Buscar
-
Understanding and Managing Childhood Asthma
Dr. Shipra Singh, a Pediatric Pulmonologist, outlines the challenges of diagnosing asthma in children due to symptoms resembling other respiratory issues. It's particularly difficult to identify in infants and young children, who may not clearly exhibit breathing difficulties. Asthma, often confused with bronchitis, croup, or allergies, is a significant chronic illness causing school absenteeism, as per the CDC. Risk factors include prenatal smoking and family history of allergies or asthma. Infants and toddlers are more susceptible due to smaller airways and respiratory viruses, which can exacerbate conditions like colds and bronchitis. How can I tell if my child has asthma? Unfortunately small children are unable to describe their symptoms, making asthma difficult to diagnose. Your child may even be active, playing and smiling, although they are experiencing chest tightness or labored breathing. Observe your child and let the child’s doctor know if: Your child’s breathing behavior has changed (coughing, wheezing, rapid breathing) Your child’s breathing pattern changes (day vs. night, with rest or activity, inside vs. outside) You have a family history of asthma or allergies Your child’s breathing is triggered by any foods or allergies With your help, your child’s doctor can make the best diagnosis to determine if your child has asthma. A pediatric pulmonologist (lung specialist) or pediatric allergist may also have to be consulted for special testing. Tests may include lung function testing, allergy tests, blood tests and X-rays for an accurate diagnosis. What is the treatment for infants and toddlers? Young children can use many of the same medications as older children and adults, although the way they take them and the dosage will differ. A nebulizer (or breathing machine) creating a medicated mist for your child to breathe through a mask may be used. An inhaler with a small spacer tube connected to a mask is also common to help your child breath medication into their lungs. Either of these options are effective. Asthma in children is treated with both fast-acting and long-term medicines to open up airways quickly for easy breathing and also to lessen asthma symptoms over time. Communicate with your child’s medical providers to create a personalized asthma management plan for them. How can I manage my child’s asthma? Recognize your child’s breathing habits and be aware of worsening symptoms. Consult with your child’s doctor on a daily asthma action plan to recognize worsening symptoms and track medications. Here’s an example of an asthma action plan provided by the U.S. Department of Health and Human Services’ National Institutes of Health). Be consistent with the plan and talk to your doctor before changing it. Have an emergency plan in case of a serious asthma attack. Know where the closest ER is and know who can take care of your other children. Also know what the medical treatment coverage is under your insurance plan. Dr. Singh explains, "Discussing asthma with your child may be difficult. Some kids find the subject frightening or confusing. Others, especially the older kids, may resent the treatment and may not be interested in doing it. Talk to your doctor about advice to build an open and trusting relationship regarding your child's asthma care."
-
Suicide Risk How to Spot a Friend in Crisis
How can you tell if a friend is in trouble or struggling with suicidal thoughts? And how can you support them in finding help? Are you feeling virtually exhausted? Life is always challenging, but the mental fallout of a global pandemic is real. Contributing to the loneliness epidemic is the shifting American lifestyle. More Americans live alone (28%) now than ever before, and fewer have kids. First, let’s acknowledge this is a time of anxiety and worry for everyone. Economic uncertainty, job transitions, grief, and loneliness are a perfect storm for mental stress. Even before the COVID-19 (coronavirus) pandemic mental health was a concerning issue, now it is a relevant topic of crisis. Secondly, anyone can struggle with suicidal thoughts. Those suffering from drug addiction are especially vulnerable. In particular the U.S. is currently seeing a rise in drug overdoses by almost 18% due to the pandemic. Unfortunately, suicide is responsible for one U.S. death every 11 minutes, according to the Centers for Disease Control and Prevention. Not to mention the millions who think about it, make a plan or attempt it. It is important to remember that suicidal thoughts, plans or intent must be helped immediately. Understanding Suicide Risk To clarify, depression is not a choice. No one wishes for endless days of feeling down, sleepless nights, and feeling as if you are in a dark tunnel. Currently, one in five Americans will experience a mental illness this year. This means one of your friends is struggling, right now. Specifically, consider this: When your body feels pain it talks to your mind. When your mind is suffering who does it talk to? So, how can you tell if a friend is in trouble? According to the National Institute of Mental Health be on the lookout for some depression clues below. Signs and Symptoms of Depression Persistent sad, anxious, or “empty” mood Feelings of hopelessness, or pessimism Irritability Loss of interest or pleasure in hobbies and activities Decreased energy or fatigue Moving or talking more slowly Feeling restless or having trouble sitting still Difficulty concentrating, remembering, or making decisions Signs and Symptoms of Suicide Risk Expressing feelings of hopelessness or having no purpose Talking about feeling trapped or being in unbearable pain Talking about being a burden to others Increasing the use of alcohol or drugs Sleeping too little or too much Withdrawing or isolation Displaying extreme mood swings. Talking about wanting to die or to kill oneself (Reference: Suicide Awareness Voices of Education) How to Help a Suicidal Friend It can feel awkward to approach the subject of suicide with a friend, but take any of the above warning signs seriously. Other ways you can help are by: Encouraging self-care and making sure they take care of basic needs Listen to their worries without judgement Ask them what they need from you, then follow through with action Let them know they are not a burden Don’t minimize or invalidate their feelings Point them to helpful resources Be their advocate and get them help If someone you know is in a life-threatening crisis situation, call 911 immediately. Suicide Risk Resources: National Suicide Prevention 24/7 Lifeline: 1-800-273-8255 Ayuda En Español: (Spanish National Suicide Prevention Lifeline) 1-800-628-9454 Crisis Text Line: Text HOME (or CONNECT) to 741741 to chat with a crisis counselor 24/7 free of charge. The National Alliance on Mental Health: 1-800-950-6264 Substance Abuse and Mental Health Services Administration: (SAMHSA) 24/7 helpline 1-800-662-4357
-
4 fantásticos beneficios para la salud de estar libre de desorden
The Benefits of Being Clutter-Free Gives you a better sense of well-being. Did you know procrastination is linked to clutter? According to a recent study clutter problems led to less life satisfaction, especially among older adults. Helps you lose weight. Constantly being in cluttered room, office or car can be stressful. All the undone cleaning tasks in the back of your of mind cause stress, which is linked to obesity. Promotes mental health. Having clutter around can make you feel anxious or overwhelmed. This prevents you from truly relaxing or focusing. Saves you money. It’s not a secret that money worries cause stress. According to a Journal of Consumer Research study, you’re more likely to make a purchase when you’re sitting in a messy room compared to a tidy room. Clutter-Free Tips Start with a plan. Make a list of your clutter-improvement priorities and the tasks needed to accomplish each one. Focus on one section of your home per week, so you don’t get overwhelmed. In fact, organizational expert Peter Walsh suggests starting with the easiest room first to gain momentum. Conversely, "The Life-Changing Magic of Tidying Up" author Marie Kondo suggests organizing by category (for example clothing or books). Experiment with an organizing plan that appeals to you. There are also many helpful on-line calendars you can use as a starting point. Delegate when you can. Include your children and spouse into your plan. Is uncle Bob an electrician? Then get him to swap out your eyesore of a ceiling fan or update an old light fixture. Of course it’s ok to outsource the duties - such as window cleaning or painting - if your budget allows. Buy less. The less you purchase the less you need to store, clean, keep track of, organize or dust. Seems simple, right? Not for everyone. On average we are bombarded with over 4,000 marketing messages a day, not to mention FOMO (Fear Of Missing Out) when we see our friends posting about their newest toys on their social media feeds. Focus on quality over quantity. When in doubt, throw it out. Still on the fence about what to throw away? Use these declutter decision-making guide questions to help you. Organize Your Health Along with taking care of your surroundings, make a commitment to get up to date on your health checkup and screenings. Preventing an illness is a bargain compared to the cost of a chronic disease. It's also a good idea to go through all of your medications and check the expiration date. Remember to properly dispose of medications. DO NOT flush medications down the drain or toilet, unless the label indicates it is safe to do so.
Read More About 4 Fantastic Health Benefits of Being Clutter-Free
-
Conexiones sociales: por qué benefician su salud
Some days a chat with a friend is all you need to feel better. Why? Because humans are social beings. Although we have more technology than ever at our fingertips, sometimes we may still feel left out or disconnected. Dr. Buddy Coard, Ed.D., Psychologist at the Stacie Mathewson Behavioral Health Addiction Institute at Renown, discusses the importance of social connections and tips on how to keep connecting, warning signs of loneliness and how to feel less lonely. Why are Social Connections Important? Dr. Coard points to significant research on the topic of loneliness and social connections. He uses the findings below to detail how social connections affect our overall health. In a recent survey 40% of participants reported they sometimes or always feel that their relationships are not meaningful and that they feel isolated. Surprisingly, this survey suggests Generation Z (18-22 years old) is the loneliest generation. Another study associates loneliness as a risk factor for early death. It indicates lack of social connection heightens health risks as much as smoking 15 cigarettes a day, or having alcohol use disorder. In fact, loneliness and social isolation are twice as harmful to physical and mental health as obesity (Perspectives on Psychological Science, Vol. 10, No. 2, 2015). A 2018 study investigated several standard measures of social isolation, including marital status, frequency of religious service attendance, club meetings/group activities and number of close friends or relatives. The findings revealed race as a strong predictor of social isolation. In particular, black men and women were more likely to be lonely than were white men and women. Loneliness also switches on your body’s long-term “fight-or-flight” stress signaling system, which negatively affects your immune system. People who feel lonely have lower immunity and more inflammation than people who don’t. Dr. Coard recommends the following tips for those who feel lonely. Tips to Increase Social Connection Get outside. More and more nature prescriptions are common. In fact even a 10 minute walk can elevate your mood and get your blood flowing. Develop a schedule of activities to accomplish in a week, setting realistic goals. Monitor your technology. Of course, watching the 24/7 news cycle can be depressing. Turn off the TV and listen to music or read a book instead. Even better, use technology to connect with family members by having a virtual game night or book club discussion. Write it out. When was the last time you sent a good old-fashioned letter or card? Or even wrote in a journal? Try to brighten someone’s day with snail mail. Writing down your hopes and fears also helps you to get worries off your mind and process your emotions. With this in mind, there are also volunteer opportunities to support others by sending a handwritten letter to others battling depression. De-clutter your surroundings. Go through those old photos and put them in an album. Clean out a drawer, cupboard or closet. You will feel a sense of accomplishment and can donate items you no longer need that others can enjoy. Increase your joy by reducing your clutter. Warning Signs of Chronic Loneliness One size does not fit all when it comes to loneliness. For this reason, loneliness can be different depending on your particular situation and your unique personality. However, if you feel some (or all) of the following symptoms, chronic loneliness may be affecting you: Lack of ‘best’ or close friends. You connect with others on a surface level, but feel no one truly understands you. People are n your life, yet you are not connecting on a deep, intimate level with them. You feel lonely even when people are around. This means feeling disengaged or not part of the group when around others. You feel less than enough. You often doubt yourself or don’t feel good enough when comparing yourself to others. And social situations feel exhausting. What Can Someone Do to Feel Less Lonely? Dr. Coard offers the following suggestion for those with a lack of social connections: Talk with your doctor, psychologist or another healthcare professional. Sometimes chronic loneliness relates to longstanding negative beliefs that an individual has about themselves. Engage in behavioral activation. For example, being more active and involved in life by scheduling activities which can potentially improve your mood and decrease feelings of isolation. Initially behavioral activation can be very challenging due to lack of motivation, but setting a reasonable schedule of activities is a good start. Pay attention to your sleep. Sometimes when people become lonely they experience significant changes in their sleep cycle. Frequently they sleep too much, or too little. Make sure to maintain a normal, healthy sleep/wake cycle, following good sleep hygiene recommendations.
Read More About Social Connections: Why They Benefit Your Health
-
Vacunas de refuerzo contra la COVID-19, lo que debe saber
Getting the COVID-19 booster is the best way to protect yourself from severe illness or death due to COVID-19, and both the CDC and the FDA have approved booster shots for people ages 18 and older. So, with the holidays right around the corner and infection rates on the rise both in Nevada and nationally, the best thing you can do to prevent the continued spread of this deadly virus is to get boosted today. The Basics: Who: It is recommended that everyone 18 years or older get a COVID-19 booster shot. When: At least 6 months after completing your primary COVID-19 vaccination series. What: Any of the COVID-19 vaccines authorized in the United States. The CDC allows for mix and match dosing for booster shots. How: To make an appointment for your COVID-19 vaccine booster, please visit vaccines.gov today. Appointment Reminders: Don’t forget to bring your CDC vaccination record card to your appointment. Refresh yourself on the potential side effects and remember that these are normal signs your body is building up protection. Commonly Asked Questions: Q: Does anything change if I received the Johnson & Johnson as my first COVID-19 vaccine? A: If you received the Johnson & Johnson COVID-19 vaccine, you are elidable for a booster two months after completing your primary vaccine. Q: Is the formula the same for the boosters as it was for the primary vaccine? A: COVID-19 booster shots are the same formulation as the current COVID-19 vaccines. However, in the case of the Moderna COVID-19 vaccine booster shot, it is half the dose of the vaccine people get for their primary series. Q: Am I still considered “fully vaccinated” if I don’t receive a COVID-19 booster shot. A: Yes, everyone is still considered fully vaccinated two weeks after their second dose in a two-shot series, such as the Pfizer-BioNTech or Moderna vaccines, or two weeks after a single-dose vaccine, such as the J&J/Janssen vaccine. All information courtesy of the Center for Disease Control and Prevention. All information courtesy of the Center for Disease Control and Prevention
Read More About COVID-19 Booster Shots, What You Need to Know
-
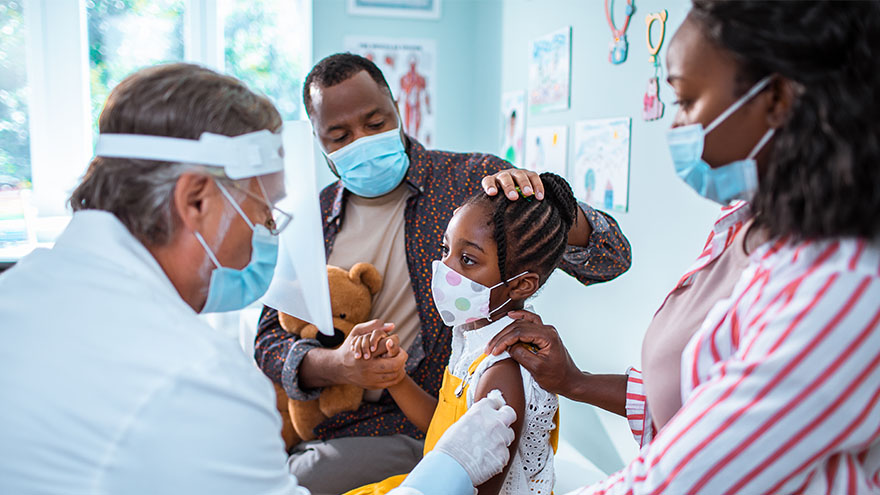
Cómo aliviar el miedo de su hijo a las vacunas
Getting a shot can be scary for kids and anxiety-inducing for parents and caregivers. With flu shot season well underway and children's COVID-19 vaccine clinics in full swing, we wanted to share ways to reduce the stress for you and your child. Plan Ahead and Be Honest A few days before the scheduled appointment, casually mention to your child that you’re both going to the doctor’s office (or vaccine clinic, or pharmacy) soon for their vaccine. Explain to them that this will help protect them and will only take a second. Being honest is important, telling your child that it will hurt for a moment. If possible, try and schedule the vaccine at a kid-specific vaccine clinic, your pediatrician's office or a school-based site. Remember that words are powerful. Take notice if you are using a word that might make them more upset, such as prick, jab, needle or shot. You can interchange words such as vaccine, immunization or injection. Bring Toys Don’t be afraid to let your child bring one of their favorite toys or stuffed animals to the appointment. This can make them feel more comfortable and provide distraction. Ask for Pain Reliever/Numbing Agent If you know from past experience (or suspect) that your child has a needle phobia, talk to the vaccination location ahead of time and ask if they can use a pain reliever or numbing agent before administering the vaccine. Distract. Distract. Distract. Sing a song, tell them a joke, make a funny face. If you can pull your child’s attention away from the needle and make them laugh, they won’t focus all their energy on worrying about the shot. Lead By Example If you haven't gotten your flu shot, COVID shot or COVID-19 booster yet, ask the facility ahead of time if you can also get a shot before your child. Show them that the shot is no big deal and that they will have no problem getting it themselves. Celebrate Don’t be afraid to celebrate this victory with your child once it is over – bring them to the park, go out for an ice cream cone, let them pick what’s for dinner. This reward will show that you’re proud of them for being brave and may also make the next time your child is due for a shot easier.
-
Cuidado confiable desde el hogar
Renown Health has always been on the frontlines of technological advancement, and that innovation remained unwavering during the COVID-19 pandemic. Our telehealth teams heeded the call to provide home monitoring for our patients, transforming how we provide care. The care providers at Renown successfully monitored lower acuity COVID-19 patients from the comfort of their own homes. Bernard Lee was diagnosed with COVID-19 and pneumonia, and was able to return home to continue his recovery with a home monitoring system. While at home, Bernard’s health took a turn for the worse while he was sleeping, but thanks to the continuous monitoring of Health at Home, his worsening vitals did not go unnoticed. “This monitoring system really saved my life,” Bernard said. “It was telling me that my sats were low, but I didn’t even feel the common COVID symptoms; I just felt tired.” Because of his low oxygen saturation (sats) and the continuous monitoring, he woke up to providers calling to check on him in the early morning. He was immediately transferred to the Renown Intensive Care Unit to be cared for and monitored by our expert care teams. Today Bernard is recovering, feeling great and continuously refers to the team and the home monitoring system as his guardian angels.
-
Tips for Coping with Smoke-Related Health Problems
Millions of people across the west live in areas where air pollution can cause serious health problems. In addition, local air quality can affect our daily lives. Who is Affected? Kouros Farro, MD, a physician with Renown Urgent Care, advises that certain people are more likely to be affected when fine particle pollution reaches an unhealthy level. People who have asthma or other breathing conditions like chronic obstructive pulmonary disease (COPD). People who have heart disease or high blood pressure. Children and older adults. People of all ages who are doing extended or heavy physical activity like playing sports or working outdoors. “Everyone should take precautions when the air quality is unhealthy. Air pollution can aggravate heart and cardiovascular disease as well as lung diseases like asthma and COPD. When the air quality is unhealthy, people with these conditions may experience symptoms like chest pain, shortness of breath, wheezing, coughing, or fatigue. If you are experiencing any of these symptoms, use your inhalers as directed and contact your health care provider,” says Dr. Farro, who is board certified in family medicine and practices at Renown Urgent Care at 975 Ryland St. in Reno. “If you do not have a health care provider, there is a Renown Urgent Care office on almost every corner, with providers ready to see you.” Dr. Farro advises the following: Take it easy and listen to your body. Limit, change or postpone your physical activity level. If possible, stay away from local sources of air pollution like busy roads and wood fires. If you have asthma or other breathing conditions like COPD, make sure you have your relief/rescue inhaler with you. People with asthma should review and follow the direction in their written asthma action plan. Make an appointment to see your health provider to be sure you have an asthma action plan. Getting Same-Day Care Renown Urgent Care provides same-day treatment for a wide range of minor injuries, illnesses and medical concerns that are urgent but not life-threatening. Avoid the long wait times and high emergency room prices at 11 convenient sites, including Reno, Sparks, Carson City, USA Parkway, Fallon and Fernley. You can walk in or book ahead online. Make an Urgent Care Appointment Community Health Resources The Washoe County Health District offers online health information on its Smoke Smart website, including fire information, daily air quality information, fire and smoke maps and how to protect yourself. In addition, an online subscription page allows you to sign up for EnviroFlash, notifying you about air quality.
Read More About Tips for Coping with Smoke-Related Health Problems
-
Stay Inside When Skies Are Smoky
Even when fires burn outside our area, the air quality in the region can reach dangerous levels. Our expert explains how to maintain your lung health when fire season strikes. It’s a sight we know all too well as northern Nevadans — a hazy or thick layer on the horizon when smoke rolls in from nearby fires. Sometimes the smoke is more evident than others, but it’s important to remember, even when the smoke may not be as visible across the valley, it still impacts our air quality. The last week or so, our air quality has been in the “unhealthy for sensitive groups” range, which can be dangerous for people who are sensitive to air pollution. Air Quality Changes: Who’s at Risk? Renown Pediatric Pulmonologist Sonia Budhecha, M.D., explains certain people are especially at risk when smoke moves in: Older people, whose lungs are not as healthy as they used to be Young children, whose lungs are still developing People with heart and lung disease including asthma, COPD and emphysema “Smoke and haze from fires carry particulates that can get into your respiratory system and eyes, which can be a danger for all ages,” Dr. Budhecha says. How You Can Protect Yourself Until the smoke clears and the air returns to the “good” range, it is best to follow these tips to protect yourself and your family: Stay indoors and keep windows closed Turn on the air conditioning to recirculate clean air Drink plenty of fluids to help your body flush out any toxins you inhale Additionally, all community members should reduce their physical activity and try to prevent heavy exertion outside. If you or a loved one has a heart or lung disease, avoid physical exertion altogether because smoke can aggravate these conditions. “People with heart disease may experience shortness of breath, chest pain, palpitations or fatigue,” Dr. Budhecha says. “People with lung disease may also have shortness of breath, chest discomfort, wheezing, phlegm or a cough.” Smoky Signs and Symptoms Smoke can also impact healthy people — irritating your eyes, nose or throat. And in some cases, inhaling smoke can lead to bronchitis. When haze moves into our area, keep an eye out for these symptoms: Burning or stinging eyes Runny nose Cough or scratchy throat Headaches Wheezing Shortness of breath Difficult taking a full breath Chest heaviness Lightheadedness Dizziness If experiencing any of the above symptoms, seek medical attention or call your doctor for advice. Sometimes, these symptoms do not appear for as long as 24 to 48 hours after smoke inhalation. For those that have pre-existing lung or heart conditions, consult with a health care provider on action or management plans. To schedule an appointment Visit Renown Pulmonary Medicine, or call 775-982-5000. Understanding Our Air Quality The Air Quality Index (AQI) is broken down by large (PM10) and small (PM2.5) particulates. According to Dr. Budhecha, large particulates are usually ones that can be seen and smelled. They can damage your eyes and nose but don’t often get deep in the lungs or blood vessels. “The more dangerous ones are PM2.5, which can’t always be seen or smelled,” Dr. Budhecha says. “Any time the AQI is above 51, children with lung or heart disease should not be outdoors.” For the latest air quality update in your area, visit AirNow.gov or call (775) 785-4110.
-
The Facts About Menopause and Early Menopause
Menopause is something that every woman experiences at some point in her lifetime. Learn what to expect and how you can help manage the symptoms and health risks. Most women don’t experience menopause until their 50s, but certain factors such as chromosomal abnormalities, glandular problems and chemotherapy can cause early menopause before the age of 40. No matter what your age, it’s a good idea be aware of the risks and treatments available to maintain a comfortable and healthy lifestyle. Health Risks of Menopause Two of the biggest health risks posed to women who have gone through menopause are bone density loss and risk of cardiovascular disease. Bone loss can be treated with bisphosphonate and estrogens. “Calcium with vitamin D and weight bearing exercise will also limit bone loss,” says Vickie Tippett, MD and OB/GYN at Renown Health. For cardiovascular risk, a healthy lifestyle is key. Discontinuing tobacco use, getting regular exercise and maintaining a healthy weight and diet all help reduce a woman’s risk of cardiovascular disease. Managing Discomforts of Menopause One of the most common complaints about menopause is the discomfort of hot flashes. “Hot flashes can be treated with systemic estrogen alone or in combination with progesterone or another agent similar to estrogen,” Dr. Tippett says. “Non-hormonal medications such as SSRIs and antidepressants also work.” Vaginal dryness, another common symptom of menopause, can also be treated with estrogen, estrogen-like compounds and personal lubricants. Pills, patches, creams and many other formulations are available to help alleviate discomfort. Knowing when, why and what to expect when it comes to menopause can help make the transition easier. Learn the facts about menopause in the infographic below.
Read More About The Facts About Menopause and Early Menopause
-
What Every Woman Needs to Know About Dense Breast Tissue
In honor of International Women’s Day, we’re working to spread the word about taking care of your breast health and encouraging the women in your life to do the same. Heather Reimer is on a mission — a mission to educate women everywhere about breast tissue type. For women with dense breasts, knowing your breast tissue type is absolutely critical, as cancers embedded in dense breast tissue are not always detectable with a mammogram alone. Dense breast tissue requires a breast ultrasound screening to get a complete breast health picture. Whole Breast Ultrasound for Dense Breast Tissue Heather knows this firsthand. She has dense breasts, and in this video she shares her story about finding breast cancer during a breast ultrasound screening — cancer that went undetected with her mammogram screening alone. As a result of that experience, Heather founded Each One. Tell One. — a movement to encourage women to pass along this information to others and to prompt those with dense breast and implants to consult with their doctor to schedule a whole breast ultrasound screening. To schedule a mammogram or a whole breast ultrasound, call 775-982-8100.
Read More About What Every Woman Needs to Know About Dense Breast Tissue