Buscar
-
Pediatric Sepsis: Causes, Symptoms and Treatment
Sepsis happens when a person's body reacts too strongly to an infection. Usually, our bodies fight infections with help from our immune system. But with sepsis, the body fights too hard, and that can be dangerous. Dr. Julianne Wilke, Pediatrics and Critical Care Medicine, examines pediatric sepsis's causes, symptoms and treatments and provides tips on preventing this potentially fatal condition. Most Common Causes Pediatric sepsis is a particularly concerning form of sepsis that can occur in children and infants. Therefore, it is vital for parents and caregivers to be aware of the indications of pediatric sepsis and to understand the causes. Bacterial infections are the most common cause of pediatric sepsis, accounting for over 80% of cases. Common Bacterial Causes: Staphylococcus infections (including Methicillin Resistant Staphylococcus Aureas - MRSA) Streptococcal infections (including those causing pneumonia and group B strep) Escherichia coli, or more commonly; E. coli Klebsiella and Pseudomonas infections Viral Infection Causes: Respiratory syncytial virus (RSV) Influenza Parainfluenza Adenovirus Human metapneumovirus Coronaviruses (including COVID-19) Other Causes: Fungal infections (but are relatively rare) Parasites, such as Giardia lamblia Pediatric Sepsis Symptoms Parents and caregivers need to be observant of sepsis symptoms in children and can include: Fever Extremely fast heart rate Rapid breathing Lethargy Pale or discolored skin Low blood pressure Confusion Slurred speech Abdominal pain Diarrhea & Vomiting Decreased urination Difficulty breathing Use the acronym SEPSIS: S – Slurred speech and confusion E – Extreme shivering or muscle pain/fever P – Passing no urine all day S – Severe breathlessness I – “I feel like I might die.” S – Skin mottled or discolored If any of these symptoms are present, seeking immediate medical attention is imperative.
Read More About Pediatric Sepsis: Causes, Symptoms and Treatment
-
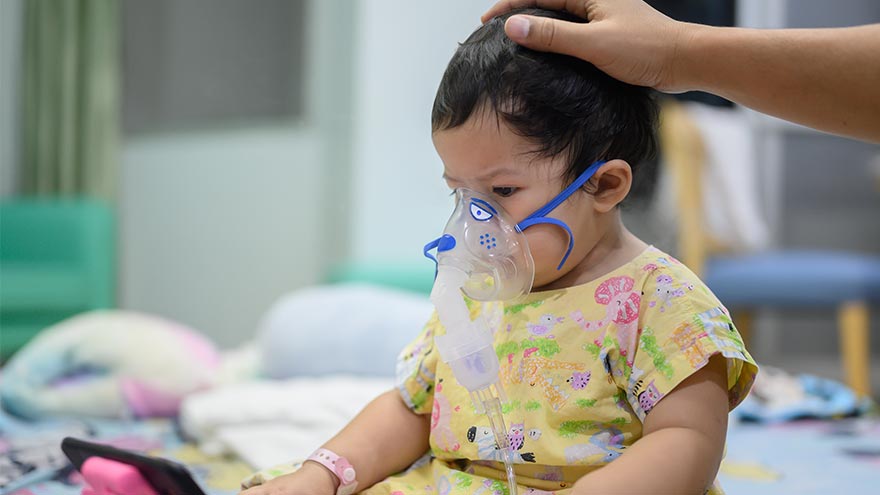
What You Need to Know About RSV
Respiratory syncytial virus, also known as RSV, is a common respiratory virus that impacts the lungs and breathing pathways. The virus can be dangerous for infants and young children and is also concerning for older adults. While most older kids and adults only experience cold-like systems and recover in a week or two, an estimated 58,000-80,000 children younger than 5 years old are hospitalized due to RSV each year, and in 2022 healthcare organizations across the country are experiencing higher infection rates than in years past. "We are experiencing a strong RSV season and do not expect it to go away anytime soon," said Dr. Kris Wilson, Division Chief of Renown Children's Primary Care. "Infants who are infected with RSV almost always show symptoms of runny noses and cough. Call your healthcare provider immediately if your child is having difficulty breathing, is not drinking enough fluids, or is experiencing any worsening of these symptoms.” Symptoms of RSV: Runny nose Decrease in appetite/inability to drink Dry diapers, an indication of dehydration Cough, which may progress to wheezing or difficulty breathing Irritability (most common in very young infants) Decreased activity (most common in very young infants) Decreased appetite (most common in very young infants) Apnea, pauses in breathing for more than 10 seconds (most common in very young infants) What to do if you think your child has RSV: Call your pediatrician! If you suspect your child might have RSV, consulting their healthcare provider is the best first line of defense. From here they will help you build an appropriate treatment plan for child. Keep in mind that many pediatrician offices offer 24/7 call lines. If your child is experiencing retracted breathing (when the area between the ribs and in the neck sinks in when a person attempts to inhale), dehydration (not drinking and decrease in wet diapers) or apnea (pauses in breathing for more than 10 seconds) please call 911 or go to the closest emergency room.
-
Departamento destacado: Float Pool
Ring in the New Year and the rest of the holiday season by celebrating Renown’s Float Pool team! After coming out of the COVID-19 pandemic, it's no mystery that healthcare across the country has shifted and adapted to the growing needs and new demands of our patient populations. Renown Health is no different. As the largest not-for-profit health system in the region, we are no stranger to change, even when change presents challenges. Who do we call on when a unit needs more team members in the eleventh hour? Who can help when our patient volume spikes up with seconds to spare? This is where the Float Pool at Renown comes to the rescue. Skilled in a wide variety of healthcare specialties, from acute care nursing and critical care to care aiding and patient safety, this is the team that can seamlessly step in to provide crucial patient care to the units that need it most, whether a team is understaffed for the day or needs extra all-hands-on-deck for a specific patient or procedure. Float Pool team members are equipped to work in virtually any clinical area at Renown, making a genuine difference with every patient they encounter. A Pool of Relief Teams across Renown can breathe a sigh of relief knowing that Float Pool has their back in times of need. As the backbone of our health system, these dedicated team members possess a wealth of clinical knowledge and the ability to navigate diverse medical environments. Their flexibility allows them to fill staffing gaps and provide essential support to many different units. “We fill in the gaps of staffing to make everyone's day better,” said Patti Crepps, Critical Care Float Pool RN. “A float nurse has to be flexible and able to adapt to different situations and places – basically, ‘go with the flow.’ Patient care is basically the same all over; we make patient care possible by being familiar with all the various specialties and providing the specific care needed depending on the population we are taking care of on that shift.” “Float Pool staff members are like healthcare chameleons, transitioning between different departments,” added Shelby Riach, Acute Float Pool RN. “We incorporate flexibility, teamwork and a commitment to ensuring patients receive the best care, regardless of the setting or circumstances.” This team thrives in uncertainty; in fact, no workday is the same in Float Pool – and that’s exactly the way they like it. Working with many different teams across a multitude of specialties, these Care Aides, RNs, Critical Care Techs, Patient Safety Assistants (PSAs), Certified Nurses Assistants (CNAs) and more enjoy facing change, while they all share a goal of providing the best patient care possible. “No day looks the same; since we are the Float Pool, we are assigned a different assignment on Smart Square every day, whether it be as a care aide, a patient safety assistant, a unit clerk or patient transport,” said Melina Castenada, Care Aide. “If we are assigned as a care aide on the floor, we help assist with call lights and help with whatever nurses and CNAs may need, including feeding, transporting, walking, helping patients use the restroom, etc. When we are assigned as a PSA ‘sitter,’ we sit for the patient to help keep them safe. If we are assigned as unit clerk, we help answer phones and direct patients appropriately, file paperwork, answer call lights if needed and assist with office work.” “I love that every day is a different floor with different tasks and a different atmosphere,” added Julia Chappell, Critical Care Technician. “I find out which floor that I will be on right before my shift starts and head to the floor to find out my assignment for the day. Depending on the specialty, such as the medical-surgical floor versus an intensive care unit (ICU), my daily job tasks can vary.” When it comes to high-risk patients, who require special attention, PSAs within Float Pool step in to help. “The PSA role within Float Pool largely consists of adverse event prevention for our high-risk patients, and being a Float Pool employee allows us to work wherever we are needed,” said Dimitri Macouin, Patient Safety Assistant. “Whether it be in the emergency department, neurology or pediatrics, the PSA will be the eyes and ears for the nurses working with this patient population.” “Great strides have been made to ensure that PSAs remain vigilant and are recognized as an integral part of the patients' care team rather than 'just a sitter,’” added Karla Phillips, Patient Safety Assistant. Float Pool also oversees our Discharge Lounge, which offers patients and their families a dedicated space to reconnect and prepare for their discharge from the hospital. “The increase in utilization of the Discharge Lounge is something we are very proud of,” said Kara Abshier, Care Aide. “We assist in discharging patients from all over the hospital to help the floor and get new patients into rooms.” Every day brings a new challenge for Float Pool. As these team members wake up with uncertainty, they are ready to embrace the diverse demands of caring for patients of all ages. “The fact that Float Pool exists is amazing,” said Hannah Luccshesi, Acute Float Pool RN. “We wake up with no clue as to whether we will be working with babies, children or adults and then fill in the needs of the hospital.”
-
3 Ways to Foster the Wellbeing of LGBTQIA+ Kids and Teens
Ensuring a healthier and more inclusive future for LGBTQIA+ children and teens is of utmost importance to health systems in our community, especially Renown. Supporting the physical and mental health of youth in this community is key to those efforts, especially as they face unique challenges in terms of identity acceptance and social integration. Dr. Caroline Barangan, Adolescent Medicine Physician with Renown Children’s Pediatric Specialty Care, discusses what you as a parent, caregiver, friend or support system can do to be a safe space for children and teens who identify as LGBTQIA+. 1. Create a Safe Space at Home The most important action you can take for your LGBTQIA+ teen or child is to accept and support them for who they are, regardless of how they identify. “Being a teenager is already difficult enough, especially within the LGBTQIA+ community, which puts them at risk of being stigmatized, rejected and targets for bullying,” said Dr. Barangan. Your supportive words and actions can make a huge difference as a profound expression of love and understanding. Being patient and willing to learn are the foundations to a healthy and loving relationship with your LGBTQIA+ teen or child. 2. Encourage Regular Check-Ups with a Primary Care Provider (PCP) Establishing your child or teen with a PCP is not only important when an illness occurs but also for annual preventative visits and regular check-ups. “A primary care provider can screen for high-risk behaviors that would put a patient’s health in jeopardy, such as sexual experience, substance use, suicidality and self-harm,” said. Dr Barangan. “These screenings are an opportunity to provide the education and support these kids and teens need to stay healthy.” One of the main concerns LGBTQIA+ youth often have is that they will experience judgment from their provider, or the PCP will disclose sensitive information, including their sexuality or gender identity to their parents, when they are not ready to do so. Dr. Barangan emphatically reminds us that this legally cannot happen. “If a patient asks me to keep something confidential, unless they disclose that they have plans to harm themselves or others, I am legally not allowed to share that information with anyone without their permission,” said Dr. Barangan. 3. Locate Local Resources Northern Nevada is home to a variety of resources for the LGBTQIA+ community at large, including youth members of this community. "Finding resources to help them develop in a positive way and provide them with the information they need, whether it be in school, the household, the community or through a medical or mental health provider, is incredibly important,” said Dr. Barangan. Below is a list of local LGBTQIA+ community resources open to you and your children: Our Center LGBTQIA+ Health Services at Northern Nevada HOPES Northern Nevada Pride Festival & Community Parade (happens every July in Reno) Sassabration (happens every September in Carson City) Lake Tahoe Pride (events and resources shared on Facebook)
Read More About 3 Ways to Foster the Wellbeing of LGBTQIA+ Kids and Teens
-
6 Healthcare Action Items for the LGBTQIA+ Community
Every patient, regardless of how they may identify, greatly benefits from preventive healthcare and early detection. Members of the LGBTQIA+ community face unique considerations when it comes to their health, and a proactive approach to preventive screenings and vaccines is important in order to address their individual health needs. Dr. Karen Thiele, Family Medicine Physician with University Health and Assistant Professor of Family and Community Medicine at the University of Nevada, Reno School of Medicine, breaks down key steps that LGBTQIA+ patients should take to safeguard their health. PrEP and PEP Pre-exposure prophylaxis (PrEP) is a strategy to prevent human immunodeficiency virus (HIV) infection. It is an important measure for those who are HIV-negative but may be at risk of contracting it. The highest risk sexual practice is receptive anal intercourse, due to the relative fragility of rectal tissue. This medication can stop HIV from spreading in the body and help patients maintain their HIV-negative status. PrEP is available in both pill form, which is taken every day, and injection form, of which the first two injections are initiated one month after another while all other injections are initiated every two months. Post-exposure prophylaxis (PEP) is an antiretroviral drug regimen taken after potential HIV exposure to prevent an HIV-negative individual from converting to HIV-positive status. PEP is only for emergency situations and must be started within 72 hours of exposure – sooner is always better than later – and must be taken for 28 days. PrEP and PEP are available in many ways, including visiting your primary care provider (PCP) or an urgent care location. HPV Immunization All genders and identities can protect themselves against human papillomavirus (HPV), a sexually transmitted infection (STI) that can lead to the risk of cervical, mouth, head, neck, throat, anal, vaginal, penile and vulvar cancers. HPV is so common that nearly all sexually active people, regardless of sexual orientation and practices, will be exposed at some point in their lifetime. The HPV vaccine (common brands include Gardasil and Cervarix) is a safe and effective method to prevent HPV, according to the Centers for Disease Control and Prevention (CDC). This vaccine protects against infections that can lead to HPV-related cancers and precancers, as well as genital warts. While patients should start receiving the vaccine at 9 years old years old, unvaccinated adults up to the age of 45 can also receive the vaccine through their PCP – better late than never! STI Testing Sexually-transmitted infections form from bacteria, viruses or parasites that can be transmitted by person-to-person sexual contact through semen, vaginal, blood and other bodily fluids. According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new STI cases across the nation each year. Luckily, most STIs are preventable. Annual STI testing for HIV, gonorrhea, chlamydia and syphilis is important to stay on top of your sexual health. Because these STIs may sometimes have no symptoms, screening is recommended regularly and with any change in sexual partners. Depending on the specific condition, tests for these infections include urine, swab and blood tests. Speak with your primary care provider on a screening schedule that works best for you. Prostate Exams Prostate exams look for early signs of prostate cancer in patients who still have a prostate. The CDC recommends those who are at least 55 years old get regular prostate screenings; however, for patients with a family history of prostate cancer, screenings may be recommended as early as 45 years old. These exams are done via two common methods – a prostate specific antigen (PSA) blood test and a digital rectal examination (DRE). Your provider can help you determine your risk and when you should start getting screened. Pap Tests and Pelvic Exams Patients of all genders who have a cervix, uterus, vagina and/or ovaries will benefit from regular pelvic exams and Pap screenings. A pelvic exam consists of a provider looking inside the vagina and at the cervix for anything unusual. A Pap test, also known as a Pap smear, involves your provider using a small, soft swab to collect cervical cells to check for early signs of cancer. Generally speaking, people with these organs should have a Pap test every three years starting at age 21 through the age of 30. After age 30, patients should receive a Pap test with HPV co-testing every five years until age 65. These recommendations are changing based on new research, so it is important to have a conversation with your PCP about the current guidelines so you can make an informed choice about what schedule you should follow. A gynecologist or your primary care provider can counsel you and perform these screenings. Mammograms and Breast Exams People with breast tissue, especially dense breast tissue, are at risk for breast cancer, and regular breast screenings are your best line of defense. At-home breast self-exams are the first step – you will want to check your breasts for any lumps, changes, fluid leaks, irregular tissue thickening or anything else that feels unusual. The Breast Cancer Risk Assessment tool, provided by the National Cancer Institute, is a good place to start to identify your risk. Talk with your primary care provider about the risks and benefits of starting screening at age 40 so you can make an informed decision about when to start. If you have any family history of breast or ovarian cancer, your PCP will offer you genetic testing for BRCA 1 and 2 mutations. Nevadans over the age of 18 can also get BRCA genetic test for free by enrolling in the Healthy Nevada Project. Mammograms are important screening tools, but for a significant portion of people with breast tissue, density of the breast tissue may make mammograms less helpful in detecting cancer. Your primary care provider can help you decide what additional imaging (such as breast ultrasound) might be best for you.
Read More About 6 Healthcare Action Items for the LGBTQIA+ Community
-
Nurturing Your Child's Back-to-School Mental Health
The back-to-school season is here, and ensuring your child's successful transition involves more than just school supplies and schedules. At Renown Children’s Hospital, and in collaboration with Nevada Pediatric Psychiatry Solutions, we understand the vital role that mental health plays in a child's overall well-being and academic performance. Below we'll guide you through essential tips for a smooth back-to-school experience, with a special focus on nurturing your child's mental health. How to Support Your Child’s Mental Health from Home Remember, the below strategies can be adapted to align with your child's personality, learning style and household dynamics. Flexibility and understanding are key in tailoring these tips to suit your child's unique needs. 1. Be Open to Communication: Recognize that effective communication is the cornerstone of understanding your child's feelings and concerns. Create a safe space where your child feels comfortable expressing their thoughts. Listen to learn, without judgment. Make it a point to validate their emotions and ensure they are heard. Encourage sharing experiences,worries, friends and challenges they may be facing. Having open conversations about sensitive topics opens the door for discussion and understanding. Make yourself available. 2. Establish a Routine: A consistent routine can offer a sense of stability and predictability for your child, and anticipation helps to decrease anxiety and establish a sense of control. Join forces and design a daily schedule that includes time for schoolwork, play, physical activity, meals and relaxation. Be flexible about the structure to allow room for last-minute changes including extra activities based on that day’s needs as well. Always add time for play and bonding. 3. Practice Compassion: Back-to-school can come with big emotions. Listening reflexively and acknowledging these feelings can help you and your child act positively on these big emotions. 4. Get Involved: Actively engage in your child's school life by participating in school events, meetings and discussions. Show interest in their educational journey, ask about their experiences and provide guidance when needed. Being present in their academic pursuits not only boosts their confidence but also strengthens the parent-child bond. 5. Use Positive Reinforcement: Celebrate your child's achievements, no matter how small they may seem. This allows for a sense of accomplishment and boosts self-esteem. Praise efforts, progress and perseverance, whether it's completing an assignment, making a new friend or overcoming a challenge. This positivity encourages a growth mindset and resilience. 6. Organize a Schoolwork Zone: Create a comfortable workspace at home dedicated to school-related tasks. Customize the area based on your child's preferences and needs. Having a designated space for studying and completing assignments promotes focus, reduces distractions and enhances their overall learning experience.
Read More About Nurturing Your Child's Back-to-School Mental Health
-
Departamento destacado: Security
“Safety is Number One,” isn’t just a saying – it's a fact of life, especially at Renown Health. The safety of all patients, visitors, staff and volunteers is always the top priority, and our Security Department takes that commitment seriously. This team is devoted in their efforts to provide a safe environment for all, building cooperative and proactive security processes leveraging crime prevention techniques and state-of-the-art technology. Renown Security sets the safety and well-being bar high, and they continually exceed that standard day in, day out at all of our hospitals and urgent care, primary care and lab locations. Specially Trained, Continually Present Our Security Department isn’t staffed with your run-of-the-mill Security Officers; these team members surpass security and safety expectations. Think city and state police-level standards. You read that right – many of Renown’s Security Officers come from Nevada Highway Patrol, the Washoe County and Carson City Sheriff’s Offices, the state probation and parole board and more. This team fosters specialized training in a collaborative environment. Every member of the security team has extensive training in compassion, empathy and de-escalation techniques to provide the highest levels of safety and security. They implement this training in all their daily duties, whether they are saying a simple ‘hello’ to a patient passing by or preventing harm to a staff member. Before their shift begins, the team meets to debrief meeting to discuss major incidents that occurred on the previous shift. These meetings ensure the next shift is aware of situations to be on special alert for and individuals to look out for. After, the team members head off to their assignments. “The day could be as mellow as greeting someone at the welcome table, or it could be as chaotic as de-escalating someone in distress,” said Emmanuel Fernandez-Orozco, Supervisor of Security at Renown Regional. “Regardless of the day, every experience is rewarding in its own way. The only thing that is promised is that every day will be different.” While every Security Officer has varying experiences, one aspect of their job always stays the same: they are always on alert for any potential safety issue. Even on the “slowest” days, it is important for this team to stay vigilant in order to mitigate any potential risks. There are several security programs that the team uses to keep everyone at Renown safe and secure: Renown's security operations center team (also known as dispatch) monitors all cameras in real time, with security officers patrolling parking areas 24/7. Security escorts are always available for any employee, patient or guest at every Renown location. Security Officers can escort anyone to their designated site, check surroundings for danger and monitor the person until they safely leave for their next destination. Rescue officers are available for any Renown location where an employee feels unsafe. Security maintains a strong relationship with the Reno Police Department (RPD) and assists with reporting and providing information that aids RPD in pursuing and deterring criminal activity. “In security, we are a counselor, teacher and rule enforcement officer, all rolled into one,” said Bob Stone, Supervisor of Security for Renown Health. Talk about master multitaskers! Protection is only one part of the job. Through positive and meaningful interactions with guests, patients, community and staff, regardless of where they are posted, the Security Department continually helps Renown achieve its mission of making a difference for the people they serve. Devoted Dispatch Speaking of multitasking, no one does this better than the Security Dispatch Center. Security Dispatchers are the “eagle eyes in the sky” at Renown, keeping a close watch on everything that happens within every Renown location, as well as REMSA (including Care Flight). From overlooking the many cameras around campus and administering codes over the PA system to manning the radio and phones to ensure Security Officers are dispatched quickly, our dispatch team helps ensure every safety or security issue at Renown is immediately addressed. When a call comes in, dispatchers like Jessica Fernandez, Security Dispatcher for Renown Health, go through a quick discovery process (sometimes in seconds) to figure out the details of the situation or code and what level of security is needed to assess and de-escalate. According to Jessica, the ability to prioritize is something she values in her work. “80 percent of our duties are on the phone and the radios, and we are skilled in prioritizing concerns based on the sheer volume of calls we get,” she said. Jessica and her teammates are proud of the outcomes from their calls. Their attentiveness to every nook and cranny at Renown and their quick response times to make them not only a valued partner to the Security Department but also a necessity to our health system. Your In-House De-Escalation Experts Being in a hospital environment is undoubtedly stressful for any patient, and many factors can increase these emotions. The Security Department takes these feelings seriously and never hesitates to take appropriate action to ensure the safety of everyone at Renown. With the unfortunate rise of violence against healthcare workers, especially amid the pandemic, our first-rate security team has been crucial in countering violence with specialized de-escalation techniques. The key to de-escalating, according to the Security Department, is to put yourself in the shoes of whoever you are working with. As stated by Bob Stone, the team approaches each situation by asking themselves: How would I want to be treated if I was in the same circumstance? “Being empathetic to their situation and listening to what is going on in their lives is key to re-directing them accordingly,” said Bob. “Applying real-life experience to similar circumstances can make them feel like they are not alone. Educating people on hospital policies can also help them reduce their anxieties and solve the problems.” Jhorddy Lopez, Security Officer at Renown Regional, approaches each situation with the mindset of knowing that each person’s reactions are different. “Different techniques need to be implemented every time,” said Jhorddy. “You have to use your best judgment call.” Quick and effective judgment calls are a task that the Security Department has conquered. Rosie Garcia, Security Officer at Renown Regional, knows that using your best judgment means getting both sides of the story. “Whenever I need to step in and de-escalate a situation, I first speak with whoever is attending to the patient and gather information,” said Rosie. “Then, I always get the patient’s side as well. I want to understand how they’re feeling, so both the staff member and the patient can meet in the middle and come up with a collaborative solution.” An example of the heroism and advanced de-escalation displayed by our Security Officers takes us back to last spring. In the middle of the night, a Care Flight helicopter transporting a patient and their family was about to touch down on the landing pad outside of Renown Regional. Right as the helicopter was about to land, an individual jumped over the safety barricade and onto the landing pad. Alexander Pico, a former Security Officer Lead at Renown Regional (who recently joined the Carson City Sheriff’s Department) immediately communicated with the individual to leave the area. The individual then went under the rear blade, which is the most dangerous part of the helicopter. Knowing that he had to risk his own life at this point to save another, Alexander ran around the back of the helicopter and tackled the individual, preventing catastrophic injury or even death. Steve Perkins now uses this example of a swift judgment call, which was captured on dispatch cameras, as training material for new staff. Exceptional character, compassion and emotional intelligence are the attributes that every member of the Security Department holds. As noted by Steve Perkins, these attributes “allow for a quick assessment of each situation in order to de-escalate and move towards the best possible solution." Securing the Job The Security Department at Renown is actively hiring caring, dedicated team members who are ready to jump in and perform exceptional high-risk healthcare security services for our health system. “We seek people with the right combination of ability and demeanor,” said Steve Perkins. "The training and skills development we provide result in a high caliber of success.” Every team member in the Security Department is passionate about the same thing: helping others. And in a healthcare environment, this is important. “Working a healthcare security job is far different than working any other security job,” said Jhorddy Lopez. “At a hospital, you get the chance to interact with people one-on-one. I get to experience the feeling of, ‘I can make a difference in this person’s life.’” Any interaction can change the course of a person’s day, and the Security Department embraces this fact. “I really do love helping people so much, whether it be an elderly patient who needs help with their wheelchair or a situation where I need to step in and de-escalate,” said Rosie Garcia. In order to succeed in this fast-paced department, being a collaborative team member is crucial. “A good coworker is a team player – someone that loves to work in a team atmosphere,” said Emmanuel Fernandez-Orozco. Jhorddy Lopez reiterates this, adding that “communication and trust are also extremely important. Everyone has to have great communication skills and have each other’s backs.” For people like Bob Stone, having a special connection to Renown inspires him to serve. As someone who experienced two life-saving hospital stays here, he is proud to give back to the organization that gave so much to him. “It was only natural to return to a facility I was familiar with my entire life,” said Bob. “After serving as a paramedic and transporting patients into Renown from Plumas County, I knew I was not done giving back to the community. Renown was the place to do exactly that.” All Genders Welcome A common misconception about the security field is that it is strictly a “man’s job.” In Renown’s Security Department, that couldn’t be further from the truth. As a female Security Officer, Rosie Garcia is a prime example of proving that idea wrong. As a master patroller and de-escalation expert, she ensures everything is running smoothly and that everyone feels safe at all times. “When I first started here, I knew right away that nobody that works here is biased,” said Rosie. “Everyone is equal, and I am treated as an equal in this department. I know I can do the job as well as any man." Both Rosie and her counterparts in the Security Department firmly believe that this line of work is for everyone, and they continually lift each other up and support one another. “No matter your gender, as long as you have confidence and integrity, you will do well,” adds Rosie. The Bottom Line If you are passionate about creating a secure environment to ensure patients get the care they deserve and employees receive the safety they merit, the Security Department is your team to join. “I come into work with pride,” said Jhorddy Lopez. “Knowing that I can change someone’s life – that makes me proud to work here.” “You’re in good hands with us,” closes Steve Perkins.
-
Prevention Against STIs Matters
According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new sexually transmitted infection (STI) cases in the United States each year, with rates continuing to increase. What you may not know is most STIs are preventable. We talked with Renown Adolescent Medicine Specialist, Caroline Barangan, MD to learn more about STIs. How Can You Get an STI? The CDC (Center for Disease Control) says that STIs are acquired through sexual contact. There are bacteria, viruses or parasites that can cause an STI which may pass from person to person in blood, semen, vaginal and other bodily fluids. How Do You Know if You Have an STI? STIs can have a range of signs and symptoms such as: Warts, bumps or sores on or near the penis, vagina, mouth or anus Swelling, redness or severe itching near the penis or vagina Discharge from the penis Vaginal bleeding that’s not your period Painful or uncomfortable sex Vaginal discharge that has an unpleasant odor, causes irritation or is a different color or amount than usual Weight loss, diarrhea or night sweats Aches, pains, fever and chills Jaundice (yellowing of the skin and whites of the eyes) Painful or frequent urination Sore throat if you engage in oral sex It’s important to know that the majority of people who have an STI commonly have no symptoms at all, which is why it’s important to get regularly tested once you have had any sexual activity. Young people less than 25 years of age should be screened on a yearly basis at minimum.
-
What is Dry Drowning?
Whether you're a parent, grandparent, caregiver or sibling, you should know drowning is the second leading cause of death among children. Yet, while we are vigilant about protecting children from water accidents and drowning, a condition known as dry drowning or delayed drowning can go unnoticed. In fact, most people aren't even aware it exists. Dry drowning defined Dry drowning is a side-effect of a near-drowning experience and includes spasms of the vocal cords and larynx — known as a laryngospasm. This occurs when the body attempts to shut down the passage of any liquid into the lungs. Unfortunately, it can also shut down the passage of air into the lungs and force fluid into the stomach and lungs. Often the condition is not discovered until it's too late — severe cases can cause death within one to 24 hours after a water incident occurs. Who is susceptible? Novice or first-time swimmers are at increased risk, as are children with asthma and known breathing issues. In addition, children who have had pneumonia or experienced acute respiratory distress syndrome are also at greater risk. To reduce these factors, caregivers should be exceptionally watchful of inexperienced swimmers. According to Leland Sullivan, MD, of Northern Nevada Emergency Physicians, children under the age of 5 are most susceptible to drowning and often drown in residential swimming pools. Infants less than 1-year-old most often drown in bathtubs. What are the signs of a dry drowning episode? If your child has a near-drowning incident, a few moments of coughing until they calm down is normal. However, you should know the more severe signs and symptoms to watch for during the 24 hours following the incident, including: Persistent coughing Difficulty breathing and/or shortness of breath Chest pains Extreme fatigue and/or lethargy Change in typical behavior Face becomes pale What is the treatment and prognosis for dry drowning? Dr. Sullivan recommends that all victims of near-drowning incidents seek medical attention, even if they have no symptoms. If caught early, dry drowning can be treated. If you think your child is experiencing a dry drowning episode, go to the nearest emergency room as quickly as possible — do not attempt treatment at home. Healthcare professionals will work to supply oxygen to your child's lungs to restore and regulate breathing.
-
La seguridad en las residencias universitarias y la meningitis bacteriana
Bacterial meningitis is probably the last thing on your mind as you help your child prepare for college. Buying books and stocking up on necessities may top your list, but it’s a good idea to ensure your student is up-to-date on their meningitis vaccine. How Bacterial Meningitis Spreads According to the Centers for Disease Control and Prevention, people living in close quarters are more likely to spread this illness to one another. For example, you may have heard about the higher risk of meningococcal (or bacterial) meningitis for new college students. The risk is so serious that many colleges and universities require proof of a vaccine for new students moving into campus housing. This includes the University of Nevada, Reno. To clarify, all incoming freshmen under 23 years of age must show proof of their up-to-date meningitis shot. “Bacterial meningitis is considered a medical emergency, and anyone with the signs and symptoms should be evaluated in the emergency room immediately,” says Vanessa Slots, MD, Renown pediatrician. Symptoms of Bacterial Meningitis Fever Nausea Vomiting Irritability Headache Confusion Back pain Stiff or painful neck Leg pain Light sensitivity Rash on the torso or lower extremities It’s important to know many of these symptoms for both bacterial and viral meningitis are the same. However, the viral type is more common, often clearing up in seven to 10 days without complications. Nonetheless, you should go to the emergency room to be looked at, as the signs are similar for both illnesses. Why is Bacterial Meningitis Dangerous? This illness moves quickly, and in some cases, it can seem like the flu or severe strep throat and take a few days to develop. Or, it can hit in just hours. “Bacterial meningitis has an overall death rate of 10 to 15 percent despite treatment with antibiotics,” Dr. Slots warns. Another critical point is problems after recovery can also be severe. Frequently these include brain damage, amputations, infections around the heart, seizures and shock.
-
Suicide Risk How to Spot a Friend in Crisis
How can you tell if a friend is in trouble or struggling with suicidal thoughts? And how can you support them in finding help? Are you feeling virtually exhausted? Life is always challenging, but the mental fallout of a global pandemic is real. Contributing to the loneliness epidemic is the shifting American lifestyle. More Americans live alone (28%) now than ever before, and fewer have kids. First, let’s acknowledge this is a time of anxiety and worry for everyone. Economic uncertainty, job transitions, grief, and loneliness are a perfect storm for mental stress. Even before the COVID-19 (coronavirus) pandemic mental health was a concerning issue, now it is a relevant topic of crisis. Secondly, anyone can struggle with suicidal thoughts. Those suffering from drug addiction are especially vulnerable. In particular the U.S. is currently seeing a rise in drug overdoses by almost 18% due to the pandemic. Unfortunately, suicide is responsible for one U.S. death every 11 minutes, according to the Centers for Disease Control and Prevention. Not to mention the millions who think about it, make a plan or attempt it. It is important to remember that suicidal thoughts, plans or intent must be helped immediately. Understanding Suicide Risk To clarify, depression is not a choice. No one wishes for endless days of feeling down, sleepless nights, and feeling as if you are in a dark tunnel. Currently, one in five Americans will experience a mental illness this year. This means one of your friends is struggling, right now. Specifically, consider this: When your body feels pain it talks to your mind. When your mind is suffering who does it talk to? So, how can you tell if a friend is in trouble? According to the National Institute of Mental Health be on the lookout for some depression clues below. Signs and Symptoms of Depression Persistent sad, anxious, or “empty” mood Feelings of hopelessness, or pessimism Irritability Loss of interest or pleasure in hobbies and activities Decreased energy or fatigue Moving or talking more slowly Feeling restless or having trouble sitting still Difficulty concentrating, remembering, or making decisions Signs and Symptoms of Suicide Risk Expressing feelings of hopelessness or having no purpose Talking about feeling trapped or being in unbearable pain Talking about being a burden to others Increasing the use of alcohol or drugs Sleeping too little or too much Withdrawing or isolation Displaying extreme mood swings. Talking about wanting to die or to kill oneself (Reference: Suicide Awareness Voices of Education) How to Help a Suicidal Friend It can feel awkward to approach the subject of suicide with a friend, but take any of the above warning signs seriously. Other ways you can help are by: Encouraging self-care and making sure they take care of basic needs Listen to their worries without judgement Ask them what they need from you, then follow through with action Let them know they are not a burden Don’t minimize or invalidate their feelings Point them to helpful resources Be their advocate and get them help If someone you know is in a life-threatening crisis situation, call 911 immediately. Suicide Risk Resources: National Suicide Prevention 24/7 Lifeline: 1-800-273-8255 Ayuda En Español: (Spanish National Suicide Prevention Lifeline) 1-800-628-9454 Crisis Text Line: Text HOME (or CONNECT) to 741741 to chat with a crisis counselor 24/7 free of charge. The National Alliance on Mental Health: 1-800-950-6264 Substance Abuse and Mental Health Services Administration: (SAMHSA) 24/7 helpline 1-800-662-4357
-
4 fantásticos beneficios para la salud de estar libre de desorden
The Benefits of Being Clutter-Free Gives you a better sense of well-being. Did you know procrastination is linked to clutter? According to a recent study clutter problems led to less life satisfaction, especially among older adults. Helps you lose weight. Constantly being in cluttered room, office or car can be stressful. All the undone cleaning tasks in the back of your of mind cause stress, which is linked to obesity. Promotes mental health. Having clutter around can make you feel anxious or overwhelmed. This prevents you from truly relaxing or focusing. Saves you money. It’s not a secret that money worries cause stress. According to a Journal of Consumer Research study, you’re more likely to make a purchase when you’re sitting in a messy room compared to a tidy room. Clutter-Free Tips Start with a plan. Make a list of your clutter-improvement priorities and the tasks needed to accomplish each one. Focus on one section of your home per week, so you don’t get overwhelmed. In fact, organizational expert Peter Walsh suggests starting with the easiest room first to gain momentum. Conversely, "The Life-Changing Magic of Tidying Up" author Marie Kondo suggests organizing by category (for example clothing or books). Experiment with an organizing plan that appeals to you. There are also many helpful on-line calendars you can use as a starting point. Delegate when you can. Include your children and spouse into your plan. Is uncle Bob an electrician? Then get him to swap out your eyesore of a ceiling fan or update an old light fixture. Of course it’s ok to outsource the duties - such as window cleaning or painting - if your budget allows. Buy less. The less you purchase the less you need to store, clean, keep track of, organize or dust. Seems simple, right? Not for everyone. On average we are bombarded with over 4,000 marketing messages a day, not to mention FOMO (Fear Of Missing Out) when we see our friends posting about their newest toys on their social media feeds. Focus on quality over quantity. When in doubt, throw it out. Still on the fence about what to throw away? Use these declutter decision-making guide questions to help you. Organize Your Health Along with taking care of your surroundings, make a commitment to get up to date on your health checkup and screenings. Preventing an illness is a bargain compared to the cost of a chronic disease. It's also a good idea to go through all of your medications and check the expiration date. Remember to properly dispose of medications. DO NOT flush medications down the drain or toilet, unless the label indicates it is safe to do so.
Read More About 4 Fantastic Health Benefits of Being Clutter-Free

.png?rev=fcd27802b7604a96bf1056b050ef90c5)








