Buscar
-
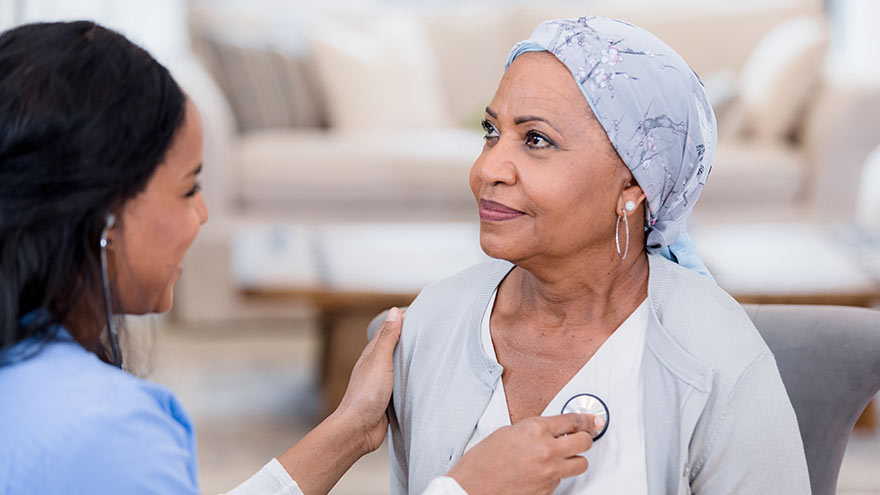
Life after Lymphedema Diagnosis: ¿Qué esperar?
Managing lymphedema effectively is essential for enhancing the quality of life for individuals affected by this condition. Katherine Bunker, a Physical Therapist and Certified Lymphedema Therapist (PT, DPT, CLT) at Renown, has expertise in this area and her insights offer valuable strategies for managing lymphedema. Lymphedema is a chronic condition characterized by swelling in one or more limbs due to a blockage in the lymphatic system. This condition can result from cancer treatments, surgery, infection, or can sometimes be congenital. While it can be challenging to live with lymphedema, understanding the condition and adopting specific lifestyle changes and strategies can significantly improve the quality of life. Understanding Lymphedema Educating yourself about lymphedema is crucial. Understanding the causes, symptoms, and potential complications can provide you with the tools to manage the condition proactively. Lymphedema can lead to discomfort, decreased mobility, and in severe cases, infections such as cellulitis. Therefore, recognizing the early signs and knowing when to seek medical advice is essential. Medical Management Consulting with healthcare professionals who specialize in lymphedema is critical. A physiotherapist or occupational therapist trained in lymphedema management can tailor a treatment plan for you that can include the following: Compression Therapy - Wearing prescribed compression garments can help move the lymph fluid and reduce swelling. It’s essential to get fitted by a professional and understand how to use these garments correctly. Manual Lymphatic Drainage (MLD) a gentle massage technique that encourages the movement of lymph fluid out of the affected limb. It’s typically performed by a trained therapist but ask about self-massage techniques you can do at home.
Read More About Life after Lymphedema Diagnosis: What to Expect
-
Departamento destacado: Cuidado de las heridas
For the average person, wounds aren’t an everyday worry. However, for at least eight million Americans, chronic wounds can pose a serious threat to health and well-being. From a person with diabetes experiencing painful neuropathy to a patient healing from a significant burn, caring for advanced wounds is a major part of their healthcare journey. Who do they go to get the care and guidance they need? The answer: Renown Wound Care. Serving patients in both the inpatient and outpatient settings, this department provides comprehensive, best-in-class treatments for severe and chronic wound healing and ostomy care. Our Wound Care team members have mastered the art of harnessing cutting-edge technologies and a patient-centric approach to redefine the standards of healing. Advanced Care for the Best Repair At Renown Health, we are fortunate to have a team full of nurses, physicians and more caring for patients with wounds caused by a wide variety of conditions. Those include: Burns Trauma Vascular diseases Radiation therapy Pressure ulcers Diabetes and diabetic neuropathy Adding to the expert-level continuum of care, Renown is the only health system offering complete ostomy services in the entire region. The Wound Care team helps ostomy patients with the fitting of their medical bags, treatment of any skin conditions that may arise after ostomy bag placement, care coordination and much more. With a multidisciplinary network of experts tailoring personalized treatment plans, there is never a dull moment on the floor. On the outpatient side, the team expects 50-60 patients in one day alone. “As a clinician, wound care is a lot of ‘arts and crafts,’ so we get to use our creative and critical thinking skills to provide the best possible care,” said Samantha Moore, Advanced Wound Care Specialist RN for Outpatient Wound Care. “Each patient has an individualized plan of care – we greet them as they come into the clinic, escort them back to their treatment rooms and get their latest health updates and life situations before providing wound or ostomy care. We prepare each morning doing chart reviews to determine patient needs, wound progression and referral needs.” “We are a highly specialized, dedicated group of professionals with a passion to treat and heal our patients’ wounds,” added Lori Conner, Advanced Wound Care Specialist RN for Outpatient Wound Care. “When a patient comes to our clinic for evaluation, they are given a dedicated appointment to thoroughly go over their medical and surgical history, medications and nature of the wound.” Switching over to the inpatient care team, they operate like a well-oiled assembly line, navigating different daily assignments with precision and flexibility. “On the inpatient side, our day starts in our office with triaging our consult list; after the triage process is completed, we get our assignments, which can consist of wound vacuum-assisted closure (VAC) patients, follow-up patients, ostomy education patients and new wound consults,” said Megan Uy, Advanced Wound Care Specialist RN for Inpatient Wound Care. “In the case of patients requiring wound VAC changes, we consider what kind of pre-medication for pain that they need. Although some patients may be seen on a time schedule, the day ends up flexible as patients are being seen by other specialties. This flexibility also benefits the patients, making them feel more empowered with their care.” “Each day in the inpatient setting, we get to our office and sort through all the new consults that came in overnight, and the charge nurse makes the assignment for the day,” added Madison Arlin, Advanced Wound Care Specialist RN for Inpatient Wound Care. “After the assignment is completed, each nurse is responsible for researching their patients and organizing their day, typically by priority – wound VACs and ostomies usually take top priority.” Now, how do these treatments actually work? This specialized field handles advanced methods of treating each condition, including: Biological skin substitutes Surgical debridement Advanced wound dressings Negative pressure therapy Pre-ostomy markings and education Offloading techniques, such as padding or dressing “Before starting treatments, we communicate with our nurses and providers to make sure that the patient is comfortable prior to wound care,” said Dianna Seo, Advanced Wound Care Specialist RN for Inpatient Wound Care. “After we see the patient, if there is a need for escalated care, we contact the provider for additional testing or consults. We continue to follow-up on patients that have severe wounds, wound VACs and ostomies.” In the hands of the Wound Care team, patients exit our hospital walls not only restored but also empowered, set on a trajectory for long-term healing. Your Expert Care Guides No matter the case or the severity of the wound or condition, patient care, comfort and communication always come first – before, during and after treatment. “Many of our patients have chronic needs, so we end up seeing them for several months, if not years in some cases; we stay up to date with their specific psychosocial needs and help remove barriers that would prevent their wounds from healing,” said Samantha Moore. “I enjoy knowing that my positive attitude can improve our patients’ days,” added Maddie Pauley, Patient Access Representative for Outpatient Wound Care. “When they’re routinely coming to appointments they might not enjoy, hearing them praise our team and give their thanks is one of the most rewarding feelings.” As a wound care patient, there can be a lot of unknowns when beginning their care journey. However, these team members carefully walk each patient through every step from beginning to end. “When we go to see a wound care patient, our team is very consistent about explaining to the patients what our role is and what we plan to do with their wound, and then we continue to actively communicate throughout wound care each step that we are doing as we are doing it,” said Madison Arlin. “We also encourage some of our patients to listen to music that they enjoy during the wound care, or we will cover their eyes with a cloth if they request so that they don't have to see their wound. Sometimes, we will ask the family to stay at the bedside to hold their family member's hand.” Education is crucial to ensuring each patient knows what to expect in order to care for their wound and understanding the stages of healing. Fortunately, this team is well-versed in the world of wound wisdom. “A lot of education is provided on the type of dressing we are applying, and if the patient is going to be performing their own dressing changes, we will go over the entire change with them and provide supplies for discharge,” said Megan Uy. “Additionally, there will be written instructions in their discharge paperwork. In the cases of wound VAC dressing changes, each step is explained to the patient before doing it, and we also go over discharge options and expectations.” “As a clinician who sees a lot of patients prior to having their ostomy placed (pre-surgical marking), one of the most important things we do is first sit with the patient and/or caregivers and talk about their fears, concerns, questions and goals,” said Samantha Moore. “We provide a lot of emotional support and education, helping identify community resources. For our wound patients, we spend a lot of time educating our patients/caregivers about how and why their wounds occurred. We try to connect with them on a personal level and help them identify ways to help their wounds heal.” To see a patient’s care journey from the second they enter through our doors to the moment they return home is one of the most rewarding feelings for the Wound Care teams. In fact, they’ve had the pleasure of treating patients for years and seeing their wounds almost completely heal. The team collectively values the successful healing journeys of their patients as their proudest achievement. “One of our team's greatest accomplishments was being able to see one of our long-term patients discharged with nearly resolved wounds,” said Megan Uy. “This patient had been in our care on-and-off for the past year with many hospitalizations and had complicated high-output enterocutaneous fistulas within his wound bed. These were incredibly hard to keep a dressing on successfully, and he often had issues with the dressing leaking. Eventually, we got a dressing that could remain intact until his next scheduled dressing change, and he was able to get surgery that fixed his fistulas. Being able to see him recover and heal his wounds was a very large accomplishment for us.” The admiration and compassion this team has for their patients also extends to each other. The cohesive way they work together only further benefits their patients, offering the best-possible collaborative care. “We have extremely skilled clinicians in our group that are not only incredible in the work that they do and the patient care that they provide but are also enjoyable to work with as well,” said Geane Weaver, Advanced Wound Care Specialist RN for Inpatient Wound Care. “There is something to be admired in each and every one of my coworkers.” “Our team is very close and supportive of each other at all times,” added Madison Arlin. “I feel very lucky to work with such an amazing group of people. Our team is very proud of the work we do.” Fervently Fighting the Good Fight So, with the highly specialized nature of advanced wound care, how did these team members get inspired to join the Wound Care team in the first place? Well, for many of these devoted employees, their first exposure to caring for wounds took place on different units – sparking their interest in making wound care their full-time career. “Renown was the most welcoming towards me as a student nurse, and I liked that it was a teaching hospital,” said Madison Arlin. “I started in the General Surgical Unit (GSU) immediately after graduating nursing school and worked there for two years before transferring to wound care. I decided to apply to the wound team after watching the wound nurses do wound VACs and ostomy changes on the floor. I would ask them if I could watch, and I was always very fascinated by the wound healing process.” “Prior to joining the inpatient wound team, like Madison, I was also a bedside nurse in GSU,” added Geane Weaver. “Working on that floor, I was already exposed to a lot of patients that were requiring some kind of advanced wound care in one way or another. Working in the GSU, I also cared for a lot of patients that had wound VACs and ostomies. These patients make up a huge group of the individuals that our team sees on a regular basis, and they've always been intriguing for me, so naturally, wound care has always been on my radar.” For other team members, wound care has always been a point of curiosity throughout their education and career. From their very first exposure to this care area, they were hooked. “I was always curious about wound care even through my nursing school experience,” said Dianna Seo. “When I was working on the floor, I would trade to do wound care for patients. When I had time, I would follow wound care and help when I could. I joined the skin team which drove me to be increasingly involved with wound care. As soon as there was a job opening, I applied for the position. I worked in outpatient wound care for approximately four years and now inpatient for another four years. I have enjoyed all aspects of wound care and patient care.” “I had great clinical experience at Renown when I was in nursing school; I also was very interested in caring for trauma patients, and Renown being a Level II trauma center aligned with my interests,” added Megan Uy. “I began my nursing career in the GSU, but my dream job was always Wound Care. During my nursing school clinicals, I had the opportunity to watch some members of the wound team do wound VAC changes and thought it was incredibly intriguing and a great combination of utilizing the knowledge of anatomy and physiology while being creative with handicraft. A position opened on the team around the time I met the prerequisites to be eligible for the position, and luckily, I got it.” Our Wound Care team has achieved significant employee and departmental milestones over the past year, reflecting their dedication to enhancing patient care and overall process improvement. “We have had many accomplishments within the last year and are currently working on more to improve the hospital,” said Dianna Seo. “Madison Arlin won the DAISY Award for her great work with our patients. Megan Uy won Top Talent of the Quarter for helping a stranger. Ande Ferriera has worked tirelessly to improve our process improvement. Allie Saunders, as our leader, has worked to improve patient skin by getting new beds for Renown Regional. All our patients that have healed or are on their way to healing under our care is our greatest achievement that we as wound team is most proud of.” “We are constantly updating protocols, notes and orders for bedside nursing so that it is a more straightforward and seamless charting process,” added Madison Arlin. “We have representatives of different supply companies come and present new products that we think may benefit our patients better. Our wonderful tech has even updated our department site on Inside Renown so that the nurses always have references available.” Renown’s strong influence in the region – and the opportunity to give back to their community – was, and continues to be, a major draw for this team. “Since I can remember, Renown has always been the most prevalent healthcare name for my family and has always taken the most amazing, thorough care of my loved ones,” said Maddie Pauley. “I have always wanted to work somewhere I could help people, and starting at Renown has really opened my eyes into how much of a difference each one of us can make.” Our Wound Care department’s success stories and proactive approach not only reflect their passion for healing but also inspire a ripple effect of positive change throughout our health system. They proudly exemplify a shared commitment to enhancing the well-being of all patients under their care. “Being part of Renown and part of this team has been my blessing; I get to do a job I love with people that love it too,” closed Dianna Seo.
-
Foods to Avoid When Taking Heart Medications
Did you know certain medications can interact with everyday food and drink? We asked VP of Pharmacy Services Adam Porath how to take these important medications safely. One in five Americans between the ages of 40 and 75 are currently taking a statin drug to reduce their cholesterol level or to prevent atherosclerosis (hardening of the arteries). Many others also take anticoagulants (blood thinners) to prevent blood clots from forming, which can increase the risk of stroke. Adam Porath, VP of Pharmacy Services at Renown Health, explains how to safely take these medications. What is a statin? A statin is a drug that can lower cholesterol by helping your body absorb cholesterol or by blocking a substance your body needs to make it. The American Heart Association cites a global study reporting the benefit of statins to help reduce heart attacks and strokes. Common statins include atorvastatin (Lipitor), pravastatin (Pravachol), rosuvastatin (Crestor) and simvastatin (Zocor). Which foods or drinks should be avoided while taking statin drugs? Grapefruit juice is the only food or drink that has a direct interaction with statins. Statins do not directly interact with any food but people taking statins should moderate their intake of saturated fats to help lower their LDL cholesterol and overall risk of cardiovascular disease. What is a blood thinning drug? Blood thinning drugs, such as warfarin, rivaroxaban (Xarelto), apixiban (Eliquis), dabigatran (Pradaxa) and edoxaban (Savaysa), are used to prevent stroke. Which foods or drugs should be avoided while taking blood thinning drugs? If taking warfarin, alcohol and cranberries (including juice) should be avoided. Patients taking warfarin should be aware of foods that contain Vitamin K (green leafy vegetables) and try to maintain a consistent diet of these foods. Warfarin interacts with many over the counter and prescription medications. Patients should consult a pharmacist when starting, stopping, or changing doses of any medication when taking warfarin. Also, patients taking any blood thinning medication should avoid over-the-counter pain relievers (i.e. aspirin, ibuprofen, etc.) How do I know whether to take my medication with food or not? Consulting with a pharmacist is the best resource to determine if a medication should be taken with or without food. In general, all statins and blood thinners can be taken with or without food. The only exception is Xarelto (rivaroxaban), which should be taken with the largest meal of the day If you are a Renown patient you can also review your prescriptions online, request a refill or ask a question via MyChart. With MyChart, you can access all your healthcare information securely 24/7.
Read More About Foods to Avoid When Taking Heart Medications
-
Trends in Cardiovascular Medicine Conference
Heart disease continues to be the leading cause of death in America and doctors face many challenges treating this and associated heart and vascular conditions. Renown is hosting a three-day conference to discuss the latest in cardiac care. Trends in Cardiovascular Medicine Doctors and healthcare providers across the region are gathering for the 33rd Annual Trends in Cardiovascular Medicine Conference Nov. 3rd – 5th at the Everline Resort & Spa in Olympic Valley, California, hosted by Renown Institute for Heart & Vascular Health and the Nevada Academy of Family Physicians. The three-day conference educates primary care providers, nurses and all other physicians and healthcare personnel interested in the most recent advances and current established guidelines for the diagnosis, treatment and prevention of cardiovascular disease, diabetes mellitus, stroke and diseases or problems associated with heart disease. It is also a chance for medical providers to ask first-hand questions on a variety of trending topics ranging from the practical evaluation and management of obesity to interpreting echocardiograms in primary care. The conference objectives include: Identifying clinical clues suggesting a diagnosis of cardiac amyloidosis. Gaining a better understanding why the differential diagnosis and patient history is key to evaluating patients with syncope. Assessing the accuracy and effectiveness of various tests and tools used in atrial fibrillation screening. Determining the appropriate diagnosis of pulmonary hypertension. Describing the evolving lipid management landscape. For a complete conference schedule, more information or to register for this conference, visit: renown.org/trends.
Read More About Trends in Cardiovascular Medicine Conference
-
6 Signs of Heart Failure
Heart failure is a serious medical condition that occurs when the heart is unable to pump blood effectively, leading to a variety of symptoms and potential complications. Although there has been progress made in the treatment of many forms of heart disease, heart failure continues to be a prevalent and life-threatening condition – nearly 6.2. million adults in the U.S. have heart failure. Recognizing the signs of heart failure is crucial for early detection and timely intervention. We talked to Ruth Skinner, APRN at the Renown Institute for Heart & Vascular Health, about recognizing common signs and symptoms of heart failure. Heart Failure Signs and Symptoms The symptoms of heart failure may be subtle and can be mistaken for normal signs of aging. Common symptoms of heart failure are due to extra fluid or congestion – typically starting with congestion of the lungs, then moving to different parts of the body. Common heart failure symptoms include: Breathing Difficulties (Dyspnea): One of the hallmark symptoms of heart failure is shortness of breath during daily activities and having trouble breathing when lying down. Fatigue and Weakness: Because heart failure can lead to reduced blood flow to the body’s tissue, patients may find themselves becoming tired and weak even during routine activities. Swelling (Edema): Fluid retention in the body can cause noticeable swelling. Weight gain along with swelling of the feet, legs, ankles or stomach is often a key sign of worsening heart failure. Rapid or Irregular Heartbeat: Heart failure can disrupt the heart's electrical signals, causing irregular heartbeats (arrhythmias) or a rapid heartbeat (tachycardia). These can be felt as palpitations or fluttering sensations in the chest. Persistent Cough or Wheezing: Fluid buildup in the lungs triggers a persistent cough, sometimes accompanied by pink or white mucus. Loss of Appetite or Nausea: Heart failure can affect blood flow to the digestive system, leading to symptoms like loss of appetite and nausea. If you or a loved one experiences any of the above signs and symptoms, it’s important to seek medical attention promptly.
-
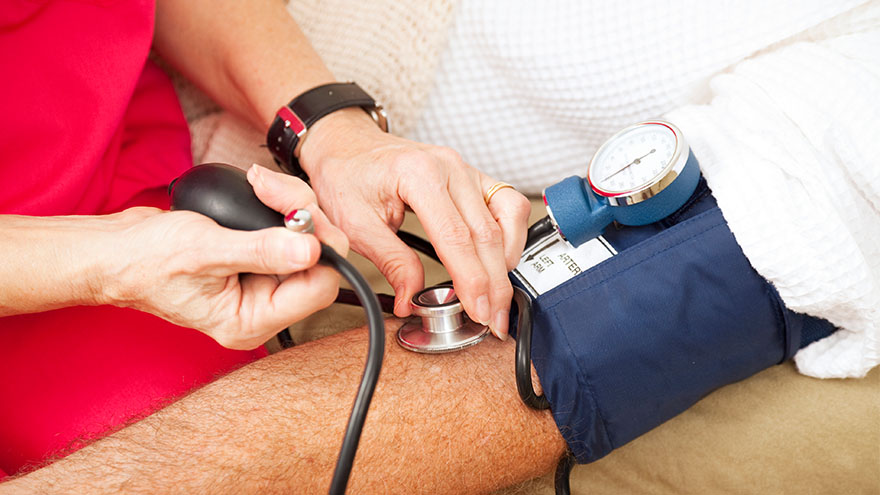
Managing Your Uncontrolled High Blood Pressure
Renown Health, the region's leading cardiology care provider, is offering a clinical trial for eligible patients struggling to control their high blood pressure. Nearly half of adults (119.9 million) in the United States have hypertension, or blood pressure that is higher than normal. Hypertension can put you at risk of other life-threatening disease, such as a heart attack or stroke. There are methods that cardiologists use to manage high blood pressure, but only 1 in 4 adults with hypertension (27.0 million) have their blood pressure under control.* Some patients with high blood pressure experience resistant hypertension, which does not respond well to multiple antihypertensive medications given at the same time. This means that there are many important opportunities for healthcare professionals to explore new ways to treat hypertension. At Renown Health, we lead the region in cardiology care with our technological expertise and patient-centered approach. That is why our cardiology team is partnering with the Renown Research Office to offer the RADIANCE Continued Access Protocol (RADIENCE CAP) clinical trial to eligible patients. RADIANCE CAP is a non-randomized study designed to allow for continued access to ultrasound renal denervation therapy via the Paradise System, and to allow for the on-going collection of safety and effectiveness data in patients with uncontrolled hypertension despite the prescription of antihypertensive medications. The body’s complex communication system between the brain, heart and kidneys can sometimes become overactive, increasing your blood pressure through messages in the nervous system. Renal denervation is a minimally-invasive procedure which reduces activity from the nerves in your kidneys to lower blood pressure. This is the third in a series of renal denervation clinical trials Renown Health has offered to patients with resistant hypertension over the last several years, with over 40 local participants. “All the participants that I have had the pleasure to work with on these studies are very excited and grateful to have this option for helping control their blood pressure” states Lisa English, Lead Clinical Research Coordinator for Cardiology studies at Renown Health. “I love getting to know each one of them and helping on their healthcare journey. We have an amazing team of providers and staff at Renown that go out of their way to make patients experiences positive and the studies successful.” Dr. Michael Bloch, Cardiologist and Principal Investigator for the RADIANCE CAP study at Renown Health’s Institute for Heart and Vascular Health adds, “Despite lifestyle modifications like diet and exercise and the widespread availability of effective and well-tolerated medications, approximately 50% of all people with hypertension have inadequate blood pressure control putting them at risk for stroke, heart failure and kidney disease. As a one-time durable procedure, renal denervation with the Paradise endovascular system from ReCor Medical, Inc. may help millions of patients improve their blood pressure control without necessarily needing to increase their medications.” Our teams of expert providers and researchers are here to support you on your healthcare journey. Talk to your provider about the RADIANCE CAP clinical trial at your next appointment to see if participation may be right for you.
Read More About Managing Your Uncontrolled High Blood Pressure
-
A Therapist's Tips to Prevent and Manage Osteoporosis
Want to know more about osteoporosis and osteopenia? We'll dive into these conditions and give you some handy tips on preventing future problems and taking care of your bones. What is Osteopenia? Osteopenia (low bone density) is the initial stage of bone mineral density loss, which can eventually progress to osteoporosis if steps are not taken to prevent it. What is Osteoporosis? Osteoporosis is a condition that weakens our bones. While it literally means “porous bone," it doesn’t mean that our bones are doomed to succumb to the changes that can happen to us silently over time. Our bones are living tissues that are constantly breaking down and remodeling themselves. Osteoporosis and osteopenia are typically diagnosed by testing bone mineral density using scans that your primary care provider can easily order. This is important testing because it dictates your risk of breaking a bone in common areas like your hip, wrist or spine. It also helps set the stage for talking with your healthcare team to develop a treatment plan. Most people will reach their peak bone mass in their mid to late twenties. There are several factors that increase our risk of osteoporosis or osteopenia as we age, such as menopause, genetics and other lifestyle factors. However, there are several things you can do to mitigate this breakdown and assist your body in the constant remodeling it does to our bones. 3 Controllable Factors to Build Strong Bones 1. Talk to your primary care provider They can go over a plan and prescribe things such as vitamin D, calcium and medications that can help if you are at risk or have osteoporosis or osteopenia. 2. Maintain a healthy diet Talk to a dietician if you need further help as they can be an invaluable resource to develop a plan. Eat foods rich in calcium, vitamin D and vitamin C. These assist with the rebuilding of bone. Examples include but aren’t limited to leafy greens, legumes, salmon and healthy dairy products. Don’t smoke — it directly correlates with a decrease in bone mass. Smokers also take longer to heal from a fracture. Limit alcohol to two to three beverages per week. Alcohol interferes with the production of vitamins needed to absorb calcium and the hormones that help protect bones. 3. Exercise Talk to your primary care provider to get a referral to physical therapy if you need help with exercise. Our bones adapt to the stresses we put them through. Therefore, exercise should be tailored to putting the right stress on our bones. There is good quality research that most exercise is safe when dealing with less bone mineral density. The exercises should be progressively challenging and increase the load for resistance and weight training at least two to three days a week. Examples include squats, step-ups, chest presses and rows. Exercises higher in velocity will lead to more power and bone adaptation. Examples include quicker push-ups, marching and quicker walks. Exercises that are weight-bearing will lead bones to adapt to the stress placed on them. Movements such as mini stomps, step-ups, jumping, jogging and so forth may be used depending on how your body tolerates these things to really stimulate bone adaptation. There are aspects of aging and bone health we can’t control, but we can take steps to minimize the chances of bone loss and osteoporosis. Talk to your healthcare team to determine your risk and don’t forget to show your bones a little TLC – you’re going to need them.
Read More About A Therapist's Tips to Prevent and Manage Osteoporosis
-
What Is an Echo-Tech?
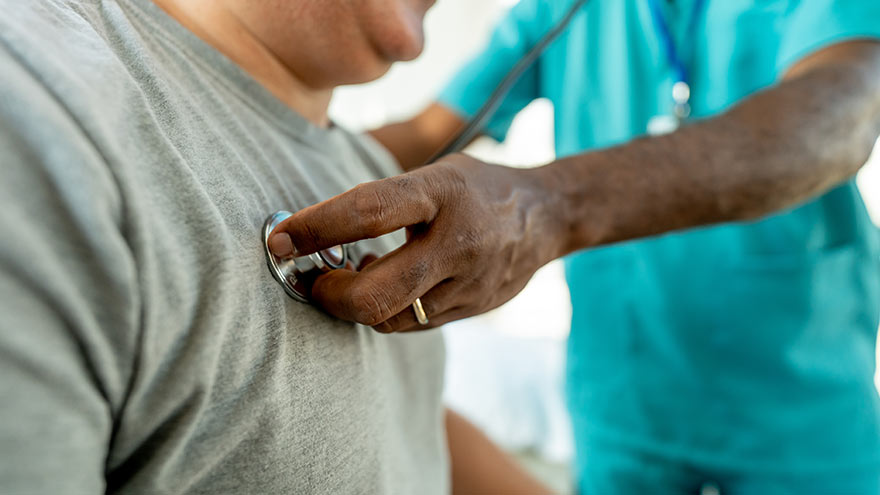
When it comes to our heart, keeping this vital source of life in tip-top shape is of utmost importance. Echo technologists or echocardiographers, otherwise known as "echo-techs," are charged with that mission, providing critical information that leads to life-saving interventions to keep our hearts beating strong. Adrianne Little, echocardiographer at Renown Health, breaks down the echo-tech's role in the health system, the educational path it takes to get there and the unique perks that come with the profession. What does an echo tech do? “Echo techs play a key role in the diagnosis and treatment of patients,” said Adrianne. “We are members of the cardiovascular imaging team that perform ‘heart ultrasounds’ or echocardiograms. Although we are most commonly known as echo techs, our official title is either ‘cardiac sonographer’ or ‘echocardiographer.’” Echo techs use imaging technology and sophisticated ultrasound equipment to produce images of the heart. These images show how well the heart functions, as well as the valves, chambers and blood flow. Echocardiograms are used to diagnosis and treat a variety of heart conditions such as murmurs, arrhythmias and heart failure. At the end of the day, the main goal of echo techs is to help our cardiovascular team provide the quickest and most accurate diagnoses to help with patient management and help them receive the highest standard of care. “When it comes to looking at the heart, we are part of the front-line team," said Adrianne. “We provide real time critical information that leads to life saving interventions down the road.”
-
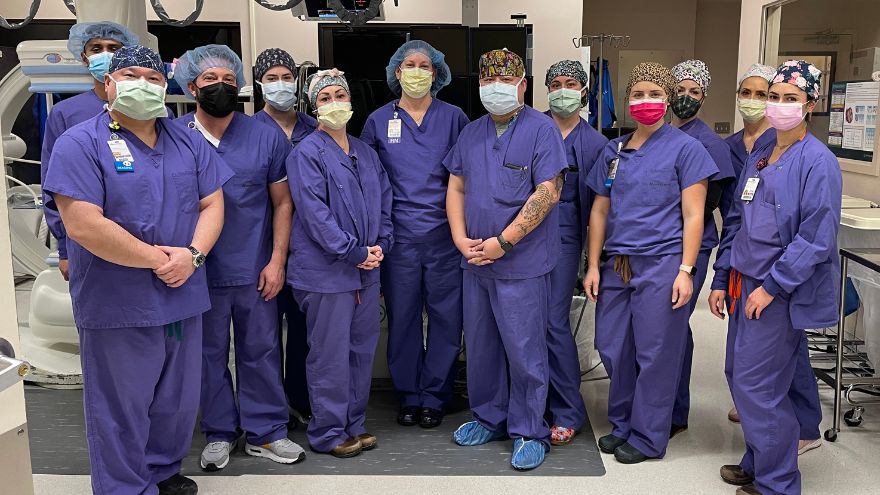
Department Spotlight Cardiac: Catheterization Lab
February is American Heart Month, but our incredible heart heroes are here to serve you all year long. So please join us in honoring the Cardiac Cath Lab team at Renown Health! At the core of who we all are, we find the heart: one of the largest sources of life that gives us the blood and oxygen we need to live full and healthy lives. When the heart doesn’t function to the best of its ability, a delicate approach led by cardiac experts might be necessary. These individuals can not only save lives but also help facilitate a higher quality of life. The team entrusted to protect that vital source of life includes the hard-working and talented individuals in the Cardiac Catheterization Lab (a.k.a. “Cardiac Cath Lab” or “Cath Lab”) at Renown Health. These team members are known for their expertise, precision and quick-thinking in emergencies. When it comes to the function of your heart, you are in the best hands with this team. Their passion for Renown’s mission of making a genuine difference in the health and well-being of the people they serve is a testament to what they do every day. Cardiac Champions Whether the procedure is emergent or planned, the Cardiac Cath Lab wears many different hats. The team is a well-coordinated group of nurses, imaging professionals, electrophysiology technologists, interventional technologists and more who band together to provide a diverse array of services, including stent placements, pacemakers, balloon pumps, interventional angioplasties, TAVRs and of course, catheters. “A day in the life in the Cath Lab can go various ways,” said Erica Drummer, RN at Renown Health. “Every day, you are either a part of the electrophysiology team, doing cardiac ablations and placing devises such as pacemakers; the structural heart team, which includes MitraClips for mitral regurgitation and TAVRs; or the heart catheterization team, which includes diagnostic angiograms, heart catheterizations, angioplasties and stents for clogged arteries.” With the wide variety of cases the team sees daily, an average day in the Cath Lab consists of many moving parts. “We handle cases from left and right heart catheterizations, where we can diagnose and fix the artery right then, to electrophysiology cases like heart ablations and pacemaker implants, all the way to emergency STEMI (heart attack) patients,” said Michael Blankenship, Electrophysiology Technologist at Renown Health. “We do so many things in the Cath Lab,” added Laurel Douglas, RN, Imaging Manager at Renown Health. “We ensure we have 24/7 coverage for emergencies, as we often have to act at a moment’s notice to care for emergent situations.” Many of those emergency situations involve heart catheterization. If someone has a heart attack, the team immediately steps in to place stents to open the coronary arteries that are causing the attack. If a patient’s heart needs any assistance during an emergency, the team can place devices such as Impella (temporary ventricular support) or intra-aortic balloon pumps. Renown is a major advocate for advanced medical technology, and the Cardiac Cath Lab team embraces these technologies to perform life-saving procedures, all while working together as a cohesive unit. “We work amongst each other to ensure sterility, safety and the best outcome for each patient,” said Zohra Benbrahim, RN at Renown Health. “We try to fit in as many cases as possible into the workday, and sometimes after hours, so patients can get the care they need.” “Each team usually has 3-4 members, and each member has a critical job to carry out in order to implement excellent cardiac care,” added Erica Drummer, RN. “Many of our patients tell us that we all work well together, and I couldn’t agree more. We have become like a well-oiled machine or a NASCAR pit crew.” Naturally, patients undergoing any heart procedure might feel frightened and anxious. Never fear – the compassionate Cardiac Cath Lab team is here to ease those fears throughout each patient’s entire visit. Their main solution? Communication. “Being a patient in the Cath Lab can be daunting,” said Erica Drummer, RN. “When we have patients who may feel scared or have concerns, we try our best to connect with them, keep them informed and educate them on the procedure and the step-by-step process, including what they may feel before, during and after.” “Overall, we try to keep spirits light,” said Zohra Benbrahim, RN. “Our team is excellent at explaining the procedure as it is happening. We also advocate for comfort throughout the procedure, which helps tremendously with anxiety, including giving patients warm blankets and music of their choice!” Our experts in the cardiac Cath Lab make sure that no stone goes unturned when it comes to optimal heart function for every patient. Together, the team mends hearts and saves lives, day in, day out. A Growth Mindset Always learning, always improving, always reaching new heights – that's the Cardiac Cath Lab team. This team’s accomplishments speak for themselves on both a local and national scale. “Over the years, we have achieved several milestones, including becoming a STEMI Receiving Center, gaining our Chest Pain Center Accreditation (which is achieved by Cath Labs who provide emergent percutaneous coronary intervention for heart attack patients 24/7) and having our accredited electrophysiology program,” said Laurel Douglas, RN. “We also offer services that other facilities do not offer. We have brought in several new procedures to the Cath Lab over the years. This is impactful, as the community members get to stay here for treatment.” The Cath Lab team is anything but ordinary. There is never a dull moment in this department, and despite an ever-growing caseload, the team is always ready to rise to the challenge and continue pushing to surpass the average. “I am so proud of my team for providing care for such sick patients,” said Zohra Benbrahim, RN. “We never really know how the day is going to go because emergencies happen, and things always change. Recently, we had a record high volume of cases, and my team powered through these busy weeks like champs.” “We strive to get our STEMI door-to-balloon times at or below 60 minutes,” added Erica Drummer, RN. “Door-to-balloon time refers to the time from when a patient arrives in the ER to the time the Cath Lab has a catheter guide wire crossing the culprit lesion in the coronary artery that is causing the heart attack. The national average (and current guideline) is 90 minutes, so our 60-minute time is a notable accomplishment for us.” The importance of staying on top of your heart health comes center stage during American Heart Month, which is a prime opportunity for our cardiology professionals to educate the community and help them grow their cardiac knowledge. The cardiac quality team participates in community events throughout the month (and beyond!) to raise awareness for cardiac health. The team also outreaches to other health systems and healthcare partners to highlight what Renown has to offer in the way of heart care. Each Cath Lab team member always reminds patients about lifestyle choices and diet changes that can improve cardiovascular health, and they take this outreach with them all around Renown Regional Medical Center as well, walking through the hallways promoting many different ways of living a heart-healthy life. The journey continues! The team will soon welcome a new Cardiac Cath Lab at Renown South Meadows Medical Center. The new lab will allow our experts in heart care to treat patients at our South Meadows location experiencing a heart attack and needing immediate intervention to open vessels in their hearts. The team is looking forward to embracing even more access to emergent cardiac care for our community at large. Learn more about how Renown is building more ways to care for our community. Now Hiring for Heart Heroes Those looking to join a caring, committed and tight-knit group of cardiac care professionals will be in good company with the Cath Lab team. According to the members of this department, being a quick-thinking, dependable team member is key to predicting a successful Cath Lab professional. “A good coworker communicates with everyone and is able to be flexible when things get hectic,” said Zohra Benbrahim, RN. “Our team stays so close with each other because of everyone’s ability to recognize where help is needed. Especially in the Cath Lab, it is important to be always aware of the patient’s vitals and clinical presentation so you can speak up if you notice changes. There are always new procedures or products coming out that become integrated into our practices, so it’s also good to welcome new policies and be adaptive.” “We are a small team, and everyone sees each other as a friend,” added Laurel Douglas, RN. “We all know we will need help at some point, whether it be covering an on-call shift or helping during a procedure, so we all help each other. Teamwork and positive attitude are really what makes you a good team member.” Not only are these individuals dedicated to impacting the lives of patients with the very organ that beats life into them, but they also are devoted to Renown – and it shows. “I started working for Renown when I was 19 years old, and Renown was the medical system I went to for care; as I spent more time working here and becoming a part of the community, I could not see myself working anywhere else or getting care at any other hospital,” said Zohra Benbrahim, RN. “I truly believe Renown provides the best care and best serves the growing community of northern Nevada.” The Cath Lab team members agree that Renown is a great place to both start and continue your career. Many of them have taken advantage of Renown’s training and educational opportunities, which in turn have helped them expand their knowledge to better serve the community. “I chose to work at Renown because it gave me the place to grow in my career and experience different avenues within my career,” said Michael Blankenship. “I first started off as a student here, and I quickly realized that everybody I worked with genuinely cares for our patients. I started off in x-ray seeing patients and eventually did rotations up in the operating room, and I got hired full time in the Cath Lab. After a short time being here, I was crossed trained in the electrophysiology lab, where I furthered my knowledge in my career.” This dynamic department is actively hiring, and many open positions are sign-on bonus eligible. The team cannot wait to welcome you to their, as Erica Drummer puts it, “well-oiled machine.” “Being a Cath Lab nurse is very rewarding, especially when you’re able to be a part of a team that can save someone’s life,” Erica closes.
Read More About Department Spotlight Cardiac: Catheterization Lab
-
Learn How to Manage Lymphedema
Katherine Bunker, Physical Therapist and Certified Lymphedema Therapist (PT, DPT, CLT) at Renown, discusses how patients can manage lymphedema with changes to daily routines along with diet and exercise. Lymphedema is a condition that affects millions of people around the world. It is a chronic and progressive disorder that results in swelling of the arms, legs, or other parts of the body due to an accumulation of lymph fluid. Lymphedema can occur because of cancer treatments, surgery, or other medical conditions. Managing Lymphedema Treatments to help reduce symptoms such as pain, swelling and discomfort associated with lymphedema can include compression garments, exercise, skin care, manual lymphatic drainage and pneumatic compression. The goal is to avoid triggering the onset of lymphedema. Lymphedema can present itself immediately after surgery or radiation. It can appear months later or even years later. There are many factors that influence the development of lymphedema which is why prevention is so important. If you have had injury or disruption to your lymphatic system, then: Avoid injuries to the skin near the affected area. For example: wearing gloves during gardening, using bug spray to ward off mosquitos, covering your limbs while playing with pets, keeping nails clean and avoiding cutting too close to cuticle, utilizing electric razors at the armpit (instead of a traditional razor)., Avoid blood pressure readings to the affected limb or request blood pressure to be taken manually, not by a machine. Avoid heat like saunas, hot tubs, sunburns, hot packs, and even massages. Avoid tight jewelry like rings or bracelets, which can be too tight.
-
Getting to the HEART of Research
In February, we think about hearts not just in honor of Valentine’s Day but because it is American Heart Association Month. This is a great reminder to focus on our personal cardiovascular health. Renown Health helps patients think about their heart health with our world-class providers and cutting-edge treatments through our Cardiovascular Clinical Trials. “Research serves a vital role in the future care of cardiovascular diseases. Being involved in research will help our medical community to further discover new treatment plans in our quest for life preservation and extension,” Dr. Thomas To, Cardiologist and Researcher at Renown Health. For example, let’s talk about atherosclerosis. When our hearts are healthy, they are a strong muscle that pumps our oxygen-rich blood through our coronary arteries. Over time, cholesterol and fats can build up in our arteries. This is a condition known as atherosclerosis. This type of plaque buildup in the arteries can lead to a heart attack or stroke if not properly managed. If you are experiencing chest pain or discomfort, shortness of breath or pain in areas of the upper body, these can be the warning signs of a heart attack, and you should call 911. One contributing factor to atherosclerosis is elevated lipoprotein(a) levels and the accumulation of cholesterol in the arteries, which increases the likelihood of a heart attack or stroke. Lipoprotein(a) is tested separately from the standard panel that is completed for cholesterol management, and while your total cholesterol levels may be in a healthy range, lipoprotein(a) levels can still be elevated. "Increasingly we are realizing that lipoprotein(a) levels can be used as an important assessment in more carefully delineating an individual's risk of future cardiovascular events and treatment targets" said Dr. Michael Bloch, Lipid Specialist and Researcher at Renown Institute for Heart and Vascular Health. While it is clear that elevated lipoprotein(a) contributes to atherosclerosis, there are currently no approved medications for reducing cardiovascular disease risk through reducing lipoprotein(a) levels. This is why Renown Health’s Research Office is proud to offer a phase III clinical trial, called the OCEAN(a) study, to our patients with elevated lipoprotein(a) levels as a care option for management of their heart disease risk. Our teams of expert providers and researchers are here to support you on your healthcare journey. “I am thrilled to be able to be part of this study and bring opportunities like this to our patients. The highlight of my day is getting to hear life stories from my patients during our study visits,” Lisa Preciado, Primary Clinical Research Coordinator for the OCEAN(a) study said. Join us in raising awareness around American Heart Month by talking to your provider about lipoprotein(a) at your next appointment. At Renown Health, our goal is to make it easy for patients to access clinical research as a care opportunity where patients can access a variety of standard care treatment options for their health condition or choose to participate in a clinical trial. For more information about clinical trial opportunities available to you or to ask any questions, contact the Renown Research Office at Renown-CRD@renown.org or 775-982-3646.
-
Your Top 5 Questions about TAVR Answered
Your heart is the muscle in charge of pumping blood to your entire body. This vital organ is made up of chambers, valves and blood vessels. Your heart valves work similarly to a one-way door: they open and close, controlling blood flow in the correct direction through the heart chambers. For patients who have been diagnosed with a heart-related condition like aortic valve stenosis (narrowing), it is important to know treatment options. Most might think open-heart surgery is the only way to treat a heart valve, but many hospitals, including Renown, also offer a minimally invasive procedure called a Transcatheter Aortic Valve Replacement (TAVR). Dr. Abhilash Akinapelli of Renown Institute for Heart & Vascular Health shares his answers to the top five TAVR questions: 1. What causes aortic valve stenosis? Aortic valve stenosis can be caused by a variety of factors. The main reasons being wear and tear of the valve due to aging; genetically abnormal heart valve (bicuspid aortic valve); long-standing high blood pressure; and other reasons like radiation exposure. 2. Am I a candidate for TAVR? Renown’s heart care teams are made up of your primary care provider, cardiologist and cardio thoracic surgeon. They will evaluate if patients are a good candidate for the TAVR procedure by performing a variety of screenings and tests. Some of these include: Echocardiogram Electrocardiogram (ECG or EKG) Chest X-ray Exercise tests or stress tests Cardiac computerized tomography (CT) scan Cardiac catheterization 3. What are the advantages of the TAVR procedure? The Transcatheter Aortic Valve Replacement (TAVR) procedure is much less invasive than open heart surgery, otherwise known as a Surgical Aortic Valve Replacement (SAVR). Patients can typically return to their normal lifestyles within a week after leaving the hospital. During the TAVR procedure, a stent valve mounted on a balloon is advanced to the heart through the blood vessels in the groin without any incision. Once in position, the balloon will be inflated to firmly expand the new valve inside the diseased old valve, pushing it away to the sides. Once the new valve is in place, it begins working immediately and the deflated balloon is removed. The surgical procedure is approximately one hour long. Patients can get up and walk after four hours and will be discharged the following day if no complications arise. Compared to a SAVR, recovery time is much shorter and less risky for patients above the age of 75. A big advantage for anyone who fits under the criteria for a TAVR. 4. Is the procedure painful? The TAVR procedure is not surgery, but you will still be asleep during the procedure. Since no incision is made, it is essentially a painless procedure. Patients may experience slight discomfort such as aches and pains at the entry site of the catheter. 5. Can I have an MRI and X-rays done after having a TAVR valve? Yes, patients can have MRI scans and X-rays after TAVR. For further questions and information about the TAVR procedure, please consult with your Renown heart care team at 775-982-2452 or through MyChart.
.png?rev=5ac90884d83d45468d7e3a5389920ff1)