Buscar
-
Optimizing Mammogram Screenings: A Genetic Approach to a Personalized Screening Schedule
Breast cancer screening has long been a cornerstone of women's healthcare. With 1 in 8 women diagnosed with breast cancer in their lifetime1, the United States Preventive Services Task Force (USPSTF) has developed screening recommendations to help detect early-stage cancer. Notably in 2023, the USPSTF revised the recommended age for biennial mammogram screenings for women with average risk to start at age 40 instead of 502, estimated to result in 19% more lives being saved3 by starting screening earlier. While initiating screening at an earlier age offers advantages to a wide demographic, concerns about the potential of over-screening prompted research into the feasibility of identifying women with lower breast cancer risk who could safely delay mammograms. While guidelines address high-risk individuals, a notable gap exists in providing recommendations tailored to those at lower risk. To gain insight into a patient's risk level, physicians are able to utilize genetic testing to understand an individual's genetic makeup, providing precise insights into their predisposition to various health conditions, including breast cancer. Armed with this genetic information, healthcare providers could craft tailored screening strategies that align with an individual’s specific risk profile. This genetic risk-based approach underscores the value of genetics in individualizing the onset of screening to help avoid over-screening and its associated costs. Surprisingly, genetic information is not currently being widely utilized to identify women at risk of breast cancer or other diseases in clinical practice, despite its potential to make a significant positive impact for patients. A recent retrospective analysis of 25,591 women from the Healthy Nevada Project4 sheds light on the potential benefits of this genetic risk-based approach. The study classified 2,338 (9.1%) of these women as having a low genetic risk for breast cancer. What's remarkable is that these women exhibited a significantly lower and later onset of breast cancer compared to their average or high-risk counterparts. This finding suggests that it might be safe for low-risk women to delay mammogram screening by 5 to 10 years without compromising their health.
-
Ladies! Get Screened for Breast Cancer
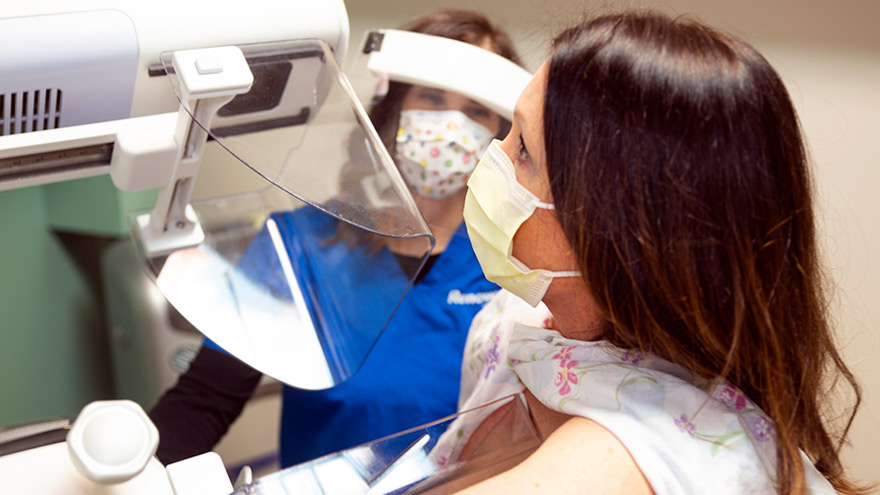
Early detection is a significant piece of the breast cancer puzzle. Susan Cox, Renown Health Director of Cancer Operations, discusses what you need to watch for and how the latest technology can help detect potential cancer sooner. When should women start getting breast exams? It depends on risk factors: Average-risk women: Most medical organizations recommend the first mammogram between 40 and 44. Higher-risk women: Dependent on their high risk, which will dictate when they start screening, but generally around the age of 30 and not before 25 years old.
-
What is Dry Drowning?
Whether you're a parent, grandparent, caregiver or sibling, you should know drowning is the second leading cause of death among children. Yet, while we are vigilant about protecting children from water accidents and drowning, a condition known as dry drowning or delayed drowning can go unnoticed. In fact, most people aren't even aware it exists. Dry drowning defined Dry drowning is a side-effect of a near-drowning experience and includes spasms of the vocal cords and larynx — known as a laryngospasm. This occurs when the body attempts to shut down the passage of any liquid into the lungs. Unfortunately, it can also shut down the passage of air into the lungs and force fluid into the stomach and lungs. Often the condition is not discovered until it's too late — severe cases can cause death within one to 24 hours after a water incident occurs. Who is susceptible? Novice or first-time swimmers are at increased risk, as are children with asthma and known breathing issues. In addition, children who have had pneumonia or experienced acute respiratory distress syndrome are also at greater risk. To reduce these factors, caregivers should be exceptionally watchful of inexperienced swimmers. According to Leland Sullivan, MD, of Northern Nevada Emergency Physicians, children under the age of 5 are most susceptible to drowning and often drown in residential swimming pools. Infants less than 1-year-old most often drown in bathtubs. What are the signs of a dry drowning episode? If your child has a near-drowning incident, a few moments of coughing until they calm down is normal. However, you should know the more severe signs and symptoms to watch for during the 24 hours following the incident, including: Persistent coughing Difficulty breathing and/or shortness of breath Chest pains Extreme fatigue and/or lethargy Change in typical behavior Face becomes pale What is the treatment and prognosis for dry drowning? Dr. Sullivan recommends that all victims of near-drowning incidents seek medical attention, even if they have no symptoms. If caught early, dry drowning can be treated. If you think your child is experiencing a dry drowning episode, go to the nearest emergency room as quickly as possible — do not attempt treatment at home. Healthcare professionals will work to supply oxygen to your child's lungs to restore and regulate breathing.
-
Celebrating Renown Health's Nursing Excellence Conference
Renown Health recently wrapped up the twentieth annual Nursing Excellence and Excellence in Critical Care Conferences, the conference theme was the Courageous Calling and over 400 nurses from specialty fields across the region attended to learn, reflect, build relationships and obtain continuing education units (CEUs). Celebrating The Courageous Calling During the first day of the Nursing Excellence Conference, local and national leaders presented topics including redefining resilience, documentation liability, transgender healthcare and caring for the homeless population. Among the list of impressive speakers were Chief Nurse Executive at Renown Health, Melodie Osborn, and Nora McInerny, writer and host of the "Terrible Thanks for Asking" podcast. On day two,speakers focused on the critical care specialties within nursing, including intensive care, emergency room, pediatric intensive care and neonatal intensive care. Topics covered included post-COVID-19 pulmonology with Dr. Graham, traumatic brain injuries with Dr. Demers, COVID-19 reflections with Anicia Beckwith, a discussion about "Mis C” with Dr. Healy, innovations in imaging with Dr. Rangaswamy and cardiology with Dr. Danaf. Thank you to our sponsors and raffle donors for making this event possible: Erik Olson and Larry Duncan, Jana Elliott, Melodie Osborn, Becky Haase, Lori Tuntland, Dr. Akbar, Dr. Lous, Mel Morris, Grand Sierra Resort, Renown Health Gift Shops, Renown Health Directors of Nursing, Renown Health Marketing & Communications Department, Renown Health Dermatology, Laser, & Skin Care and Renown Health Foundation. Learn more about finding purpose in the health of our community when working at Renown Health here.
Read More About Celebrating Renown Health's Nursing Excellence Conference
-
What You Need To Know About Cold Water Drowning
Northern Nevada is home to some of the most gorgeous and pristine lakes in the country — but also some of the most unforgiving. Lake Tahoe water temperatures average 50 degrees in the summer, making the danger of hypothermia real and always present. Here are the signs, symptoms and ways to prevent cold water drowning. When we think of air temperature at 50 degrees Fahrenheit, it’s not all that cold. But when it comes to water that’s 50 degrees, there is no comparison. Immersion in cold water is life threatening and can happen within a minute. Taking the right precautions before entering the water can save your life. The 4 Phases of Cold Water Drowning 1. Cold Shock Response: This response affects breathing and happens within the first minute. An automatic gasp reflex occurs in response to rapid skin cooling. If the head goes below water, water may be breathed into the lungs, resulting in drowning. A life jacket will help keep your head above water during this critical phase. Additionally, hyperventilation, like the gasp reflex, is a response to the cold and will subside. Panic will make this worse, so the key is to control breathing. 2. Cold Incapacitation: This response occurs within the first five to 15 minutes in cold water. In order to preserve core heat, vasoconstriction takes place decreasing blood flow to the extremities to protect the vital organs. The result is a loss of movement to hands, feet, arms and legs. Unless a life jacket is being worn, the ability to stay afloat is next to impossible. 3. Hypothermia: Important to note, it can take 30 minutes or more for most adults to become hypothermic. So there’s time to take action and survive. Keeping panic at bay is critical, as you have more survival time than you think. Symptoms include: Shivering Slow and shallow breathing Confusion Drowsiness or exhaustion Slurred speech Loss of coordination Weak pulse 4. Circum-rescue Collapse: This experience can happen just before rescue and is not well understood. Symptoms range anywhere from fainting to death. Some experts believe an abrupt drop in blood pressure may cause this final stage of cold water drowning, post-rescue. Additional Cold Water Drowning Safety Tips and Helpful Resources Always wear a personal flotation device as well as a wetsuit or drysuit. Your personal flotation device is the most important piece of water safety gear. Try not to panic as the first phases will subside. Controlled breathing is to staying calm. Research suggests the body can withstand the cold longer than we think. The Heat Escape Lessening Posture (HELP) is a position which helps conserve energy if you’re wearing a personal flotation device. By hugging your knees to your chest, this posture helps maintain body heat for some time.
Read More About What You Need To Know About Cold Water Drowning
-
SOGI – The Most Important Terms to Know
SOGI stands for sexual orientation and gender identity. Being a SOGI-inclusive medical facility means regardless of our differences, we treat others with dignity and respect. Sean Savoy, Renown Health Manager of Spiritual Care, explains SOGI terms and their importance in a healthcare setting below. SOGI History Although the UN passed a historic resolution on SOGI in 2016, it is still a relatively new term for some. Above all, an inclusive environment where every patient feels safe and valued, improves the quality of care in our community. In reality, defining gender and sexuality can be confusing. However, the terms we use to define gender and sexuality are an important influence on how we relate to each other. Generally, "sex" refers to the biological differences between males and females. Still the term “sex” doesn’t fully capture the complex biological, anatomical and chromosomal variations that can occur. Accordingly, having only two (binary) options – biological male or biological female – might not describe what’s going on inside a person’s body. In essence, assigned sex (also called "biological sex) is given at birth based on medical factors. These include your hormones, chromosomes and genitals. Most people are assigned male or female, and this is what’s put on their birth certificate. When someone’s sexual and reproductive anatomy isn’t clearly female or male, that person may be described as “intersex.” However, a person’s biological or assigned sex may be different from a person’s actual or perceived gender identity or expression. The word “gender,” therefore, is more difficult to define. It could refer to the gender or sex role society determines is acceptable, desirable or appropriate based on a person’s perceived sex. Likewise, it could refer to an individual’s own gender identity or preferred gender expression. What is Gender Identity? To summarize, gender identity is one's innermost concept of self as male, female, a blend of both or neither. To clarify - how individuals perceive themselves and what they call themselves. Of course sometimes a person's genetically assigned sex does not line up with their gender identity. These individuals might refer to themselves as transgender, non-binary, or gender-nonconforming, for example. Another key point is the process of gender transition. This specifically refers to more closely aligning your internal knowledge of gender with your outward appearance. According to the American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders (DSM), the term – which replaces Gender Identity Disorder – "is intended to better capture the experiences of affected children, adolescents, and adults." What is Sexual Orientation? Sexual orientation is an internal or enduring emotional, romantic or sexual attraction to other people. For example, you could be heterosexual (straight), gay, lesbian, bisexual or even pansexual. SOGI Terms to Know Below are some common SOGI terms according to the National LGBT Health Education Center and the Human Rights Campaign. The following list is not meant to represent every term (or definition) used by the LGBTQ+ community. LGBTQ+ Stands for lesbian, gay, bisexual, transgender and queer (or questioning). The plus encompasses other identities that fall under the queer umbrella with one common theme: they are not strictly straight or cisgender. Queer An umbrella term used by some to describe people who think of their sexual orientation or gender identity as outside of societal norms. Some people view the term “queer” as more fluid and inclusive than traditional SOGI identities. Due to its history as a derogatory term, the term is not always embraced or used by all members of the LGBTQ+ community. Sexual Orientation Terms Asexual (adj.) – Describes a person who experiences little or no sexual attraction to others. Asexuality is not the same as celibacy. Bisexual (adj.) – A sexual orientation that describes a person who is emotionally and sexually attracted to people of their own gender and people of other genders. Gay (adj.) – A sexual orientation that describes a person who is emotionally and sexually attracted to people of their own gender. It can be used regardless of gender identity, but is more commonly used to describe men attracted to other men. Heterosexual or Straight (adj.) – A sexual orientation that describes a person whose sexual or emotional attractions and behaviors focus exclusively or mainly on members of the opposite sex or gender identity. Lesbian (adj., noun) – A sexual orientation that describes a woman who is emotionally and sexually attracted to other women. Pansexual or Omnisexual (adj.) – A sexual orientation that describes a person who is sexually and emotionally attracted to people of any sex or gender identity. Pansexual people may refer to themselves as gender-blind, asserting that gender and sex are insignificant or irrelevant in determining whether they will be sexually attracted to others. Gender Identity Terms Bigender or Binary (adj.) – Describes a person whose gender identity is a combination of two genders. Cisgender (adj.) – A person whose gender identity aligns with the assigned sex at birth or biological sex. Gender non-conforming (adj.) – Describes a gender expression that differs from a given society’s norms for males and females. Gender transition (noun) - The process by which some people strive to more closely align their internal knowledge of gender with its outward appearance. Some people socially transition, whereby they might begin dressing, using names and pronouns and/or be socially recognized as another gender. Others undergo physical transitions in which they modify their bodies through medical interventions. Intersex (adj.) - A variation in sex characteristics including chromosomes, gonads, or genitals that do not allow an individual to be distinctly identified as male or female. Non-binary Alternate terms are gender queer and gender non-conforming. Transgender (adj.) – Describes a person whose gender identity and assigned sex at birth do not correspond. Also used as an umbrella term to include gender identities outside of male and female. Sometimes abbreviated as trans. SOGI Awareness Again, not all people use the above terms in the same way, so respect and sensitivity are key. And the healthcare setting is an especially vulnerable one. Maintaining the dignity and humanity of every individual during a medical interaction is essential. The U.S. Department of Health and Human Services requires all Electronic Health Record (EHR) systems be able to collect SOGI information from patients. This promotes better understanding of health treatment outcome disparities in order to reduce them. Renown Health’s mission is to make a genuine difference in the health and well-being of the people and communities we serve.
-
3D vs Whole Breast Ultrasound Which is Right for You
Breast cancer is the leading cause of cancer deaths in women in the U.S. That’s why early detection is so important. Dr. George Krakora, a radiologist with Renown Institute for Cancer, explains what to watch for and how new technology can lead to early detection. Most women know the importance of breast health and staying current with annual breast exams, but may not know that both screening guidelines and technology is evolving. So we asked George Krakora, MD, a radiologist for the Renown Institute for Cancer, what every woman should know about breast cancer detection and which screening method is right for them. First off, when should women start getting breast exams? Generally, women should start getting breast exams using mammography or ultrasound after they turn 40 years old. But we also want women ages 18 to 39 to talk to their primary care provider and ask for what’s called a formal risk assessment to see if screening is needed sooner. And you want to make sure your care provider is giving you a breast exam starting at age 25. It’s also a good idea to be familiar with how your breasts look and feel so you can report any changes to your care provider. What are the risk factors for breast cancer? Are there any preventive steps women can take? There a few risk factors you can’t control, like your age, family history of breast or other cancers, and if you have dense breast tissue. Your risk for breast cancer increases as you get older, and most breast cancers are diagnosed after age 50. Knowing your family history is important because a history of cancer and shared lifestyle can raise your risk. Your breast density can also increase your risk: Women with high breast density are four-to-five times more likely to get breast cancer than women with low breast density. But the good news is there are quite a few things you can do to prevent breast cancer, like not smoking, watching your alcohol intake, and maintaining a healthy weight with good diet and exercise. There are a lot of newer screenings out today. What is the difference between 2-D and 3-D mammography? In a 2-D mammogram, the tech takes X-rays of the breast. These pictures can show the radiologist if there are any lumps or tumors you might not be able to feel. In 3-D mammography, the process is largely the same but more X-rays are taken and it takes a few seconds longer for each image. This kind of exam detects 41 percent more cancers and reduces the number of false-positive results given to patients. This improvement in technology is great for both patients and their care providers. 3-D mammography provides better images of the breast, which allow doctors to more clearly diagnose and avoid false positives, especially in women with dense breast tissue. And what about a whole breast ultrasound. What is that? A whole breast ultrasound uses sound waves to detect cancerous tumors in the breast without using any radiation — it’s an ultrasound just like pregnant women get to check up on their baby. And the exam only takes about 20 minutes. We recommend these exams for patients whose mammograms have shown that they have dense breast tissue. Dense breast tissue can make it harder for doctors to see any abnormalities, lumps or tumors in a mammogram, so this technology ensures better early detection.
Read More About 3D vs Whole Breast Ultrasound Which is Right for You
-
The Facts About Menopause and Early Menopause
Menopause is something that every woman experiences at some point in her lifetime. Learn what to expect and how you can help manage the symptoms and health risks. Most women don’t experience menopause until their 50s, but certain factors such as chromosomal abnormalities, glandular problems and chemotherapy can cause early menopause before the age of 40. No matter what your age, it’s a good idea be aware of the risks and treatments available to maintain a comfortable and healthy lifestyle. Health Risks of Menopause Two of the biggest health risks posed to women who have gone through menopause are bone density loss and risk of cardiovascular disease. Bone loss can be treated with bisphosphonate and estrogens. “Calcium with vitamin D and weight bearing exercise will also limit bone loss,” says Vickie Tippett, MD and OB/GYN at Renown Health. For cardiovascular risk, a healthy lifestyle is key. Discontinuing tobacco use, getting regular exercise and maintaining a healthy weight and diet all help reduce a woman’s risk of cardiovascular disease. Managing Discomforts of Menopause One of the most common complaints about menopause is the discomfort of hot flashes. “Hot flashes can be treated with systemic estrogen alone or in combination with progesterone or another agent similar to estrogen,” Dr. Tippett says. “Non-hormonal medications such as SSRIs and antidepressants also work.” Vaginal dryness, another common symptom of menopause, can also be treated with estrogen, estrogen-like compounds and personal lubricants. Pills, patches, creams and many other formulations are available to help alleviate discomfort. Knowing when, why and what to expect when it comes to menopause can help make the transition easier. Learn the facts about menopause in the infographic below.
Read More About The Facts About Menopause and Early Menopause
-
What Every Woman Needs to Know About Dense Breast Tissue
In honor of International Women’s Day, we’re working to spread the word about taking care of your breast health and encouraging the women in your life to do the same. Heather Reimer is on a mission — a mission to educate women everywhere about breast tissue type. For women with dense breasts, knowing your breast tissue type is absolutely critical, as cancers embedded in dense breast tissue are not always detectable with a mammogram alone. Dense breast tissue requires a breast ultrasound screening to get a complete breast health picture. Whole Breast Ultrasound for Dense Breast Tissue Heather knows this firsthand. She has dense breasts, and in this video she shares her story about finding breast cancer during a breast ultrasound screening — cancer that went undetected with her mammogram screening alone. As a result of that experience, Heather founded Each One. Tell One. — a movement to encourage women to pass along this information to others and to prompt those with dense breast and implants to consult with their doctor to schedule a whole breast ultrasound screening. To schedule a mammogram or a whole breast ultrasound, call 775-982-8100.
Read More About What Every Woman Needs to Know About Dense Breast Tissue