Buscar
-
Optimizing Mammogram Screenings: A Genetic Approach to a Personalized Screening Schedule
© Arthon Meekodong via Canva.com Breast cancer screening has long been a cornerstone of women's healthcare. With 1 in 8 women diagnosed with breast cancer in their lifetime1, the United States Preventive Services Task Force (USPSTF) has developed screening recommendations to help detect early-stage cancer. Notably in 2023, the USPSTF revised the recommended age for biennial mammogram screenings for women with average risk to start at age 40 instead of 502, estimated to result in 19% more lives being saved3 by starting screening earlier. While initiating screening at an earlier age offers advantages to a wide demographic, concerns about the potential of over-screening prompted research into the feasibility of identifying women with lower breast cancer risk who could safely delay mammograms. While guidelines address high-risk individuals, a notable gap exists in providing recommendations tailored to those at lower risk. To gain insight into a patient's risk level, physicians are able to utilize genetic testing to understand an individual's genetic makeup, providing precise insights into their predisposition to various health conditions, including breast cancer. Armed with this genetic information, healthcare providers could craft tailored screening strategies that align with an individual’s specific risk profile. This genetic risk-based approach underscores the value of genetics in individualizing the onset of screening to help avoid over-screening and its associated costs. Surprisingly, genetic information is not currently being widely utilized to identify women at risk of breast cancer or other diseases in clinical practice, despite its potential to make a significant positive impact for patients. A recent retrospective analysis of 25,591 women from the Healthy Nevada Project4 sheds light on the potential benefits of this genetic risk-based approach. The study classified 2,338 (9.1%) of these women as having a low genetic risk for breast cancer. What's remarkable is that these women exhibited a significantly lower and later onset of breast cancer compared to their average or high-risk counterparts. This finding suggests that it might be safe for low-risk women to delay mammogram screening by 5 to 10 years without compromising their health.
-
11 Tips Caregivers Need to Know
Becoming a caregiver or playing a more active role in another’s healthcare is a big responsibility. At some point, almost all adults will support an aging parent or a loved one in need. Keeping track of their needs and wellbeing, while also prioritizing your own can become overwhelming. It’s important to know: you are not alone, and help is available. Read on for 11 tips to help you manage your time, your own wellbeing and your loved one’s care. Self-care comes first. When your main priority is the person in your life who needs care, it’s easy for your own needs to take the backseat. Give yourself time each day to focus on your personal wellbeing. It’s hard to give a loved one the care they need if your own needs are not met. Prioritize the Activities of Daily Living (ADL). Make a note of what ADLs your loved one can do alone, what they need help with and what activities require the most help. This will help you work through the day with them, as well as plan out how the day’s activities will go. Do a home safety audit. Do showers, bathtubs and steps have safety grab bars? Look around the house for additional tripping hazards, like rugs or electrical cords. If your loved one struggles with day-to-day navigation of the home, consider scheduling an occupational therapy appointment. This type of therapy helps a person develop or maintain the motions required to accomplish daily tasks. You might also qualify for a referral to in-home healthcare, such as Home Care. Have the hard conversation. The best time to discuss views about end of life care and to learn what choices are available is before a life-limiting illness or crisis occurs. With advance care planning, you can help reduce the doubt and anxiety related to decision making at the end of life. Completing an Advance Directive is a great tool to sort out all these decisions before they’re needed. Attend a free workshop to learn more and complete this important document. Identify when you need respite. Respite care involves receiving a short-term break from caregiving. Organizing in-home care for your loved one will allow you to step away and tend to your needs. By identifying what kind of respite care you are seeking, you can find the right person to provide you with that much-needed break. Don’t wait until you feel overwhelmed, plan ahead. Write down insurance contact information. Have a direct connection to the right insurance professional for support and advice. If your loved one is eligible Medicare, this is a good opportunity to review their current selections and if they would benefit from a Medicare Advantage Plan or Medicare Supplement Insurance. Seeking out expert advice or information on Medicare options is a great way to navigate this. Consider calling a broker, or attend a free educational seminar with Senior Care Plus. Gather legal and financial information. Make a list of all existing legal documents and financial accounts that your loved one has. These might include a will, advance directive, power of attorney, bank accounts or investment accounts. If you have questions about how to manage them, or need assistance in setting up additional framework, reach out to a lawyer, legal service, financial adviser or bank representative. Create an inventory of medical information. Identify where all of your loved one’s medical records are, as well as a list of providers or healthcare practices where they have received care. Consider if you should have your loved one give you Proxy Access in MyChart, which allows you to access all the features in MyChart on their behalf, including viewing upcoming appointments, viewing test results and emailing a doctor on their behalf. Make a list of what others can do. Think about all the little (and big) things that need to happen, and write down tasks that others could take care of you. When someone says “let me know what I can do” you’ll be ready with a pre-written list of items they may be able to assist with. Tasks could include tackling around-the-house repairs, scheduling lawn work, helping to walk the dog, taking a car for an oil change and cleaning. Find programs and events for social enjoyment. If and when possible, seek an activity outside of the home. Look for community centers that have programs for seniors, recreational activities or meals that you can patriciate in together. If leaving the home is not an option, arrange for visits or in-home activities, such as movie nights, card games or time to visit with family. Research long-term options. If you will be considering a nursing home or assisted living, make a list of amenities that you and the person you are caring for would like. Take this list with you when visiting potential locations to make sure you don’t forget to ask about each item.
-
Plan Early: Completing Your Advance Directive
We plan for the birth of a child, weddings and retirement, but rarely do we discuss how we want to be cared for at the end of our lives. Getting through this challenging conversation and completing an Advance Directive can give you peace of mind that your loved ones will not have to make difficult choices on your behalf. The best time to complete an Advance Directive is now – don’t wait until a life-limiting illness or crisis occurs to discuss your views about end-of-life care and to learn what choices are available. By preparing in advance, you can help reduce the doubt and anxiety related to decision-making for your family if you cannot speak for yourself. What are Advance Directives? An Advance Directive is a document that states your choices about medical treatment and names another person to make medical decisions on your behalf if you are unable to. This document allows you to make legally valid decisions about future medical care. “Completing your Advance Directive is a gift you give your family,” says Director of Palliative Care, Mary-Ann Brown RN, MSN. “The stress associated with these difficult decisions is decreased if everyone knows what is important to you and what you want at the end of life.”
Read More About Plan Early: Completing Your Advance Directive
-
Sobreviviente del cáncer de ovario cuenta cómo decidió probar con ensayos clínicos
While there used to be three basic treatment options for cancer -- surgery, radiation and chemotherapy, or a combination of the three -- there's a fourth option: clinical trials. Here, a Renown patient shares her successful battle with ovarian cancer, aided by a clinical trial. Shari Flamm's battle with ovarian cancer began in 2011. She was experiencing prolonged bleeding, irregular thyroid levels and anemia and was scheduled to undergo a hysterectomy. Before the surgery, her gynecologist ran routine tests to check for cancer as a precautionary measure. All tests were negative for cancer, expect her CA 125 test. A CA 125 test measures the amount of the protein CA 125 (cancer antigen 125) in the blood. In some cases, a CA 125 test may be used to look for early signs of ovarian cancer in women with a very high risk of the disease. In most laboratories, the normal level is 0 to 35 units/ml. Flamm's CA 125 level was 121. As Flamm can attest, early diagnosis played a key role in her battle with ovarian cancer. September is Gynecologic Cancer and Ovarian Cancer Awareness Month – an important time to learn the signs, symptoms and risk factors of this type of cancer so your doctor can diagnosis the disease as early as possible. Ovarian Cancer: Round One Despite the elevated CA 125 results, her doctor recommended they move forward with the hysterectomy. But when surgery began, doctors discovered a mass. She had stage 4 cancer. The procedure was halted, the mass was biopsied and she was immediately seen by Dr. Peter Lim of the The Center of Hope. Following diagnosis, Flamm underwent surgery with Dr. Lim to remove the cancer, which had spread to part of diaphragm, spleen, colon and other organs. Three months after surgery, Flamm had recovered enough to start six rounds of chemotherapy in her hometown of Carson City. She continued working at a doctor's office during her treatment, and was grateful for Dr. Lim’s ability to co-manage her care so she could stay close to work and family. “To me, chemo was the scariest part because I didn’t like feeling sick,” Flamm says. Thankfully, her body responded well to the treatments and she was back to the things she loved. “I stated working out at the gym, even if it was only for 10 minutes,” she says. She also stayed positive by spending time with her grandchildren, attending a San Jose Sharks hockey game, going for walks and enjoying concerts. Ovarian Cancer: Round Two In November 2014, Flamm had a cancer check-up. That’s when doctors discovered three cancerous tumors. For this round, Flamm choose another treatment option -- clinical trials at Renown Institute for Cancer. Clinical trials are the studies that test whether drugs work, and inform doctors' decisions about how to treat their patients. Flamm participated in a clinical trial that featured oral-targeted therapy stronger than IV chemotherapy. The hope was for the drug to shrink her tumors, however the result was stabilization -- meaning the lumps weren’t growing or spreading. The best part of the clinical trial, Flamm says, was the constant monitoring. Between the CT scans every six weeks, a heart scan every three months and monthly doctor visits, she was confident that if the cancer started growing or spreading, her healthcare team would catch it right away. For Flamm, the benefits of the clinical trial included less hair loss, less fatigue and more time to focus on what’s important in her life -- her family. “I decided I wasn’t going to be that sick grandma on the couch with cancer,” Flamm says. After taking the oral medication for one year, Flamm developed a rash and discontinued treatment due to discomfort. Clinical Trials, Setbacks and Survival In June 2016, two of the three tumors began to grow and had to be surgically removed. Despite the setback, Flamm was determined to maintain a positive outlook. "You have to stay positive because cancer feeds off anger, depression and stress," Flamm says. Flamm was released to go home with clear margins, meaning the tumors were removed and are surrounded by a rim of normal tissue that does not have cancerous cells. Flamm says her outlook on life has changed drastically since her first cancer diagnosis. “Your whole mentality changes when cancer disturbs your life," Flann says. "The things that weren’t important, are now ever so important. I’m a lot calmer now,” Flamm says.
Read More About Ovarian Cancer Survivor Shares Decision to Try Clinical Trial
-
Here's How to Commemorate National Healthcare Decision Day
National Healthcare Decision Day is forthcoming. Here’s an easy and free way to commemorate the occasion: openly discussing how we want to be cared for at the end of our lives. Join Renown Health’s experts at a workshop about making decisions about an advance directive. Among the random national holidays, this one has significance: April 16 is National Healthcare Decision Day. And experts agree that the best time to discuss your views about end-of-life care and to learn what choices are available is before a life-limiting illness or crisis occurs. By preparing in advance, you can help reduce the doubt and anxiety related to decision making for your family if you cannot speak for yourself. “Completing your advance directive is a gift you give your family,” says Mary-Ann Brown, RN, MSN, director of Palliative Care. “The stress associated with these difficult decisions is decreased if everyone knows what is important to you and what you want the end of life.” What Are Advance Directives? An advance directive is a document that states your choices about medical treatment and names another person to make medical decisions on your behalf if you are unable to. This document allows you to make legally valid decisions about future medical care. Find more information about advance directives and the form online. The Conversation The first step in completing an Advance Directive is to think about what’s important to you and talk to your loved ones. The Conversation Project provides helpful tools to guide you and your family through this challenging topic. Getting this information together will help you fill out and complete your advance directives. Some things to consider and discuss with your family include: When you think about the last phase of your life, what’s most important to you? Who do you want involved in your care? Who should make decisions on your behalf if you’re not able to? Where do you want or not want to receive care? Are there specific treatments you would or would not want? Complete Your Advance Directive Planning In order to complete an advance directive, you will need either two witnesses or a notary to sign the form. Be sure to note restrictions on the witness process. When an advance directive is complete, you should keep the original. Copies should be given to your agent named in the form, your family, your doctor(s) and the location that you receive care. Renown Health offers four advance directive workshops every month to cover the details of filling out this document. A healthcare team is available to answer questions and work through the process with you. A notary is also present to finalize the process, which means you can complete your advanced directives during this workshop. Find the workshop by calling 775-982-RSVP for more information. Advance Care Planning Workshop April 17, 1-2:30 p.m. | Free Join Renown Health’s experts for a workshop about making decisions regarding end-of-life care. You will learn how to fill out an advance directive, receive one-on-one assistance and have your documents signed by a notary. Workshops are typically held several times each month. To RSVP, call 775-982-7787
Read More About Here's How to Commemorate National Healthcare Decision Day
-
What Is the Importance of Having an Institute for Cancer?
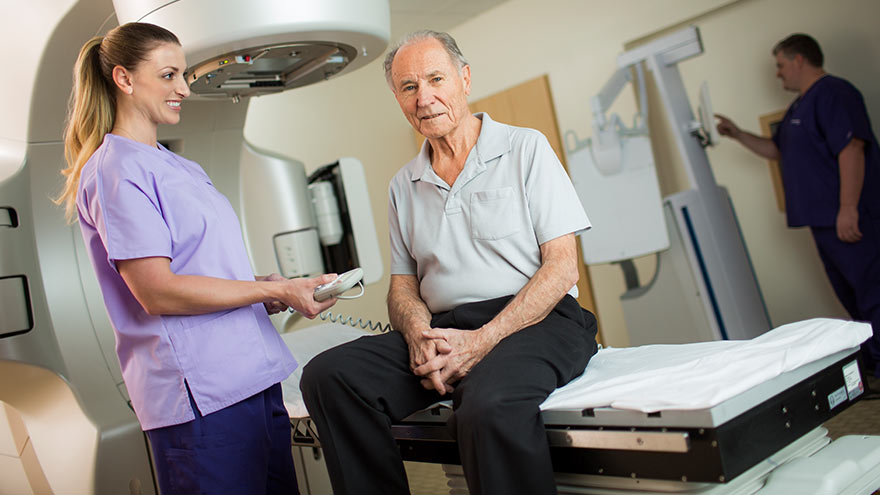
What is an institute for cancer — and why does it matter that we have one right here in Reno? Here, a radiation oncologist answers those questions and more. Sadly, our community health needs assessment shows cancer is the second leading cause of death in Washoe County. But many residents may not know there is an institute for cancer right here in Reno that can care for you or your loved one after diagnosis. Dr. Michael Hardacre, a radiation oncologist with Renown Institute for Cancer is here with more. What is an institute for cancer? The way I like to think of it: An Institute has healthcare providers highly trained in patient-centered care. For example, when you have cancer, many times you’ll see a lot of doctors. A program brings those doctors together — so you really have one team working together. An Institute takes that one step further. Say there are other needs beyond the doctor’s office such as nurse navigators, dietitians, physical therapists to help you get on track, etc. An Institute really proactively thinks of the need of the cancer patient. It then makes sure all those things are available to them throughout their treatment. The term “institute for cancer” identifies a cancer program that is comprehensive and multidisciplinary in nature. For Renown, that means that we have the specialists in medical oncology, surgical oncology and radiation oncology working together with other specialists to assure that a patient has coordinated care throughout the entire treatment course of cancer care. Together with cancer prevention and diagnostics, genetic assessment, supportive care, clinical trials, and cancer survivorship, the institute for cancer provides care for the community, families and patients along the entire spectrum of cancer care. What types of cancer do you treat? We’re fortunate to be able to provide cancer treatments for all types of cancers, and we’re one of the major referral centers for northern Nevada. Most commonly, just like much of the country, lung cancer, prostate cancer and breast cancer are the most frequent we see. Our care spans brain, to neck cancer and everything in between. As an accredited comprehensive community cancer program, Renown Health provides services for all cancer types. The highest volume cancers treated at Renown are breast, colorectal, lung, genitourinary, blood and gynecologic cancers. Most treatments can be done right here in Reno, but when there are specialty needs such as stem cell or bone marrow transplantation, we partner with quaternary centers, like Stanford, to assure a smooth transition of care both to and from the quaternary center. What kinds of care and treatments are offered? We offer a wide range of comprehensive care. We treat the cancer itself — surgical, radiation oncology, medical oncology in the form of chemotherapy or pills. Also addressed: dietary needs, physical therapy and navigation through this whole process. People may be surprised by the scope and scale of the Renown Institute for Cancer. For instance, our Radiation Center has the latest technologies to treat cancers. This includes the Linear Accelerators, which are machines with treatment planning software tools. In addition to the traditional external radiation treatments provided in most centers, Renown performs specialty treatments using High-Dose Brachytherapy, a treatment with an active radiation “source” and in Brain Stereotactic Radiosurgery, assuring that patients can stay right here in northern Nevada — close to home. What does that mean for the quality of care? I think it’s always great in any environment to have external people come into your program and not only share what’s happening nationally and what we could do better, but also to validate “are you doing things at the highest level you can?” That accreditation process is just one way to give us that seal of approval. We’re lucky enough this year to get the gold award by the American College of Surgeons — its highest honor. We were honored to receive it. Why is important that you’re an accredited institute? Accreditation assures our community that quality is a top priority for us. Each of the accrediting bodies has a set of standards that identify service and quality standards. Renown Institute for Cancer has the following accreditations: American College of Surgeons’ Commission on Cancer: Full Cancer Program accreditation, standards address issues from cancer prevention/diagnosis to treatment to survivorship and/or end-of-life. Renown received the Gold Level Accreditation in 2018, the highest level of accreditation possible; American College of Surgeons’ National Accreditation Program for Breast Centers: Full Breast Center/Program accreditation, standards address issues from breast cancer prevention/diagnosis to treatment to survivorship and/or end-of-life; American College of Radiology – Radiation Therapy: Full Radiation Oncology accreditation for radiation equipment, treatment planning, treatment and treatment follow-up; and American College of Radiology – Mammography Services.
Read More About What Is the Importance of Having an Institute for Cancer?