D vs Whole Breast Ultrasound Which is Right for You