Buscar
-
Ladies! Get Screened for Breast Cancer
Early detection is a significant piece of the breast cancer puzzle. Susan Cox, Renown Health Director of Cancer Operations, discusses what you need to watch for and how the latest technology can help detect potential cancer sooner. When should women start getting breast exams? It depends on risk factors: Average-risk women: Most medical organizations recommend the first mammogram between 40 and 44. Higher-risk women: Dependent on their high risk, which will dictate when they start screening, but generally around the age of 30 and not before 25 years old.
-
8 pruebas de evaluación de la salud importantes para hombres
Unfortunately, men are less likely to visit their doctor for exams, screenings, and consults than women. So with the help of Bonnie Ferrara, MD of Renown Health, we've put together a list of eight screenings to help men stay on top of their health game. 1. Blood Pressure Tests Ages 20+ Blood Pressure tests measure the pressure in your arteries as your heart pumps. Biennial (every two years) checks are recommended if you have normal blood pressure or more frequently if you have high blood pressure (hypertension) or low blood pressure (hypotension). The United States Preventative Services Taskforce cites normal blood pressure below 120 systolic (top number) and 80 diastolic (bottom number). 2. Cholesterol Screening Ages 20+ High levels of cholesterol increase your risk of stroke and heart disease. A simple blood test will help your healthcare provider determine your numbers and if you're at risk. If you have a family history of diabetes or heart disease, you may need yearly screenings. But, again, your doctor can provide the best course of action.
-
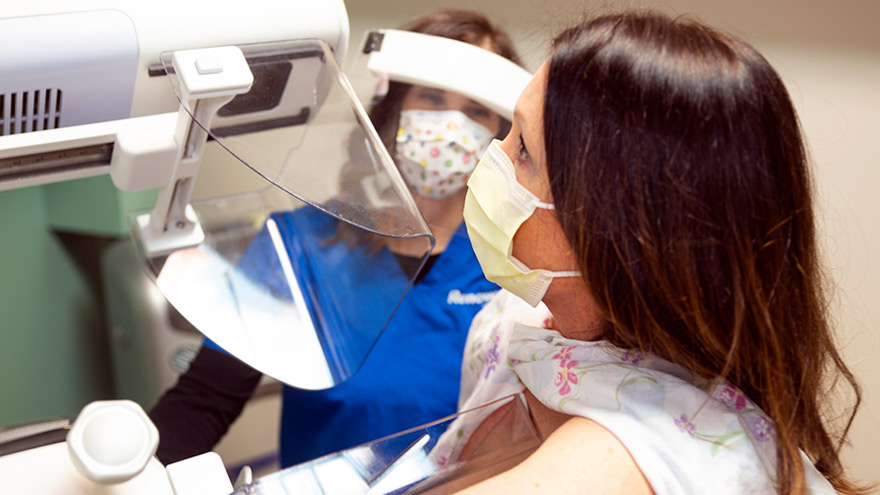
Why Your First Mammogram at 40 is a Vital Health Priority
A mammogram may not be on the top of your to-do list when you turn 40, but it needs to be. The American College of Obstetrics and Gynecology recommends a first mammogram at age 40, however you may need one earlier, so talk with your provider about your breast cancer risk. The purpose of a first time or baseline breast screening, is to get an accurate image of your breasts for future comparisons. Amber Snow, Supervisor of Renown Health Imaging, tells us why it’s important to get a baseline mammogram and what to expect during your visit. Mammogram Screenings Save Lives Simply put, a mammogram is a low-dose x-ray image of your breast from two views: top to bottom and side to side. A yearly screening reduces your risk of dying from breast cancer. Mammograms can detect signs of breast cancer even before you can see or feel it. That’s why it’s important to get a first- time mammogram. About 85% of breast cancers happen to those with no family history of it and in the U.S., one in eight women will develop breast cancer. Unfortunately, the two main risk factors for breast cancer: being female and aging. “Your baseline screening is important when you’re young, so that we know when changes occur,” explains Snow. “We compare your current mammogram to all your previous ones to know if anything changes year to year.” If you are under 40, talk to your provider about getting a formal risk assessment to see if a screening is right for you. If you have a family history of breast cancer a mammogram before age 40 or additional testing may be recommended for you. 3D Mammogram Technology Renown Health uses the latest 3D mammogram technology allowing our radiologists to see early changes in your breast tissue. This also reduces the number of false readings compared to traditional mammograms. While breast screening technology has improved, it is not uncommon to get called back after your first mammogram. According to the American Cancer Society, fewer than 10% of women called back for further testing have been found to have cancer. Reasons for being called back for further imaging include: Dense breast tissue, which can make it hard to see tumors A cyst, mass or unusual tissue is seen A possible area of concern needing another, closer look Preparing for Your Mammogram For an accurate image of your breasts do not wear deodorant, powders or lotions, as they can make it difficult to read your breast images. This is what will happen during your breast screening: A gown will be given to you and you will go to a private area to undress from the waist up, putting on the gown. You will then be escorted to the imaging room and a care team member will place one of your breasts between two plates. The plates will flatten to allow the most breast tissue to be seen and you will feel a firm pressure. You will be asked to hold your breath while the image is taken. An adjustment will be made to the plates to get a side view of the breast. The plate adjustments and images will be done on your other breast. Typically, a mammogram appointment is quick – only lasting about 15 minutes. Be Your Breast Friend While breast screenings are important, it’s also key that you know how your breasts normally look and feel. A monthly self-exam to check for lumps is essential, as breast cancers are often found during a routine self-exam. Remember your hormone levels change monthly, with your breast feeling tender and swollen right before your period. It’s best to perform a breast exam the week after your period after the swelling is gone. To avoid breast tenderness, this is also the best time for a mammogram.
Read More About Why Your First Mammogram at 40 is a Vital Health Priority
-
Sobreviviente del cáncer de ovario cuenta cómo decidió probar con ensayos clínicos
While there used to be three basic treatment options for cancer -- surgery, radiation and chemotherapy, or a combination of the three -- there's a fourth option: clinical trials. Here, a Renown patient shares her successful battle with ovarian cancer, aided by a clinical trial. Shari Flamm's battle with ovarian cancer began in 2011. She was experiencing prolonged bleeding, irregular thyroid levels and anemia and was scheduled to undergo a hysterectomy. Before the surgery, her gynecologist ran routine tests to check for cancer as a precautionary measure. All tests were negative for cancer, expect her CA 125 test. A CA 125 test measures the amount of the protein CA 125 (cancer antigen 125) in the blood. In some cases, a CA 125 test may be used to look for early signs of ovarian cancer in women with a very high risk of the disease. In most laboratories, the normal level is 0 to 35 units/ml. Flamm's CA 125 level was 121. As Flamm can attest, early diagnosis played a key role in her battle with ovarian cancer. September is Gynecologic Cancer and Ovarian Cancer Awareness Month – an important time to learn the signs, symptoms and risk factors of this type of cancer so your doctor can diagnosis the disease as early as possible. Ovarian Cancer: Round One Despite the elevated CA 125 results, her doctor recommended they move forward with the hysterectomy. But when surgery began, doctors discovered a mass. She had stage 4 cancer. The procedure was halted, the mass was biopsied and she was immediately seen by Dr. Peter Lim of the The Center of Hope. Following diagnosis, Flamm underwent surgery with Dr. Lim to remove the cancer, which had spread to part of diaphragm, spleen, colon and other organs. Three months after surgery, Flamm had recovered enough to start six rounds of chemotherapy in her hometown of Carson City. She continued working at a doctor's office during her treatment, and was grateful for Dr. Lim’s ability to co-manage her care so she could stay close to work and family. “To me, chemo was the scariest part because I didn’t like feeling sick,” Flamm says. Thankfully, her body responded well to the treatments and she was back to the things she loved. “I stated working out at the gym, even if it was only for 10 minutes,” she says. She also stayed positive by spending time with her grandchildren, attending a San Jose Sharks hockey game, going for walks and enjoying concerts. Ovarian Cancer: Round Two In November 2014, Flamm had a cancer check-up. That’s when doctors discovered three cancerous tumors. For this round, Flamm choose another treatment option -- clinical trials at Renown Institute for Cancer. Clinical trials are the studies that test whether drugs work, and inform doctors' decisions about how to treat their patients. Flamm participated in a clinical trial that featured oral-targeted therapy stronger than IV chemotherapy. The hope was for the drug to shrink her tumors, however the result was stabilization -- meaning the lumps weren’t growing or spreading. The best part of the clinical trial, Flamm says, was the constant monitoring. Between the CT scans every six weeks, a heart scan every three months and monthly doctor visits, she was confident that if the cancer started growing or spreading, her healthcare team would catch it right away. For Flamm, the benefits of the clinical trial included less hair loss, less fatigue and more time to focus on what’s important in her life -- her family. “I decided I wasn’t going to be that sick grandma on the couch with cancer,” Flamm says. After taking the oral medication for one year, Flamm developed a rash and discontinued treatment due to discomfort. Clinical Trials, Setbacks and Survival In June 2016, two of the three tumors began to grow and had to be surgically removed. Despite the setback, Flamm was determined to maintain a positive outlook. "You have to stay positive because cancer feeds off anger, depression and stress," Flamm says. Flamm was released to go home with clear margins, meaning the tumors were removed and are surrounded by a rim of normal tissue that does not have cancerous cells. Flamm says her outlook on life has changed drastically since her first cancer diagnosis. “Your whole mentality changes when cancer disturbs your life," Flann says. "The things that weren’t important, are now ever so important. I’m a lot calmer now,” Flamm says.
Read More About Ovarian Cancer Survivor Shares Decision to Try Clinical Trial
-
3D vs Whole Breast Ultrasound Which is Right for You
Breast cancer is the leading cause of cancer deaths in women in the U.S. That’s why early detection is so important. Dr. George Krakora, a radiologist with Renown Institute for Cancer, explains what to watch for and how new technology can lead to early detection. Most women know the importance of breast health and staying current with annual breast exams, but may not know that both screening guidelines and technology is evolving. So we asked George Krakora, MD, a radiologist for the Renown Institute for Cancer, what every woman should know about breast cancer detection and which screening method is right for them. First off, when should women start getting breast exams? Generally, women should start getting breast exams using mammography or ultrasound after they turn 40 years old. But we also want women ages 18 to 39 to talk to their primary care provider and ask for what’s called a formal risk assessment to see if screening is needed sooner. And you want to make sure your care provider is giving you a breast exam starting at age 25. It’s also a good idea to be familiar with how your breasts look and feel so you can report any changes to your care provider. What are the risk factors for breast cancer? Are there any preventive steps women can take? There a few risk factors you can’t control, like your age, family history of breast or other cancers, and if you have dense breast tissue. Your risk for breast cancer increases as you get older, and most breast cancers are diagnosed after age 50. Knowing your family history is important because a history of cancer and shared lifestyle can raise your risk. Your breast density can also increase your risk: Women with high breast density are four-to-five times more likely to get breast cancer than women with low breast density. But the good news is there are quite a few things you can do to prevent breast cancer, like not smoking, watching your alcohol intake, and maintaining a healthy weight with good diet and exercise. There are a lot of newer screenings out today. What is the difference between 2-D and 3-D mammography? In a 2-D mammogram, the tech takes X-rays of the breast. These pictures can show the radiologist if there are any lumps or tumors you might not be able to feel. In 3-D mammography, the process is largely the same but more X-rays are taken and it takes a few seconds longer for each image. This kind of exam detects 41 percent more cancers and reduces the number of false-positive results given to patients. This improvement in technology is great for both patients and their care providers. 3-D mammography provides better images of the breast, which allow doctors to more clearly diagnose and avoid false positives, especially in women with dense breast tissue. And what about a whole breast ultrasound. What is that? A whole breast ultrasound uses sound waves to detect cancerous tumors in the breast without using any radiation — it’s an ultrasound just like pregnant women get to check up on their baby. And the exam only takes about 20 minutes. We recommend these exams for patients whose mammograms have shown that they have dense breast tissue. Dense breast tissue can make it harder for doctors to see any abnormalities, lumps or tumors in a mammogram, so this technology ensures better early detection.
Read More About 3D vs Whole Breast Ultrasound Which is Right for You