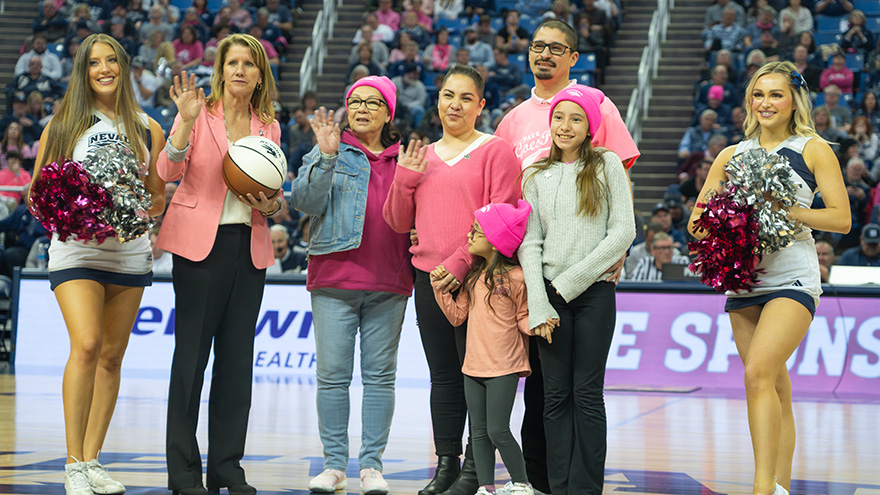Buscar
-
A Therapist's Tips to Prevent and Manage Osteoporosis
Want to know more about osteoporosis and osteopenia? We'll dive into these conditions and give you some handy tips on preventing future problems and taking care of your bones. What is Osteopenia? Osteopenia (low bone density) is the initial stage of bone mineral density loss, which can eventually progress to osteoporosis if steps are not taken to prevent it. What is Osteoporosis? Osteoporosis is a condition that weakens our bones. While it literally means “porous bone," it doesn’t mean that our bones are doomed to succumb to the changes that can happen to us silently over time. Our bones are living tissues that are constantly breaking down and remodeling themselves. Osteoporosis and osteopenia are typically diagnosed by testing bone mineral density using scans that your primary care provider can easily order. This is important testing because it dictates your risk of breaking a bone in common areas like your hip, wrist or spine. It also helps set the stage for talking with your healthcare team to develop a treatment plan. Most people will reach their peak bone mass in their mid to late twenties. There are several factors that increase our risk of osteoporosis or osteopenia as we age, such as menopause, genetics and other lifestyle factors. However, there are several things you can do to mitigate this breakdown and assist your body in the constant remodeling it does to our bones. 3 Controllable Factors to Build Strong Bones 1. Talk to your primary care provider They can go over a plan and prescribe things such as vitamin D, calcium and medications that can help if you are at risk or have osteoporosis or osteopenia. 2. Maintain a healthy diet Talk to a dietician if you need further help as they can be an invaluable resource to develop a plan. Eat foods rich in calcium, vitamin D and vitamin C. These assist with the rebuilding of bone. Examples include but aren’t limited to leafy greens, legumes, salmon and healthy dairy products. Don’t smoke — it directly correlates with a decrease in bone mass. Smokers also take longer to heal from a fracture. Limit alcohol to two to three beverages per week. Alcohol interferes with the production of vitamins needed to absorb calcium and the hormones that help protect bones. 3. Exercise Talk to your primary care provider to get a referral to physical therapy if you need help with exercise. Our bones adapt to the stresses we put them through. Therefore, exercise should be tailored to putting the right stress on our bones. There is good quality research that most exercise is safe when dealing with less bone mineral density. The exercises should be progressively challenging and increase the load for resistance and weight training at least two to three days a week. Examples include squats, step-ups, chest presses and rows. Exercises higher in velocity will lead to more power and bone adaptation. Examples include quicker push-ups, marching and quicker walks. Exercises that are weight-bearing will lead bones to adapt to the stress placed on them. Movements such as mini stomps, step-ups, jumping, jogging and so forth may be used depending on how your body tolerates these things to really stimulate bone adaptation. There are aspects of aging and bone health we can’t control, but we can take steps to minimize the chances of bone loss and osteoporosis. Talk to your healthcare team to determine your risk and don’t forget to show your bones a little TLC – you’re going to need them.
Read More About A Therapist's Tips to Prevent and Manage Osteoporosis
-
What You Need To Know About Cold Water Drowning
Northern Nevada's stunning lakes, including Lake Tahoe, with its average summer water temperature of 50 degrees, present a potential risk of hypothermia. Unlike mild 50-degree air, water at the same temperature poses severe, life-threatening risks, including rapid-onset hypothermia and drowning. Awareness of the symptoms and taking proper precautions are crucial to prevent cold-water drowning. The 4 Phases of Cold-Water Drowning 1. Cold Shock Response: This response affects breathing and happens within the first minute. An automatic gasp reflex occurs in response to rapid skin cooling. If the head goes below water, water may be breathed into the lungs, resulting in drowning. A life jacket will help keep your head above water during this critical phase. Additionally, hyperventilation, like the gasp reflex, is a response to the cold and will subside. Panic will make this worse, so the key is to control breathing. 2. Cold Incapacitation: This response occurs within the first five to 15 minutes in cold water. In order to preserve core heat, vasoconstriction takes place decreasing blood flow to the extremities to protect the vital organs. The result is a loss of movement to hands, feet, arms and legs. Unless a life jacket is being worn, the ability to stay afloat is next to impossible. 3. Hypothermia: Important to note, it can take 30 minutes or more for most adults to become hypothermic. So there’s time to take action and survive. Keeping panic at bay is critical, as you have more survival time than you think. Symptoms include: Shivering Slow and shallow breathing Confusion Drowsiness or exhaustion Slurred speech Loss of coordination Weak pulse 4. Circum-rescue Collapse: This experience can happen just before rescue and is not well understood. Symptoms range anywhere from fainting to death. Some experts believe an abrupt drop in blood pressure may cause this final stage of cold water drowning, post-rescue. Additional Safety Tips and Helpful Resources Always wear a personal flotation device as well as a wetsuit or drysuit. Your personal flotation device is the most important piece of water safety gear. Try not to panic as the first phases will subside. Controlled breathing is to staying calm. Research suggests the body can withstand the cold longer than we think. The Heat Escape Lessening Posture (HELP) is a position which helps conserve energy if you’re wearing a personal flotation device. By hugging your knees to your chest, this posture helps maintain body heat for some time.
Read More About What You Need To Know About Cold Water Drowning
-
What is Dry Drowning?
Whether you're a parent, grandparent, caregiver, or sibling, it's vital to recognize that drowning is the second leading cause of death among children," states Dr. Leland Sullivan, of Northern Nevada Emergency Physicians. "While we diligently work to protect children from water-related accidents, there's a lesser-known threat that often goes unnoticed—dry drowning, also known as delayed drowning. Surprisingly, many people remain unaware of its existence and potential dangers. Dry drowning defined Dry drowning is a side-effect of a near-drowning experience and includes spasms of the vocal cords and larynx — known as a laryngospasm. This occurs when the body attempts to shut down the passage of any liquid into the lungs. Unfortunately, it can also shut down the passage of air into the lungs and force fluid into the stomach and lungs. Often the condition is not discovered until it's too late — severe cases can cause death within one to 24 hours after a water incident occurs. Who is susceptible? Novice or first-time swimmers are at increased risk, as are children with asthma and known breathing issues. In addition, children who have had pneumonia or experienced acute respiratory distress syndrome are also at greater risk. To reduce these factors, caregivers should be exceptionally watchful of inexperienced swimmers. According to Dr. Sullivan, children under the age of 5 are most susceptible to drowning and often drown in residential swimming pools. Infants less than 1-year-old most often drown in bathtubs. What are the signs of a dry drowning episode? If your child has a near-drowning incident, a few moments of coughing until they calm down is normal. However, you should know the more severe signs and symptoms to watch for during the 24 hours following the incident, including: Persistent coughing Difficulty breathing and/or shortness of breath Chest pains Extreme fatigue and/or lethargy Change in typical behavior Face becomes pale What is the treatment and prognosis for dry drowning? Dr. Sullivan recommends that all victims of near-drowning incidents seek medical attention, even if they have no symptoms. If caught early, dry drowning can be treated. If you think your child is experiencing a dry drowning episode, go to the nearest emergency room as quickly as possible — do not attempt treatment at home. Healthcare professionals will work to supply oxygen to your child's lungs to restore and regulate breathing.
-
When Care Can’t Wait: True Stories of Renown ER
Renown Health is home to three 24/7 Emergency Rooms (ERs) providing comprehensive emergency and trauma care, access to specialists and inpatient services backed by the area's most extensive health system. In 2023, Renown Health cared for 132,340 patients across three ER locations. Renown is also home to the region’s only level II trauma centers for both adult and pediatric patients. We spoke to three patients who sought immediate medical attention for various ailments and conditions to learn more about their emergency care experience and why they chose Renown ERs. Kamrin’s Story: From Worrisome to Critical In the spring of 2021, Danielle and her 13-year-old son Kamrin visited his primary care doctor for unexplained vomiting and were promptly referred to Renown Children's ER via ambulance for further evaluation and seen by board-certified emergency physician, Dr. Lisa Nelson. What initially began as an unassuming doctor's visit quickly turned into something much more severe after several tests confirmed a devastating abdominal tumor and a stage-four cancer diagnosis, unbeknownst to the family. Kamrin was immediately admitted to the Pediatric Intensive Care Unit (PICU) and referred to a Pediatric Oncologist at Renown Children’s Hospital to begin his plan of care with expert pediatric hematology and oncology specialists. Regarding the board-certified physician, who delivered the results to the family, Danielle said, “She was so calming to us, even as the diagnosis haunted us. She led us by guiding our family through the unknowns. She felt like a family member to us in that moment, letting all the unknowns be well known.” “The love, empathy, support and guidance these employees gave us carried us. The care team quickly and easily became a source of relief, knowing we were their priority and in the best hands. We are forever grateful for the team at Renown Children's Hospital and Renown Children’s ER; they truly saved our son's life and continue to be our guiding light whenever it's needed in our son’s health journey,” Danielle said. Today, Kamrin is in remission and navigating the aftereffects of chemotherapy, including an immune system deficiency. However, his family chooses to navigate each day by embracing the positive side of things, such as the life-saving impact of his treatment. Did you know? Renown Children's Pediatric Hematology and Oncology is located within Renown Regional Medical Center and offers expert pediatric specialists dedicated to providing comprehensive treatment for pediatric hematology and oncology, including chemotherapy, radiation therapy and infusion services. Taylor’s Story: From Crisis to Recovery Promptly after cosmetic surgery performed by a medical professional not associated with Renown, Taylor Salas (Chacon) began to lose consciousness and notice her post-surgery drainage systems, also known as Jackson-Pratt drains, fill with blood. She was transported to Renown Regional ER via ambulance and immediately seen by ER staff and board-certified emergency physician Thea Berning, MD, for medical assessment. Taylor drifted in and out of consciousness as the ER team began blood transfusions and a CT scan to determine her plan of care. Dr. Berning began facilitating communication with a community plastic surgeon with privileges at Renown Health and emergency surgery was performed to stop Taylor’s internal bleeding. Taylor was placed on a ventilator due to respiratory distress and trauma from the event, then transferred to Renown’s Intensive Care Unit (ICU) to continue her care. Thankfully, Taylor listened to her gut when something didn’t feel right after her surgery and sought immediate medical attention. The ER team's quick response, communication and collaboration with a plastic surgeon saved Taylor from severe internal bleeding. “I was informed every step of the way about what was happening and why. I felt comfort in this,” she said. Did you know? Because of Renown Regional Medical Center’s Level II Trauma Center distinction, you have immediate access to an extensive list of specialists and physicians trained in a wide array of specialties, in the event of a traumatic injury or accident. This is one of the many benefits of Renown Regional’s Level II Trauma status. Ted’s Story: The Unsuspected Threat Bothered by symptoms of heartburn, fatigue, neck pressure and arm discomfort, Ted was in the middle of a busy workweek in June 2023 when he began to suspect something was wrong. Knowing the importance of addressing early heart attack symptoms immediately, Ted and his wife headed to Renown Regional ER because of proximity and some familiarity with Renown’s leading cardiology care and technological expertise. After prompt assessment by the Renown ER team, including blood work, imaging tests and the administration of medication, Ted was admitted to the hospital to treat the blockage and narrowing of his coronary artery. On June 8, Ted was admitted for treatment, where he successfully underwent a single bypass surgery and recovered in the Cardiac Intensive Care Unit (CICU), before being discharged and following up with the Intensive Cardiac Rehab (ICR) program at Renown. The ICR program at Renown played a pivotal role in Ted's 55-pound weight loss and overall health improvement, empowering him to embrace a healthier lifestyle and find ways to use his newfound energy and strength today. “Overall, I believe I had the best care possible because of the collective group of people at Renown caring for this community, who we could see in the grocery store, at the ball game and in the shopping malls. This community feeling is something you might not get in a big city hospital,” Ted said. Did you know? Intensive Cardiac Rehab at Renown Health is a medically supervised program designed to improve cardiovascular health after a significant heart condition or procedure. Since its inception in 2016, this program has been a pioneer in the region for cardiac rehabilitation focusing on three key pillars including exercise, nutrition and stress management.
Read More About When Care Can’t Wait: True Stories of Renown ER
-
Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
Raquel was 33 when she was diagnosed with breast cancer. It was April 2023, when she found a lump in her breast and was referred to the William N. Pennington Cancer Institute. After comprehensive imaging, she was diagnosed with invasive lobular carcinoma, which is a type of breast cancer that begins in the milk-producing glands of the breast. Between June 2023 and January 2024, she received a total mastectomy, chemotherapy and radiation at Renown Health. “Breast cancer is uncommon in women under 40, but any woman with a mass or lump in her breast should have an exam by a physician and imaging at any age,” said Dr. Lee Schwartzberg. In fact, according to the Centers for Disease Control and Prevention (CDC), only 9% of all new cases of breast cancer in the U.S. are found in women younger than 45. “It was a pretty scary diagnosis, but I’ve been led by great people through the process,” she said. “They were so helpful and there for me throughout the chemo and radiation.” Raquel's journey through breast cancer treatment at the William N. Pennington Cancer Institute was marked by the exceptional care provided by the Renown Health team, including nurses, nurse navigators, therapists, support teams and providers. Among the dedicated professionals, Dr. Michelle Chu and Dr. Lee Schwartzberg played pivotal roles in Raquel's diagnosis and subsequent treatment plan. Their expertise, compassion and commitment to patient care left an indelible impact on Raquel's experience. Their thorough examination and comprehensive approach ensured that Racquel received the best possible care for her invasive lobular carcinoma. In addition to the care provided at Renown, Raquel greatly benefitted from being connected with a mentor by Dr. Chu. This mentor, Kayla, had undergone a similar diagnosis and treatment plan, and at the same age Raquel. They texted and called each other throughout Raquel’s treatment, providing additional support through a challenging time. As of January 2024, Raquel is done with her treatment and continues to see her care team for follow-up appointments. “I’m through the worst and ready to rebuild my life,” Raquel said. To help celebrate this milestone, Nevada Athletics invited Raquel to receive the game ball at a Nevada Men’s Basketball game. She was joined on the basketball court for this special recognition by her husband, Raul; mother, Arlene; and two daughters, Ryleigh and Rhiannon. Racquel's journey is not only a testament to her resilience but also a tribute to the invaluable contributions of Dr. Chu and Dr. Schwartzberg in guiding her towards triumph over breast cancer.
Read More About Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
-
Departamento destacado: Patología
Celebrate Leap Day by leaping into the world of Pathology at Renown Health! Think of discovering a diagnosis like solving a mystery: the condition is the suspect, the nurses are the frontline police force and the doctors are the lieutenants or captains finalizing the results of the case. You may notice that one crucial role is missing on this list – the detectives. In the diverse network of healthcare, the detectives are a significant part of each patient’s mystery-solving care team and represent many roles across our health system. When it comes to figuring out the elaborate details of a growth, disease, organ abnormality or cause of death, one team of detectives, quite literally, goes as deep as possible. Those detectives are the team members within Renown Pathology. For each specialized field within medicine or surgery, the Pathology department is here to play a crucial role in accurate diagnoses. With each slide examined and each test meticulously conducted in their bright laboratories, these dedicated professionals shape a path towards wellness and recovery. Meet Your Anatomy Experts Whether you have a chronic disease that needs consistent testing, a high-risk birth that requires placenta testing, a suspected cancerous tumor that needs a biopsy or a gall stone that must be removed (or anything in between), Renown’s Pathology team steps in to provide biological answers to your body’s questions. This department offers the most comprehensive in-house diagnostic testing in the region, from routine histology to full pathology. As the busiest pathology department in northern Nevada, this team boasts the fastest turnaround times from respected experts, including: Pathologists Pathology Assistants Histotechnicians Histotechnologists Clinical Lab Assistants Let’s break down the complex nature of these team members' jobs by walking through their everyday responsibilities at work! Pathologists Pathologists are medical doctors who specialize in the study and diagnosis of disease. With every slide they scrutinize and every sample they analyze, pathologists unravel the mysteries of disease with precision and compassion. Their responsibilities include interpreting laboratory tests, analyzing tissue and fluid samples (obtained from a variety of different sources, including biopsies and surgeries), staging cancer diagnoses and providing diagnostic insights that guide treatment decisions. “Our job is to help the patients and their doctors figure out what’s wrong,” said Dr. Christie Elliott, Pathologist and Medical Director of the Clinical Laboratory at Renown Regional Medical Center. “As the bulk of our cases deal with cancer, almost every day we start with a tumor board alongside fellow surgeons, oncologists, radiologists and geneticists. From there, we order extra studies, run through our cases to make diagnoses, review slides and ensure all information goes into the charts, which is especially important as 70% of data in medical charts is from the lab. A patient’s history is everything.” Pathology Assistants With the steadiest of hands, pathology assistants, also known as PAs (not to be confused with physician assistants), guide the diagnostic journey from patient specimen to diagnosis. They can typically be found processing surgical and biopsy specimens (includes accessioning, gross examination, description, and sampling for microscopic analysis), preparing tissue samples for microscopic evaluation, helping the pathologist determine a cause of death for autopsies by conducting organ dissections and maintaining detailed records of all diagnostic findings. “As a PA, I still impact patient care without being directly patient-facing,” said Andrew Whitner, Pathology Assistant. “I handle 300-350 small tissue blocks a day. During dissections, I identify landmarks, document what I see and turn those landmarks into slides, looking for things that don’t look normal.” “Our job is 90% all about gross specimens, and we also do eviscerations for autopsies,” added Leslieann Haffner, Pathology Assistant. “We are trained on what normal looks like; our goal is to find the abnormal.” Histotechnicians Histotechnicians work behind the scenes to help transform ordinary tissue into extraordinary windows of insight, revealing the inner workings of the human body. As vital members of the Pathology team, histotechnicians embed tissue specimens in paraffin wax blocks (a process that preserves the tissue's structure for examination), cut thin sections of tissue from the paraffin blocks using a microtome, mount tissue onto glass slides and stain the tissue slides using histological stains to highlight structures or cells. “With all the patient specimens we work with, we get to see a lot of organs and learn what is causing the abnormalities,” said Reiny Hitchcock, Histotechnician. “I enjoy the opportunities to expand my knowledge, especially while working alongside the doctors.” “Our job can change by the week,” added Jessica Fahrion, Histotechnician. “One week I’ll be in the grossing room, and the next week I might be training in cytology." Histotechnologists In a world where every slide holds the key to a patient's future, histotechnologists are the champions of progress. One career ladder step above histotechnicians, these team members often have a broader scope of responsibilities, including more complex laboratory procedures, developing and validating new techniques, managing laboratory operations, interpreting results and troubleshooting technical issues. You can count on histotechnologists for validating antibodies and handling orders from pathologists, oncologists, emergency physicians and more. “My day always involves looking into cases, reading reports, getting orders together and working with pathologists to help them with their diagnoses; I also work a lot with immunohistochemistry, helping out with routine slides,” said Charles Koeritz, Histotechnologist. “I especially enjoy doing validations, which help maintain the integrity of lab testing and our diagnostic processes.” Clinical Lab Assistants Our pathology clinical lab assistants are the masters at “filling in the blanks,” assisting in whatever area needs it most, especially in cytology and the grossing room. They are essential aspects of the Pathology team, collecting and storing specimens for further testing, assisting in managing test results, gathering data, managing supply inventory and more. “As a Clinical Lab Assistant, I can be scheduled anywhere, from tissue cassetting to grossing,” said Ellie Somers, Clinical Lab Assistant. “Working in cytology is one of my favorite parts of my job. It’s very rewarding to work with the doctors to uncover what treatments will help each patient. We do cytology very well here.” The Bottom Line Even though the Pathology department doesn’t always experience a lot of patient face-to-face time, they interact with patients in a different way – by uncovering the story that is the inner workings of the human body, one slide and one sample at a time. “It’s important to remember that the slide IS a patient,” said Dr. Elliott. “We are constantly learning from every case so we can continue to provide the best patient care possible.” Take a Photo Tour of the Pathology Lab!
-
A Transformative Journey: Mary's Bariatric Surgery Story at Renown Health
Embarking on the path to bariatric surgery is a unique and deeply personal journey. Individuals like Mary Escobar choose this life-changing route for reasons ranging from improved cardiovascular health to managing diabetes or finding relief from various health complications. In Mary's case, her two-decade-long healthcare journey not only underscores the challenges she faced but also highlights the support and expertise that ultimately led to her successful transformation through bariatric surgery. Mary's Resilience: December 2002 through February 2003 More than two decades ago, Mary experienced unforeseen health complications just days after giving birth via c-section. Septic shock, hemolytic uremic syndrome, thrombocytopenia, renal failure and a blood clot in her lung plunged her into a critical state. Intensive care, plasma exchange and a long recovery followed. After being discharged with compromised kidney function, Mary faced complete renal failure two years later, leading to dialysis and a spot on the donor list. Mary's brother, a perfect match, selflessly donated his kidney on Dec. 14, 2007, marking a turning point in Mary's health. However, the post-transplant period brought new challenges, including diabetes, high blood pressure and a significant weight gain, reaching 230 pounds. Determined to regain control, Mary explored various diets without success until she consulted with a bariatric doctor. Journey to Bariatric Surgery: November 2009 - April 2021 In November 2009, Mary opted for a gastric band, shedding 40 pounds within a year. Despite initial success, issues with the gastric band arose, prompting a consultation with Dr. John Ganser at Renown Health in April 2021. Together, they decided to transition to a gastric sleeve, with comprehensive education provided to ensure long-term success.
Read More About A Transformative Journey: Mary's Bariatric Surgery Story at Renown Health
-
Living with COPD? How to Maximize Your Summer Experience
June offers an official welcome to summer and the height of outdoor activities in northern Nevada such as hiking, camping, days spent at the lake and embracing long days and warm evenings with friends and family. Enjoying all that the summer season has to offer may not be as easy for those living with chronic obstructive pulmonary disease, or COPD, which effects more than 15 million Americans. What is COPD? COPD is a group of lung diseases including emphysema and chronic bronchitis that result in airflow blockages from the lungs. People may experience frequent coughing and shortness of breath among other symptoms. COPD typically impacts adults ages 65 and older and is becoming increasingly more common among women. Although smoking plays a key role in the development of COPD, air pollution and indoor air quality, and respiratory infection also contribute to disease development. While there is no cure for COPD, limiting progression of disease and managing symptoms can be achieved through lifestyle changes, therapy, and medications. Tips for Living with COPD This Summer, and Always Stay Hydrated: Staying hydrated is extremely important for people with COPD, especially during the summer. Not drinking enough water can make breathing more difficult because it increases respiratory symptoms. Make sure to always keep a water bottle with you and aim to drink 8-10 glasses of water daily. Be Mindful of Temperature: COPD symptoms can be exacerbated by hot weather. It is best to participate in outdoor activities during the cooler times of day, like the morning or evening. Check Air Quality Before You Go: Before engaging in outdoor activities, be sure to check the air quality index and plan your activities accordingly. Pace Yourself: Exercising can be difficult for people who have COPD. To make the most of your summer, try not to push yourself too hard and take breaks when you need them. If you start to feel out of breath or tired, take a break in a cool, shaded area until you feel better. Take Matters Into Your Own Hands To address the needs of community members living with COPD, the Renown Health Research Office has teamed up with Pulmonary Medicine to provide patients who are former or current smokers and have a history of frequent exacerbations with an option to participate in the ARNASA study. "COPD exacerbations have a huge negative impact on patient’s lung function” states Dr. Farah Madhani-Lovely, Chief of Pulmonary Medicine at Renown Health and Assistant Dean of Clinical Research at the University of Nevada, Reno School of Medicine. “We have had inhalers and prednisone for decades but patients are still having exacerbations. Now we have a new pathway we think will prevent exacerbations which is what this clinical trial is designed to prove.” This study will evaluate the efficacy and safety of astegolimab compared with placebo in participants 40-80 years of age with COPD. “This study in particular is so exciting because of the enthusiasm from the sponsor’s end” says Katie Buckley, Lead Clinical Research Coordinator working on pulmonology studies at Renown’s Clinical Research Office. “Often times sites aren’t assigned particularly passionate or engaged personnel who aid in carrying out these studies, but you can tell Roche Genentech’s team truly cares about the success of the study, the safety of their participants, and proving the efficacy of the investigational agent. Working on a study like this takes a village, and when the individuals on all ends share similar mindsets and work towards success as a collective unit instead of as individual moving parts, it’s amazing to see everything we’re able to accomplish.” Renown’s team of expert pulmonologists and researchers are available to join patients with COPD in support of their healthcare journey. If you are interested in learning more about this clinical trial option at Renown Health, talk to your pulmonologist at your next appointment or contact us at 775-982-3646. At Renown Health, our goal is to make it easy for patients to access clinical research as a care opportunity where patients can access a variety of standard care treatment options for their health condition or choose to participate in a clinical trial. For more information about clinical trial opportunities available to you or to ask any questions, contact the Renown Research Office at Renown-CRD@renown.org or 775-982-3646.
Read More About Living with COPD? How to Maximize Your Summer Experience
-
Why I Give: The Meinzer Family’s Story
Losing a loved one is a devastating experience that can leave a permanent mark on one's heart. It is a journey that's difficult to navigate, but with the help of family and friends the process can be eased. For the Meinzer family, the healing process was made a little easier because of the exceptional care their loved one, Susie, received at Renown. In the fall of 2022, Susie Meinzer, a breast cancer survivor, suffered a fatal stroke. The care provided by Renown’s team was a reminder of the important role healthcare workers play in the lives of their patients and families. “We just knew, the doctors, the nurses, everyone… we knew that we didn’t have much time left with Susie,” said Ken Meinzer, Susie’s widower. Humanizing Healthcare The compassion provided by the care team at Renown made a significant impact on the Meinzer family. They ensured that Susie's last moments were as comfortable as possible, and their kindness and empathy have stuck with the family since. Dr. William Graham, pulmonologist with Renown Health, was among the many healthcare workers who provided care to Susie. "It was hard enough to lose her, and we ask ourselves, ‘Why?’ a lot, but the compassion we received from Dr. Graham made it a little bit easier,” said Ken. “One night he sat with us for over an hour, just grieving with us." This act of kindness made a profound impact on the family. “As an ICU doctor, I try not only to care for my patients, but also for their families,” said Dr. Graham. “Ken and his family displayed such sincerity, compassion and love for Susie and one another. They are just wonderful people; the kind of people that inspire me to be the best doctor possible.” A Family Legacy In gratitude for the exceptional care Susie received, the Meinzer family, including Ken and his three daughters, Melissa, Nicole and Kyra, decided to donate to Renown Health Foundation. Their gift is a beautiful reflection of their love and devotion to Susie. “The donation was a way to say thank you, and a way to support the healthcare workers who continue to make a difference in the lives of patients and families every day,” said Ken. "The nurses in Renown’s ICU went above and beyond. They were a constant source of comfort and support for our entire family," said Melissa Meinzer-Benson, Ken and Susie’s eldest daughter. This was not the first time the family had experienced exceptional care at Renown. Ken and Susie had both undergone cancer treatment the previous year. Susie was diagnosed with breast cancer and had recently completed her treatment before her stroke, while Ken was treated for neck cancer. Dr. Abhinand Peddada, oncologist with Renown Health, led both their care teams, demonstrating a deep dedication to their well-being throughout their treatments. “I am grateful and humbled by the trust that Mr. and Mrs. Meinzer placed in Renown and me for their care in difficult times,” said Dr. Peddada.” Both Ken and Susie deeply appreciated Dr. Peddada’s care for them throughout their respective battles with cancer. The Meinzer family, who own Pinnacle Heating and Air Conditioning in Reno, are known for their commitment to giving back to the community. Melissa is a Veteran and has spoken about the importance of supporting others in any way possible. Susie instilled in Melissa and her sisters a spirit of compassion from an early age, and they have continued to donate to charitable causes throughout their lives. “She was such a force of inspiration, compassion and love. She was aways caring for others,” said Kyra, Ken and Susie’s youngest daughter. Susie was a beloved member of the Oak Community Church. It was there that she spent many Thanksgivings alongside her daughters, volunteering to serve meals to those in need. Charity work was a passion for Susie, and she always found ways to help those around her. She was a shining example of the importance of supporting your community and making a positive impact on the world.
-
A Fighting Chance at 24 Weeks Sloans Story
Most babies weigh just one pound and are roughly the size of an eggplant when they reach 24 weeks of development inside the womb. It is a crucial stage when internal organs begin functioning, and the babies' respiratory and central nervous systems are still developing. So, in November 2021 when Kallie Johnson experienced a premature rupture of amniotic fluid around this point in her pregnancy, her care team in Winnemucca decided to transport her via Care Flight to Renown Regional Medical Center. The team at Renown Children’s Hospital immediately began discussing the risks of delivering at 24 weeks with the Johnson family. Moving Forward with Hope Knowing the stakes, Kallie remembers never feeling rushed to decide about delivering her baby preterm. “I felt educated and supported by my care team at Renown throughout our entire stay, starting with the education they provided about what it meant to deliver my baby early,” Kallie said. “The team really helped me make the best decision for myself and my family.” Together, Renown employees and the Johnson family moved forward with a healthy set of nerves and a powerful feeling of hope. Weighing in at one pound 11 ounces, Sloan entered the world on Nov. 19, 2021, via emergency Cesarean section. Her birth was classified as a micro preemie because she was born before week 26 of pregnancy and so small that she fit inside the palm of her father Sterling’s hand. A full-term pregnancy is classified as reaching 39 weeks. A Fighting Chance Called a fighter by many Renown Children’s Hospital care team members, Sloan spent over five months in the neonatal intensive care unit (NICU). She was placed on a ventilator, fed through a feeding tube and monitored 24/7, overcoming daily challenges with the Renown team and her family. As a result of being born prematurely, Sloan developed a grade one brain bleed and a congenital heart defect called patent ductus arteriosus, a persistent opening between two major blood vessels, causing too much blood to flow to the lungs and heart. To meet the oxygen needs of her tiny lungs, Sloan was intubated and developed a severe oral aversion and high-arched palate as a result. The effects would lead to difficult developmental and physical challenges that she still conquers today. Yet, with the help of her care team – including physical, occupational and speech therapists, dieticians and doctors – Sloan continues to make progress every day.
-
What Is an Echo-Tech?
When it comes to our heart, keeping this vital source of life in tip-top shape is of utmost importance. Echo technologists or echocardiographers, otherwise known as "echo-techs," are charged with that mission, providing critical information that leads to life-saving interventions to keep our hearts beating strong. Adrianne Little, echocardiographer at Renown Health, breaks down the echo-tech's role in the health system, the educational path it takes to get there and the unique perks that come with the profession. What does an echo tech do? “Echo techs play a key role in the diagnosis and treatment of patients,” said Adrianne. “We are members of the cardiovascular imaging team that perform ‘heart ultrasounds’ or echocardiograms. Although we are most commonly known as echo techs, our official title is either ‘cardiac sonographer’ or ‘echocardiographer.’” Echo techs use imaging technology and sophisticated ultrasound equipment to produce images of the heart. These images show how well the heart functions, as well as the valves, chambers and blood flow. Echocardiograms are used to diagnosis and treat a variety of heart conditions such as murmurs, arrhythmias and heart failure. At the end of the day, the main goal of echo techs is to help our cardiovascular team provide the quickest and most accurate diagnoses to help with patient management and help them receive the highest standard of care. “When it comes to looking at the heart, we are part of the front-line team," said Adrianne. “We provide real time critical information that leads to life saving interventions down the road.”
-
Jakob’s Journey at Renown Children’s Hospital
In August 2016, six-year-old Jakob was admitted to Renown Children's Hospital with what seemed like a common ear infection. Jakob's condition quickly progressed, and he started experiencing neurological symptoms such as difficulty speaking and a full-body shutdown. Doctors, neurologists and specialists from Renown worked with doctors from Stanford, where he was ultimately diagnosed with Bickerstaff brainstem encephalitis (BBE). BBE is a rare, autoimmune response that attacks the nerves in the body due to an acute illness such as a cold, flu or, in Jakob's case, an ear infection. Jakob could not breathe or eat and experienced paralysis on the side of his face, throat, stomach, bowels, lungs and legs. In addition, he started to rapidly lose weight as well as body function. Jakob lost half his body weight which resulted in the need for a Gastrostomy tube. This device is placed surgically and gives direct access to the stomach to give the child the nutrition needed. He also needed occupational therapy, and after three and a half months of ICU respiratory therapy, surgeries and treatments, he was released home to regain his strength. Forever Grateful Anica, Jakob's mom, said, "If it were not for the quick response and unconditional support and compassion from the team at Renown, Jakob would not be here today." Jakob's family is forever grateful to the staff, community and expertise at Renown for their unwavering commitment to their son and family during their most trying time in life. "When I met Jakob on the first day of his illness, so much was unknown. My team and I were worried, as his symptoms were very unusual. His rapid deterioration, after being a perfectly healthy child, was clearly terrifying for his parents. Handing over a child's care to a team of strangers is one of the scariest things that can happen to parents,” said Dr. Kris Deeter, Physician in Chief at Renown Children’s Hospital. “However, Anica and Jeremiah were also very clear that they did not want Jakob transferred somewhere else. So, we used all our resources to care for him, arrive at a diagnosis, and start aggressive therapies. They listened to every word we said, educated themselves, and became partners in Jakob's care. We all became part of Team Jakob, and soon, he proved to us just how strong he was." Today, Jakob is 13 years old and thriving in every aspect of his life. He is currently on the honor roll in school and finds joy in his newfound passion for the violin. He loves spending his free time learning about mixing music, making new friends and traveling to different parts of the country. This summer, he will travel to Europe to explore his passion for culture. The family says, "We owe it all to the family and staff at Renown."
Read More About Jakob’s Journey at Renown Children’s Hospital