Buscar
-
When Should You Consider Hospice? 5 Important Signs
Deciding on hospice care for a loved one is a deeply personal and challenging decision, balancing their wishes and medical realities. Rebecca Edwards, DNP, from Renown Hospice Care, explains the signs indicating when it might be time for hospice and offers guidance on navigating this decision with compassion and clarity. Understanding Hospice Care Before exploring the decision-making process, it’s crucial to have a clear understanding of what hospice means. Hospice care represents a shift in how we approach living with a terminal condition, emphasizing comfort, dignity, and quality of life above all else. When there is no longer a pathway to a cure, side effects of treatment outweigh the benefits, or someone is simply tired of frequent hospital visits, then it may be time for hospice. Hospice care is mainly done in the home, where most people wish to be. It's a compassionate, team approach to care that focuses on meeting the physical, emotional, and spiritual needs, supporting their families, and honoring individual preferences. 5 Critical Signs to Be Aware Of Decline in Overall Health: When a loved one's health continues to decline despite ongoing medical interventions, this may be a sign that these treatments are no longer effective. Increasing Pain and Symptoms: When managing symptoms such as pain, nausea, fatigue or shortness of breath becomes increasingly challenging, hospice can offer specialized support and expertise in symptom management. Frequent Hospitalizations: Repeated hospitalizations or emergency room visits can signify that the disease has progressed to a point where managing symptoms and providing comfort at home or in a hospice setting is a more appropriate approach. Difficulty with Daily Activities: If your loved one is experiencing difficult with activity of daily living such as dressing, bathing, or mobility, it may be a sign that they require additional support and assistance. Prognosis of Six to 12 Months: Hospice Care is typically recommended for patients with a prognosis of about one year or less if the disease follows its normal course. However, it’s important to remember that every individual is unique and prognosis can vary.
Read More About When Should You Consider Hospice? 5 Important Signs
-
Departamento destacado: Surgery & Procedure Scheduling
When it comes to intimidating procedures such as surgery, cardiac catheterization (Cath) or interventional radiology (IR), there can be a lot of unknowns. What can I expect on the big day? What will happen after I’m all done? Will I have to worry about my orders not being in the system? Who can I call if I have any last-minute questions? It’s easy for your thoughts to race as you approach your procedure date, but luckily, there is a team who puts your mind at ease. With Renown Health’s Surgery & Procedure Scheduling department, patients can breathe a sigh of relief knowing that all the nitty-gritty is taken care of before they step foot in the procedure room. This team operates in the mindset of a complex Tetris board – fitting in all the pieces to make sure every patient is set on the path for surgery success. Consistent Contact Our Surgery & Procedure Scheduling team has a unique history. Initially operating as two separate teams, over the last year, our leaders skillfully combined the two teams together under one umbrella. That allows the now singular team to have line of sight across every surgery and Cath or IR procedure plan and be better stewards of the resources they have at their fingertips to provide streamlined, more-connected care for patients. As one might imagine, with the merger of the two teams, the day-in-the-life of each team member is full of a variety of crucial checklist items to cross off – all supporting constant communication from patients to providers. On the surgery scheduling front, these team members are resource rockstars. From working with referring providers to get patients scheduled appropriately to ensuring rooms and equipment are available for every patient, this team makes sure everything and everyone is in place when the time comes to help create a successful procedure and the best possible patient experience. “In surgery scheduling, we handle inbound calls for the outside offices to get time scheduled for each patient in the operating room (OR),” said Lydia Sharkey, Senior Scheduler. “We make sure there are plenty of anesthesia resources and equipment for every surgery, including any important information that we need to schedule patients appropriately and adding all documents to the OR board. If we need to swap rooms or move patients around, we handle that process too.” Over on the IR/Cath scheduling side of things, this team is on the frontlines of patient communication. They are experts in helping patients navigate their procedure from start (seeing their provider and obtaining the proper referrals) to finish (the day of the procedure and post-procedure process). “My day is a little different than the hospital schedulers; our part of the team handles the outpatient aspect,” said Adrienne White, Senior Scheduler. “We are in constant contact with patients and the IR and Cath departments. We help them navigate their procedure, including what to expect during and after the procedure. We get them through the process as easily as possible and ease their minds, so they know what is going to happen every step of the way. It’s all about communication, communication, communication!” This department has a significant overarching role: make sure all documents and ancillary information is set up for all our clinical teams that help with surgeries and procedures. This critical work means that every process is followed, and no important details are left out. “No one wakes up and says, ‘I want to have surgery;” our team goes above and beyond to make sure every single detail is taken care of so that when patients arrive, everything is in place,” said Trisha White. “Our team works hard to ensure everything runs as efficiently as possible because we want to use our resources in the best way possible to serve our patients without delays. We make sure we receive all the orders, codes and insurance and that the teams that follow after us – including our pre-admit team and nurses – have all the information they need to do their job seamlessly." With all the work they accomplish daily – not to mention how they wholeheartedly support each other through it all – it’s no question that the entire team has a lot to be proud of. Besides helping make patient care possible, the team puts their departmental merger and the move to fully remote work at the top of the list. “We’re most proud of merging the surgery scheduling and procedure scheduling teams together and therefore more cohesive,” said Mary Gray, Senior Scheduler. “The merger has made our team blossom and be able to connect with and rely on one another even more. We aren’t afraid to speak up and say something. At the end of the day, we’re here to take care of the patient, but we also help each other out. Our morale has gone up, and everybody is happier. Even though we all work remotely, we are more connected and have a great work-life balance.” “Along with transitioning the two teams into one big team, the move to being fully remote was huge," added Patricia Cruz-Hernandez, Surgical RN Scheduling Coordinator. “We worked through all the glitches, and it was a seamless transition to move into a remote setting. What’s great is that it did not affect patients at all; everything still gets done exactly as it should.” No matter how busy the days may get, Renown’s surgery and procedure schedulers always remember one thing: they are incredibly grateful for their fellow team members. “We have a very efficient and hard-working team of women,” said Pam Chapa Valencia, Senior Scheduler. “I could not have handpicked better people for our team,” added Trisha White. “I feel so lucky to have the team that we have.” A Renown “Why” Our Surgery and Procedure Scheduling team members all have diverse stories to tell about their road to Renown and why they’ve stayed in the department for as long as they have. Whether they’ve been with us for two years or two decades, they all share the same strong calling to care for their community. “I always wanted to help people, and my grandma was a nurse,” said Pam Chapa Valencia, Senior Scheduler. “I loved hearing her stories, and it made me want to be involved in patient care.” “I have a caring nature, and a hospital nature seemed like the right fit – I've been here for 25 years,” added Mary Gray. Several of our schedulers recognized the influence Renown has within our community and the ability to grow professionally and personally, both of which were a driving factor in their decision to make our health system their long-term career. “I’m originally from southern California, and I moved here about eight years ago; my husband always talked so positively about Renown, especially with how big it is and how it has the only level II trauma center in northern Nevada, so my goal was always to get a job here,” said Lydia Sharkey. “It’s been a great environment to be a part of.” “I’ve been with Renown for 17 years, and I chose to come here because of the reputation of the services Renown provided and care they gave,” added Trisha White. “I also knew what opportunities there were for me professionally, and in doing so, we are taking care of our community. I’ve had the chance to grow within my own professional skills and leadership skillset.” A profound feeling of ‘home’ is a common theme among this department. These team members appreciate the sense of community Renown has, the strides we’ve made in expanding our reach and how our health system gives healthcare professionals who are new to the field a chance to succeed. “At the time, Renown was the only hospital that would train nurses, and as a brand-new nurse, I had no experience – Renown took a chance on me,” said Patricia Cruz-Hernandez. “I feel like this is home. Our health system is so community-based and people-first minded, keeping ‘mission over margin.’ We’re growing, we’re expanding, we’re everywhere!” “I was a part of a transition as the cardiology private practice I worked with became a Renown practice, and it was great,” added Adrienne White. “This transition enabled us to provide more services and better care to patients. I stay here because I see the leaps and bounds we’ve been able to make in terms of procedures, accessibility and patient experience.” As true advocates for both patients and each other, the team is proud to have found their niche – and the ultimate beneficiaries? Everyone undergoing a surgery or procedure at Renown. A Culture of Kindness and Gratitude When you meet the Surgery & Procedure Scheduling team, you are greeted with warm smiles and an enthusiastic “Nice to meet you!” You can’t help but smile back and feel the infectious kindness they exude. Renown operates with a People-First mindset, a vision that this department especially takes to heart. They emulate the exact definition of our “Collaboration” cultural commitment. “We’ve built very good relationships and rapport with the OR managers and board runners,” said Lydia Sharkey. “The communication that we have at all three locations is very solid.” “The OR leadership is always so willing to help out whenever they can, and the resources they’ve provided have been huge for us,” added Adrienne White. “All the teams that see the patients after us – especially the surgical pre-admit team and the case managers, are fantastic about collaborating with us and reaching out to solve any issues they may have,” added Trisha White. “We all work so well together, especially since we all impact patient care.” In any organization, strong and compassionate leadership is key to a thriving team. Luckily for our surgery and procedure schedulers, they have Trisha White on their side. They attribute a lot of their success to having a supportive leader who “gets it.” “Trisha has been a scheduler like us, so she completely understands when we’re having an issue, because she’s struggled with the same thing and knows where we are coming from,” said Mary Gray. “It makes us feel like we are not alone – I can always reach out to her, or any of my other coworkers, to ask questions and figure out a solution together.” Despite being a remote-only team that meets in-person only one or two times a month, this group never misses an opportunity to reconnect both online and offline. They frequently shout out their Culture Ambassadors, schedulers Pam Chapa Valencia and Roxanne Abundis, for their team’s high morale. “Even though we all primarily work remotely, our in-person days are some of my favorite days of the month,” said Trisha White. “We feel so uplifted, we laugh and we have fun. We love being with each other. Pam and Roxanne are our Culture Ambassadors, and they both have been amazing at planning fun things for our teams. They go above and beyond to make our team feel cohesive and included.” “Pam and Roxanne have been leaders in creating a fun environment and supportive culture for us,” added Lydia Sharkey. “Whether it’s creating care packages or making sure we all have a good time when we see each other in person, they deserve a lot of credit.” As this team excels in their roles and foster a culture rooted in kindness and gratitude, we can trust that Renown’s surgeries and procedures will continue to thrive, and patients will continue to benefit from their diligent efforts and commitment to efficiency. “We make the magic happen!” closes Mary Gray.
Read More About Department Spotlight: Surgery & Procedure Scheduling
-
Departamento destacado: Patología
Celebrate Leap Day by leaping into the world of Pathology at Renown Health! Think of discovering a diagnosis like solving a mystery: the condition is the suspect, the nurses are the frontline police force and the doctors are the lieutenants or captains finalizing the results of the case. You may notice that one crucial role is missing on this list – the detectives. In the diverse network of healthcare, the detectives are a significant part of each patient’s mystery-solving care team and represent many roles across our health system. When it comes to figuring out the elaborate details of a growth, disease, organ abnormality or cause of death, one team of detectives, quite literally, goes as deep as possible. Those detectives are the team members within Renown Pathology. For each specialized field within medicine or surgery, the Pathology department is here to play a crucial role in accurate diagnoses. With each slide examined and each test meticulously conducted in their bright laboratories, these dedicated professionals shape a path towards wellness and recovery. Meet Your Anatomy Experts Whether you have a chronic disease that needs consistent testing, a high-risk birth that requires placenta testing, a suspected cancerous tumor that needs a biopsy or a gall stone that must be removed (or anything in between), Renown’s Pathology team steps in to provide biological answers to your body’s questions. This department offers the most comprehensive in-house diagnostic testing in the region, from routine histology to full pathology. As the busiest pathology department in northern Nevada, this team boasts the fastest turnaround times from respected experts, including: Pathologists Pathology Assistants Histotechnicians Histotechnologists Clinical Lab Assistants Let’s break down the complex nature of these team members' jobs by walking through their everyday responsibilities at work! Pathologists Pathologists are medical doctors who specialize in the study and diagnosis of disease. With every slide they scrutinize and every sample they analyze, pathologists unravel the mysteries of disease with precision and compassion. Their responsibilities include interpreting laboratory tests, analyzing tissue and fluid samples (obtained from a variety of different sources, including biopsies and surgeries), staging cancer diagnoses and providing diagnostic insights that guide treatment decisions. “Our job is to help the patients and their doctors figure out what’s wrong,” said Dr. Christie Elliott, Pathologist and Medical Director of the Clinical Laboratory at Renown Regional Medical Center. “As the bulk of our cases deal with cancer, almost every day we start with a tumor board alongside fellow surgeons, oncologists, radiologists and geneticists. From there, we order extra studies, run through our cases to make diagnoses, review slides and ensure all information goes into the charts, which is especially important as 70% of data in medical charts is from the lab. A patient’s history is everything.” Pathology Assistants With the steadiest of hands, pathology assistants, also known as PAs (not to be confused with physician assistants), guide the diagnostic journey from patient specimen to diagnosis. They can typically be found processing surgical and biopsy specimens (includes accessioning, gross examination, description, and sampling for microscopic analysis), preparing tissue samples for microscopic evaluation, helping the pathologist determine a cause of death for autopsies by conducting organ dissections and maintaining detailed records of all diagnostic findings. “As a PA, I still impact patient care without being directly patient-facing,” said Andrew Whitner, Pathology Assistant. “I handle 300-350 small tissue blocks a day. During dissections, I identify landmarks, document what I see and turn those landmarks into slides, looking for things that don’t look normal.” “Our job is 90% all about gross specimens, and we also do eviscerations for autopsies,” added Leslieann Haffner, Pathology Assistant. “We are trained on what normal looks like; our goal is to find the abnormal.” Histotechnicians Histotechnicians work behind the scenes to help transform ordinary tissue into extraordinary windows of insight, revealing the inner workings of the human body. As vital members of the Pathology team, histotechnicians embed tissue specimens in paraffin wax blocks (a process that preserves the tissue's structure for examination), cut thin sections of tissue from the paraffin blocks using a microtome, mount tissue onto glass slides and stain the tissue slides using histological stains to highlight structures or cells. “With all the patient specimens we work with, we get to see a lot of organs and learn what is causing the abnormalities,” said Reiny Hitchcock, Histotechnician. “I enjoy the opportunities to expand my knowledge, especially while working alongside the doctors.” “Our job can change by the week,” added Jessica Fahrion, Histotechnician. “One week I’ll be in the grossing room, and the next week I might be training in cytology." Histotechnologists In a world where every slide holds the key to a patient's future, histotechnologists are the champions of progress. One career ladder step above histotechnicians, these team members often have a broader scope of responsibilities, including more complex laboratory procedures, developing and validating new techniques, managing laboratory operations, interpreting results and troubleshooting technical issues. You can count on histotechnologists for validating antibodies and handling orders from pathologists, oncologists, emergency physicians and more. “My day always involves looking into cases, reading reports, getting orders together and working with pathologists to help them with their diagnoses; I also work a lot with immunohistochemistry, helping out with routine slides,” said Charles Koeritz, Histotechnologist. “I especially enjoy doing validations, which help maintain the integrity of lab testing and our diagnostic processes.” Clinical Lab Assistants Our pathology clinical lab assistants are the masters at “filling in the blanks,” assisting in whatever area needs it most, especially in cytology and the grossing room. They are essential aspects of the Pathology team, collecting and storing specimens for further testing, assisting in managing test results, gathering data, managing supply inventory and more. “As a Clinical Lab Assistant, I can be scheduled anywhere, from tissue cassetting to grossing,” said Ellie Somers, Clinical Lab Assistant. “Working in cytology is one of my favorite parts of my job. It’s very rewarding to work with the doctors to uncover what treatments will help each patient. We do cytology very well here.” The Bottom Line Even though the Pathology department doesn’t always experience a lot of patient face-to-face time, they interact with patients in a different way – by uncovering the story that is the inner workings of the human body, one slide and one sample at a time. “It’s important to remember that the slide IS a patient,” said Dr. Elliott. “We are constantly learning from every case so we can continue to provide the best patient care possible.” Take a Photo Tour of the Pathology Lab!
-
Living with COPD? How to Maximize Your Summer Experience
June offers an official welcome to summer and the height of outdoor activities in northern Nevada such as hiking, camping, days spent at the lake and embracing long days and warm evenings with friends and family. Enjoying all that the summer season has to offer may not be as easy for those living with chronic obstructive pulmonary disease, or COPD, which effects more than 15 million Americans. What is COPD? COPD is a group of lung diseases including emphysema and chronic bronchitis that result in airflow blockages from the lungs. People may experience frequent coughing and shortness of breath among other symptoms. COPD typically impacts adults ages 65 and older and is becoming increasingly more common among women. Although smoking plays a key role in the development of COPD, air pollution and indoor air quality, and respiratory infection also contribute to disease development. While there is no cure for COPD, limiting progression of disease and managing symptoms can be achieved through lifestyle changes, therapy, and medications. Tips for Living with COPD This Summer, and Always Stay Hydrated: Staying hydrated is extremely important for people with COPD, especially during the summer. Not drinking enough water can make breathing more difficult because it increases respiratory symptoms. Make sure to always keep a water bottle with you and aim to drink 8-10 glasses of water daily. Be Mindful of Temperature: COPD symptoms can be exacerbated by hot weather. It is best to participate in outdoor activities during the cooler times of day, like the morning or evening. Check Air Quality Before You Go: Before engaging in outdoor activities, be sure to check the air quality index and plan your activities accordingly. Pace Yourself: Exercising can be difficult for people who have COPD. To make the most of your summer, try not to push yourself too hard and take breaks when you need them. If you start to feel out of breath or tired, take a break in a cool, shaded area until you feel better. Take Matters Into Your Own Hands To address the needs of community members living with COPD, the Renown Health Research Office has teamed up with Pulmonary Medicine to provide patients who are former or current smokers and have a history of frequent exacerbations with an option to participate in the ARNASA study. "COPD exacerbations have a huge negative impact on patient’s lung function” states Dr. Farah Madhani-Lovely, Chief of Pulmonary Medicine at Renown Health and Assistant Dean of Clinical Research at the University of Nevada, Reno School of Medicine. “We have had inhalers and prednisone for decades but patients are still having exacerbations. Now we have a new pathway we think will prevent exacerbations which is what this clinical trial is designed to prove.” This study will evaluate the efficacy and safety of astegolimab compared with placebo in participants 40-80 years of age with COPD. “This study in particular is so exciting because of the enthusiasm from the sponsor’s end” says Katie Buckley, Lead Clinical Research Coordinator working on pulmonology studies at Renown’s Clinical Research Office. “Often times sites aren’t assigned particularly passionate or engaged personnel who aid in carrying out these studies, but you can tell Roche Genentech’s team truly cares about the success of the study, the safety of their participants, and proving the efficacy of the investigational agent. Working on a study like this takes a village, and when the individuals on all ends share similar mindsets and work towards success as a collective unit instead of as individual moving parts, it’s amazing to see everything we’re able to accomplish.” Renown’s team of expert pulmonologists and researchers are available to join patients with COPD in support of their healthcare journey. If you are interested in learning more about this clinical trial option at Renown Health, talk to your pulmonologist at your next appointment or contact us at 775-982-3646. At Renown Health, our goal is to make it easy for patients to access clinical research as a care opportunity where patients can access a variety of standard care treatment options for their health condition or choose to participate in a clinical trial. For more information about clinical trial opportunities available to you or to ask any questions, contact the Renown Research Office at Renown-CRD@renown.org or 775-982-3646.
Read More About Living with COPD? How to Maximize Your Summer Experience
-
What Is an Echo-Tech?
When it comes to our heart, keeping this vital source of life in tip-top shape is of utmost importance. Echo technologists or echocardiographers, otherwise known as "echo-techs," are charged with that mission, providing critical information that leads to life-saving interventions to keep our hearts beating strong. Adrianne Little, echocardiographer at Renown Health, breaks down the echo-tech's role in the health system, the educational path it takes to get there and the unique perks that come with the profession. What does an echo tech do? “Echo techs play a key role in the diagnosis and treatment of patients,” said Adrianne. “We are members of the cardiovascular imaging team that perform ‘heart ultrasounds’ or echocardiograms. Although we are most commonly known as echo techs, our official title is either ‘cardiac sonographer’ or ‘echocardiographer.’” Echo techs use imaging technology and sophisticated ultrasound equipment to produce images of the heart. These images show how well the heart functions, as well as the valves, chambers and blood flow. Echocardiograms are used to diagnosis and treat a variety of heart conditions such as murmurs, arrhythmias and heart failure. At the end of the day, the main goal of echo techs is to help our cardiovascular team provide the quickest and most accurate diagnoses to help with patient management and help them receive the highest standard of care. “When it comes to looking at the heart, we are part of the front-line team," said Adrianne. “We provide real time critical information that leads to life saving interventions down the road.”
-
11 Tips Caregivers Need to Know
Becoming a caregiver or playing a more active role in another’s healthcare is a big responsibility. At some point, almost all adults will support an aging parent or a loved one in need. Keeping track of their needs and wellbeing, while also prioritizing your own can become overwhelming. It’s important to know: you are not alone, and help is available. Read on for 11 tips to help you manage your time, your own wellbeing and your loved one’s care. Self-care comes first. When your main priority is the person in your life who needs care, it’s easy for your own needs to take the backseat. Give yourself time each day to focus on your personal wellbeing. It’s hard to give a loved one the care they need if your own needs are not met. Prioritize the Activities of Daily Living (ADL). Make a note of what ADLs your loved one can do alone, what they need help with and what activities require the most help. This will help you work through the day with them, as well as plan out how the day’s activities will go. Do a home safety audit. Do showers, bathtubs and steps have safety grab bars? Look around the house for additional tripping hazards, like rugs or electrical cords. If your loved one struggles with day-to-day navigation of the home, consider scheduling an occupational therapy appointment. This type of therapy helps a person develop or maintain the motions required to accomplish daily tasks. You might also qualify for a referral to in-home healthcare, such as Home Care. Have the hard conversation. The best time to discuss views about end of life care and to learn what choices are available is before a life-limiting illness or crisis occurs. With advance care planning, you can help reduce the doubt and anxiety related to decision making at the end of life. Completing an Advance Directive is a great tool to sort out all these decisions before they’re needed. Attend a free workshop to learn more and complete this important document. Identify when you need respite. Respite care involves receiving a short-term break from caregiving. Organizing in-home care for your loved one will allow you to step away and tend to your needs. By identifying what kind of respite care you are seeking, you can find the right person to provide you with that much-needed break. Don’t wait until you feel overwhelmed, plan ahead. Write down insurance contact information. Have a direct connection to the right insurance professional for support and advice. If your loved one is eligible Medicare, this is a good opportunity to review their current selections and if they would benefit from a Medicare Advantage Plan or Medicare Supplement Insurance. Seeking out expert advice or information on Medicare options is a great way to navigate this. Consider calling a broker, or attend a free educational seminar with Senior Care Plus. Gather legal and financial information. Make a list of all existing legal documents and financial accounts that your loved one has. These might include a will, advance directive, power of attorney, bank accounts or investment accounts. If you have questions about how to manage them, or need assistance in setting up additional framework, reach out to a lawyer, legal service, financial adviser or bank representative. Create an inventory of medical information. Identify where all of your loved one’s medical records are, as well as a list of providers or healthcare practices where they have received care. Consider if you should have your loved one give you Proxy Access in MyChart, which allows you to access all the features in MyChart on their behalf, including viewing upcoming appointments, viewing test results and emailing a doctor on their behalf. Make a list of what others can do. Think about all the little (and big) things that need to happen, and write down tasks that others could take care of you. When someone says “let me know what I can do” you’ll be ready with a pre-written list of items they may be able to assist with. Tasks could include tackling around-the-house repairs, scheduling lawn work, helping to walk the dog, taking a car for an oil change and cleaning. Find programs and events for social enjoyment. If and when possible, seek an activity outside of the home. Look for community centers that have programs for seniors, recreational activities or meals that you can patriciate in together. If leaving the home is not an option, arrange for visits or in-home activities, such as movie nights, card games or time to visit with family. Research long-term options. If you will be considering a nursing home or assisted living, make a list of amenities that you and the person you are caring for would like. Take this list with you when visiting potential locations to make sure you don’t forget to ask about each item.
-
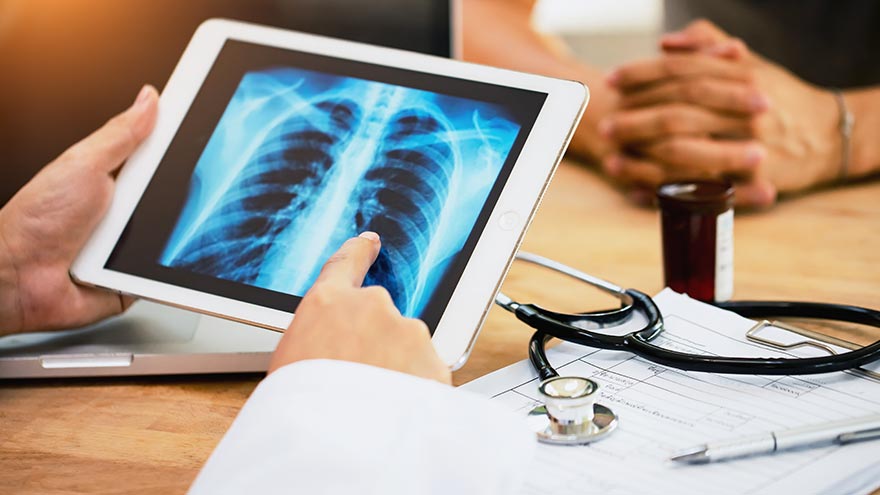
Lung Cancer Screening and Early Detection
Lung cancer is the leading cause of cancer deaths in both men and women in the U.S. The good news is the five-year survival rate increases dramatically if lung cancer is treated before spreading to other parts of the body. Julie Locken, MD, of Renown Health Imaging, explains more. What are the signs and symptoms of lung cancer? As you might expect, most lung cancer symptoms appear in the chest and can affect your breathing. Watch for signs such as: Persistent cough Constant chest pain Shortness of breath Wheezing Bloody or rust-colored phlegm Hoarseness Swelling of the neck Pain or weakness in the shoulder, arm or hand Recurring pneumonia, bronchitis or other lung infections Loss of appetite and loss of weight can also be signs of lung cancer That said, there are usually no symptoms in the early stages of lung cancer, which means getting screened can truly be a lifesaver. If you have a history of smoking, you should get screened as a precaution. What are the risk factors of lung cancer? Around 80% of lung cancer cases stem from a history of smoking tobacco. But there are other known causes, such as secondhand smoke, radon, asbestos and diesel exhaust. It’s important to do what you can to eliminate exposure to all of these to reduce your lung cancer risk. People with an immediate relative – a parent, sibling or child – diagnosed with lung cancer and people between 50 and 80 years old are also at higher risk and may need to consider screening. People who are at the highest risk are those with a history of smoking tobacco, particularly smokers who averaged one pack of cigarettes per day for 20 years or more, as well as former heavy smokers who quit in the last 15 years.
-
Alzheimer's Safety Tips for Caregivers to Know
November is National Alzheimer’s Disease Awareness Month. At Renown Health, we know that Alzheimer's safety for your loved one is a priority, as the symptoms can sometimes lead to unsafe situations. We asked Dr. Jonathan Artz – a neurology physician with Renown Health and an assistant professor of clinical neurology at the University of Nevada, Reno School of Medicine – for tips on keeping loved ones safe and secure. According to the Alzheimer’s Association, Alzheimer’s disease affects safety in various ways, specifically due to body and brain adjustments. These changes can include: Judgment, including forgetfulness Sense of place – getting lost on the way home Behavior – being suspicious or fearful Body difficulty – losing balance Sensing ability – noticeable sensitivity in hearing, seeing or temperature Dr. Artz gives us four major tips to ensure your loved one’s safety as you both navigate this disease together. Watch for Wandering Those experiencing Alzheimer’s disease tend to wander and get lost. Try the following tips to reduce the risk of wandering: Get your loved one an ID bracelet and have them wear it at all times. You can also enroll your loved one in “Wandering Support.” Install door chimes so you know when exterior doors are open. Ask neighbors to call you if they see your loved one out alone. Go with your loved one when they insist on leaving the house. Don’t argue or yell. Instead, use distraction or gentle hints to get them to return home. Discourage Driving Driving can be unsafe for someone with this disease. With this in mind, ask a doctor whether it’s safe for your loved one to drive. For example, on a case-by-case basis, there are certain situations where doctors are required to report individuals with particular cognitive impairments, wherein a form of a driving assessment will be recommended. Limit access to the car. Keep the keys with you or lock them away. Ask an authority figure, such as an insurance agent or a doctor, to tell them not to drive. Adult-Proof Your Abode A simple living space is a safe living space. This means reducing clutter and removing any issues that may pose a safety concern. You may also want to get advice from an occupational therapist (home safety expert). Keep in mind that some changes may not be needed right away. Focus on major safety concerns first. Try the following tips: Add lighting (or glow-in-the-dark tape) to brighten dark areas, including stairways and halls. Use color contrast or texture indicators for dials, knobs and appliance controls. Remind your loved one not to carry items while walking to avoid a fall. Remove sharp objects from drawers and countertops. Avoid using small throw rugs or doormats, as they are easy to trip on. Move frequently used items so that they are easy to reach. Lock away alcohol and tobacco products, as they are not recommended for dementia patients. Install handrails in the shower, tub and near the toilet. Bathroom falls are especially common. Adjust the setting on your hot water heater so water does not scald. Those with Alzheimer’s can lose their sensitivity to temperature. Move and lock up hazardous chemicals and cleaning supplies, such as bleach and insecticides. Disable and remove guns or any weapons. Supervise any medication taken by your loved one. Promote a Positive & Healthy Lifestyle Continually emphasize the strengths of your loved one by promoting participation in meaningful activities, wellness visits and healthy habits to help them improve their well-being. Here are some ways to keep them physically and mentally active: Maintain regular vision and hearing screenings and make necessary adaptations. Establish a routine for daily activities. Encourage participation in self-care and leisure activities. Work with your loved one’s doctor to establish a healthy diet. Ensure proper hydration. It may help to set reminders for your loved one to drink fluids. Encourage regular exercise. Exercise delivers oxygen to the brain, improving brain health. Promote good sleep habits. Good quality sleep can increase overall brain health and has been associated with improving memory, attention and concentration. Resources and support are available with the Renown Memory Disorders Program. Providers within this program are specifically dedicated to treating several different memory-related disorders. Memory Disorders Resources & Support.
Read More About Alzheimer's Safety Tips for Caregivers to Know
-
3 datos importantes de atención médica para la generación milenial
Many millennials are fortunate to have good health, but it’s important to be prepared for your next doctor’s visit. Here are three things that millennials should stay on top of for tracking and maintaining their health. For many millennials, doctor visits and preventive healthcare fall by the wayside. Alison Lynch, MD, a family medicine provider with Renown Medical Group says there are a few key things you can do now to set yourself up for a healthy future. 1. Establish with a Primary Care Provider Millennials are more likely to go to urgent care or consult the internet when a healthcare issue arises. While these are helpful tools, here’s a better one: a primary care provider. The benefit of establishing with a primary care provider is that your medical records, history and a baseline for your health will be documented. That means that when a problem or question comes up, your doctor will already have helpful information on file and can help you navigate your needs. Having a primary care provider is often required for prescription refills and referrals to a specialist. By establishing now, you’ll be able to get what you need in the future much faster. Make an Appointment Today 2. Protect Yourself and Your Community There are a few vaccinations and screenings that Dr. Lynch recommends for millennials. Flu Shots: These are available every year and are recommended for protecting not only yourself against the flu but also others you may come into contact with. Flu shots are usually available from August through December through your healthcare provider, pharmacies and pop-up events. Tetanus or Tdap: Most people receive a tetanus shot as a child, but it’s recommended that everyone get a booster every 10 years. If you are overdue, talk to your primary care provider or pharmacist about getting updated. Pap smear: If you’re a woman, a pap smear is recommended every three years in your 20s and every five years in your 30s. HPV vaccine: This vaccine helps prevent the virus that causes cervical cancer as well as the majority of head and neck cancers and warts. The HPV vaccine is recommended for all genders up until age 45. STD screening: Consider an STI/STD screening if you’re sexually active.
-
Cuidadores serviciales hacen realidad el sueño de una boda
A wedding is a big day for the wedding couple, but it’s also special for loved ones. A patient at Renown, Ken, got to take part in his daughter’s special day as her wedding plans changed to accommodate his medical condition. Grab some tissues and read how Renown’s team of compassionate caregivers and chaplains planned a wedding in Fianna’s Healing Garden. Ken was hospitalized at Renown Regional Medical Center where he was battling a lung problem – which was unrelated to COVID-19 – and his condition worsened rapidly on Wednesday, Aug. 12. His family made the decision to transition him to palliative care, which helps patients near the end of their lives remain comfortable, while supporting their dignity and quality of life. Ken’s medical condition altered wedding plans for his daughter, Chandra, and her fiancé, Tyler, who were planning to tie the knot later in 2020. Chandra wanted her father there, but knew he could not leave the hospital. That’s why Chandra’s sister, Heather, approached Ken’s care team with a request to have a small wedding ceremony at the hospital. Planning the Wedding A member of Ken’s care team, Amy Heston, registered nurse (RN), began planning how the wedding could be held outdoors in Fianna's Healing Garden in the E. L. Wiegand Pavilion, which was donated by the E. L. Wiegand Foundation. In 24 hours, Amy planned a wedding ceremony with the help of her colleague, Breyanna Aufiero, RN; the Renown Spiritual Care team; and nursing leaders on the coronary intensive care unit (ICU). Together, they decorated the aisle in the garden with flowers and battery-operated candles. They also made a sign for Ken’s hospital bed, which read, “Father of the Bride,” and crafted a bow tie for him to wear for the special occasion. With visitor restrictions in place at the hospital due to coronavirus (COVID-19), having the wedding outside in the Healing Garden allowed for more members of Ken’s family to attend including his wife, Charlotte, and his dog, Bella. Every step in planning the wedding required thoughtful and thorough care coordination so Ken could participate. His breathing was supported by oxygen and special arrangements were made to transport the oxygen tanks he needed to take part in his daughter’s wedding. Amy worked with respiratory technician, Kasey Benfield, and critical care technician, Ruben Duckworth, to ensure Ken’s oxygen needs were met using portable machines. Celebrating Love and Life Together Ken’s team of caregivers bathed him and shaved his face so he could look and feel his best for the ceremony. They put on his bow tie, covered his bed in decorations and his favorite blue, flannel blanket, and wheeled his bed outside for the ceremony. Renown associate chaplains Terri Domitrovich and Susan Palwick coordinated music and performed the ceremony for Chandra and Tyler on Thursday, Aug. 13, 2020. The bride and groom shared their first dance in the garden and Ken’s care team provided water and treats to give the family a full wedding experience. Shortly after the ceremony, Ken passed away. This wedding provided Ken and his family meaningful memories for their big life-changing moments as they celebrated and said goodbye. “Seeing Ken surrounded by family he never would have gotten to see again while in the hospital, watching him get to share a father-daughter dance with Chandra on her wedding day, and having him tell me that this day meant more to them than we would ever know were some of the most moving moments I’ve witnessed as a nurse,” Amy said. “I am so thankful for the team we have here. I know that this beautiful day wouldn’t have happened without the help of every single person who gave their time, money, creativity and passion to make it a day to remember.”
Read More About Helpful Caregivers Make a Wedding Dream Come True
-
Stay Inside When Skies Are Smoky
Even when fires burn outside our area, the air quality in the region can reach dangerous levels. Our expert explains how to maintain your lung health when fire season strikes. It’s a sight we know all too well as northern Nevadans — a hazy or thick layer on the horizon when smoke rolls in from nearby fires. Sometimes the smoke is more evident than others, but it’s important to remember, even when the smoke may not be as visible across the valley, it still impacts our air quality. The last week or so, our air quality has been in the “unhealthy for sensitive groups” range, which can be dangerous for people who are sensitive to air pollution. Air Quality Changes: Who’s at Risk? Renown Pediatric Pulmonologist Sonia Budhecha, M.D., explains certain people are especially at risk when smoke moves in: Older people, whose lungs are not as healthy as they used to be Young children, whose lungs are still developing People with heart and lung disease including asthma, COPD and emphysema “Smoke and haze from fires carry particulates that can get into your respiratory system and eyes, which can be a danger for all ages,” Dr. Budhecha says. How You Can Protect Yourself Until the smoke clears and the air returns to the “good” range, it is best to follow these tips to protect yourself and your family: Stay indoors and keep windows closed Turn on the air conditioning to recirculate clean air Drink plenty of fluids to help your body flush out any toxins you inhale Additionally, all community members should reduce their physical activity and try to prevent heavy exertion outside. If you or a loved one has a heart or lung disease, avoid physical exertion altogether because smoke can aggravate these conditions. “People with heart disease may experience shortness of breath, chest pain, palpitations or fatigue,” Dr. Budhecha says. “People with lung disease may also have shortness of breath, chest discomfort, wheezing, phlegm or a cough.” Smoky Signs and Symptoms Smoke can also impact healthy people — irritating your eyes, nose or throat. And in some cases, inhaling smoke can lead to bronchitis. When haze moves into our area, keep an eye out for these symptoms: Burning or stinging eyes Runny nose Cough or scratchy throat Headaches Wheezing Shortness of breath Difficult taking a full breath Chest heaviness Lightheadedness Dizziness If experiencing any of the above symptoms, seek medical attention or call your doctor for advice. Sometimes, these symptoms do not appear for as long as 24 to 48 hours after smoke inhalation. For those that have pre-existing lung or heart conditions, consult with a health care provider on action or management plans. To schedule an appointment Visit Renown Pulmonary Medicine, or call 775-982-5000. Understanding Our Air Quality The Air Quality Index (AQI) is broken down by large (PM10) and small (PM2.5) particulates. According to Dr. Budhecha, large particulates are usually ones that can be seen and smelled. They can damage your eyes and nose but don’t often get deep in the lungs or blood vessels. “The more dangerous ones are PM2.5, which can’t always be seen or smelled,” Dr. Budhecha says. “Any time the AQI is above 51, children with lung or heart disease should not be outdoors.” For the latest air quality update in your area, visit AirNow.gov or call (775) 785-4110.
-
Get Moving: How to Exercise with Arthritis
An arthritis diagnosis doesn’t mean your exercise routine has to end. In fact, a consistent routine can actually improve mobility. Although stiff and painful joints can make it difficult to keep moving, staying active is essential for easing pain. October 11 is World Arthritis Day, so we asked Michelle Higgins, MPT at Renown Physical Therapy & Rehab some advice about exercising with arthritis. According to the Arthritis Foundation, arthritis affects one in five adults and 300,000 children. As a matter of fact arthritis is the nation’s leading cause of disability. Your joints certainly don’t need to suffer when you exercise. In general exercise is actually necessary for those with arthritis. Not only does it reduce joint pain, but it also increases strength and flexibility. Furthermore those adopting a regular exercise routine also have more energy, deeper sleep and find it easier to maintain a healthy weight. “Exercise is a necessary component to managing your arthritis,” says Higgins. “Consistent participation in an exercise program has been shown to promote long-term pain relief, increased body function and an improved quality of life. Alternatively, a lack of exercise can actually increase joint pain or stiffness and eventually lead to long term disability and suffering.” Exercising With Arthritis Exercise truly is the most effective non-drug arthritis treatment available for reducing pain and improving movement. And it can even include daily activities like gardening, dancing or walking your dog. Of course talk to your doctor or physical therapist about what exercises fit into your specific treatment plan. With this is mind, the four specific components below are important to an effective arthritis exercise program: Range of motion Moving joints through their full available range of movement is important. This frequently increases function and decreases joint stiffness and pain. For this reason, aim to complete these exercises daily. Examples include bending, straightening, and rotating specific joints, or static and dynamic stretching. Strengthening These exercises target muscles supporting and protecting our joints and bones. Strengthening is also necessary for weight control, so two-to-three sessions per week are recommended. In order to allow your body to adapt, begin with light resistance and start slow. Strength exercises include weightlifting and using resistance bands. Low-impact aerobic exercise Aerobic exercise is certainly necessary for overall well-being, weight management and heart health. Aim for two-to-three sessions a week. Low-impact exercises include walking, swimming, cycling, elliptical machine exercises and water aerobics. Balance Good balance is also vital for an effective arthritis program. On the positive side, solid balance prevents falls by increasing your ability to stay upright whether you are moving or sitting still. Likewise, it improves your confidence with walking and daily activities. In order to keep excellent balance, incorporate daily balance exercises. Examples of balance exercises include the use of an exercise ball, Tai Chi and exercises such as standing on one foot. Start Slow, Finish Strong As you begin your exercise program, remember to listen to your body. Start slowly – it can take several weeks for your body to adjust to exercise. Consult your doctor, or physical therapist, if you experience increasing pain or swelling which doesn’t go away with rest. Above all, incorporate fun and motivating activities so you’ll stick to them long term and improve your results. Renown Physical Therapy & Rehab 775-982-5001 Through outpatient physical, occupational and speech therapy, Renown Physical Therapy & Rehab gives you hands-on, individualized treatment in convenient Reno/Sparks locations. We have the latest, most advanced physical therapy and rehab equipment, specialty services and treatments. Renown Physical Therapy & Rehab is now open on Robb Drive in addition to three additional locations in Reno and Sparks. Call 775-982-5001 or visit us online.