Buscar
Results for 'clinic'
Clear-
Padres, sus hijos necesitan vacunas contra la gripe. Este es el por qué
Vanessa Slots, MD, of Renown Medical Group – Pediatrics, explains why getting a flu shot each season can save lives—especially true for the very young and elderly. Why Kids Need Flu Shots The flu is not a passing cold. It is a serious illness that takes lives every year. And this year, flu activity is increasing late in the season. And it happens like clockwork — the onset of an influenza epidemic as fall transitions into winter, and lasts into the spring months. This acute respiratory illness is caused by influenza A or B viruses with yearly outbreaks occurring worldwide. No one is immune, and everyone is susceptible to the flu. Flu Signs and Symptoms: Abrupt onset of fever Headache Body aches and fatigue along with respiratory-tract symptoms including cough Sore throat and an irritated nose Who’s at Risk? Once again: Everyone is susceptible, but children and the elderly are at greater risk of complication from influenza, specifically toddlers less than 2 years. At this age, immunities are underdeveloped. Seniors over 65 are also at increased risk because their immune systems have weakened with age. The severity of a child’s symptoms depend on age and prior exposure to the virus. And with young children, flu is more problematic, since they cannot verbalize certain symptoms like body aches and headaches. As a result, children often experience higher fevers, which can lead to seizures or convulsions. Coupled with gastrointestinal issues such as nausea, vomiting, diarrhea and poor appetite, children are at risk of dehydration and other complications from the virus that can require hospitalization. In fact, an average of 20,000 children are hospitalized from flu each year. Pre-Existing Health Issues Health conditions, including but not limited to asthma, cystic fibrosis, heart conditions, cerebral palsy, epilepsy or diabetes, can intensify flu symptoms. Still, a substantial number of children with none of these risk factors experience severe complications from the flu. How to Protect Your Child from the Flu The best way to guard against influenza is with a flu shot. Children and adults should get the flu vaccine before flu season kicks in — usually by the end of October. Shots are provided as long as flu viruses are circulating and the vaccine is in supply.
Read More About Parents, Your Kids Need Flu Shots. Here's Why.
-
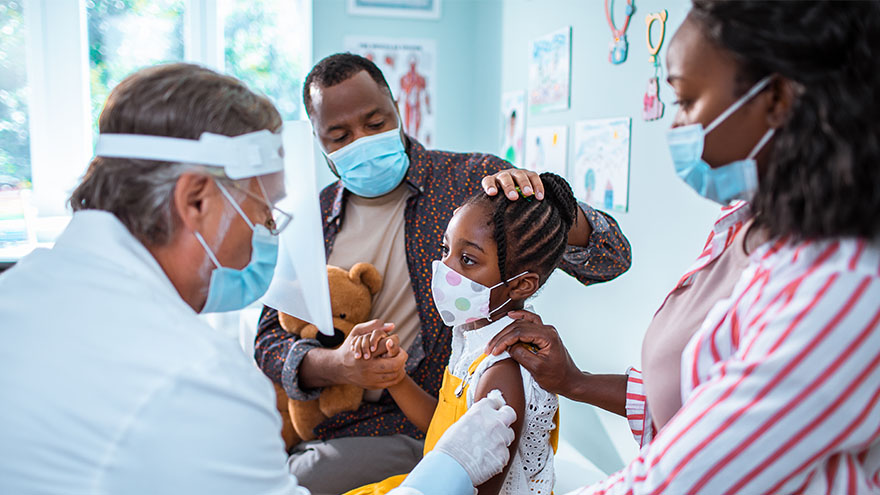
Cómo aliviar el miedo de su hijo a las vacunas
Getting a shot can be scary for kids and anxiety-inducing for parents and caregivers. With flu shot season well underway and children's COVID-19 vaccine clinics in full swing, we wanted to share ways to reduce the stress for you and your child. Plan Ahead and Be Honest A few days before the scheduled appointment, casually mention to your child that you’re both going to the doctor’s office (or vaccine clinic, or pharmacy) soon for their vaccine. Explain to them that this will help protect them and will only take a second. Being honest is important, telling your child that it will hurt for a moment. If possible, try and schedule the vaccine at a kid-specific vaccine clinic, your pediatrician's office or a school-based site. Remember that words are powerful. Take notice if you are using a word that might make them more upset, such as prick, jab, needle or shot. You can interchange words such as vaccine, immunization or injection. Bring Toys Don’t be afraid to let your child bring one of their favorite toys or stuffed animals to the appointment. This can make them feel more comfortable and provide distraction. Ask for Pain Reliever/Numbing Agent If you know from past experience (or suspect) that your child has a needle phobia, talk to the vaccination location ahead of time and ask if they can use a pain reliever or numbing agent before administering the vaccine. Distract. Distract. Distract. Sing a song, tell them a joke, make a funny face. If you can pull your child’s attention away from the needle and make them laugh, they won’t focus all their energy on worrying about the shot. Lead By Example If you haven't gotten your flu shot, COVID shot or COVID-19 booster yet, ask the facility ahead of time if you can also get a shot before your child. Show them that the shot is no big deal and that they will have no problem getting it themselves. Celebrate Don’t be afraid to celebrate this victory with your child once it is over – bring them to the park, go out for an ice cream cone, let them pick what’s for dinner. This reward will show that you’re proud of them for being brave and may also make the next time your child is due for a shot easier.
-
Tips for Keeping Your Kids Safe on ATVs
In the state of Nevada, all-terrain vehicles (ATVs) are one of the pediatric population's top three mechanisms of injury. Kids under 16 are the leading victims of ATV incidents and fatalities because they cannot reach controls, cannot activate controls and they have a restricted field of vision. Tips to Safely Utilize ATVs ATVs are off-road vehicles used for activities such as off-roading and farm work. In the state of Nevada, it is legal for teens to ride them, even without a driver's license. However, even though it is legal for teens to ride these vehicles, it is not always safe. Here are a couple of tips and tricks to stay safe while using ATVs: Be at least 16 years old. Health and safety experts strongly discourage ATV use by anyone younger than 16. Operating an ATV demands that drivers be skilled at making quick adjustments, such as speeding up, slowing down and shifting their weight to help turn the vehicle. People under 16 are less likely to have the physical strength and decision-making experience necessary to drive an ATV safely. Get safety certified. Before you ride an ATV on a trail, learn how to do it safely in a controlled setting. Visit the ATV Safety Institute's website for course information. Ride an ATV that's right for your size and age. Full-size ATVs can weigh more than 600 pounds and be very difficult to handle. Select an ATV designed for you or your child's age group. This sizing can be found on the manufacturer's warning label right on the vehicle. Always wear an approved helmet and eye protection. The best helmets for ATV use have a full-face shield and meet Department of Transportation safety standards. Many helmets have flip-down visors for eye protection. If yours doesn't, be sure to wear shatterproof goggles and not just sunglasses. Wear long pants, long sleeves, gloves and over-the-ankle boots. ATVs have a high center of gravity and no safety cages, roll bars or seatbelts. If they tip, you can fall off. Protective clothing will help prevent scrapes and cuts if you get thrown from an ATV. Always ride at a safe speed on a trail meant for ATV use. When ATVs get going fast, they become less stable and more likely to tip. ATV tires are not meant for pavement or high speeds. Both factors can make turning an ATV difficult and dangerous.
-
Departamento destacado: Children’s Infusion Services
Help us celebrate the holiday season by sharing joy with our Children’s Infusion Services team! Thinking about blood can make any of us squeamish, and seeing it can be even more intimidating to the children in our lives. Being treated for a condition that requires blood transfusions or chemotherapy infusions is no easy feat, especially during the holiday season. This time of year, we are proud that we can offer our pediatric patients the power of proximity and excellence by having access to high level care close to home. The Children’s Infusion Services (CIS) department at Renown Children’s Hospital is committed to bringing the gift of quality care to our community’s youngest patients. Whether they are caring for a child with a blood disorder or giving expert infusion care for a child battling cancer, no team does what they do better than these expert nurses, medical assistants, intake coordinators and physicians. ‘Tis the Season to Bring Hope As the only pediatric oncology and hematology program in the region, the CIS department has a lot of responsibility on their shoulders. From inpatient chemotherapy to outpatient infusion services, this team treats a long list of pediatric blood conditions including: Pediatric cancers Anemias Immune-mediated blood disorders Sickle-cell disease Bone marrow failure syndromes Bleeding disorders “Our team provides a large variety of services from labs draws, sedations for procedures, infusions for diagnoses such as Crohn's disease, blood transfusions, as well as chemotherapy,” said Jen Torres, RN. “Our team works extremely well together. We try to go above and beyond for our patients every day. It may be something as simple as a hug to comfort a parent or a special birthday gift for a patient.” “My job allows me to work with several departments and providers when coordinating care for our littlest of patients,” added Jane Strawn, Intake Coordinator. “I assure proper authorizations are in place for the care that is needed, I communicate with our families when scheduling appointments, I organize End of Treatment Celebrations, as well as birthday shout outs and work closely with our Child Life team to help make the challenging appointment little easier.” To best serve their patients, the team thrives on being expert multitaskers. Central line care, chemotherapy administration, blood transfusions, medication management, preventative injections, lab draws, lumbar punctures, biopsies, imaging – you name it, they do it. And they do it all with the utmost focus on safety and support. “Our days have a lot of variation, as we perform a number of different services,” said Meagan Bertotti, RN. “We provide infusions for patients with chronic or acute medical conditions and chemotherapy/biotherapy treatment to patients undergoing cancer treatments. Overall, though, we work as a team to make these difficult procedures and treatments as easy as possible for the patients and families by providing engagement and support.” “While we handle a lot of chemotherapy treatments for pediatric patients, we also do other infusions and transfusions as well such as blood and platelet transfusions, enzyme replacement therapies, different types of injections such as Rabies vaccine or Synagis for high-risk babies who need that extra protection during the RSV season, and lab draws,” said Chelsea Angues, RN. “We care for patients that get their therapies from outside hospitals, but the patient lives within the Reno area. We receive orders from those outside hospitals to care for those patients, so they can still be with their families and not have to travel.” As members of the Children’s Oncology Group, a highly-regarded clinical trials group where over 90% of pediatric cancer patients across the U.S. receive treatment, teams like CIS in Renown Children’s Hospital deliver the highest standard of care. This partnership is a true testament to the devoted collaboration and relationship-building this team commits to on behalf of their patients every day. "One of the biggest accomplishments of our team is the fact that we became a member of the Children’s Oncology Group, and the Children's Infusion Center and Pediatric Oncology became one unit,” said Shelby Nolte. "Instead of being a clinic on one side and an infusion center on the other, we really came together to make it a whole unit that collaborates on almost everything.” “We've put much time into trying to understand other departments, their flow, their rationales and their processes so we can come to a solution that benefits our patients the greatest,” added Tiffany Macie, RN. “We've taken the last few years to really build our relationships with our pharmacy staff, our lab staff and our central supply resources. Our relationship building extends beyond the walls of the Renown building as well and out to the community providers too. In the past few years, we've been able to build relationships with the providers in the community where they trust they can send us their patients for treatment and lab draws. Finally, we've spent much time working on the relationships as a team. It's emotional work we do on our unit, and these families become our family. It's important to us that we take the time to be together outside of our shifts to enjoy one another and laugh!” In the compassionate realm of pediatric healthcare, CIS knows that the complexities of a cancer or blood disorder diagnosis can take an emotional toll on their patients and families. The team firmly believes that emotional support can be as important as the physical and medical support throughout each patient’s unique care journey, striving to be a comforting presence during daunting times. “The most important part of my day is collaborating with the Children's Infusion team to make life manageable for the families that are going through this experience,” added Shelby Nolte, Senior Medical Assistant. “We work as a team to make life easier for the blow of a cancer diagnosis. We are there for our families in every way. If they need a shoulder to cry on, an ear to listen or just someone to play cards with or tell a funny story too, we are there.” “One of the things our team does extremely well to help our patients and their families with new diagnoses is to simply meet them where they are,” said Tiffany Macie. “That looks different for every family and every patient. We work in an environment where can build relationships with our patients and their families. This allows us the unique opportunity to really get to know them. We learn their fears, their joys, their worries, what their family lives are like, and we learn how to best meet them where they are.” Transcending the conventional boundaries of care, the CIS department closely supports each patient, offering them solace tailored to the unique fabric of each family's life.
Read More About Department Spotlight: Children’s Infusion Services
-
Tummy Trouble? Renown Children’s Hospital Adds Another New Specialty, Pediatric Gastroenterology
Two pediatric gastroenterologists bring life-saving care to kids and make Renown their new home The Renown Children’s Hospital team and our community is celebrating the addition of a new life-saving pediatric specialty to its practice serving children and families in northern Nevada. Parents and guardians will now be able to seek professional pediatric gastroenterologist care with the addition of Drs. Juan Gregory and Kathleen Holland to Renown Medical Group. “Recognizing the importance of diagnosing and caring for children who have conditions that affect the organs in the digestive system, including the stomach, liver and bowel, while also helping children who have issues feeding and eating, is critically important to us at Renown,” said Kristina Deeter, MD, MBA, FAAP, Chair of Pediatrics, University of Nevada Reno School of Medicine (UNR Med) and Physician-in-Chief, Renown Children’s Hospital. “Both Drs. Gregory and Holland are superb clinicians, we are excited to have them join Renown Children’s Hospital to offer pediatric gastroenterology services, including a wide range of complex and vital procedures and screenings, endoscopies and colonoscopies.” Juan Carlos Gregory, MD, has 18 years of experience caring for children in northern Nevada. He is a clinical associate professor of pediatrics at UNR Med with a special interest in celiac disease, abdominal pain, and gastroesophageal reflux in children. Gregory earned his undergraduate degree at Texas Christian University in Fort Worth, TX before completing his medical training, including a residency in pediatrics at the University of San Diego in Pediatrics and fellowships in Pediatric Gastroenterology and Nutrition at both Children’s National Medical Center in Washington, DC, and at the National Institutes of Health, Digestive Disease Section in Bethesda, MD. He is board-certified in Pediatric Gastroenterology and speaks Spanish. Kathleen Holland, MD, MPH brings a global health perspective to her work caring for children. A graduate of the University of Nevada Reno School of Medicine (UNR Med) with her medical doctorate and her master’s in public health with a social and behavioral health emphasis, she has donated her skills to providing international medical relief for children in Uganda and Nicaragua. Holland earned her undergraduate degree at University of Nevada Reno in Biology, Health Ecology and Healthcare Ethics before completing her medical training and residency in Pediatrics and a fellowship in Pediatric Gastroenterology at Indiana University School of Medicine in Indianapolis, IN. Her research and scientific interests include vaccination rates and family barriers among children with inflammatory bowel disease, Crohn’s and colitis, pediatric autoimmune pancreatitis, and cystic fibrosis. How Pediatric Gastroenterologists Help Children and Families The Pediatric Gastroenterology Program at Renown Children’s cares for children experiencing common GI-related problems of childhood; nausea, vomiting, abdominal pain, diarrhea, constipation, reflux, colic, milk protein allergy, poor growth and feeding difficulties, and sees patients from infancy to 18 years old. “As specialists in the care of children with gastrointestinal and liver problems, we focus on the diagnosis and treatment of these issues,” said Larry Duncan, MD, Vice President of Pediatrics and Surgery & Administrator of Renown Children’s & Women’s Services. “Our physicians play an active role in teaching and research. We have several areas of expertise including prevention, diagnosis and treating disease of the digestive tract including the esophagus, gallbladder, stomach, pancreas, colon, small intestine and liver disease.” Special expertise includes: Pediatric feeding and growing disorders Aerodigestive disorders Food and hypersensitivity disorders Inflammatory bowel disease Celiac disease Liver diseases Children requiring parenteral and enteral nutrition Renown Children’s Hospital is the only dedicated children’s hospital in northern Nevada, offering programs and services for families from a 100,000 square mile area, from Sacramento, CA to Salt Lake City, Utah. Renown Children’s provides the area’s only Children’s Emergency Room, Pediatric ICU (PICU), children’s imaging center and the largest neonatal ICU (NICU), a level III intensive care unit. Specialty Children’s Care at Renown Today, over 90% of families in northern Nevada seek care from the experts at Renown Children’s Hospital. “We are so grateful to the William N. Pennington Foundation for its support in establishing the William N. Pennington Fund for Advance Pediatric Care in 2016, which allowed us to hire our first 15 pediatric specialists,” said Dr. Deeter. “Today we have over 40 pediatric physician specialists at Renown Children’s Hospital who provide care in adolescent medicine, pediatric endocrinology, pediatric hematology/oncology, pediatric pulmonology, pediatric neurology, pediatric nephrology, pediatric infectious diseases, pediatric ophthalmology, pediatric orthopedic surgery, pediatric cleft and craniofacial surgery, pediatric urology, pediatric dentistry, pediatric emergency medicine, and now, pediatric gastroenterology. Our clinicians provide 30,000 patient visits annually, offering an exceptional level of care. The Pennington gift is truly a gift that keeps giving to the families in our area.” Now Being Constructed: Expanded Inpatient Care at Renown Children’s Hospital New construction of an expanded Neonatal Intensive Care Unit (NICU) with increased capacity to 49 bassinets, an expanded Pediatric Intensive Care Unit (PICU) with increased capacity to 16 private patient and family rooms, and a new Renown Children's Hospital inpatient floor with increased capacity for 38 private patient and family rooms for a total capacity of 58 pediatric beds are currently being constructed on Tahoe Tower, Level 5 of Renown Regional Medical Center. It is expected that the new units will open to patients and families in April 2023. In the most recent US News & World Report Best Hospital rankings, Renown Regional Medical Center was named as the number one hospital in Nevada. Ningún otro hospital del estado cumplió con sus estrictos estándares para el ranking de 2021. Renown Health is High Performing, its highest rating possible, in eight procedures and conditions including Heart Failure, Colon Cancer Surgery and Chronic Obstructive Pulmonary Disease, Hip Replacement and Knee Replacement. A hospital's score is based on multiple data categories, including patient outcomes, safety, and volumes. Los hospitales calificados como sobresalientes eran significativamente mejores que el promedio nacional. Renown Medical Group is an in-network provider for Hometown Health and other health plans. Drs. Gregory and Holland are pleased to see new patients at their location at the Renown Children’s Subspecialty Clinic inside Renown Regional Medical Center at 75 Pringle Way, Suite 505, Reno, Nev. Ask your pediatrician for a referral to a medical specialist when further evaluation of a particular issue is necessary. About Renown Health Renown Health is Nevada’s largest, not-for-profit integrated healthcare network serving Nevada, Lake Tahoe, and northeast California. With a diverse workforce of more than 7,000 employees, Renown has fostered a longstanding culture of excellence, determination, and innovation. The organization comprises a trauma center, two acute care hospitals, a children’s hospital, a rehabilitation hospital, a medical group and urgent care network, and the locally owned not-for-profit insurance company, Hometown Health. Renown is currently enrolling participants in a community-based genetic population health study, the Healthy Nevada Project®. About UNR Med The University of Nevada, Reno School of Medicine (UNR Med), Nevada’s first public medical school, is a community-based, research-intensive medical school with a statewide vision for a healthy Nevada. Since 1969, UNR Med has trained more than 3,900 students, residents, and fellows. UNR Med continues to improve the health and well-being of all Nevadans and their communities through excellence in student education, postgraduate training and clinical care, research with local, national and global impact and a culture of diversity and inclusion. For more information, visit med.unr.edu.
-
A Day in the Life of a Child Life Specialist
March is Child Life Month, meaning this is the perfect time to ask: What exactly does a Child Life Specialist do? To find out, we “virtually” tagged along with one for a day. This is what a typical day looks like in this important role. For Child Life Specialist Brittany Best, play is a natural part of her work day. She approaches her role with a keen understanding of how the seemingly small tasks she performs every day — comforting children prior to a procedure, writing thank-you notes to donors, training interns — positively impact the lives of the children she serves and their families. So what does it take to work in Renown’s Child Life Program? Best shares some of the highlights from a “typical” shift. A Child Life Specialist’s Day 7:30 a.m. Clock in, put my belongings in my office, and print the patient census information. This helps me to get a sense of the day ahead, as I’m covering three areas today. 8-9 a.m. I look over the census sheets for all three areas and check in with the nurses in each area and then try to prioritize my day. 9:00 a.m. I attend Interdisciplinary Rounds for the Pediatric Intensive Care Unit, where the most critically ill or injured children are treated. Additionally, Interdisciplinary Rounds enable several key members of a patient’s care team to come together and offer expertise in patient care. 10:00 a.m. I come up to the specialty clinic/infusion center to check on the patients that have arrived already and see how things have been going since I had last seen them. We see patients frequently up here, as they are receiving treatment for cancer or other disease processes. 10:55 a.m. I’m notified by an RN that a patient needs an IV started, so I go meet with the patient and their family. I meet with a 6-year-old and mother to explain what an IV is and why it is needed. We go through an IV prep kit, looking at all the different items the nurse will use including cold stinky soap, a tight rubber band and also a flexible straw. I also teach this patient a breathing exercise to help them relax during the procedure with a simple exercise known as “smell flowers, blow out candles.” I demonstrate how to take a deep breath in through the nose — like smelling flowers — then how to blow that breath out — like blowing out birthday candles. 11:10 a.m. I walk with the patient and mom to the procedure room on the Children’s Patient Floor for an IV procedure. The Vecta distraction station is set up and running with its bright lights and water tube that bubbles with plastic fish swimming. The parent holds the patient in their lap, and with the distraction and medical preparation, we are successful! I give the patient a toy and provide emotional support to both the young patient and his mom. It’s easy to forget that these procedures can be stressful for the parents as well. 11:30 a.m. I finish rounding with staff to catch up on patients. In addition, I introduce myself to patients and put my contact number on the board in each room so the families know how to get a hold of me should they need anything. With support from volunteers, we distribute movies, games, and “All About Me” forms to patients and their families. These forms help us get to know our patients with things like their favorite foods and televisions shows. 12:45 p.m. I help with a lab draw in Children’s Specialty Care. A 3-year-old patient is very anxious about the “shot,” so I meet with the patient and parents to discuss coping techniques. The patient holds the Buzzy Bee and does well during the lab draw. The mom is relieved, and the patient is excited for a toy. The Buzzy Bee actually helps block the transmission of sharp pain on contact through icy numbing and also tingly vibration. 1 p.m. Joan, an artist with our Healing Arts Program, arrives on the Children’s Patient Floor to perform art therapy with patients. She helps two young patients who are interested in watercolor paintings. 1:15 p.m. Time for lunch and also a trip to Starbucks. 1:45 p.m. I finishing rounding and introducing myself and our services to the patients I have not met yet. 3 p.m. At this time, I meet with the parents of a newly diagnosed diabetic patient who is in intensive care. A new chronic diagnosis is always difficult, so I am there to provide emotional support. It’s instances like this that remind me every day why I love the work I do. 3:30 p.m. I meet with a new volunteer, discuss their role and also give the new volunteer a tour of the units. We are very thankful for all our volunteers on the floor, as their contributions help us provide a variety of basic services to a larger number of children. This also allows the Child Life Specialist to devote time to children who require more intense or specialized service. 4-5 p.m. I finish charting on patients and help two newly admitted families before I start to wrap up for the day. This evening we have a volunteer covering the times during shift change, which is helpful as it makes for a smooth transition for families during the meal time and change of shift. During this time, I write a note for this volunteer indicating the patients I want her to focus on. 5-5:30 p.m. Check in with critical patients and families before leaving for the day. All-in-all, it was a good day.
Read More About A Day in the Life of a Child Life Specialist