Buscar
-
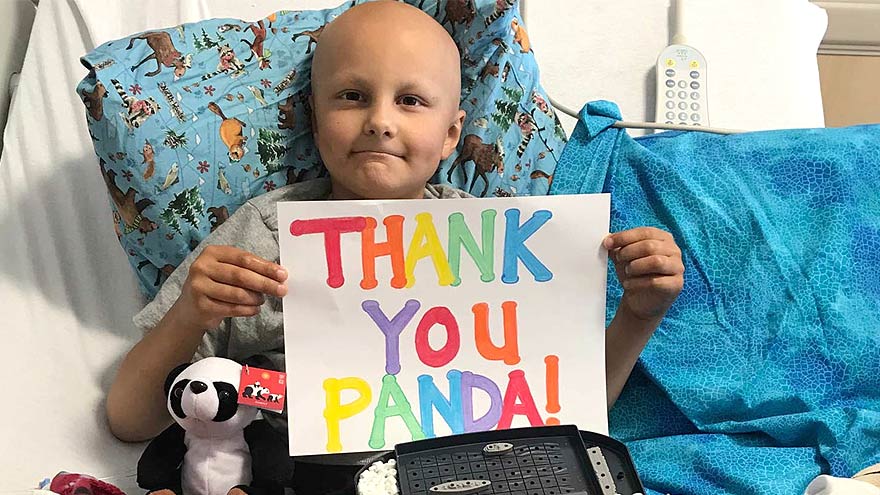
Panda Cares Center of Hope at Renown Children's Hospital
When you have an ill child in the hospital, it is a stressful event. And Panda Express is helping local families support children who need special care. Their generous donation provides much-needed equipment, programs, and resources via the new Panda Cares Center of Hope, Renown Children’s Specialty Center. Their partnership directly benefits patients and their families! The ‘Panda Cares Center of Hope, Renown’s Children’s Specialty Center’ In fact, this new center provides care to not only children, but also comprehensive support to the entire family. Similarly, it creates an environment that reduces stress, promotes healing, and provides a superior patient and family experience. This facility upholds Panda Express’ mission, vision, and values and its four pillars: to directly help fund the emotional, mental, physical, and spiritual needs of children. This center, the first-ever in northern Nevada, will provide care for children who have chronic conditions. In particular, it offers ongoing treatment, health management, and specialty medical services, including: Nephrology Endocrinology Neurology Pulmonary Infectious Diseases Medical Genetics Adolescent Medicine How You Can Help! When you order from Panda Express, you can opt to round up your change, which will help support programs and services, such as the Center of Hope for Renown Children’s Hospital. Order Online A Partnership for Health & Education of Underserved Youth This partnership allows Renown Children’s Hospital to continue to strengthen regional services and increase Panda’s visibility within our growing community. Last year, 21,930 sick children received care from Renown Children’s Hospital. To date, Panda Express has raised $449,200 in financial support to assist us in providing health and education to every child, regardless of illness, injury, insurance, or ability to pay. Panda Express funds have already supported: Giraffe omni beds for the NICU Ultrasound machine for the Children’s ER Panda warmers and a hand held Accuvein machine Child Life Program to support sick patients and families Meeting room in the Children’s Specialty Center In kind donations, volunteer time and support of local events such as the University of Nevada Reno, Wolf Pack Dance Marathon
Read More About Panda Cares Center of Hope at Renown Children's Hospital
-
Stay Inside When Skies Are Smoky
Even when fires burn outside our area, the air quality in the region can reach dangerous levels. Our expert explains how to maintain your lung health when fire season strikes. It’s a sight we know all too well as northern Nevadans — a hazy or thick layer on the horizon when smoke rolls in from nearby fires. Sometimes the smoke is more evident than others, but it’s important to remember, even when the smoke may not be as visible across the valley, it still impacts our air quality. The last week or so, our air quality has been in the “unhealthy for sensitive groups” range, which can be dangerous for people who are sensitive to air pollution. Air Quality Changes: Who’s at Risk? Renown Pediatric Pulmonologist Sonia Budhecha, M.D., explains certain people are especially at risk when smoke moves in: Older people, whose lungs are not as healthy as they used to be Young children, whose lungs are still developing People with heart and lung disease including asthma, COPD and emphysema “Smoke and haze from fires carry particulates that can get into your respiratory system and eyes, which can be a danger for all ages,” Dr. Budhecha says. How You Can Protect Yourself Until the smoke clears and the air returns to the “good” range, it is best to follow these tips to protect yourself and your family: Stay indoors and keep windows closed Turn on the air conditioning to recirculate clean air Drink plenty of fluids to help your body flush out any toxins you inhale Additionally, all community members should reduce their physical activity and try to prevent heavy exertion outside. If you or a loved one has a heart or lung disease, avoid physical exertion altogether because smoke can aggravate these conditions. “People with heart disease may experience shortness of breath, chest pain, palpitations or fatigue,” Dr. Budhecha says. “People with lung disease may also have shortness of breath, chest discomfort, wheezing, phlegm or a cough.” Smoky Signs and Symptoms Smoke can also impact healthy people — irritating your eyes, nose or throat. And in some cases, inhaling smoke can lead to bronchitis. When haze moves into our area, keep an eye out for these symptoms: Burning or stinging eyes Runny nose Cough or scratchy throat Headaches Wheezing Shortness of breath Difficult taking a full breath Chest heaviness Lightheadedness Dizziness If experiencing any of the above symptoms, seek medical attention or call your doctor for advice. Sometimes, these symptoms do not appear for as long as 24 to 48 hours after smoke inhalation. For those that have pre-existing lung or heart conditions, consult with a health care provider on action or management plans. To schedule an appointment Visit Renown Pulmonary Medicine, or call 775-982-5000. Understanding Our Air Quality The Air Quality Index (AQI) is broken down by large (PM10) and small (PM2.5) particulates. According to Dr. Budhecha, large particulates are usually ones that can be seen and smelled. They can damage your eyes and nose but don’t often get deep in the lungs or blood vessels. “The more dangerous ones are PM2.5, which can’t always be seen or smelled,” Dr. Budhecha says. “Any time the AQI is above 51, children with lung or heart disease should not be outdoors.” For the latest air quality update in your area, visit AirNow.gov or call (775) 785-4110.
-
How to Safely Give Children Over-the-Counter Medications
How can you ensure you’re giving your children safe doses of over-the-counter medications? The safest bet: Confirming dosages and recommendations with your doctor. With that in mind, here are a few answers to basic questions about OTC medications and children. It’s cold and flu season in Northern Nevada. This means you’ll find parents in the aisles of practically every drug store, wondering what will and will not work for their sick children. Over-the-counter (OTC) medications — and their dosages, side effects, interactions and more — can inspire abundant anxiety for parents. At the outset, the U.S. Food and Drug Administration offers the following warning about use of medicines for cough and colds in children: The FDA doesn’t recommend over-the-counter medicines for cough and cold symptoms in children younger than 2 years old. Prescription cough medicines containing codeine or hydrocodone are not indicated for use in children younger than 18 years old. Codeine and hydrocodone are opioids that are available in combination with other medicines, such as antihistamines and decongestants, in prescription medicines to treat cough and symptoms associated with allergies or the common cold for adults. Caregivers should also read labels on OTC cough and cold products, because some might contain codeine. So how can you feel comfortable administering any OTC medication to your children? The short answer is: Check with a doctor first. And with that in mind, here are a few common questions and answers from Kristin L. Wilson, MD, of Renown Pediatrics about children and OTC medications. Please talk about the importance of correct dosage of pediatric medications. Pediatric dosing is weight-based and unique to each medicine (and sometimes even the circumstance you are treating.) Therefore, there are no standardizations of “safe” amounts that apply to all medications. What are signs of an overdose of pediatric medications? Signs of intoxication/overdose are also unique to each medication and supplement. And to make it more confusing, mixing current prescriptions with various supplements or over-the-counter medications can cause significant adverse effects as well. Is there an age at which children take adult over-the-counter medications? Infants through adolescents can take medications that are also prescribed to adults, but only under a healthcare provider’s careful guidance. Dosing is determined by various factors dependent on child’s age and also medical history, as above. What is the takeaway about administering medications to children? When in doubt, ask a healthcare professional whether a medication or supplement is safe for your child based on his/her age and medical history as well as recommended dosing based on recent weights and other vital signs.
Read More About How to Safely Give Children Over-the-Counter Medications
-
Cómo aliviar el miedo de su hijo a las vacunas
Getting a shot can be scary for kids and anxiety-inducing for parents and caregivers. With flu shot season well underway and children's COVID-19 vaccine clinics in full swing, we wanted to share ways to reduce the stress for you and your child. Plan Ahead and Be Honest A few days before the scheduled appointment, casually mention to your child that you’re both going to the doctor’s office (or vaccine clinic, or pharmacy) soon for their vaccine. Explain to them that this will help protect them and will only take a second. Being honest is important, telling your child that it will hurt for a moment. If possible, try and schedule the vaccine at a kid-specific vaccine clinic, your pediatrician's office or a school-based site. Remember that words are powerful. Take notice if you are using a word that might make them more upset, such as prick, jab, needle or shot. You can interchange words such as vaccine, immunization or injection. Bring Toys Don’t be afraid to let your child bring one of their favorite toys or stuffed animals to the appointment. This can make them feel more comfortable and provide distraction. Ask for Pain Reliever/Numbing Agent If you know from past experience (or suspect) that your child has a needle phobia, talk to the vaccination location ahead of time and ask if they can use a pain reliever or numbing agent before administering the vaccine. Distract. Distract. Distract. Sing a song, tell them a joke, make a funny face. If you can pull your child’s attention away from the needle and make them laugh, they won’t focus all their energy on worrying about the shot. Lead By Example If you haven't gotten your flu shot, COVID shot or COVID-19 booster yet, ask the facility ahead of time if you can also get a shot before your child. Show them that the shot is no big deal and that they will have no problem getting it themselves. Celebrate Don’t be afraid to celebrate this victory with your child once it is over – bring them to the park, go out for an ice cream cone, let them pick what’s for dinner. This reward will show that you’re proud of them for being brave and may also make the next time your child is due for a shot easier.
-
5 consejos sencillos para el cuidado de la piel en invierno
Winter skin alert – cold temperatures can put your skin into chaos. We asked for skin tips from Heidi Nicol, an esthetician with Renown Dermatology, Laser & Skin Care. She shares how to keep your skin glowing through the frosty months ahead. 1. Re-think your shower Few things feel better on a cold day than a long, hot shower. But hot showers can lead to dry skin because they strip your skin of its natural protective oils. Avoiding them altogether is best – choose a lukewarm, or warm, shower instead. If you have an occasional hot shower, the American Academy of Dermatology (AAD) suggests keeping it at five to ten minutes. Nicol recommends using a gentle cleanser and avoid using too much. Moisturizing after a shower or bath while your skin is still damp is also a must. Slathering on your favorite lotion helps your skin hold on to precious moisture. 2. Stay away from smoke and fire Although sitting close to a roaring fireplace can feel good, it is drying to your skin. Smoking and exposure to smoke also harms your skin. Smoking reduces healthy blood flow to the skin. This also causes your skin to wrinkle faster, making you looker older. Additionally your skin heals much slower if you smoke. 3. Consider a humidifier Cranking up the thermostat dries out indoor air. Skin is our largest organ, and in general, heat is very drying to your skin. To clarify, over time dry air degrades your skin’s natural moisture (lipid) barrier leading to flaking, peeling and cracking. Your skin can overcompensate for the dryness by producing even more oil. In other words it is possible for your skin to be both oily and dehydrated at the same time. Even oily skin needs a daily lightweight, non-pore clogging moisturizer. 4. Use SPF daily The sun’s rays damage your skin even on cloudy days. Sunlight contains UVB (burning) and UVA (aging) rays. Although UVB rays are less strong in the winter, the UVA rays are same strength all year. And snow can reflect almost 90% of UV radiation. With this in mind make sure you have suitable skin and eye protection when going outdoors. 5. Take care of your hands and feet Don't forget your fingers and toes when moisturizing. These areas tend to be drier than other parts of the body. Gloves help to protect hands from winter weather and lock in moisture. Similarly, putting lotion on your feet before your socks will keep them your skin from flaking and cracking. Follow the tips above to make sure your skin is at its best, despite the winter weather.
-
Llevando la atención pediátrica cerca de casa
As our community grows, so does the need for specialized care. Thanks to a generous gift, there’s a healthier future for families in the region as a $7.5 million gift to the Renown Health Foundation is helping keep care close to home. Being in the hospital is often a stressful experience, especially for a child and their caregivers. If you add the need to travel out-of-state for care into the mix, unnecessary anxiety and financial burdens can be placed on a family that is already worried about a sick child. With our quickly growing community and close to 100,000 children under the age of 18 in Washoe County alone, the need for local specialty care is needed. The William N. Pennington Foundation recognized this need and donated $7.5 million to the Renown Health Foundation – the largest gift the health system has received – to keep care close to home and establish the William N. Pennington Fund for Advanced Pediatric Care. Thanks to this gift, Renown Children’s Hospital has hired more than 15 pediatric specialists who provide care for children in our community. Below, we introduce you to three key specialized pediatricians in northern Nevada: Joseph A. Gassen, M.D. “Having pediatric specialists in the community is invaluable,” says Joseph A. Gassen, M.D., pediatric emergency medicine. “It allows families and patients to stay in Reno and not have to travel far distances to get quality care.” Gassen, the only doctor specializing in pediatric emergency medicine in the region, moved to Reno to provide care in the emergency room at Renown Children’s Hospital. “The hospital is dedicated to improving the care of children in northern Nevada, and I wanted to be a part of this amazing vision," Dr. Gassen says. I would not have been able to relocate to Reno without the support from the hospital and the William N. Pennington gift.” Working with children and their families are what Dr. Gassen finds most rewarding. "I get to provide care for a child, which in turn makes the parent feel better,” he says. “Essentially, I get to treat the whole family, even though I only directly care for the kids.” Colin Nguyen, M.D. Also among the first new specialists is Pediatric Neurologist Colin Nguyen, M.D., who has done extensive work with epilepsy and epilepsy surgery. “In any growing and expanding community, we need the multitude of social, financial, political and well-being services to sustain that growth and progress,” Dr. Nguyen says. “The ability to offer more breadth of medical services to our local population allows families to spend more time together and fulfill work obligations, without the need to travel long distances to obtain that specialized care.” Dr. Nguyen says he enjoys caring for children because they are honest in their emotions and reactions, as well as simple in their intentions. “It is the overall joy and unique sadness that comes in working with children, which drives many of us to continue our work -- I am no exception.” Jacob Zucker, M.D. The third pediatric specialist providing care thanks to the Pennington gift has close ties to northern Nevada. Jacob Zucker, M.D., pediatric hematologist-oncologist, was born and raised in Reno and attended medical school at the University of Nevada, Reno School of Medicine before moving to the Midwest for his residency and fellowship. Dr. Zucker feels fortunate to have been offered the opportunity to return home and give back to the community that has given so much to him. “I can say with absolute resolve that northern Nevada is an exceptional community to practice medicine in. The care offered here at home is top rate and the providers that live and practice here truly understand the purpose of community.” The addition of these three specialists and the future specialists that will be coming to our area will impact thousands of children and their families. “With a growing population, the vision of leadership at Renown, and with the generosity of the William N. Pennington Foundation, northern Nevada is in position for the first time to make local pediatric subspecialty care a reality and to keep our families at home in their community,” Dr. Zucker says.
-
What Is the Role of a Child Life Specialist?
What is the role of the child life specialist? Here are common questions and answers about how these special individuals give both parents and kids peace of mind. Let’s face it: A hospital can be an intimidating place for just about anyone. But add in being a small human with very little worldly experience — aka a child — and it’s easy to imagine how overwhelming a hospital visit can be. Enter the role of the child life specialist. Liz Winkler, a child life specialist with Renown Children’s Hospital, explains how a Renown program puts young patients and their families at ease. What does a child life specialist do? Child life specialists help young patients develop ways to cope with the anxiety, fear and separation that often accompany the hospital experience. They give special consideration to each child’s family, culture and stage of development. As professionals trained to work with children in medical settings, specialists hold a bachelor’s or master’s degree in the areas of child life, child development and special education or recreational therapy. Our child life specialists are also professionally certified and affiliated with the national Child Life Council. Child life specialists also offer tours of Renown Children’s Hospital for families whose children are scheduled to have surgery. Child life supports children and families by: Helping children cope with anxiety, fear, separation and adjustment Making doctors, needles and tests a little less scary Providing art, music and pet therapy Organizing activities Addressing your concerns Telling you what to expect Creating a therapeutic and medical plan Offering a hand to hold What else is available at the Children’s Hospital that helps ease some of the stress of a hospital visit? Whether it’s seeing a pediatrician, getting a sports physical or looking for advice, our care is centered on supporting and nurturing patients and families at our many locations. We have kid-friendly environments to help ease some of the stress of a hospital visit. These include colorful exam rooms, kid-friendly waiting and common areas, and medical equipment designed especially for children. Our children’s ER is open 24 hours a day, seven days a week. So parents and caregivers have access to emergency care tailored to little ones — anytime, day or night. We have several pediatric specialists on the Renown team in areas including diabetes, emergency medicine, neurology, pulmonology, blood diseases and cancer. How can parents start to ease their children’s mind when they know a hospital visit is in the future? As with many things in life, good preparation can help kids feel less anxious about the experience and even get through recovery faster. It’s important to provide information at your child’s level of understanding, while correcting any misunderstandings, and helping to eliminate fears and feelings of guilt. If you’re anxious and nervous, your child may reflect these feelings and behaviors. So make sure you educate yourself, feel comfortable with the process, and get your questions answered.
Read More About What Is the Role of a Child Life Specialist?
-
¡Adiós a las fiestas, hola a las rutinas! Hacer que los niños retomen el ritmo cotidiano
The kids are back in school and the holidays are all but a distant memory: Now what? Karen Wagner, APRN, offers specific tips about getting kids back to their routines in the post-holiday-hustle-and-bustle. Are you finding the kids struggling with bedtime routines? Having trouble getting them to tackle homework? There’s a simple reason: The holidays messed with their mojo! Here, we talk with Nurse Practitioner Karen Wagner about what to do to get them back on the straight and narrow. Why Routines Are Important “Holidays are a fantastic time to get together with family and friends, so our routines are usually off — and this is understandable, “Wagner says. “While the holidays are exciting, they are chaotic and can put our kids out of the routines.” So how do you get kids back into those routines they crave? “Consistency/routines are crucial for our kids,” she says. “Most people — kids and adults — experience a let-down feeling after the holidays, and post-holiday adjustment takes time.” So what can we do, specifically? Wagner recommends the following: Re-establish family routines, including before- and after-school programs or child care routines. Once kids are back on the regular schedule, they’ll find that sense of familiarity as the old routine returns. But keep in mind, this won’t happen overnight. Encourage healthy eating, as the upheaval of their schedule can be offset by a balanced diet. Make sleep time a priority: Keep in mind that it might take up to three nights of strict bedtime to get them back on track. But enforcing normal bedtime will get their bodies back on a normal schedule. Return to usual chores and expectations. Nothing encourages a return to routine like reminding them of the basics. Incorporate indoor and outdoor time. They likely spent lots of time outdoors during our unseasonably warm winter break — and they even had a snow day or two! So encouraging both indoor and outdoor time will help them return to a circadian rhythm and tire them out from exposure to fresh air. “It is never too early to encourage a love for physical activity in kids by exposing them to fun fitness activities and sports,” Wagner says. “Physical activity improves bone health, cardiorespiratory and muscular fitness, decreases levels of body fat, reduces symptoms of depression, and improves cognitive skills and the ability to concentrate.”
Read More About Bye-Bye Holidays, Hello Routines! Getting Kids Back into the Groove
-
Padres, sus hijos necesitan vacunas contra la gripe. Este es el por qué
Vanessa Slots, MD, of Renown Medical Group – Pediatrics, explains why getting a flu shot each season can save lives—especially true for the very young and elderly. Why Kids Need Flu Shots The flu is not a passing cold. It is a serious illness that takes lives every year. And this year, flu activity is increasing late in the season. And it happens like clockwork — the onset of an influenza epidemic as fall transitions into winter, and lasts into the spring months. This acute respiratory illness is caused by influenza A or B viruses with yearly outbreaks occurring worldwide. No one is immune, and everyone is susceptible to the flu. Flu Signs and Symptoms: Abrupt onset of fever Headache Body aches and fatigue along with respiratory-tract symptoms including cough Sore throat and an irritated nose Who’s at Risk? Once again: Everyone is susceptible, but children and the elderly are at greater risk of complication from influenza, specifically toddlers less than 2 years. At this age, immunities are underdeveloped. Seniors over 65 are also at increased risk because their immune systems have weakened with age. The severity of a child’s symptoms depend on age and prior exposure to the virus. And with young children, flu is more problematic, since they cannot verbalize certain symptoms like body aches and headaches. As a result, children often experience higher fevers, which can lead to seizures or convulsions. Coupled with gastrointestinal issues such as nausea, vomiting, diarrhea and poor appetite, children are at risk of dehydration and other complications from the virus that can require hospitalization. In fact, an average of 20,000 children are hospitalized from flu each year. Pre-Existing Health Issues Health conditions, including but not limited to asthma, cystic fibrosis, heart conditions, cerebral palsy, epilepsy or diabetes, can intensify flu symptoms. Still, a substantial number of children with none of these risk factors experience severe complications from the flu. How to Protect Your Child from the Flu The best way to guard against influenza is with a flu shot. Children and adults should get the flu vaccine before flu season kicks in — usually by the end of October. Shots are provided as long as flu viruses are circulating and the vaccine is in supply.
Read More About Parents, Your Kids Need Flu Shots. Here's Why.
-
Prevention Against STIs Matters
According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new sexually transmitted infection (STI) cases in the United States each year, with rates continuing to increase. What you may not know is most STIs are preventable. We talked with Renown Adolescent Medicine Specialist, Caroline Barangan, MD to learn more about STIs. How Can You Get an STI? The CDC (Center for Disease Control) says that STIs are acquired through sexual contact. There are bacteria, viruses or parasites that can cause an STI which may pass from person to person in blood, semen, vaginal and other bodily fluids. How Do You Know if You Have an STI? STIs can have a range of signs and symptoms such as: Warts, bumps or sores on or near the penis, vagina, mouth or anus Swelling, redness or severe itching near the penis or vagina Discharge from the penis Vaginal bleeding that’s not your period Painful or uncomfortable sex Vaginal discharge that has an unpleasant odor, causes irritation or is a different color or amount than usual Weight loss, diarrhea or night sweats Aches, pains, fever and chills Jaundice (yellowing of the skin and whites of the eyes) Painful or frequent urination Sore throat if you engage in oral sex It’s important to know that the majority of people who have an STI commonly have no symptoms at all, which is why it’s important to get regularly tested once you have had any sexual activity. Young people less than 25 years of age should be screened on a yearly basis at minimum.
-
Sepsis: Causes & Symptoms
According to the Global Sepsis Alliance, 1 in 5 deaths worldwide are associated with sepsis. If not recognized early and treated promptly, sepsis is the final common pathway to death from most infectious diseases worldwide, including viruses such as COVID-19. We spoke with Jeremy Gonda, MD, a critical care physician from Renown Health’s Sepsis Committee to increase public awareness of this preventable medical emergency. What is sepsis? Sepsis is a response to infection—bacterial, viral or fungal—and can start anywhere in the body and spread into the bloodstream. The body is trying so hard to fight an infection that it begins releasing chemicals into the bloodstream that cause inflammation and the shutdown of multiple organ systems. “It carries a very poor prognosis in general unless you catch and treat it very early,” said Dr. Gonda. “Any infection can lead to sepsis. Typically your immune system takes care of the infection. It doesn’t progress, but in cases where the infection becomes severe, or the immune system doesn’t function properly, people can certainly die. So there’s, unfortunately, a very high mortality rate associated with sepsis.” According to the Centers for Disease Control and Prevention, each year at least 1.7 million adults in America develop sepsis. While you can recover from sepsis if caught early, many sepsis survivors suffer from long-term physical and psychological effects. What are the signs of sepsis? One way to spot sepsis is to use the acronym SEPSIS: S – Slurred speech and confusion E – Extreme shivering or muscle pain/fever P – Passing no urine all day S – Severe breathlessness I – “I feel like I might die” S – Skin mottled or discolored Keep in mind that sepsis symptoms can vary depending on where the infection starts. “Patients may experience urinary burning if they have a urinary tract infection or a cough and shortness of breath if they have pneumonia first,” said Dr. Gonda. “However, often symptoms are more generalized or subtle such as fevers, confusion and malaise.” How do you develop sepsis? When germs enter your body, they can cause an infection. If you don’t stop that infection, it can cause sepsis. Areas of infection that more commonly result in sepsis include: Lungs, such as pneumonia Kidney, bladder and other parts of the urinary system Digestive system Bloodstream (bacteremia) Catheter sites Wounds or burns Who is most at risk? People with compromised immune systems are at greater risk for sepsis, such as “The very young, the elderly and any people who may have conditions that suppress your immune system,” said Dr. Gonda. “For instance, if you have diabetes or if you’re an organ transplant patient who is on immunosuppressant therapy, you’re at somewhat higher risk.” Sepsis is often considered a hospital-acquired infection, but a study in The Journal of American Medical Association found that 80% of sepsis cases occur outside of a hospital. That’s why it’s especially important to remember any infection can lead to sepsis, and anyone can develop sepsis from an infection. What do I do? Timing is critical in the case of sepsis and septic shock. According to a study on septic shock patients, there is a 7.6 percent decrease in survival for each hour treatment is delayed. On the other end, if treatment is given within an hour of the first drop in blood pressure, the survival rate is 80 percent. Because sepsis can be so deadly, it’s important to seek medical attention as soon as possible. “If you’re not getting any better, if you think symptoms are progressively worsening – you should definitely be evaluated by a doctor,” said Dr. Gonda. You can help #StopSepsis by getting involved at worldsepsisday.org.
-
Understanding and Managing Childhood Asthma
Dr. Shipra Singh, a Pediatric Pulmonologist, outlines the challenges of diagnosing asthma in children due to symptoms resembling other respiratory issues. It's particularly difficult to identify in infants and young children, who may not clearly exhibit breathing difficulties. Asthma, often confused with bronchitis, croup, or allergies, is a significant chronic illness causing school absenteeism, as per the CDC. Risk factors include prenatal smoking and family history of allergies or asthma. Infants and toddlers are more susceptible due to smaller airways and respiratory viruses, which can exacerbate conditions like colds and bronchitis. How can I tell if my child has asthma? Unfortunately small children are unable to describe their symptoms, making asthma difficult to diagnose. Your child may even be active, playing and smiling, although they are experiencing chest tightness or labored breathing. Observe your child and let the child’s doctor know if: Your child’s breathing behavior has changed (coughing, wheezing, rapid breathing) Your child’s breathing pattern changes (day vs. night, with rest or activity, inside vs. outside) You have a family history of asthma or allergies Your child’s breathing is triggered by any foods or allergies With your help, your child’s doctor can make the best diagnosis to determine if your child has asthma. A pediatric pulmonologist (lung specialist) or pediatric allergist may also have to be consulted for special testing. Tests may include lung function testing, allergy tests, blood tests and X-rays for an accurate diagnosis. What is the treatment for infants and toddlers? Young children can use many of the same medications as older children and adults, although the way they take them and the dosage will differ. A nebulizer (or breathing machine) creating a medicated mist for your child to breathe through a mask may be used. An inhaler with a small spacer tube connected to a mask is also common to help your child breath medication into their lungs. Either of these options are effective. Asthma in children is treated with both fast-acting and long-term medicines to open up airways quickly for easy breathing and also to lessen asthma symptoms over time. Communicate with your child’s medical providers to create a personalized asthma management plan for them. How can I manage my child’s asthma? Recognize your child’s breathing habits and be aware of worsening symptoms. Consult with your child’s doctor on a daily asthma action plan to recognize worsening symptoms and track medications. Here’s an example of an asthma action plan provided by the U.S. Department of Health and Human Services’ National Institutes of Health). Be consistent with the plan and talk to your doctor before changing it. Have an emergency plan in case of a serious asthma attack. Know where the closest ER is and know who can take care of your other children. Also know what the medical treatment coverage is under your insurance plan. Dr. Singh explains, "Discussing asthma with your child may be difficult. Some kids find the subject frightening or confusing. Others, especially the older kids, may resent the treatment and may not be interested in doing it. Talk to your doctor about advice to build an open and trusting relationship regarding your child's asthma care."