Buscar
-
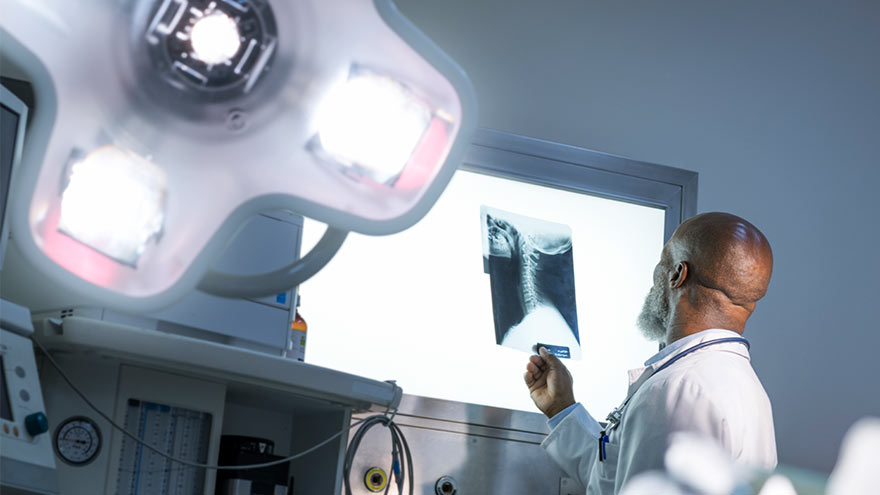
Optimizing Mammogram Screenings: A Genetic Approach to a Personalized Screening Schedule
Breast cancer screening has long been a cornerstone of women's healthcare. With 1 in 8 women diagnosed with breast cancer in their lifetime1, the United States Preventive Services Task Force (USPSTF) has developed screening recommendations to help detect early-stage cancer. Notably in 2023, the USPSTF revised the recommended age for biennial mammogram screenings for women with average risk to start at age 40 instead of 502, estimated to result in 19% more lives being saved3 by starting screening earlier. While initiating screening at an earlier age offers advantages to a wide demographic, concerns about the potential of over-screening prompted research into the feasibility of identifying women with lower breast cancer risk who could safely delay mammograms. While guidelines address high-risk individuals, a notable gap exists in providing recommendations tailored to those at lower risk. To gain insight into a patient's risk level, physicians are able to utilize genetic testing to understand an individual's genetic makeup, providing precise insights into their predisposition to various health conditions, including breast cancer. Armed with this genetic information, healthcare providers could craft tailored screening strategies that align with an individual’s specific risk profile. This genetic risk-based approach underscores the value of genetics in individualizing the onset of screening to help avoid over-screening and its associated costs. Surprisingly, genetic information is not currently being widely utilized to identify women at risk of breast cancer or other diseases in clinical practice, despite its potential to make a significant positive impact for patients. A recent retrospective analysis of 25,591 women from the Healthy Nevada Project4 sheds light on the potential benefits of this genetic risk-based approach. The study classified 2,338 (9.1%) of these women as having a low genetic risk for breast cancer. What's remarkable is that these women exhibited a significantly lower and later onset of breast cancer compared to their average or high-risk counterparts. This finding suggests that it might be safe for low-risk women to delay mammogram screening by 5 to 10 years without compromising their health.
-
La detección temprana es clave para sobrevivir al cáncer colorrectal
Colorectal cancer is the number two cancer killer in Nevada, only second to lung cancer, yet it is also one of the most preventable. Still, in 2020, 20.7% of Nevadans said they had never been screened for this deadly disease, according to the Nevada Cancer Coalition. At the start of the COVID-19 pandemic, unfortunately many healthcare services were halted, including colorectal cancer screenings. Those delays in screenings can lead to delays in diagnoses of colorectal cancer, resulting in poorer outcomes. Per the American Cancer Society, if colorectal cancer can be found early the relative 5-year survival rate is approximately 90%. Screening is key, and it is important to engage in preventative care. Even if you have no personal or family history of colorectal cancer, ask your doctor about colorectal risk factors and when to start screening, and if you’re up to date on your screenings, talk to loved ones and make sure they are too. According to the American Cancer Society, most colorectal cancer cases are found in those without a family history. This month let us help raise awareness for colorectal cancer and the importance of routine, life-saving screenings. To learn more, we spoke to Renown Health oncology nurse Christina Alsop, APRN. What is Colorectal Cancer Colorectal cancer is a disease in which the cells in the colon or rectum grow out of control. It usually forms from precancerous polyps, or abnormal growths, in the colon or rectum, which can become malignant without presenting any symptoms. How do Screenings Work Screening tests like stool tests, colonoscopies and others can detect these precancerous polyps, so they can be removed by a physician before turning into cancer. Screening tests can also find colorectal cancer early, resulting in better treatment outcomes. As of 2021, the U.S. Preventative Services Task Force recommends adults begin colorectal cancer screenings beginning at age 45, through 75. Screening methods include a blood stool test, which needs to take place every year or a colonoscopy, which takes place every 5-10 years. Healthy Habits Can Help Stave Off Risk Routine screenings are the only way to determine colorectal health, yet some healthy habits may reduce your risk for colorectal cancer. These factors include maintaining a healthy weight, being physically active, eating a diet rich in fresh fruits, vegetables and whole grains, limiting alcohol intake and not smoking.
Read More About Early Detection is Key to Surviving Colorectal Cancer
-
Head, Neck and Oral Cancers: How You Can Spot and Treat Them
Head, neck and oral cancers account for just 3 percent of all cancer in the U.S. and can be hard to diagnose. Dr. Abhinand Peddada, radiation oncologist with the Renown Institute for Cancer, explains. While you likely don’t frequently hear about head, neck and oral cancers — they are significantly less common than many kinds of cancer — they can be extremely dangerous. One of the primary reasons: some symptoms mimic the common cold, making them difficult to detect without a medical professional. We asked Abhinand Peddada, M.D., radiation oncologist with the Renown Institute for Cancer, to break down the symptoms and lifestyle risks of these rare cancers. First off, what are some of the signs and symptoms of head, neck and oral cancers? Symptoms can vary based on where the cancer is. For example, throat cancer may show up as a persistent sore throat, while sinus cancer may present as soreness or pressure in the sinuses that doesn’t get better. Some other symptoms to watch may include: Swelling in the throat Painless swelling in the neck Red or white patches in the throat Hoarseness Bloody noses or blood in the mucus or saliva A new and unexplained lump or bump anywhere on the face, neck, mouth or throat Difficulty breathing Difficulty swallowing, chewing or moving the muscles in your face, neck, mouth or throat Bad breath, even with good oral hygiene Loose teeth Dentures or retainers that no longer fit Double vision Who is most at risk for head, neck and oral cancers? Both men and women can develop head, neck and oral cancers, but men are at almost twice the risk of women. People over the age of 40 are also at a higher risk, and these cancers tend to be more common in African Americans. Tobacco use — including cigarettes, cigars, pipes and chewing tobacco — is another risk factor. Tobacco is linked to 85 percent of head and neck cancers. Exposure to fumes and chemicals can increase your risk as well. We’re also seeing more HPV-related head and neck cancers in the U.S., so patients with HPV may want to watch more closely for symptoms. What about screening and prevention? Your dentist already looks for signs and symptoms at your regular dental checkups. Additionally, if you have one of these risk factors and are experiencing signs and symptoms, it’s a good idea to check with your doctor about possible screenings. To help prevent these types of cancers, try to minimize your controllable risk factors. This means quitting tobacco, watching your alcohol consumption and taking care of your oral hygiene by brushing and flossing regularly. We also recommend the HPV vaccination for both boys and girls starting at age 11. By vaccinating at an earlier age, one is less likely to develop oral HPV. What do diagnosis and treatment look like for these cancers? At Renown Institute for Cancer we offer the most advanced diagnostic testing available including fiberoptic photos, CT and PET scans, as well as MRIs. Together, you and your care team will decide which treatment best fits your needs. For these types of cancers, treatment options include radiation, chemotherapy and surgery. Renown Institute for Cancer | 775-982-4000 At the Renown Health Institute for Cancer, our experienced team provides the support and care to maintain the highest quality of life and then achieve the best possible outcome, all in one location that’s close to home. Our dedicated team, clinical expertise and advanced treatment options allow us to tailor care to each patient. Learn about: Our Team Cancers We Treat Screening and Prevention Treatment Options Find a Cancer Doctor
Read More About Head, Neck and Oral Cancers: How You Can Spot and Treat Them